Previous Issues Volume 3, Issue 1 - 2018
Prevalence of Specific IgG to Food Antigens in Bulgarian IBS Patients: A Preliminary Study
Tsvetelina Velikova1*, Iskra Altankova1, Milena Peruhova2, Antoaneta Mihova1, Alexander Kukov3, Viktoriya Georgieva2 , Nonka Yurukova2, Gergana Mizgova4, Tsanka Mehandzhiyska-Marinova4,6, Velislava Terzieva1, Galina Zhelezova5, Ludmila Ivanova6
1 Institute for Research and Development of the Sustainable Ecosystems (IRES), Srebrnjak 59, 10000 Zagreb, Croatia. 2 University Hospital Centre Zagreb, Department of Oncology, Kispaticeva 12, 10000 Zagreb, Croatia. 3 Aviva Medical Center, Nemetova 2, 10000 Zagreb, Croatia. 4 University of Zagreb, School of Dental Medicine, Gunduliceva 5 10000 Zagreb, Croatia. 5 RUDN University, Miklukho-Maklaya str. 6 Moscow 117198, Russia. 6 University Psychiatric Hospital Vrapce, Bolnicka cesta 32, 10090 Zagreb, Croatia
Corresponding Author: Tsvetelina Veselinova Velikova, Clinical Immunology, University Hospital 'Lozenetz', Kozyak 1 Str., 1407 Sofia, Bulgaria, Tel: 00359883306049; E-Mail: [email protected]
Received Date: 06 Nov 2018 Accepted Date: 15 Nov 2018 Published Date: 20 Nov 2018
Copyright © 2018 Velikova TV
Citation:Velikova TV, Altankova I, Peruhova M, Mihova A, et al. (2018). Prevalence of Specific IgG to Food Antigens in Bulgarian IBS Patients: A Preliminary Study. Mathews J Nutr Diet. 3(1): 017.
ABSTRACT
Since food intolerance in IBS patients may be mediated by IgG-dependent mechanisms, we aimed to investigate the prevalence of specific IgG antibodies to a panel of common food antigens in a Bulgarian cohort of IBS patients. We enrolled fifteen patients with IBS at mean age 36-10 years, diagnosed according to the Rome IV criteria. Specific IgG to food antigens in serum samples were assessed by IgG Screen Nutritional 24 ELISA. In our IBS patients we found that 40% have significant levels (> 3.51 U/ml) of specific IgG to egg white, 53,3% to cow milk, 33,3% to wheat, 20% to orange, 33,3%, to kiwi, 20% to tomato, 26,7% to garlic, 26,8% to hazelnut. Moreover, we found that 6,7 - 13,3% of IBS patients have IgG to egg white, cow milk, wheat, kiwi and hazelnut above 50 U/ml. We found also correlations of the specific IgG antibodies of some pairs of food antigens (mostly for codfish, wheat and other grains) where the correlations were assessed as moderate to strong. In conclusion, the serological determination of specific antibodies (IgG) against different food antigens may be beneficial to all individuals who are suffering from food intolerance, including patients with IBS. However, we should use these test with caution.
Keywords: IBS; Food Intolerance; Food Antigen; Specific IgG Antibodies; IgG-Mediated Hyperreactivity.
BACKGROUND
Irritable bowel syndrome (IBS) is a common functional gastrointestinal disorder which thought to be a multifactorial condition. However, many IBS patients associate their symptoms with food intolerance. In addition, the predicted prevalence of food hypersensitivity in IBS appears to be higher than in the general population (20-65% of patients with IBS complain of adverse food reactions) [1]. Food hypersensitivity in IBS patients may be mediated by IgG-dependent mechanisms (thought to be mostly Ig4) that are not yet fully understood. The aim of our study was to investigate the prevalence of specific IgG antibodies to a panel of common food antigens in a Bulgarian cohort of IBS patients.
MATERIALS AND METHODS
In this single-center study, we enrolled fifteen patients with IBS (three males and twelve females at mean age, 36-10 years (range 25-58). Patients with IBS were diagnosed according to the Rome III criteria after conducting necessary studies to exclude physical, radiological or endoscopic abnormalities or laboratory findings indicating an organic disease. The exclusion criteria included any clinically significant systemic disorder, inflammatory bowel disease, immunodeficiency, prior abdominal operation, or pregnancy. All participants were asked to fill a questionnaire about their symptoms, complaints, etc. We recruited patients from the Gastroenterology Clinic at the University Hospital 'Lozenetz' (Sofia, Bulgaria). This study was approved by the ethical committee of the Medical Faculty, Sofia University, Bulgaria, and we obtained written informed consent from all participants after explaining them the purpose of this study.
Enzyme immunoassays were performed in the serum samples for the detection of specific IgG to food antigens by IgG Screen Nutritional 24 ELISA (ILE-SCG25; IMMUNOLAB GmbH, Germany) according to the manufacturer`s instructions. The results are presented as intervals of reaction classes (<0.35 U/ml - class 0, 0.36-0.70 U/ml - 1; 0.71-3.50 U/ml - 2; 3.51-17.50 U/ ml - 3; 17.51-50 U/ml - 4; 51-100 U/ml - 5; >100 U/ml - 6). The raw data were analyzed using the Software Package for Statistical Analysis SPSS, v.19 (IBM). Differences were considered statistically significant at p < 0.05.
RESULTS AND DISCUSSION
Clinically significant results are assumed when IgG to food antigens are found to be above class 3, where the higher the class, the more antibodies are detected and more clinical symptoms are expected.
In our IBS patients we found the following percentages of them having clinically relevant intolerance (specific IgG > 3.51 U/ml) as follows - to egg white - 40%, to cow milk - 53,3%, to wheat - 33,3%, to rye - 13,3%, to oat - 13,4%, to rice - 13,3%, to orange - 20%, to kiwi - 33,3%, to celery - 6,7%, to carrot - 6,7%, to tomato - 20%, to garlic - 26,7%, to hazelnut - 26,8%, to peanut - 6,7%, to curry - 13,4%, to pepper - 13,3%, to sesame - 6,7%, to baker`s yeast - 13,3% of the investigated patients.
No one of the tested patients were detected as being intolerant to banana, strawberry, soybean, pork, and beef (specific IgG < 3.50 U/ml). When the results of specific IgG to food antigens are determined as class 1 and 2, as in this case, tested foods should not cause any problem assuming no further intolerance.
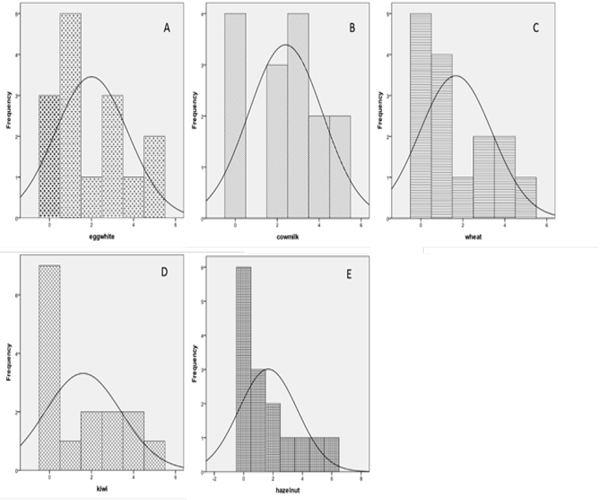
We present our data for the five most sensitizing food antigens, inducing specific serum IgG in different degrees (Figure 1). We found that 13,3% of IBS patients have specific IgG to egg white and cow milk above 50 U/ml (Figure 1A and B), to wheat and kiwi - 6,7% (Figure 1C and D), to hazelnut - 13,4% (and 6,7% above 100 U/ml) (Figure 1E).
Figure 1: Prevalence of specific IgG to egg white (A), cow milk (B), wheat (C), kiwi (D) and hazelnut (E) in patients with IBS. The results are presented as a number of patients and the quantity of specific IgG as reaction classes. The reference line represents the normal distribution.
Many studies indicate that the elimination of foods to which IBS patients have an elevated IgG titer results in an improvement in the symptoms and their quality of life [2-6]. Thus, based on the results of the tests for the determination of specific IgG to food, the physician could recommend an appropriate exclusion or rotation diet as follows. Foods found with classes 3 and 4 should be consumed every fourth day over a time period of 4 - 6 months only. Exceptions are milk, egg, wheat, peanuts and some special antigens which should be already eliminated from a class 3 result. When the specific IgG to certain food are determined as classes 5 and 6, these foods should be eliminated up to one year depending on the detected food and symptom. It is assumed that the period of 1 year could allow to specific IgG antibodies to be eliminated of the body [7,8]. However, one should have in mind, that memory B cells could secrete specific antibodies once again after the encounter of the same food antigens. However, not all positive results mirror the clinical presentation of the IBS patients. Thus, it is recommended to repeat the test after several weeks to measure the success of the diet.
We found also some correlations of the specific IgG antibodies of some pairs of food antigens. The most prevalent associations were observed for codfish and other foods, wheat and other grains among them, and with other foods, where the correlations were assessed as moderate to strong. Our preliminary results emphasize the possibility of a higher association between intolerance to certain pairs of food antigens.
However, due to the lack of convincing scientific evidence to support eventual mechanisms of detrimental action of foodspecific IgG on patients with IBS and the possible deprivation of valuable nutrients due to elimination diet, which might deepen the complaints of the patients, we accept the opinion of some organizations, such as American Academy of Allergy, Asthma and Immunology (AAAI), the Canadian Society of Allergy and Clinical Immunology (CSACI) and the European Academy of Allergy and Clinical Immunology (EAACI) recommending more investigations and caution in using the results for diagnosis [9].
CONCLUSION
The serological determination of specific antibodies (IgG) against different food antigens may be beneficial to all individuals who are suffering from food intolerance, including patients with IBS due to the limitations of skin tests and elimination diets. However, we should use these test with caution.
ACKNOWLEDGEMENT
The study was supported by Grant funding of Sofia University - Grant project 80-10-160/25. 04. 2018, Sofia University, Medical faculty, Sofia.
CONFLICT OF INTERESTS
The authors declare no conflict of interest.
REFERENCES
- Choung RS and Talley NJ. (2006). Food Allergy and Intolerance in IBS. Gastroenterology & Hepatology. 2(10): 756- 760.
- Atkinson W, Sheldon TA, Shaath N, Whorwell PJ, et al. (2004). Food elimination based on IgG antibodies in irritable bowel syndrome: a randomised controlled trial. Gut. 53(10): 1459-1464.
- Drisko J, Bischoff B, Hall M and McCallum R. (2006). Treating irritable bowel syndrome with a food elimination diet followed by food challenge and probiotics. J. Am. Coll. Nutr. 25(6): 514-522.
- Zar S, Benson MJ and Kumar D. (2005). Food-specific serum IgG4 and IgE titers to common food antigens in irritable bowel syndrome. Am J Gastroenterol. 100(7): 1550- 1557.
- Zar S, Mincher L, Benson MJ and Kumar D. (2005). Foodspecific IgG4 antibodyguided exclusion diet improves symptoms and rectal compliance in irritable bowel syndrome. Scand J Gastroenterol. 40(7): 800-807.
- Zeng Q, Dong SY, Wu LX, Hong Li, et al. (2013). Variable food-specific IgG antibody levels in healthy and symptomatic Chinese adults. PLoS ONE. 8(1): e53612.
- Ligaarden SC, Lydersen S and Farup PG. (2012). IgG and IgG4 antibodies in subjects with irritable bowel syndrome: a case control study in the general population. BMC Gastroenterol. 12: 166.
- Kvehaugen AS, Tveiten D and Farup PG. (2018). Is perceived intolerance to milk and wheat associated with the corresponding IgG and IgA food antibodies? A cross sectional study in subjects with morbid obesity and gastrointestinal symptoms. BMC Gastroenterol. 18(1): 22
- AAAAI support of the EAACI Position Paper on IgG4. Position Statement. 2010.