Information Links
Related Conferences
Previous Issues Volume 7, Issue 1 - 2023
Nails Changes and Disorders in Elderly Libyans
Elfaituri Safa Suleman*
Dermatology Department, Medical faculty, Benghazi University, Libyan Arab Jamahiriya
*Corresponding author: Dr. Safa Suleman Elfaituri, Dermatology Department, Medical faculty, Benghazi University, Libyan Arab Jamahiriya; Email: [email protected].
Received Date: May 02, 2023
Published Date: May 15, 2023
Citation: Elfaituri SS. (2023). Nails Changes and Disorders in Elderly Libyans. Mathews J Dermatol. 7(1):21.
Copyrights: Elfaituri SS. © (2023).
Abstract
Our nails change as we get older. Aging can affect color, contour, surface, thickness, growth rate, chemical composition and histology of the nail unit. Our aim was to study the frequency and spectrum of nail abnormalities in elderly Libyans attended dermatology outpatient clinic. One thousand patients of variable ages were subjected to onychologic study. Elderly patients constituted 13% of the total patients seen. Frequency of nail conditions among elderly was significantly higher (100%) than the other age groups (27%). All the elderly patients have at least one nail change because of ageing. Other conditions caused by infections (60%), trauma (26%), and tumors (3%) or associated with skin (18%) or systemic diseases (12%). The observed senile nail changes were longitudinal ridges (92%), brittle nails (19%), onychauxis (37%), onychocromia (86%), pincer nail (7%) and onychogryphosis (3%). Nail infection were tinea ungums (47%), chronic paronychia (9%) and periungual wart (3%). Though nail disorders are frequently asymptomatic, however they may cause pain and affect daily activities. Understanding the signs and symptoms of the aging nail and the associated diseases is important for better assessment, diagnosis and management of the onychologic disorder in the large and growing senile population.
Keywords: Nails, Old People, Nutritional Problems, Trauma, Infections, Diabetic, Chemotherapy, Breast Cancer.
BACKGROUND AND OBJECTIVES
Nail abnormalities are frequently seen in old people, these occur as a result of chronological ageing as well as in association with disorders affecting the elderly more commonly as impaired circulation, nutritional problems, trauma, infections, ultraviolet radiation and neoplasms. Nail involvement occurs also in association with cutaneous and systemic diseases. Nail abnormalities may affect any part of the nail unit including the matrix, nail bed, hyponychium, nail folds and nail plate [1-3]. They may be asymptomatic and only of cosmetic concern, however, they may cause pain, impair daily activities and may affect function and ambulation, with negative psychological impact and quality of life affection [1,4].
Although nail conditions are common among elderly population, they are often unnoticed. No information exists regarding nail disorders among the elderly population in Benghazi, Libya and there is a need to evaluate various nail diseases in our geriatric population.
This study aims at studying nail changes in Libyan elderly people to determine the frequency and spectrum of nail conditions due to aging and associated dermatologic or systemic disorders.
It would provide important data for general practitioners, dermatologists as well as geriatricians aiming to improve understanding of senile nail disorders.
MATERIALS AND METHODS
This prospective, cross-sectional study was done in dermatology department outpatient clinic at Jumhoria hospital over 2 years. One thousand patients of variable age groups (20-92 years) were selected randomly, irrespective of their presenting symptoms, and subjected to onychologic study. A history was elicited including the onset, progression and job and any environmental factor. Detailed fingers and toes nail examination as well as general examination of the skin and hair was done. KOH examination of nail clipping as well as nail biopsy were done in selected cases.
The patients were grouped into elderly group above 65 years and adult group (20-64 years) to compare frequency of nail involvement.
Nail conditions were classified into age related, infections, traumatic, neoplastic, inflammatory dermatological disease, and systemic disease related. The senile nail changes were classified into four categories including changes in color, contour, surface and thickness.The data were statistically analyzed using the computerized program SPSS.
RESULTS
One thousand patients of variable age groups were included. Elderly patients constituted 13% of the total patients seen. All the elderly patients have at least one nail change because of ageing frequency of nail changes among elderly (100%) was significantly higher (P < 0.001) than the other age groups (27%).
Among the elderly group, median age was 71 years, 40% of them were females and only 4% were of black race. Although many elderly patients were not aware of their nail problem, nail disease was the presenting complaint in only 9%.
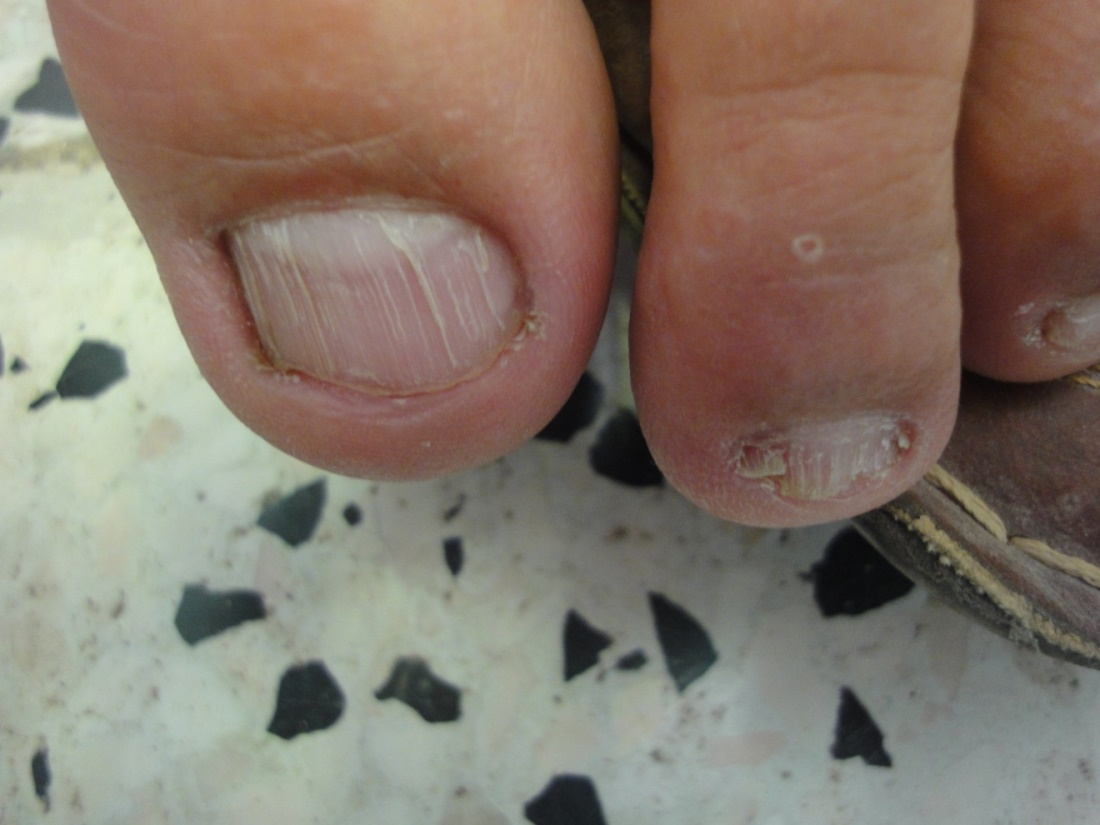
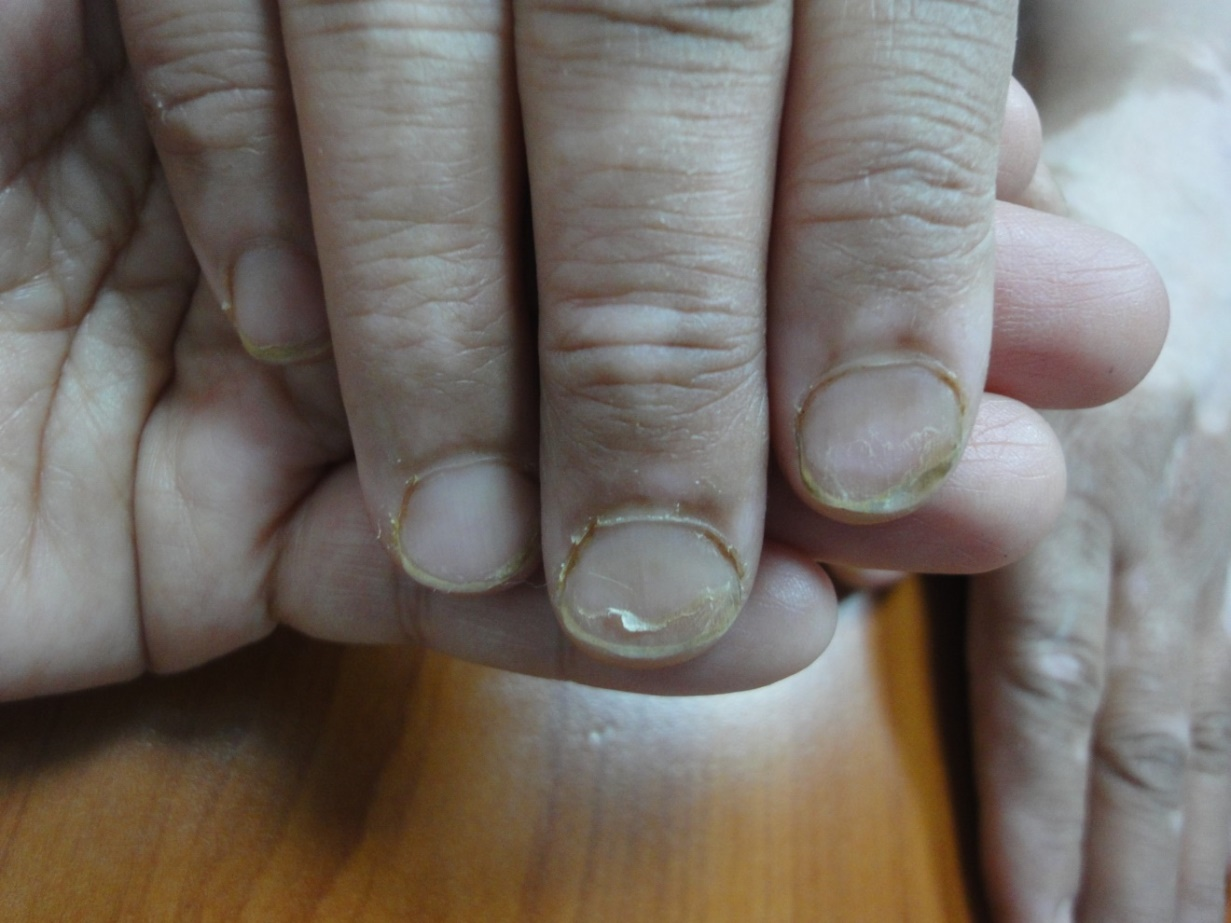
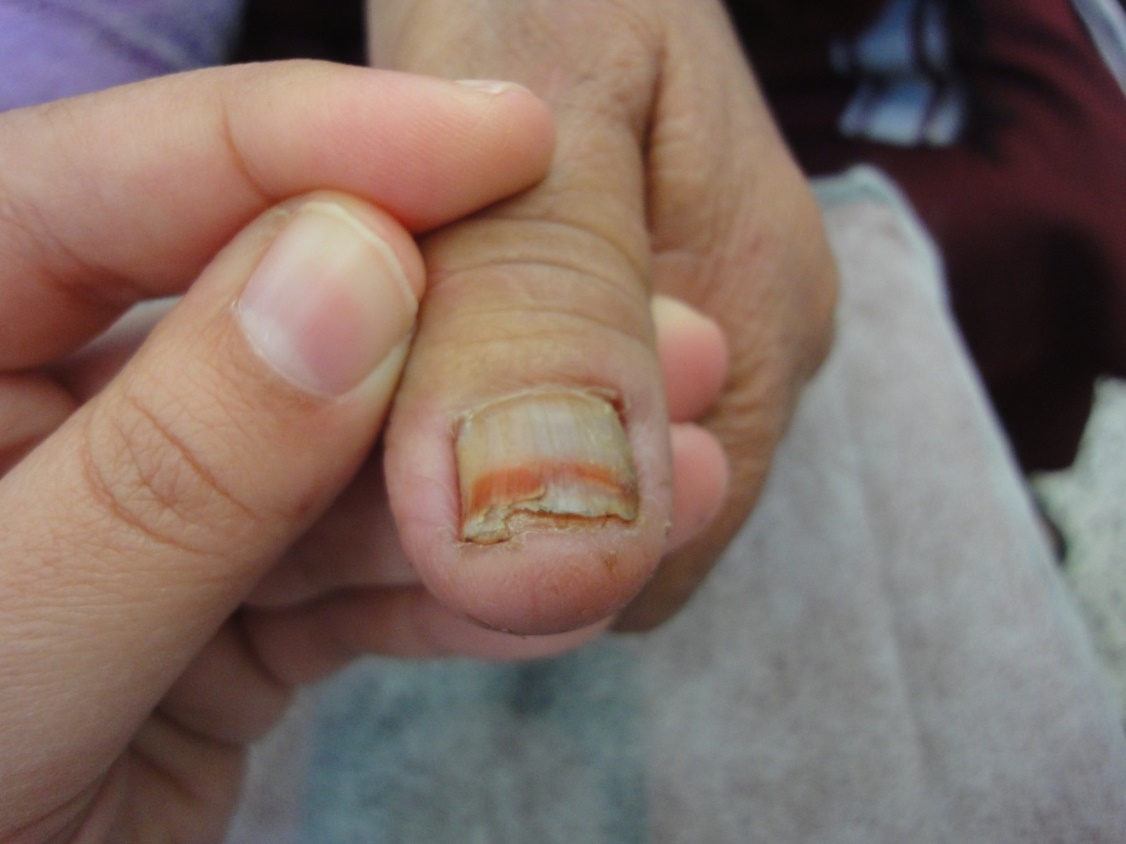
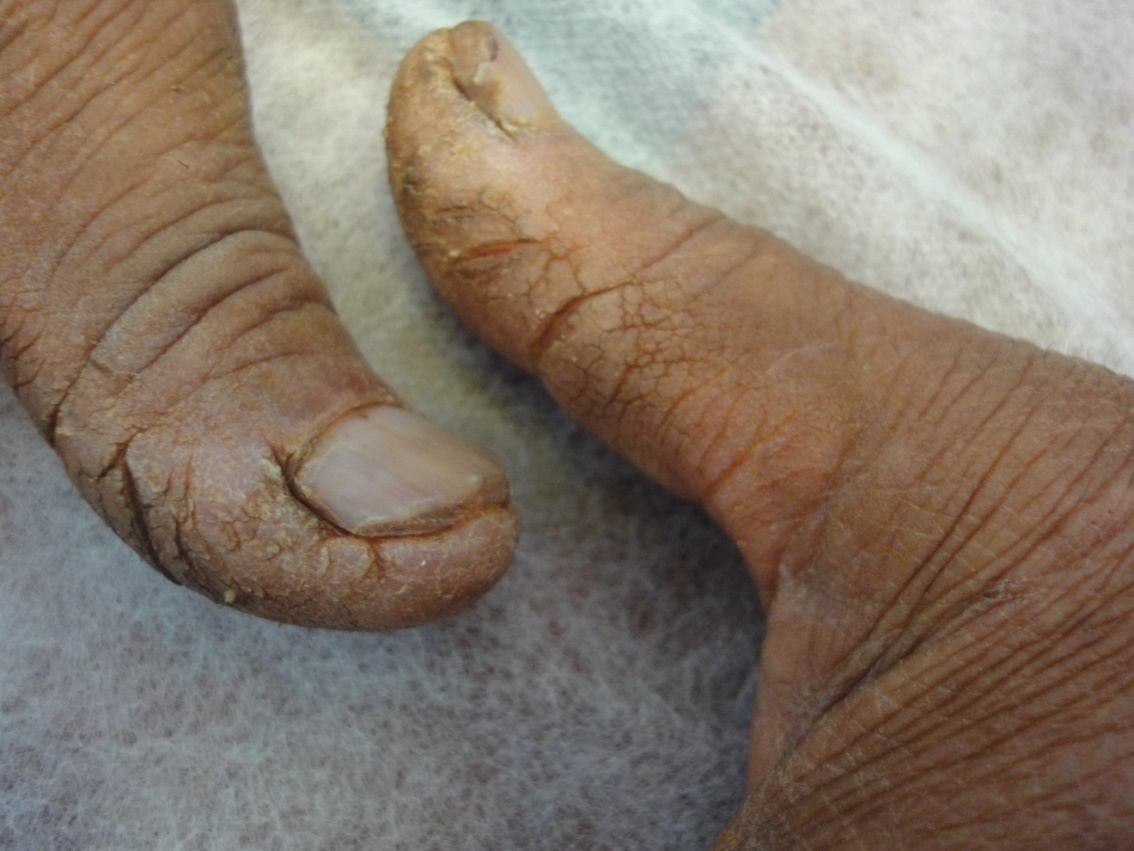
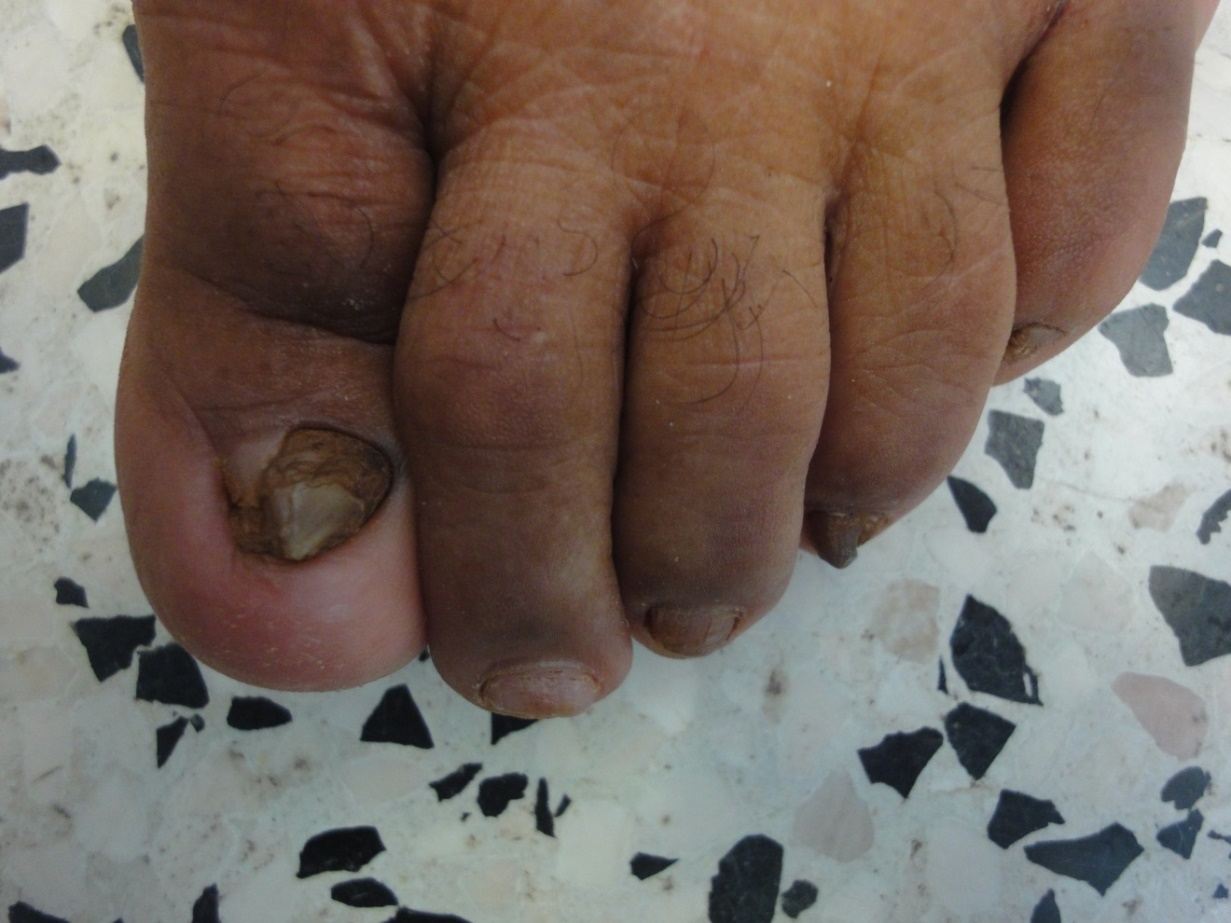
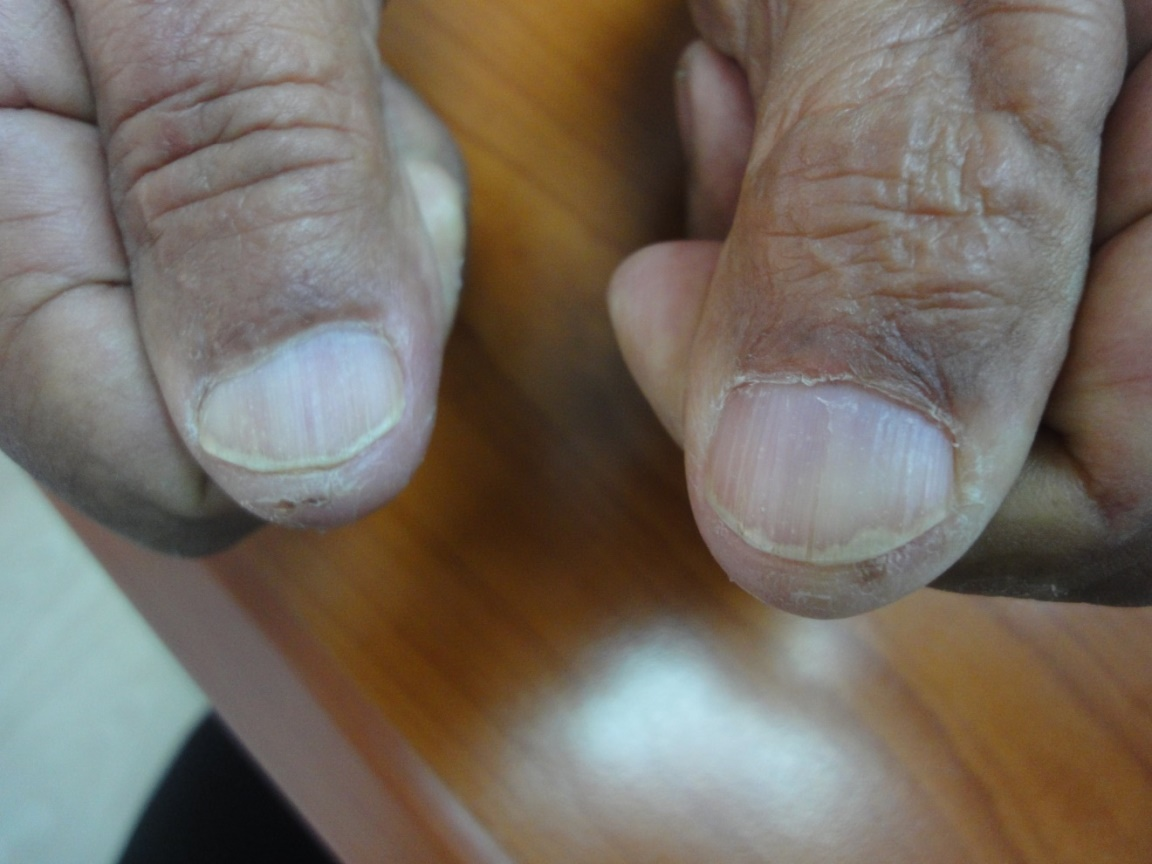
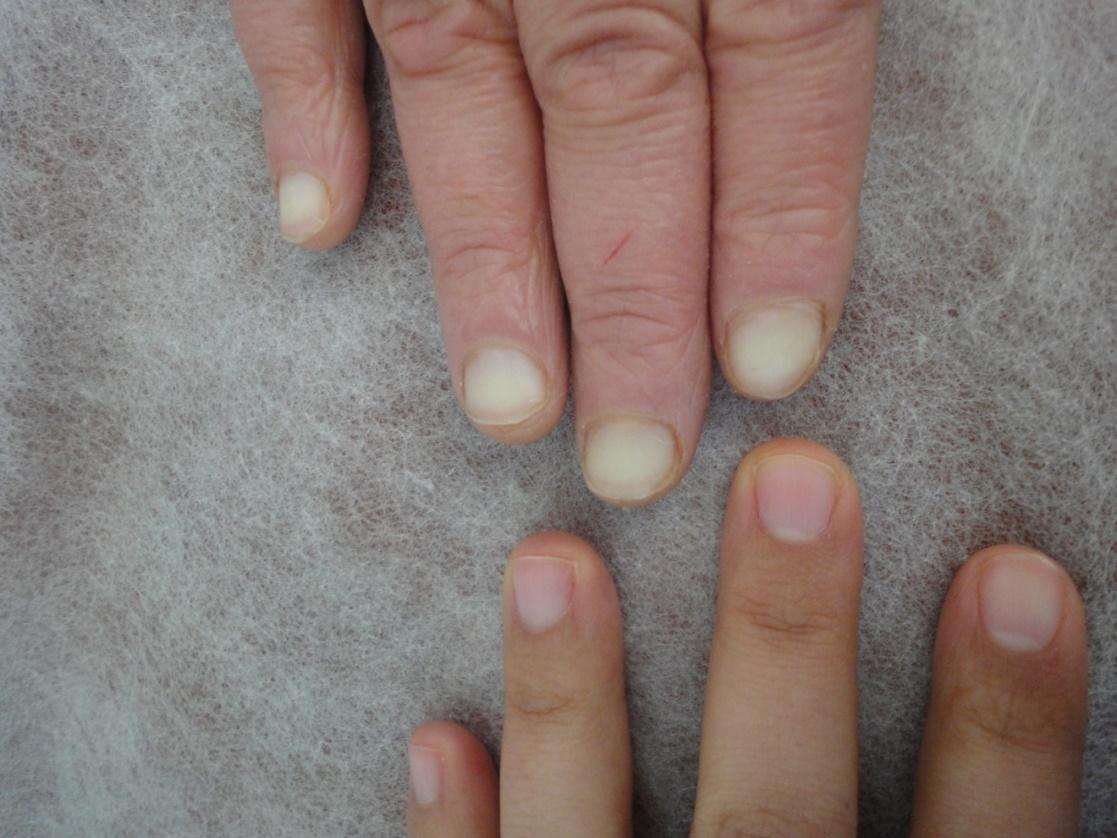
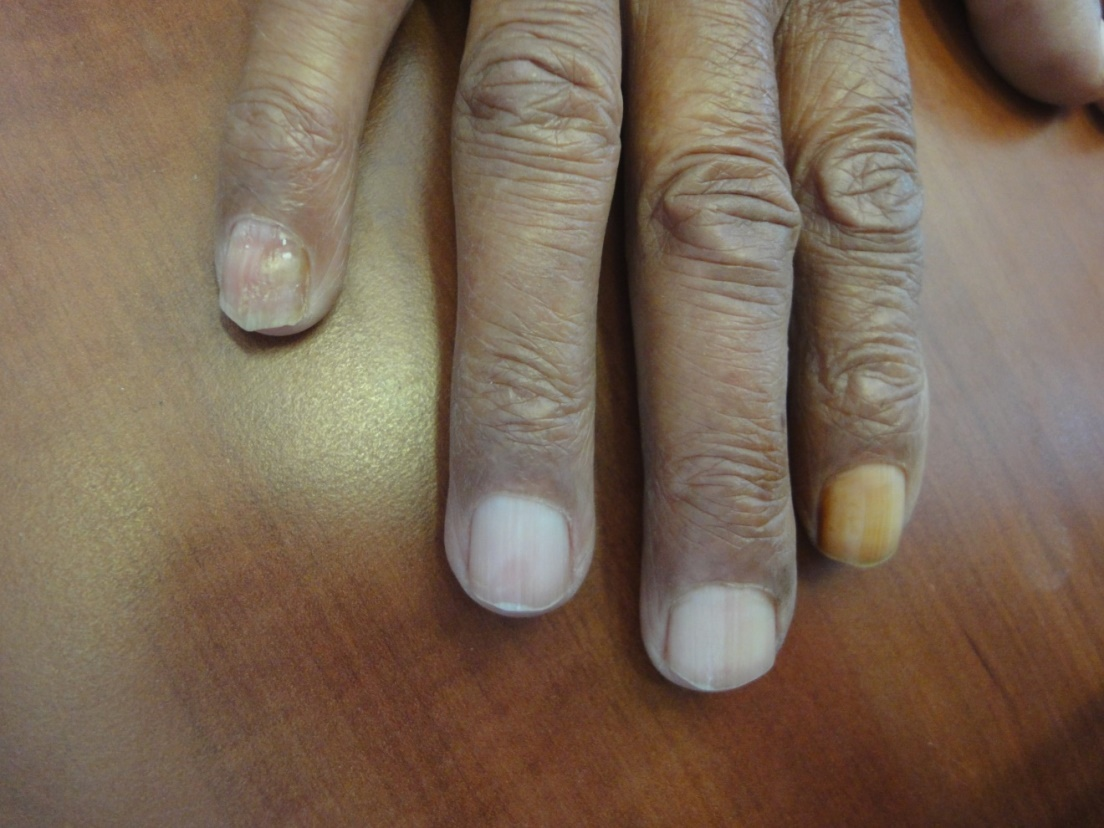
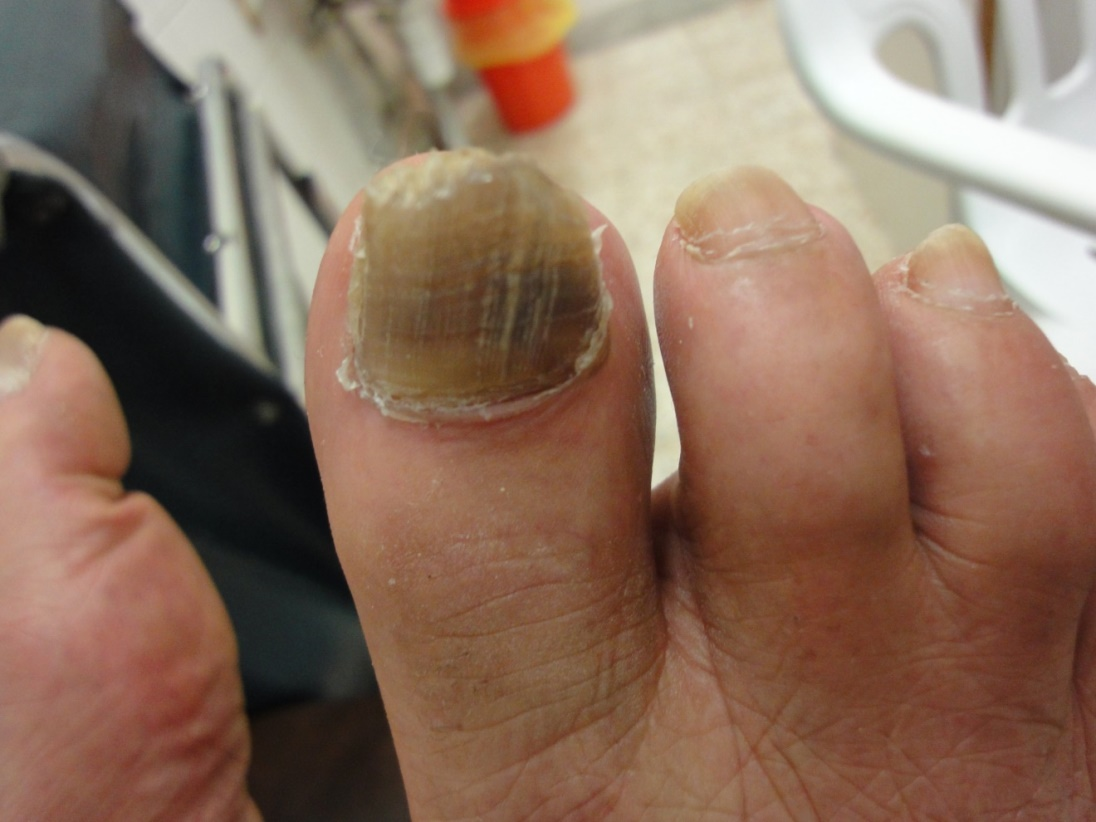
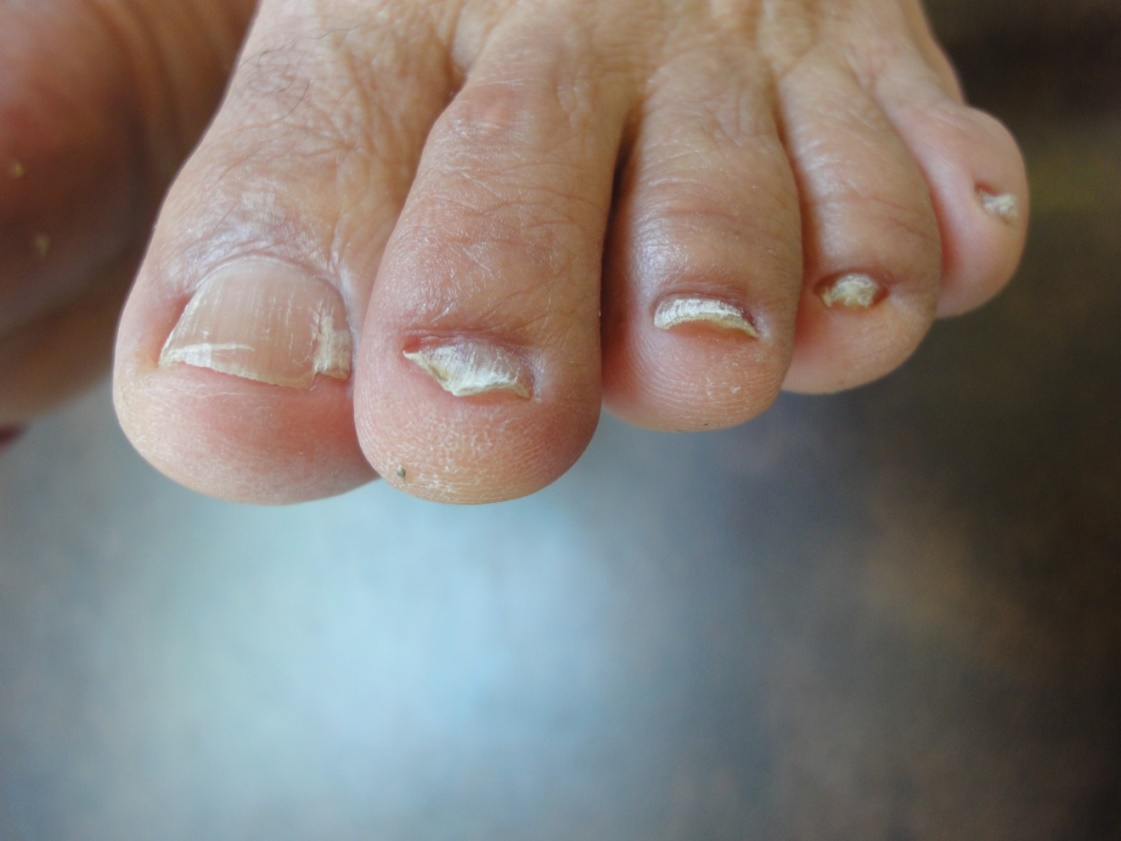
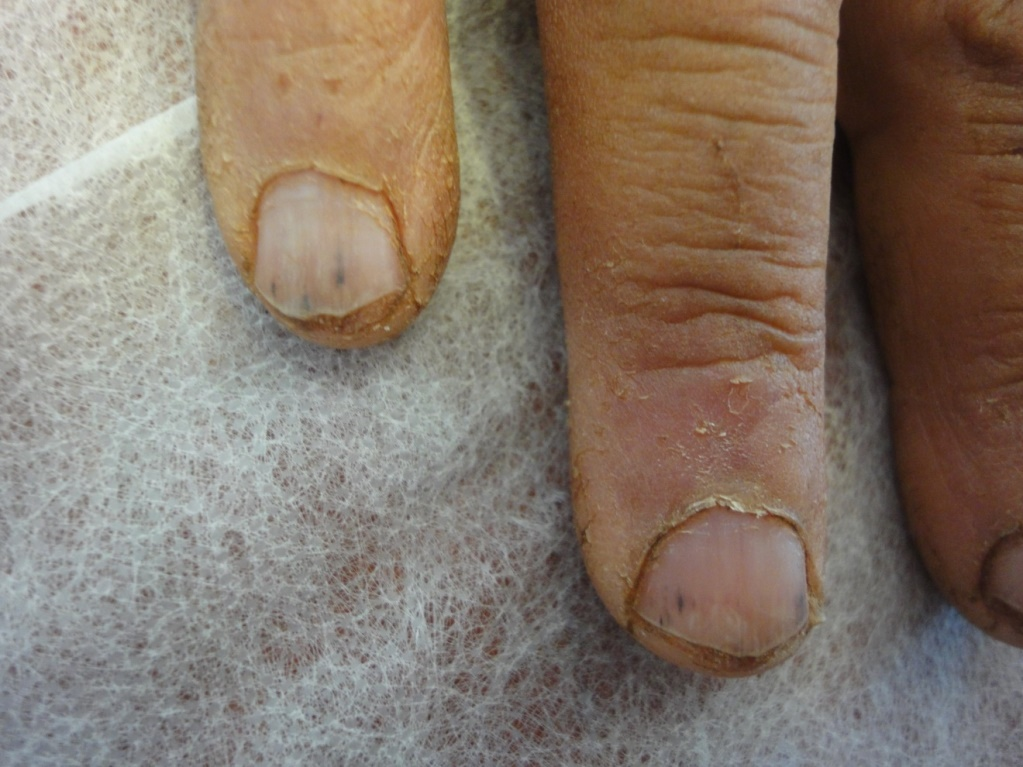
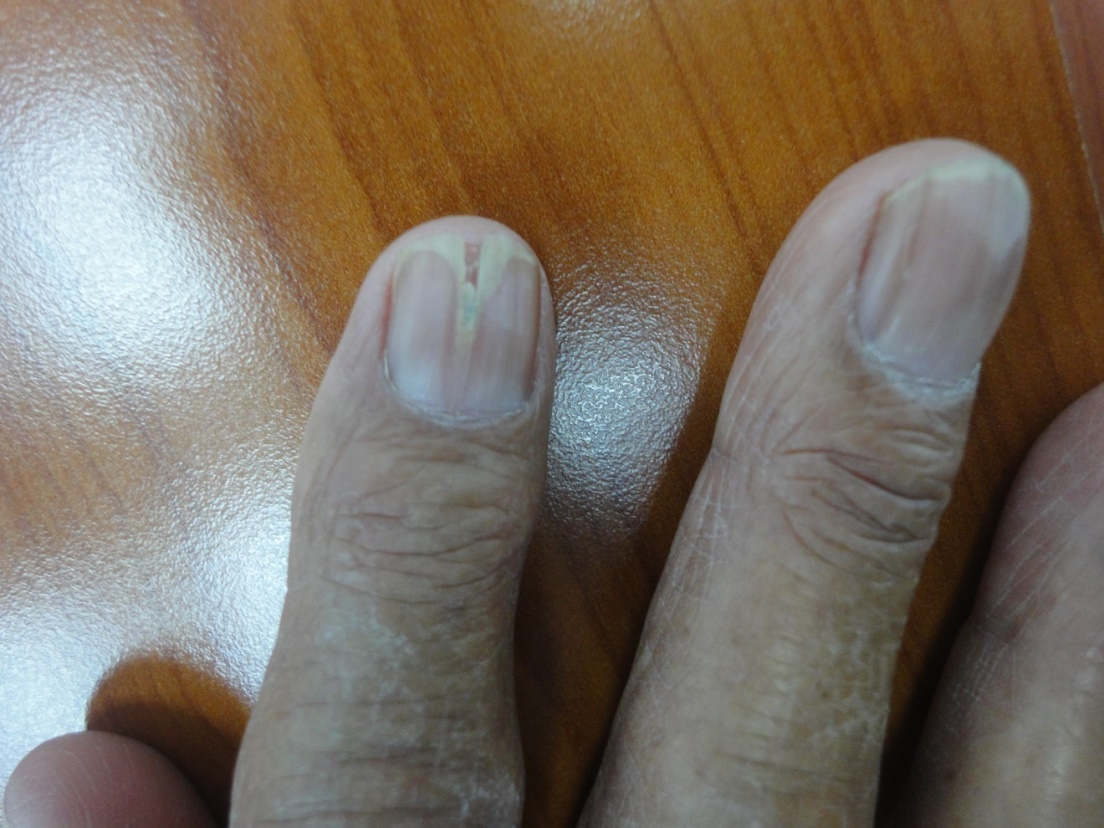
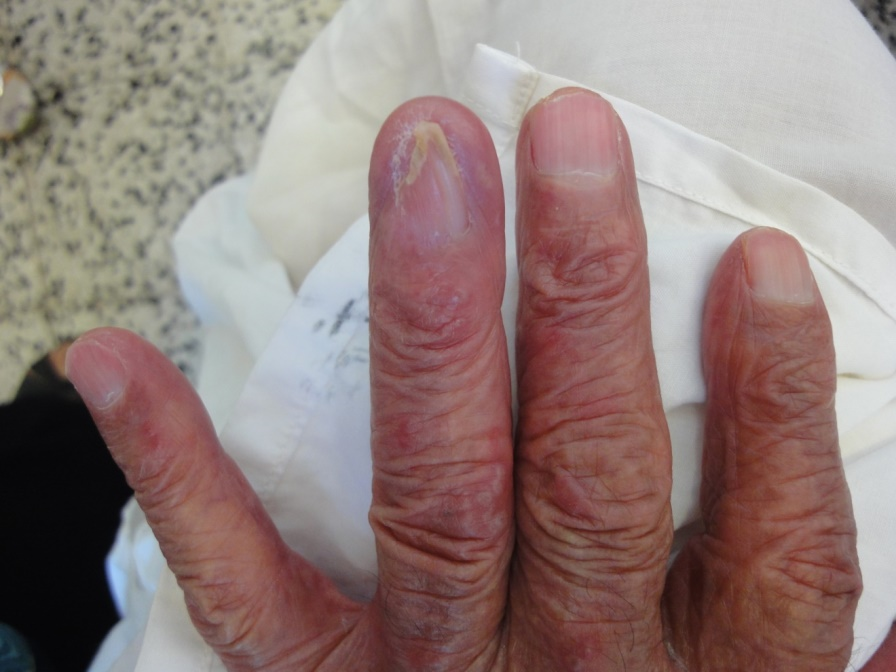
The observed senile nail surface changes in elderly were longitudinal ridges (92%), transverse ridges (25%), and lamellar split (10%) (Figure 1,2). Brittle nails were reported in19% (Figure 3). Increased nail thickness was observed in 37% (Figure 4), while thin nails in 8%.
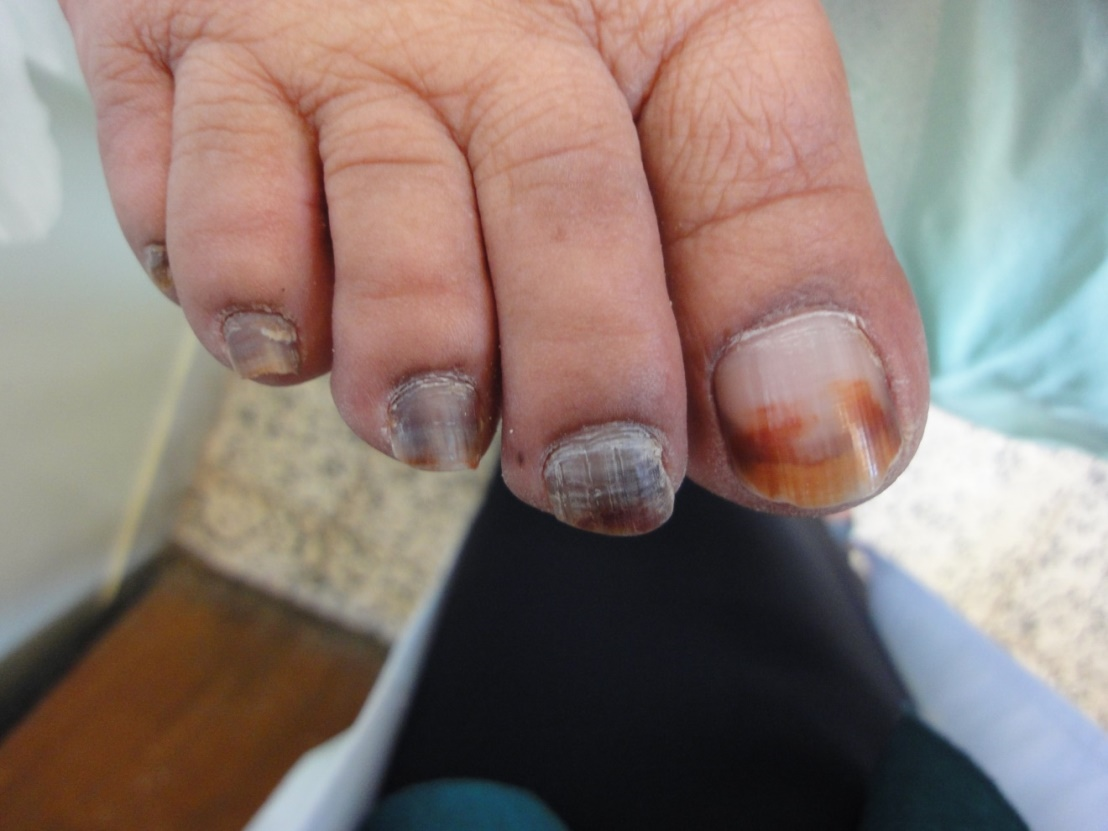
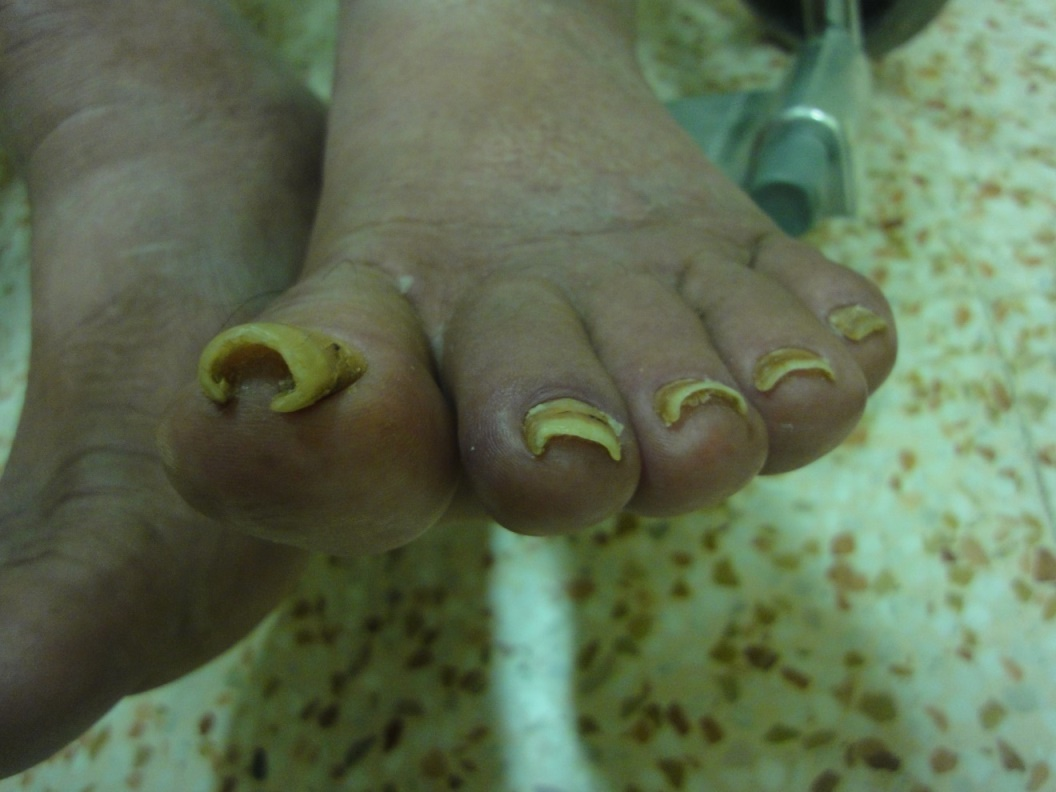
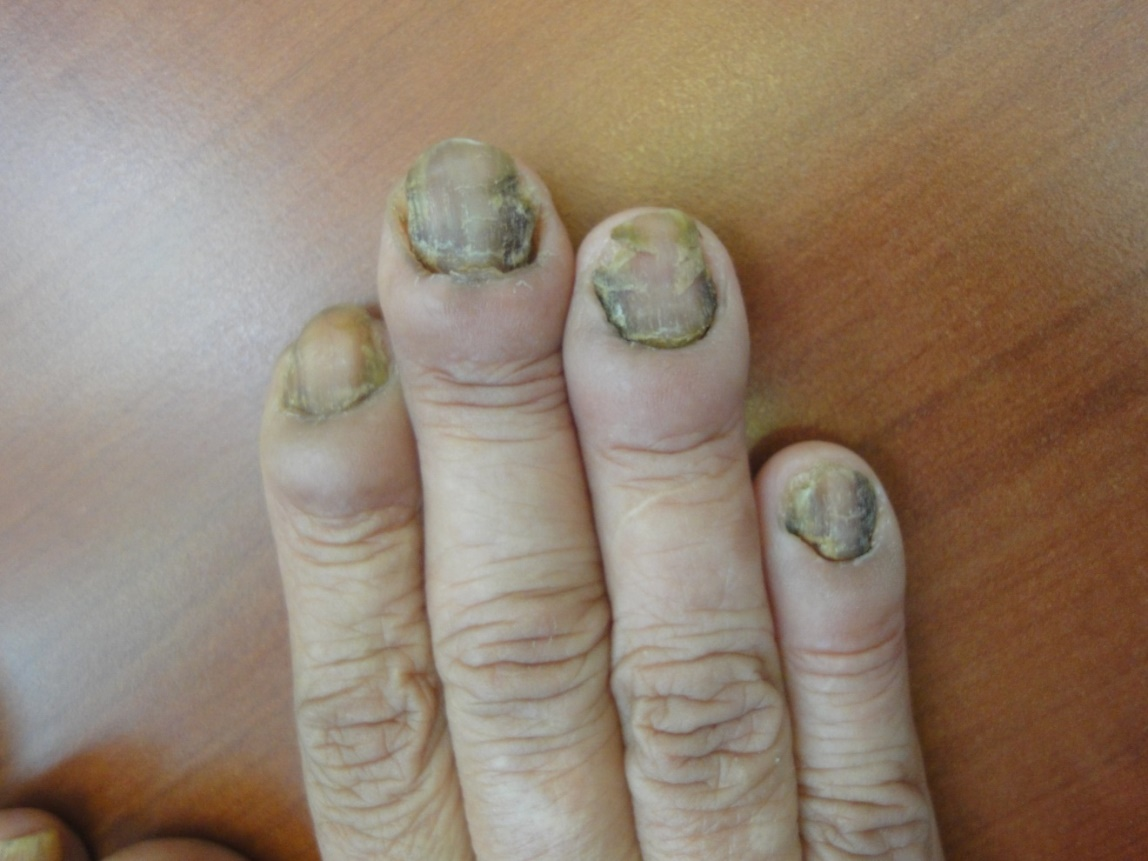
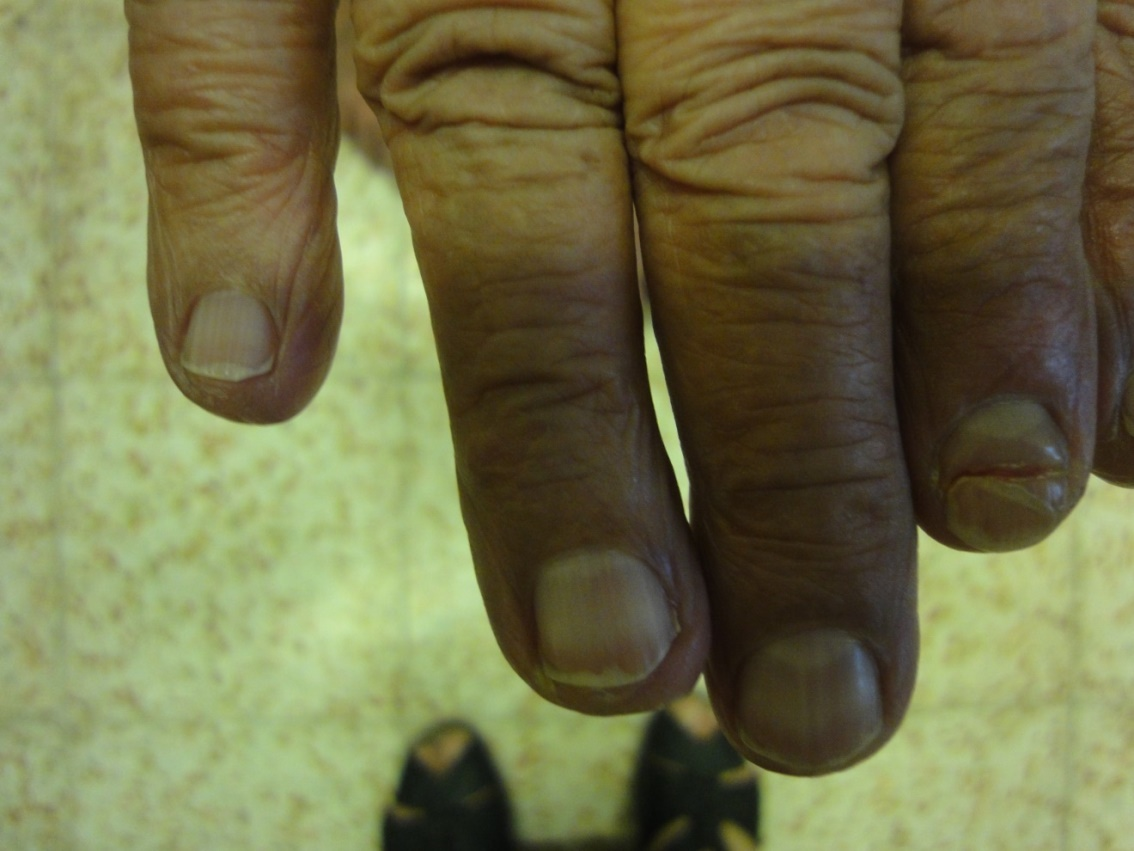
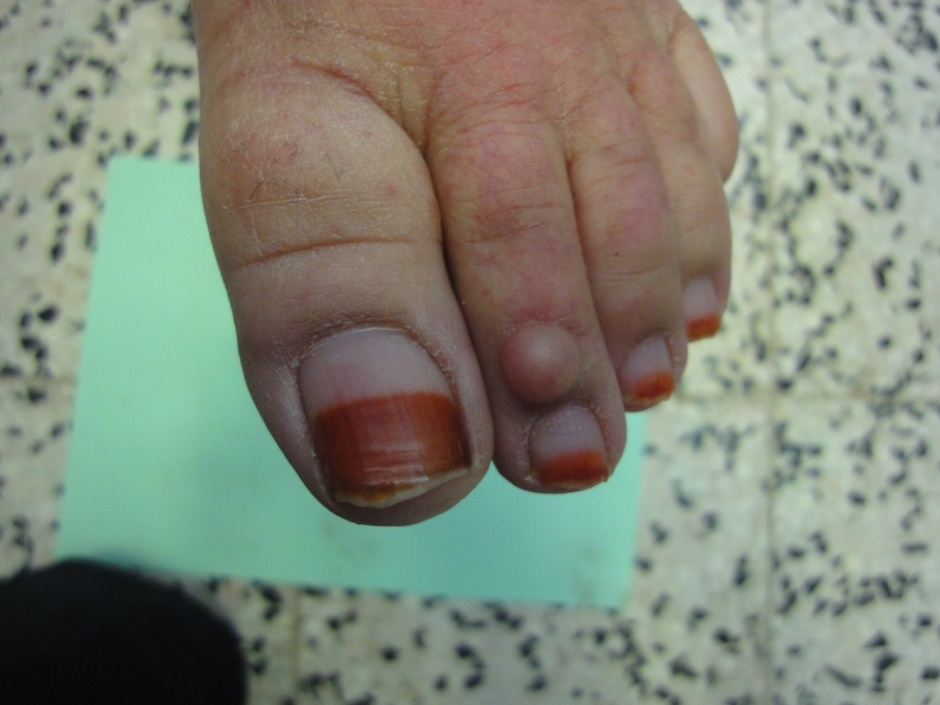
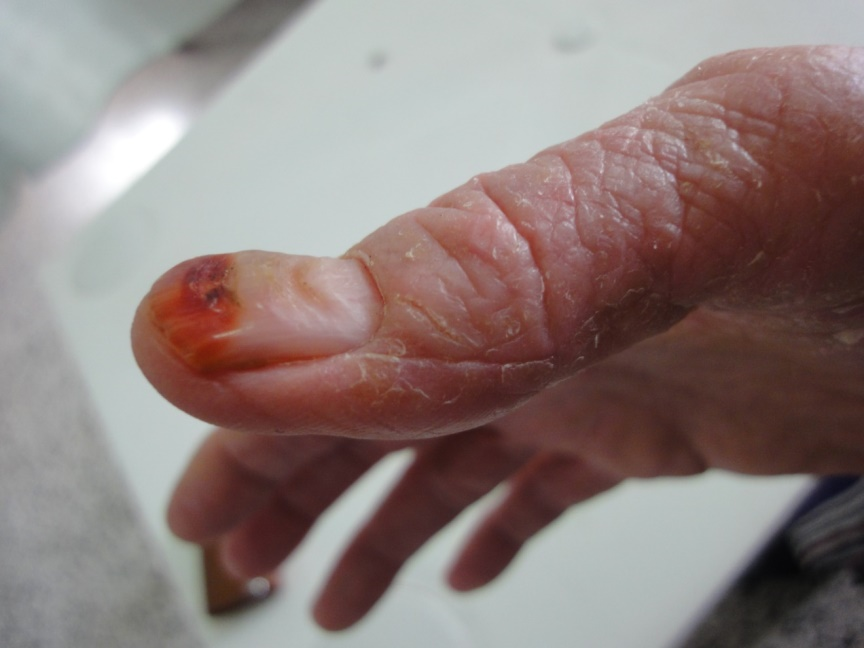
Regarding the abnormalities of nail color; 11% of our elderly females were having the traditional henna stains which partially obscure color of nail. Nearly quarter of the elderly (27%) have visible lunula, mostly it was seen in the thumb and first toe. Gray opaque nails were seen in 86%. Other nail color abnormalities include nicotine staining of nails (9%), melanonychia (8%) and blue cyanotic nail in one case. Nail color alterations due to mycotic or bacterial infection was observed in about half of the patients. Figures 5-12 show variable color changes in elderly nails. Pincer nail (7%), onychogryphosis (3%) (Figures 13-14) and platenychia (5%) constitute the main changes in nail contour. Onychoclavus was reported in one case (Figure 15).
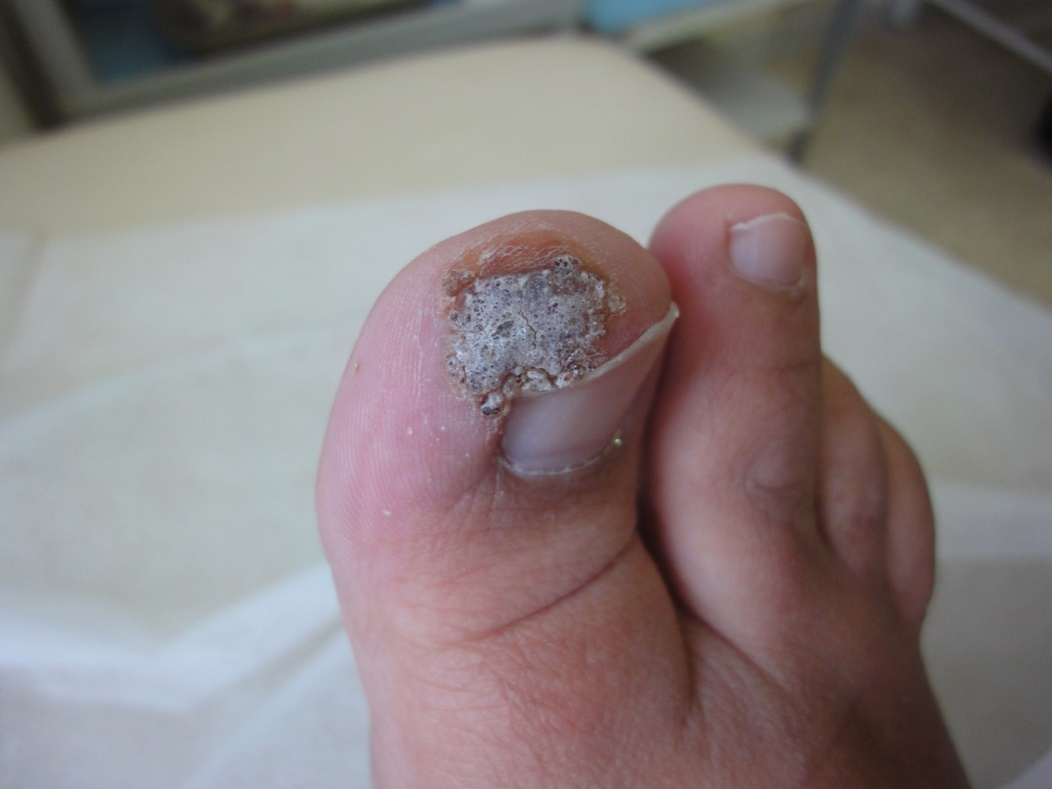
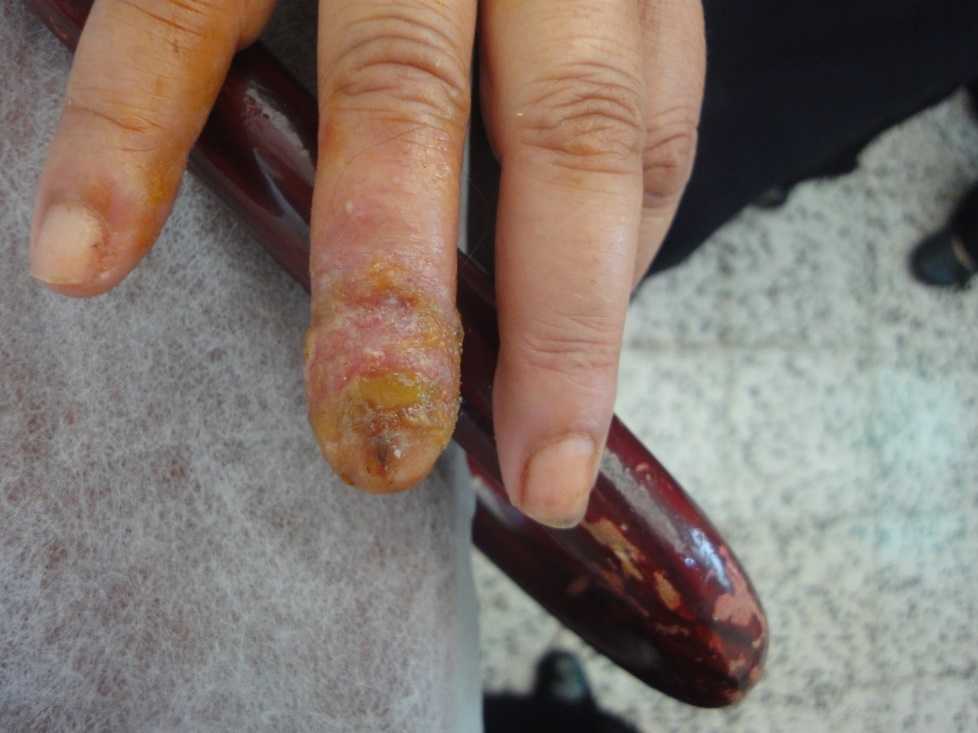
Tinea ungums was the main nail infection reported in this study (47%) (Figures 16a-c) whereas chronic paronychia was seen in 9% (Figure 17), periungual wart in 3% (figure 18) and nail loss associated with lepromatous leprosy (figure 19) was reported in one case.
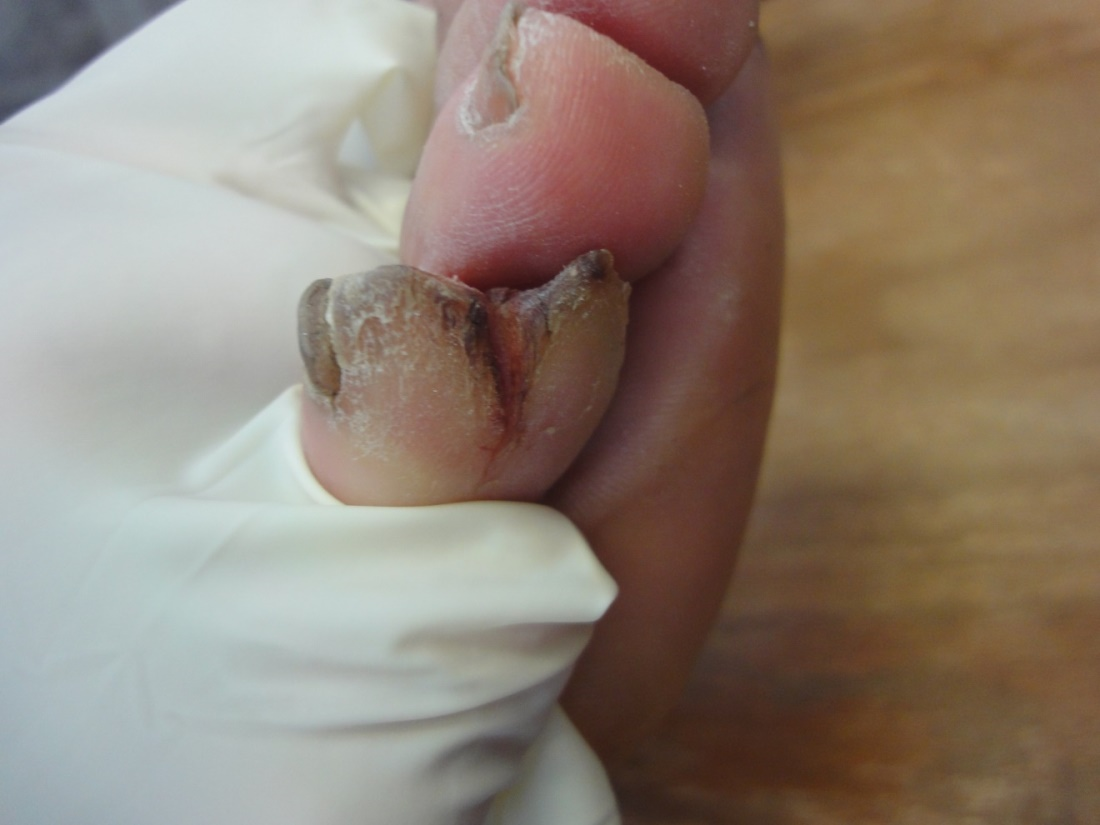
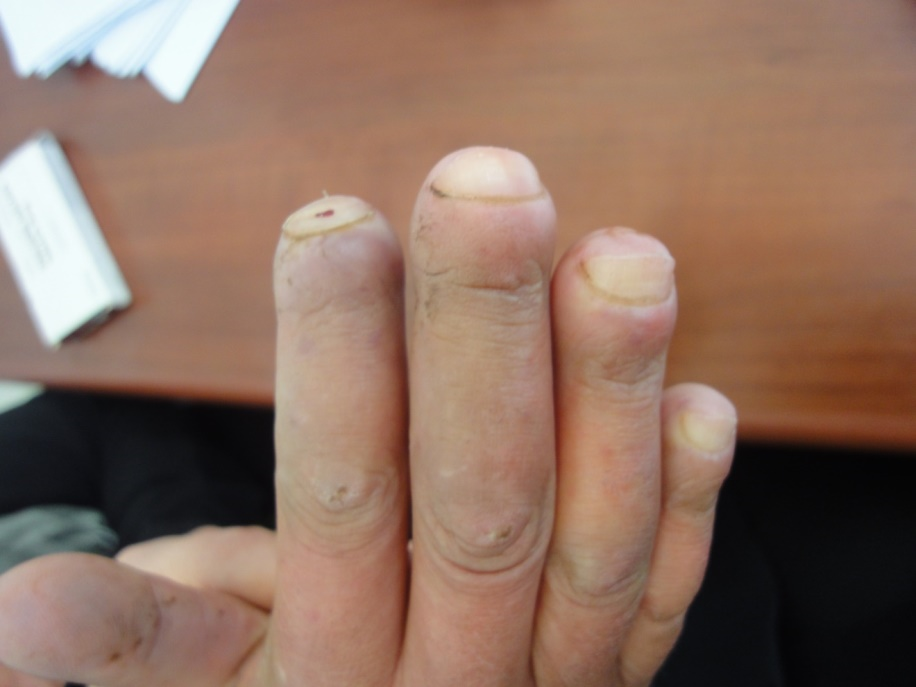
Traumatic nail disorders (26%) include splinter hemorrhage (12%), subungual hematoma (9%), in growing nails 3%, nail scaring and dystrophy (2%) and Beau′s lines (2%). Figures 20-25 show different traumatic nail conditions.
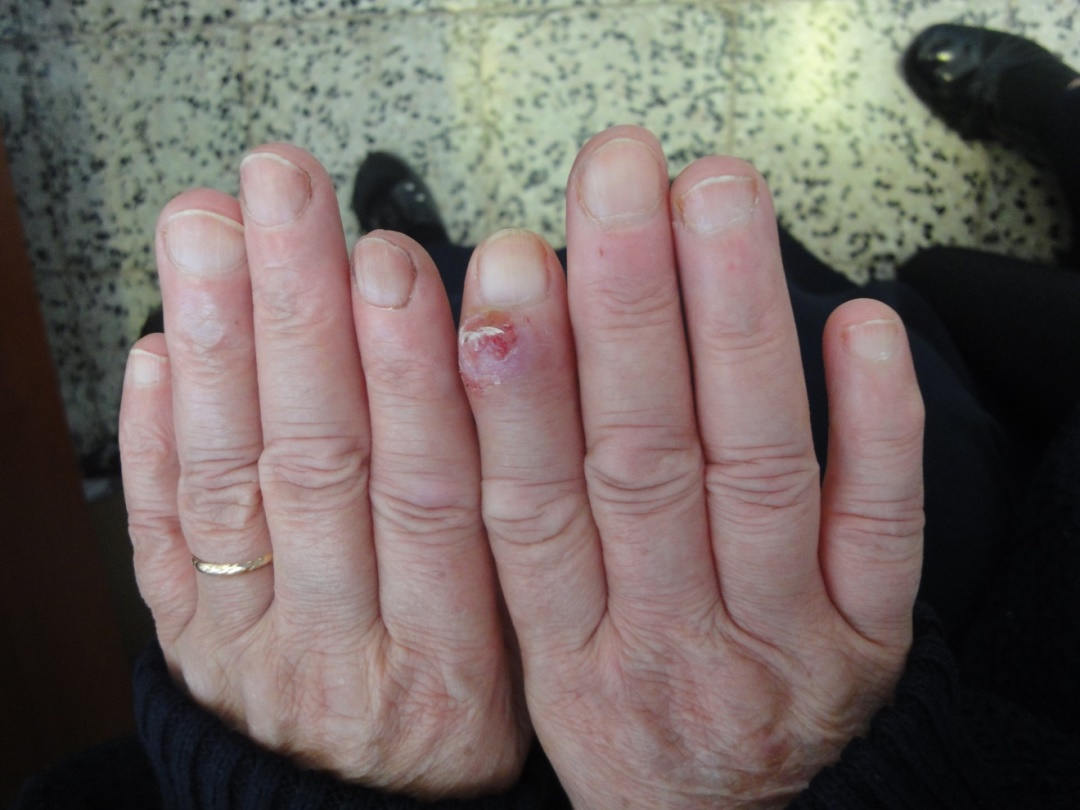
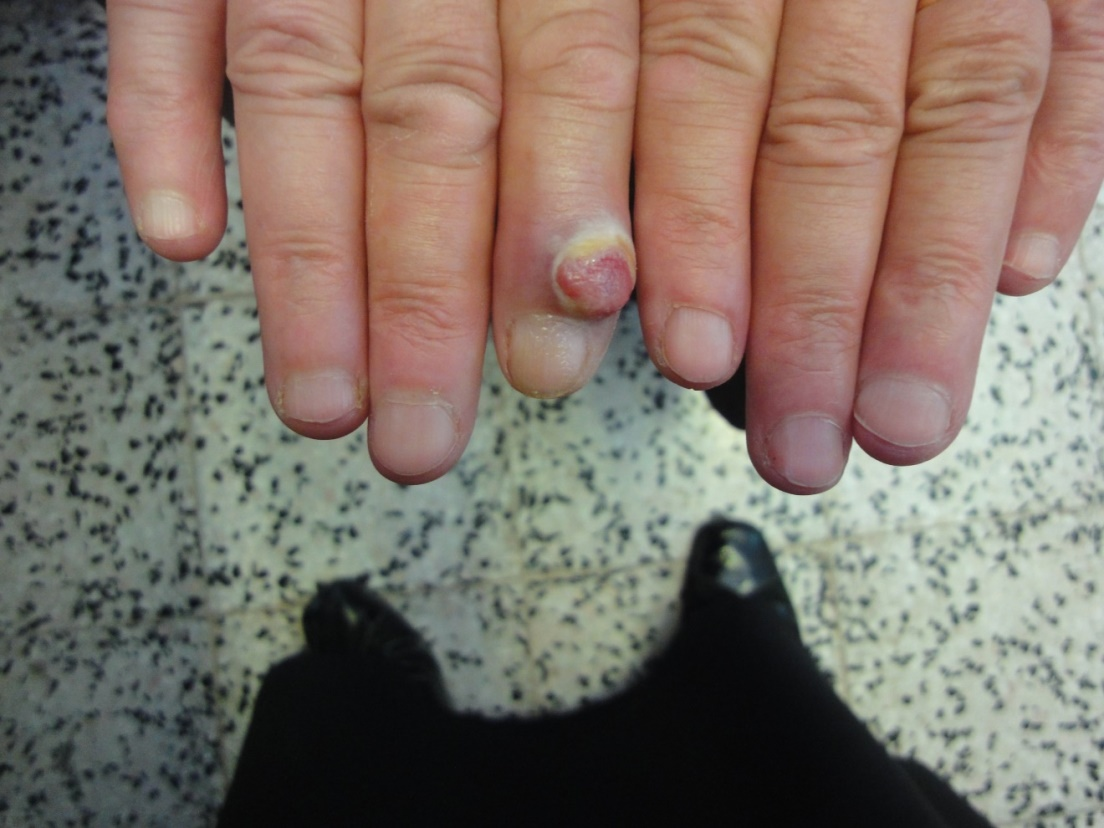
Regarding the benign neoplastic tumors of nail unit; pyogenic granuloma, digital myxoid cyst and acquired digital fibrokeratoma, each reported in single case. (Figure 26-28).
Squamous cell carcinoma was the only malignancy reported and it was seen in one patient only (Figure 29).
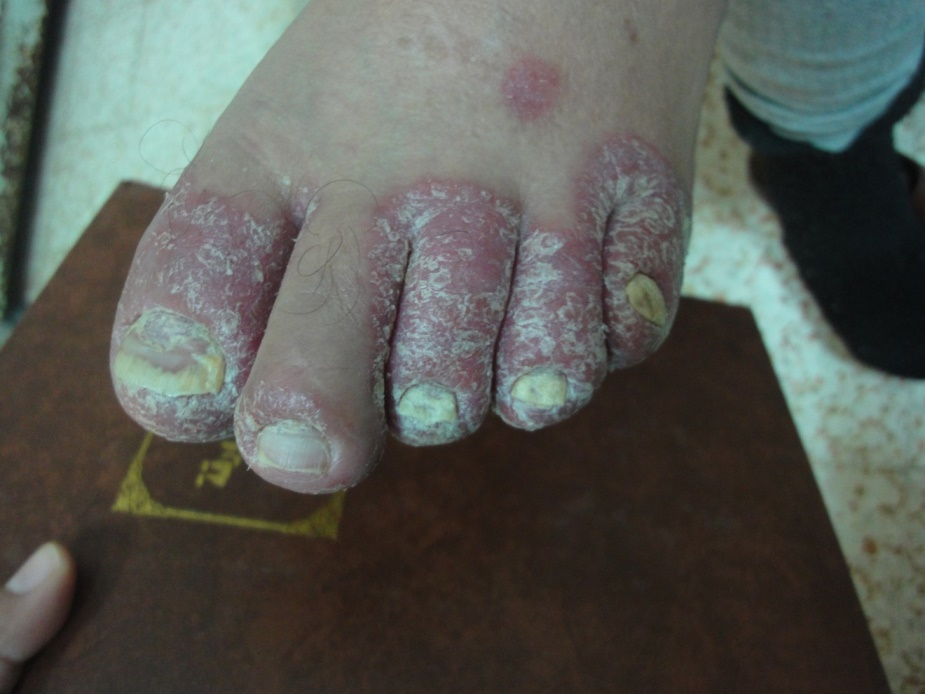
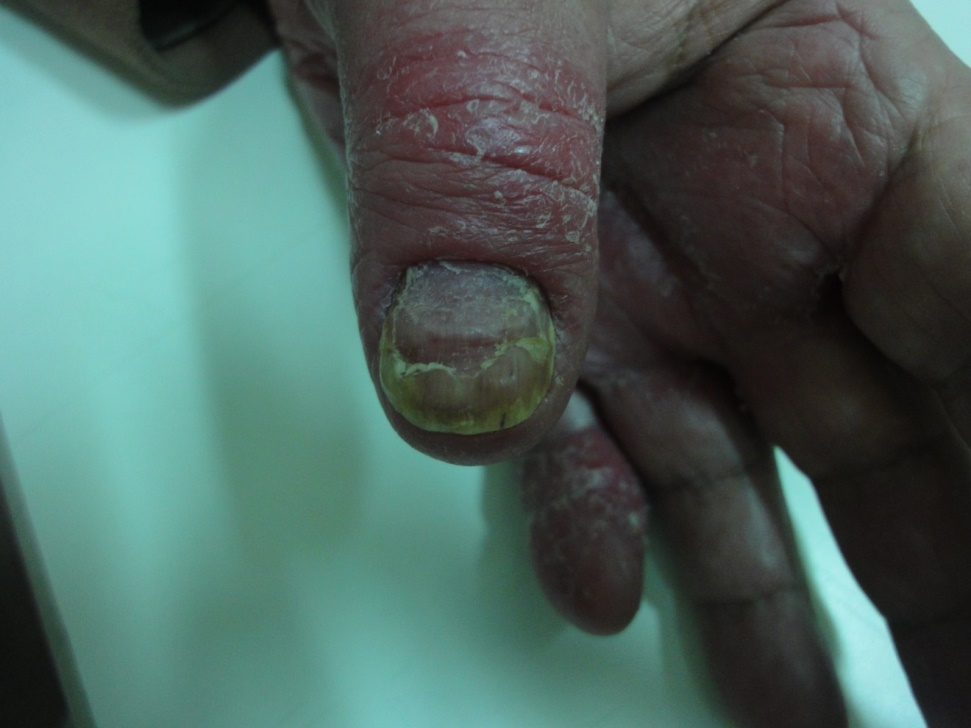
Nail changes were associated with inflammatory skin diseases were present in 18% including yellow discoloration, onycholysis, subungual hyperkeratosis, and nail pitting associated with psoriasis (5%) (Figure 30a-b). Transverse ridging associated with eczema (11%) (Figure 31) whereas nail changes including pterygium were associated with lichen planus in 2% (Figure 32).
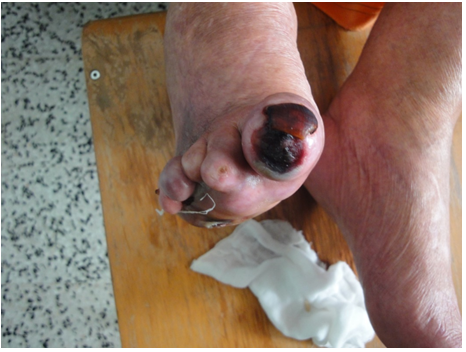
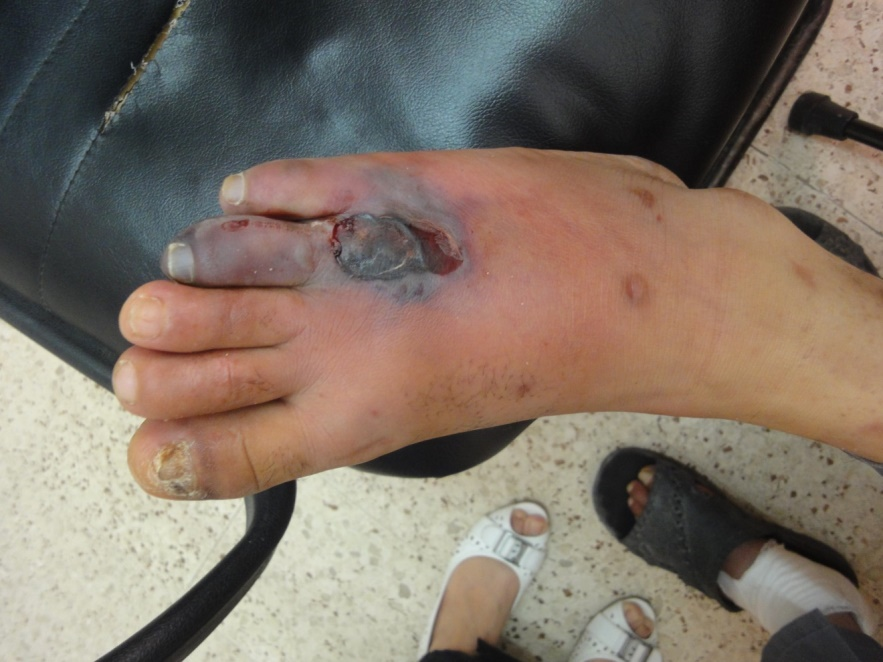
Nail changes in associated with systemic diseases was reported in 12% (Figures 33-38), these include diabetic ischemic changes in 5%, and anemia related koilonychias 3%. Leukonychia 7% including one case of Lindsay nail and Terry’s nail. Clubbing and pseuoclubbing each was observed in single case.
Figure 1. Superficial long striation (onychorrhexis) with brittle nails.
Figure 2. Flat nails with transverse splitting (Onychoschizia).
Figure 3. Brittle nail with lamellar splitting at distal nail plate
Figure 4-a. Thickening of the nail plate.
Figure 4-b. Onychauxis; localized nail hypertrophy.
Figure 5. Invisible lunula in gray opaque nails with traumatic onycolysis on left side.
Figure 6. leukonychia
Figure 7. Traditional Henna stain, obscuring assessment of nail color.
Figure 8. Nicotine staining of right index finger nail.
Figure 9. Longitudinal racial melanonychia.
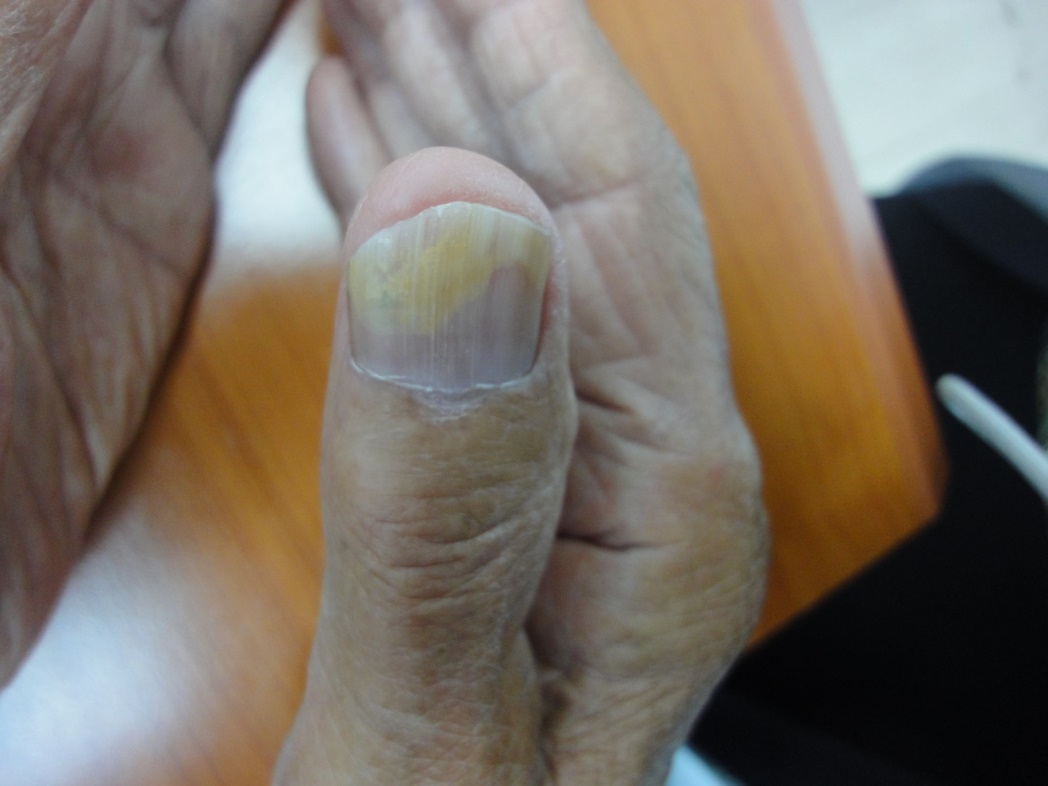
Figure 10. Fungal melanonychia.
Figure 11. Frictional melanonychia.
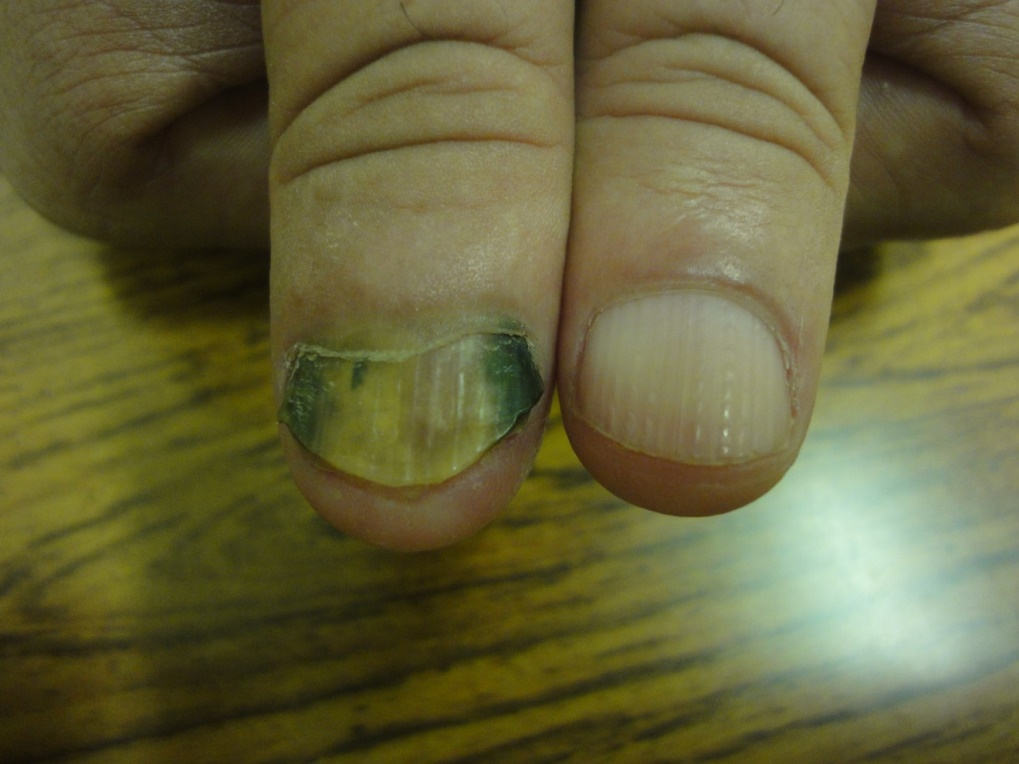
Figure 12. Pseudomonas infection of right thumb nail and longitudinal ridges with beading in left thumb nail.
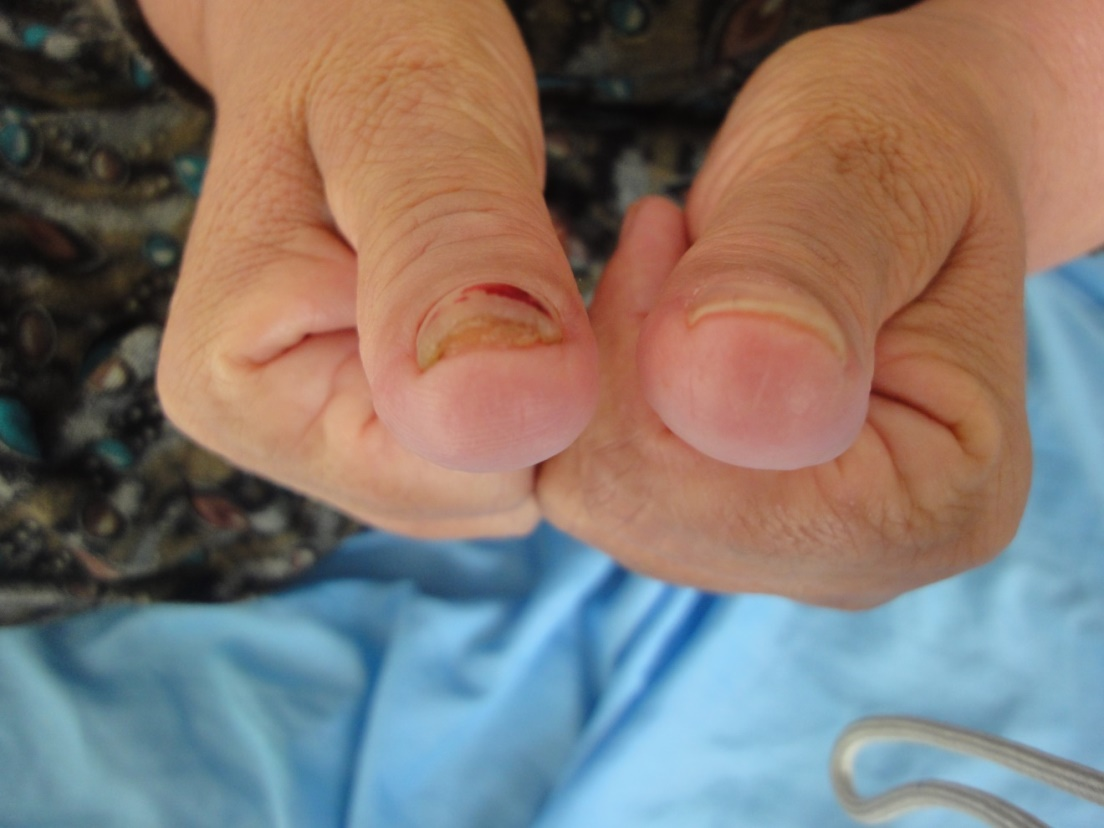
Figure 13. Pincer nails.
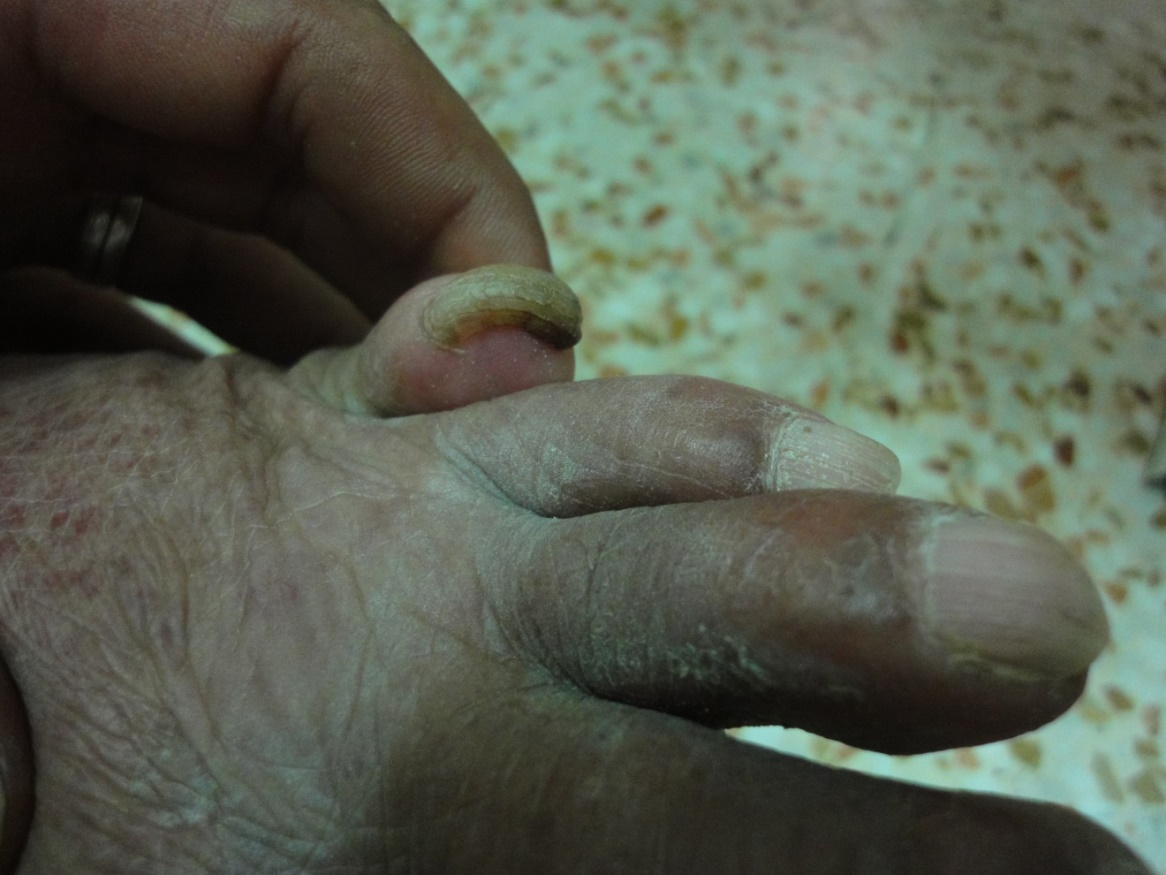
Figure 14. Onychogryphosis, a horn-like thickening of the nail plate.
Figure 15. Onychoclavus.
Figure 16-a. Onychomycosis, distal type.
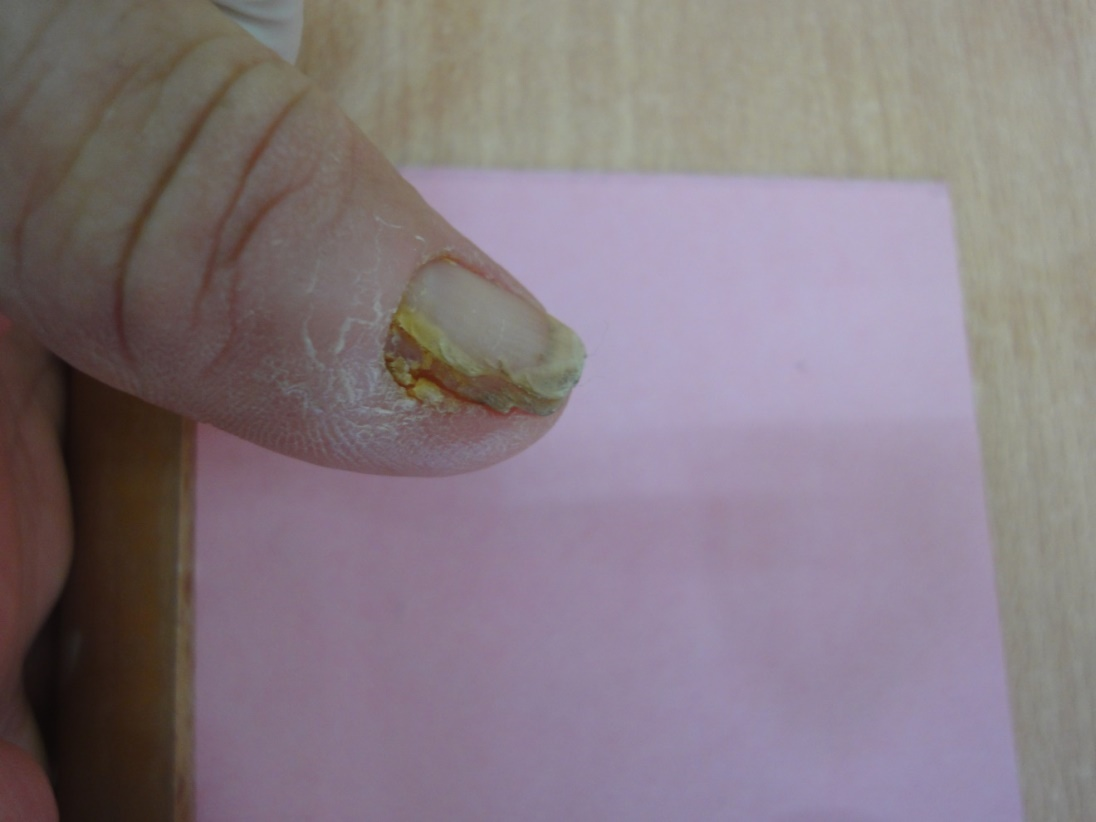
Figure 16-b. Lateral subungual onychomycosis.
Figure 16-c. Superficial white onychomycosis (Pseudoleukonychia) with koilonychias in second toe.
Figure 17. Chronic paronychia, candida and pseudomonas were isolated.
Figure 18. Periungual wart.
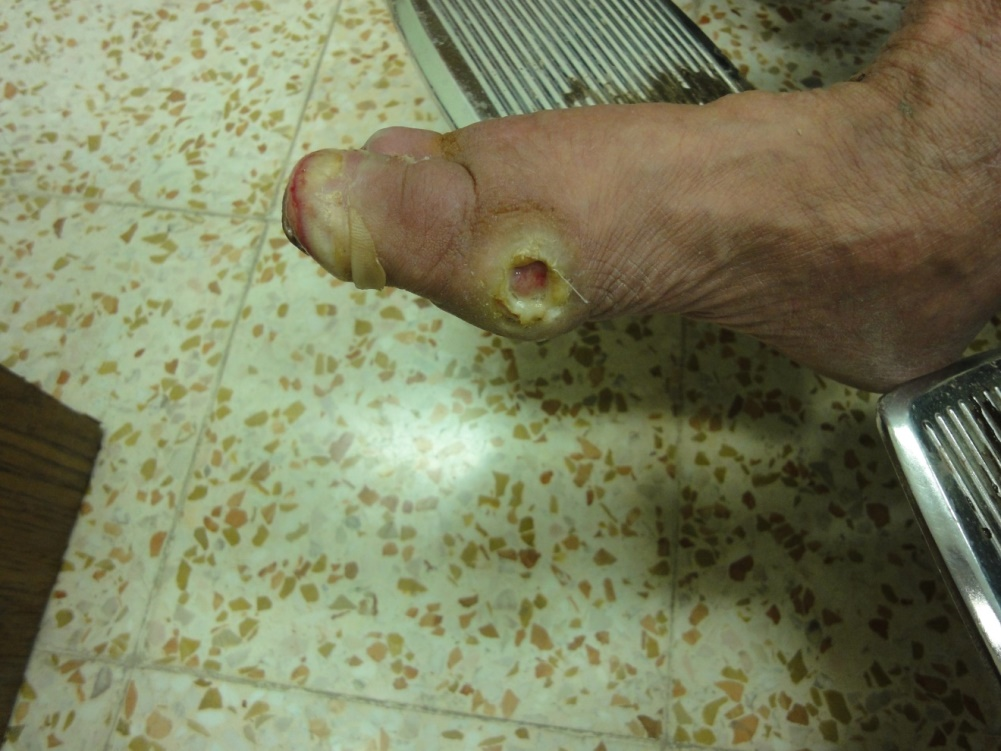
Figure 19. Nails loss with toe resorption in leprosy patient with neuropathy.
Figure 20. Traumatic splinter hemorrhage.
Figure 21. Subungual hematoma.
Figure 22. Ingrown nail.
Figure 23. A single Beau's line due to trauma.
Figure 24. Median nail dystrophy.
Figure 25. Post traumatic polynychia.
Figure 26. Myxoid cysts.
Figure 27. Pyogenic granuloma after cryotherapy, with pitting of nail plate.
Figure 28. Acquired digital fibrokeratoma
Figure 29. Squamous cell carcinoma.
Figure 30-a. Nail changes in psoriasis; Onycholysis, yellowish thick nails
Figure 30- b. Nail changes in psoriasis; onychomadesis.
Figure 31. Transverse grooving and cuticle loss in eczema.
Figure 32. Pterygium in lichen planus
Figure 33. Blue cyanotic right 4th toe secondary to ischemia in diabetic patient.
Figure 34. Nails in scleroderma; leukonychia with pseudoclubbing.
Figure 35. Leukonychia and clubbing in chronic liver disease.
Figure 36. Nail atrophy in advanced diabetic neuropathy.
Figure 37. Terry′s nails with white color proximally and pink distally in diabetic patient
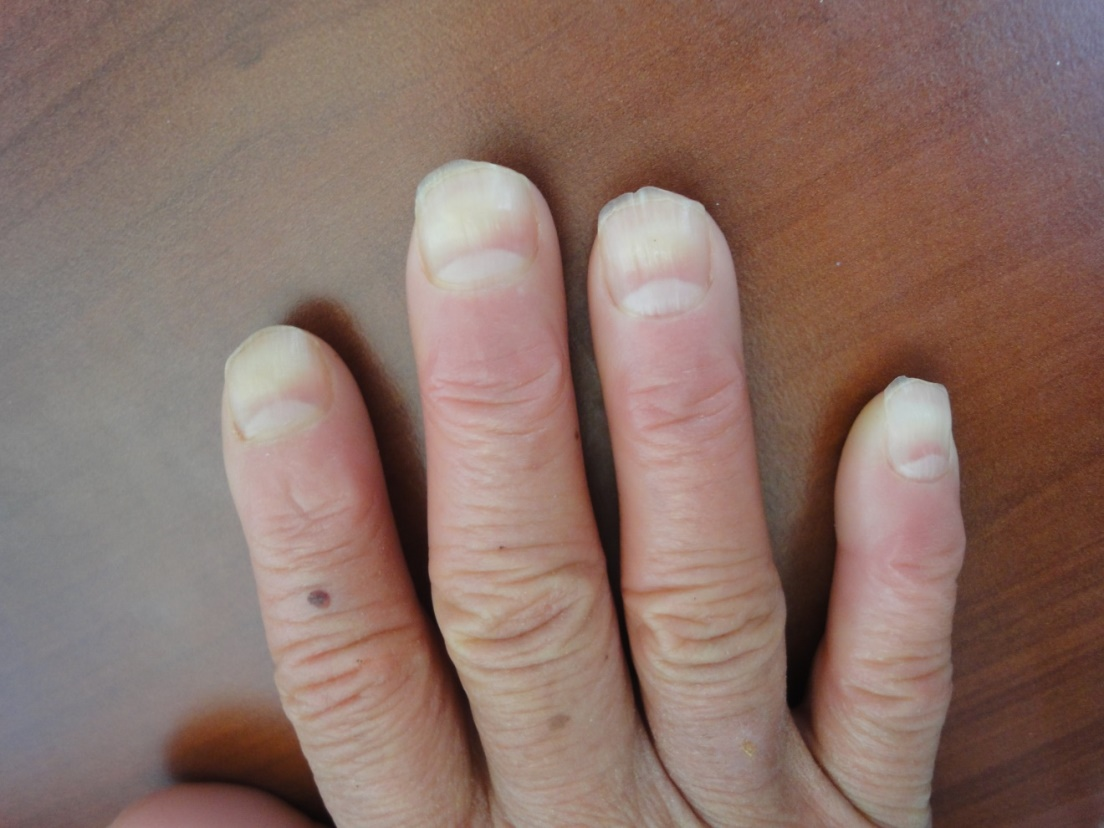
Figure 38. Macro lunula, leukonychia and acral erythema in a patient receiving chemotherapy for breast cancer
DISCUSSIONS
Nail conditions are common in the geriatric population, aging associated impaired peripheral circulation, susceptibility to infection, defective biomechanics are important contributing factors. Concurrent dermatological and systemic diseases, as well as their treatments may affect the nails. With aging, the rate of growth, chemical composition, color, contour, surface and thickness of the nail change [3,4].
The calcium contents of the senile nails are increased while the iron contents are decreased. Keratinocytes of the nail plate are increased in size with prominent remnants keratinocyte nuclei. The nail bed dermis have thickened blood vessels and degenerated elastic fibers [5,6].
Nail conditions related to aging were seen in all patients, longitudinal ridges were the most observed surface nail changes (92%), they present as superficial striations (onychorrhexis) or deep beaded ridges [7]. They occur commonly with aging because of the abnormalities in turnover rate of nail matrix with subsequent changes in epithelial growth and keratinization. Decrease vascularization associated with arteriosclerosis is a contributing factor for development of senile surface changes. Elderly nails may be rough (trachyonychia) and may have transverse fissuring and splitting (Onychoschizia) and lamellar splitting at distal nail plate. The splitting are caused by adhesion loss between the corneocytes of the nail plate [8,9]. In our study, transverse ridges were seen in 25%, and lamellar split in 10%.
Brittle nails are a common finding in the elderly, manifested clinically with variable degree of onychorrhexis and onychoschizia. Normal nail contains 18% water whereas water content of brittle nails is less than 16%. Excessive wetness as well as drying and trauma may cause nails brittleness. Brittle fragile nails were a finding in 19% of our elderly [10,11].
Onychauxis is an age-associated thickening of the nail plate; nail plate thickness may change with aging, usually finger nails become softer and fragile whereas toe nails thick and hard. Thickened plate (37%) may present with hyperkeratosis, discoloration, and subungual hyperkeratosis. Mechanical factors as overlapping of toes and wearing of unfitted shoes may be contributing factors. Patients may have pain and increased susceptibility to onychomycosis and subungual hemorrhage. Thickening of all nail plate called pachyonychia whereas localized hypertrophy called onychauxis [2,12].
Senile nail contour changes including reduction of longitudinal curvature, prominent transverse curvature and pincer nail deformity as well as flattening of the nail plate (platyonchia) are found more frequently in the elderly [10,12]. Pincer nail may occur because degenerative osteoarthritis of distal interphalangeal joints and foot deformities and it may lead to bilateral painful ingrown nails. Pincer nail were observed in 7% and platyonychia in 5%.
Onychogryphosis is horn-like thickening of the nail plate, mostly affecting the great toenail. Infrequent cutting of the nails, trauma, hypertrophy of nail bed and bony deformities like hallux valgus may be contributing factors in formation of the onychogryphosis [4]. In this study onychogryphosis was reported in 3%.
Regarding color alterations, the elderly nail may appears opaque and dull. In this study gray opaque nails was found in 86% of elderly patients. However 11% of our elderly females were having the traditional henna stain which obscures the nail color partially. This exogenous orange red pigment grows out parallel to the cuticle.
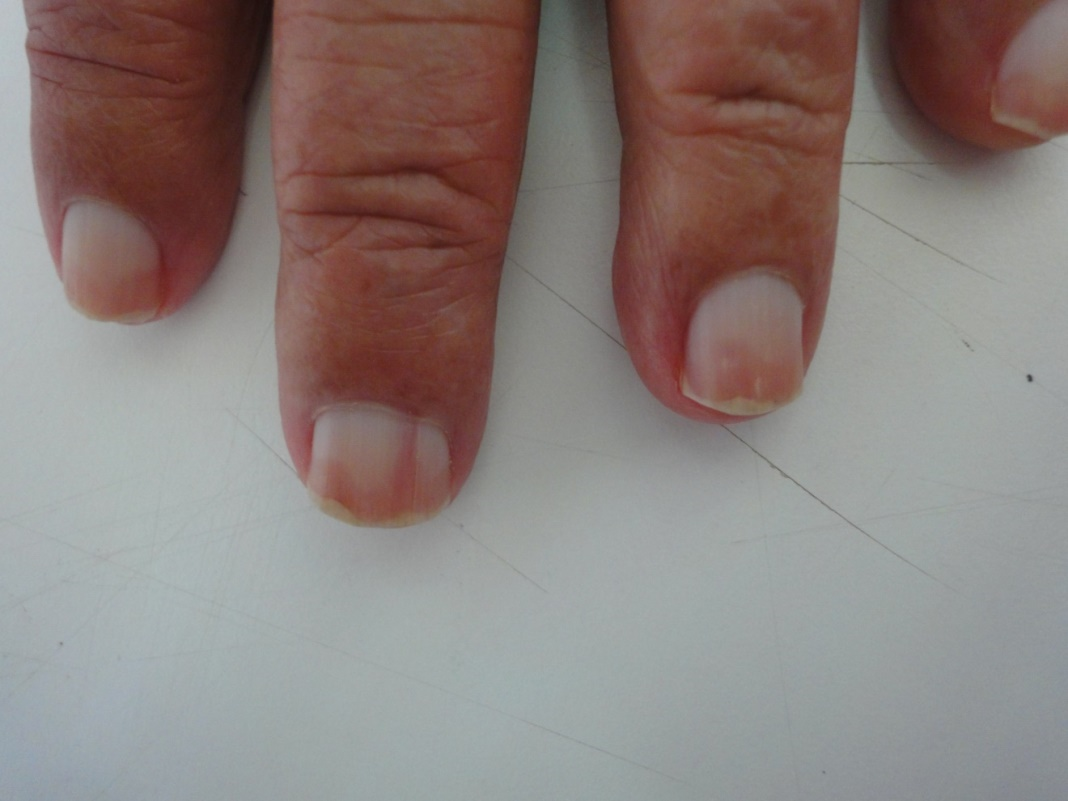
The lunula is small or absent in senile population. Visibility of lunula is significantly less than adults [10]. Nearly quarter of our studied elderly have visible lunula, mostly it was seen in the thumb and first toe.
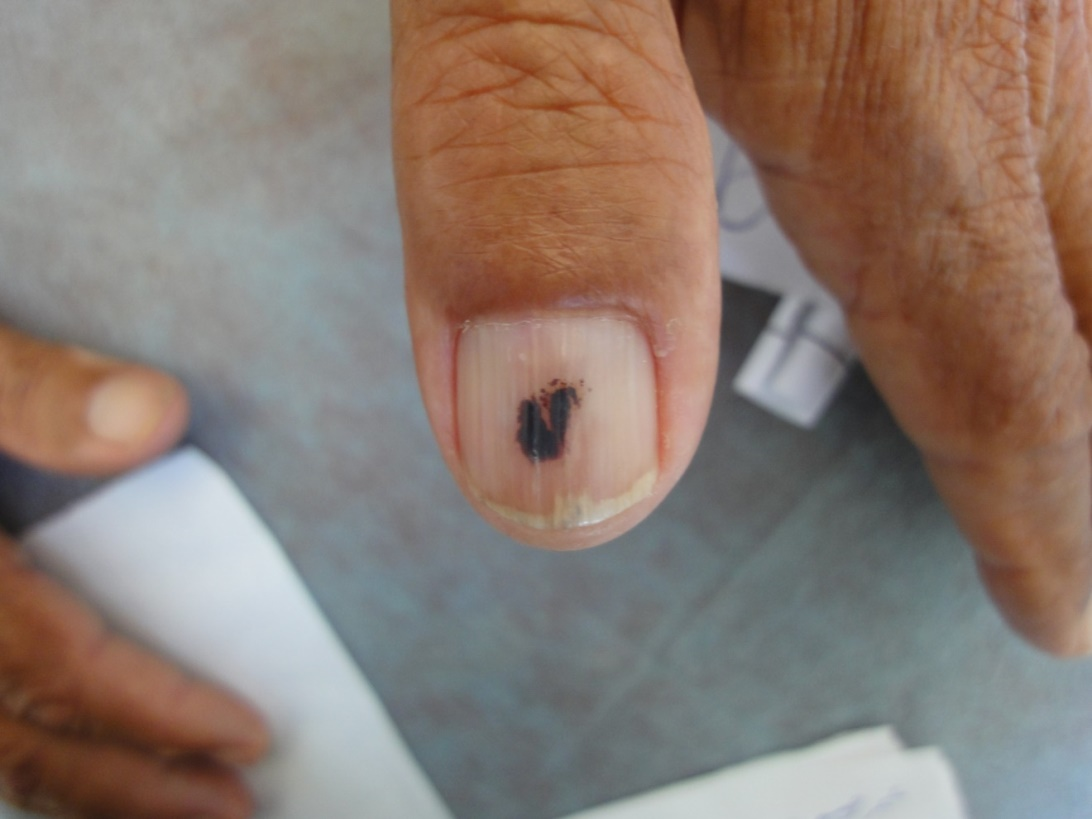
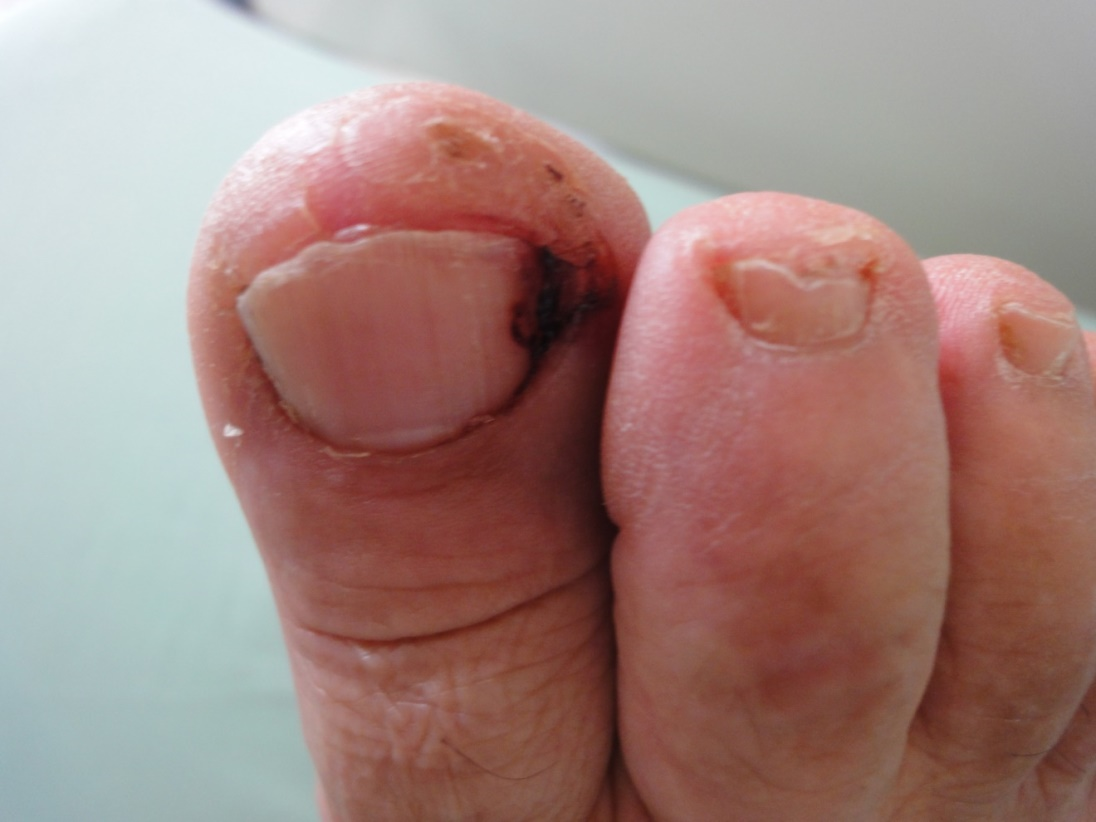
Terry nail, an apparent leukonychia with a proximal white and distal pink bands, which is usually seen in systemic diseases, however, it has been observed as senile change of the normal aging process [13]. Melanonychia is brown-black discoloration of the nail plate; longitudinal racial melanonychia is common in dark-skinned races, especially in people of African descent. Frictional melanonychia is common and it is mainly present on lateral toe nails due to repeated trauma from footwear. Fungal melanonychia caused by fungi Trichophyton rubrum and Scytalidium that produce melanin into the nail plate. However, melanonychia may be a result of melanocytic nevus, malignant melanoma or Addison’s disease. Drugs as minocycline, antimalarials, psoralens and chemotherapy may be the cause. Longitudinal racial melanonychia was reported in 2% of our elderly patients, frictional in 2% and associated with nail infection in fungal melanonychia (4%) [14].
Infection of nail apparatus may be due to fungus, bacteria, virus or parasite. Onychomycosis is the most common nail infection in old people, reaching about 20% and often affecting toenails and fingernails. It may be isolated or associated with diabetes or psoriasis [11]. In our study, nearly half of elderly patients (47%) were having onychomycosis. increased onychomycosis frequency with aging may be due to associated diabetes and peripheral arterial disease, impaired immunity, slow growth rate of the nails, and difficulty in cutting and cleaning the nails. Types of onychomycosis include proximal, lateral and distal subungual onychomycosis, white superficial onychomycosis and total dystrophic type. These are produced by dermatophytes including trichophyton species. However, Candida and molds as Scytalidium hyalinum, are frequent pathogens in elderly [2,15,16].
Pseudomonas aeruginosa infection of the nail plate is the most common bacterial nail infections, predisposing factors include trauma, chronic paronychia, prolonged exposure to water and detergents, and associated nail disorders like psoriasis [17].
Paronychia occurs infrequently in elderly, acute or chronic nail fold infection may result in nail plate changes. Acute paronychia presents as tender red nail fold swelling following trauma and it is usually caused by staphylococcus aureus, whereas chronic paronychia caused mostly by candida species and gram negative bacteria. It presents as red, swollen tender nail folds with cuticle loss [18]. Chronic paronychia was reported in 9% in the present study.
Periungual warts (3%) are due to infection with human papilloma virus. These occur in nail fold and may extend to the bed, it may cause discomfort and pain [2,4].
The nails can be involved in leprosy, leading to dry, lusterless, atrophic nails with subungual hyperkeratosis. Clofazimine causes pigmentation of the nails. We report a lepromatous leprosy patient with neuropathy, toes resorption, nail atrophy and loss [19].
Sarcoptes scabiei may inhabit the subungual hyperkeratotic debris, leading to persistent infestations. No reported scabetic nail involvement in this study.
Many senile nail disorders are due to repeated trauma [11], splinter hemorrhages are most commonly traumatic in the elderly, and they are black and found in the middle or distal third of the nail. Other benign causes are psoriasis and onychomycosis. However, splinter hemorrhages of systemic cause as infective endocarditis are red and located proximally. We report splinter hemorrhages in 12% of elderly, all were black and distal.
Subungual hematomas (9%) are traumatic and painful; they become asymptomatic with time [4].
Onychocryptosis or the ingrown nails may result from improper cutting of the nails, ill-fitting footwear, prominent nail folds and hyperhidrosis. Inflammation of the nail fold often associated with pain and tenderness. In the elderly associated comorbidity as impaired arterial circulation and sensation may predispose to secondary infection [4,20].
Beau’s lines on all nails are usually caused by any illness which disrupts the nails growth. In addition it may result from Raynaud’s disease. A single Beau's line on one nail may occur due to injury [21]. We report 2 cases of traumatic Beau’s lines. Trauma may divide the nail matrix causing splitting of the nail with chronic deformity [23]. We report a rare case of post traumatic polynychia.
Onychoclavus is tender dark hyperkeratotic lesion commonly seen in the elderly. It is caused by bony deformity, pressure or ill-fitting shoes, typically found under the distal nail plate margins of great toe [4,8]. Subungual exostosis which is a hyperkeratotic benign bony proliferation associated with nail dystrophy [4].
Single cases of pyogenic granuloma, digital myxoid cyst and acquired digital fibrokeratoma were the reported benign tumors in this study. Pyogenic granuloma is a benign vascular tumor which may involve the nail apparatus. It may be caused by drug intake or local trauma and nerve injury [23].
Digital myxoid cyst is relatively common benign tumors on the proximal nail fold usually associated with osteoarthritis and secondary nail changes. It presents as asymptomatic semi-translucent papulonodule, we report one case in this study [24].
Acquired digital fibrokeratoma is fleshy benign tumor on a finger or toe manifested as painless solitary, skin-colored, dome-shaped papule surrounded by a thin, raised skin called a collarette creating a moat like configuration [25].
Squamous cell carcinoma is the most common primary malignant tumor of the hand, constituting 75-90% of hand malignancies. Possible risk factors include sun exposure, smoking, chronic inflammation, immunosuppression and human papillomavirus infection. Clinically it may present with variable features; from a small erythematous hyperkeratotic lesion to a large ulcerated tumors. Scaling, bleeding and crusting which may be mistaken as unhealed infection as in our reported case.
Squamous cell carcinoma is locally invasive; however, metastasis occurs in 20% especially from marjolin ulcers [26].
Subungual melanoma is common in the elderly patients. The greatest frequency appears in eighth decade. It is not related to sun exposure. However trauma may be a predisposing factor causing the higher incidence in the big toe and thumb.
Bowen′s disease, basal cell carcinoma and glomus tumor are also more frequent in old age group [27]. No reported cases in this study.
Nail changes may occur in association with inflammatory skin disease (18%) as psoriasis, lichen planus and eczema. Nail involvement is common in psoriasis including pitting, yellow discoloration with oil drop appearance, onycholysis, subungual hyperkeratosis and nail thickening. It has been reported in about 10-50% of psoriasis patients [23]. Pitting occurs when parakeratotic cells, which result from keratinization defect of the matrix, detached from the nail plate surface. Pitting may be seen in psoriasis, eczema, alopecia areata, connective tissue diseases and pemphigus. In this study pitting was seen in psoriasis and eczema as well as in sporadic cases. Onycholysis occurs when the nail is lifted mechanically off the bed, it may be seen as a result of trauma or in association with skin diseases as psoriasis and onychomycosis. Systemic causes include impaired circulation and hyperthyroidism [4,12,21].
Pterygium deformity is an irreversible scarring of the nail matrix with subsequent nail splitting. It is caused by trauma, though it can be associated with inflammatory diseases involving the nail matrix as lichen planus, total epidermal necrosis and autoimmune bullous disorders [28].
Nail changes in association with systemic diseases (12%) include koilonychias, Terry’s nails, Lindsay nail, clubbing, pseuoclubbing and diabetic ischemic and neuropathic changes. True leukonychia occur due to systemic disease in which the nail matrix is affected and it could be total or partial as punctate and striate leukonychias. Apparent leukonychia occur when the nail bed is diseased changing the color of the nail plate over it whereas in Pseudoleukonychia, the nail plate is diseased due to external factors as onychmycosis. When nails are colored white proximally and pink distally, called Terry′s nails, they are associated with diabetes mellitus, malnutrition, liver disease and heart failure. However in renal disease, nails are proximally white and have brownish distal part (nails of Lindsay) [12,29,30]. Leukonychia of variable types were reported in (6%). Koilonychia is spoon shaped concave nail, it can be idiopathic or associated with iron deficiency anemia, malnutrition and hemochromatosis. Occupational softening may result in Koilonychia. Subungual hyperkeratosis may cause koilonychias, in addition, old age and digital ischemia may cause thinning of nails with koilonychia.
Clubbing occurs mainly due to cardiopulmonary disorders, in addition chronic liver disease, gastrointestinal tract and kidney diseases may present with clubbing [12,29,30]. We report one patient having clubbing associated with chronic liver disease.
Diabetes is one of the diseases that present with nail dystrophy secondary to peripheral neuropathy, vasculopathy, trauma and infections [31].
CONCLUSIONS
In geriatric people, prevalence of nail changes and disorders is high, the most common nail conditions are the age-related changes involving the color, surface, thickness and contour of the nails. Mycotic nail infections constitute an important problem in elderly reflecting impaired immunity and circulation as well as difficulty in maintaining foot hygiene. Several elderly nail conditions are related to trauma, skin diseases or systemic disorders. This study provides important data for general practitioners, dermatologists as well as geriatrician, aiming to improve the understanding of features of aging nail and the associated diseases for better assessment, accurate diagnosis and management.
Care giver advice regarding preventative care measures is important as regular nail cutting, limiting trauma, keeping nails dry and clean and using moisturizing creams as well as encouraging nutritional support.
REFERENCES
- Murdan S. (2016). Nail disorders in older people, and aspects of their pharmaceutical treatment. Int J Pharm. 512(2):405-411.
- Abdullah L, Abbas O. (2011). Common nail changes and disorders in older people: Diagnosis and management. Can Fam Physician. 57(2):173-181.
- Rubeiz N, Abbas O, Kibbi AG. (2015). Changes in Nail in the Aged. In: Farage M, Miller K, Maibach H. (eds). Textbook of Aging Skin. Springer, Berlin, Heidelberg, Germany.
- Singh G, Haneef NS, Uday A. (2005). Nail changes and disorders among the elderly. Indian J Dermatol Venereol Leprol. 71(6):386-392.
- Sarshar F, Adil M, Mudassir M, et al. (2022). Nail changes in elderly: A cross-sectional study in tertiary care hospital. Journal of Pakistan Association of Dermatologists. 32(1):68-72
- Kumar Y, Singh K, Yadav N, Paliwal N. (2017). A Study on Pattern of Nail Changes in Geriatric Population. JMSCR. 5(8):26467-26472.
- Chawla A, Singh K, Mathon S, Grewal P. (2022). Nail Disorders and Nail Changes in Geriatric Age Group, A Clinical Study. IOSR Journal of Dental and Medical Sciences (IOSR-JDMS). 21(07):35-39.
- Cohen PR, Scher RK. Aging. In: Hordinsky MK, Sawaya ME, Scher RK. (editor). Atlas of hair and nails. USA, Philadelphia: Churchill Livingstone; 2000. p. 213-225.
- Holzberg M. Nail signs of systemic disease. In: Hordinsky MK, Sawaya ME, Scher RK, (editors). Atlas of hair and nails. USA, Philadelphia: Churchill Livingstone; 2000. pp. 59-70.
- Rao S, Banerjee S, Ghosh SK, Gangopadhyay DN, Jana S, Mridha K. (2011). Study of nail changes and nail disorders in the elderly. Indian J Dermatol. 56(5):603-606.
- Baran R. (2011). The nail in the elderly. Clin Dermatol. 29(1):54-60.
- Singal A, Arora R. (2015). Nail as a window of systemic diseases. Indian Dermatol Online J. 6(2):67-74.
- Saraya T, Ariga M, Kurai D, Takeshita N. (2008). Terry’s nails as a part of aging. Intern Med. 47(6):567-568.
- Singal A, Bisherwal K. (2020). Melanonychia: Etiology, Diagnosis, and Treatment. Indian Dermatology Online Journal 11(1):1-11.
- Gupta AK, Ricci MJ. (2006). Diagnosing onychomycosis. Dermatol Clin. 24(3):365-369.
- De Berker D. (2009). Clinical practice. Fungal nail disease. N Engl J. Med. 360(20):2108-2116.
- Chiriac A, Brzezinski P, Foia L, Marincu I. (2015). Chloronychia: green nail syndrome caused by Pseudomonas aeruginosa in elderly persons. Clin Interv Aging. 10:265-267.
- Rigopoulos D, Larios G, Gregoriou S, Alevizos A. (2008). Acute and chronic paronychia. Am Fam Physician. 77(3):339-346.
- Sharma VK. Leprosy: Classification and clinical features. In: Valia RG, Valia AR, (editors). IADVL Textbook and atlas of dermatology. 2nd ed. India, Mumbai: Bhalani Publishing House; 2001. p. 1578-603.
- Noël B. (2008). Surgical treatment of ingrown toenail without matricectomy. Dermatol Surg. 34(1):79-83.
- Mayeaux EJ. (2000). Nail disorders. Prim Care. 27(2):333-351.
- Lade NR, Jain DB, Singh AL. (2012). Post-traumatic acquired polyonychia: a rare occurrence. Dermatol Online J. 18(6):10.
- Alessandrini A, Bruni F, Starace M, Piraccini BM. (2016). Periungual Pyogenic Granuloma: The Importance of the Medical History. Skin Appendage Disord. 1(4):175-178.
- Lin YC, Wu YH, Scher RK. (2008). Nail changes and association of osteoarthritis in digital myxoid cyst. Dermatol Surg. 34(3):364-369.
- Kakurai M, Yamada T, Kiyosawa T, et al. (2003). Giant acquired digital fibrokeratoma. J Am Acad Dermatol. 48(5 Suppl):S67-S68.
- Mull JL, Phelan PS, Mull AB, Russell AJ, Hurst EA, Council ML. (2020). Squamous Cell Carcinoma of the Hand: A Retrospective Study in Immunosuppressed and Immunocompetent Individuals. Dermatol Surg. 46(8):1014-1020.
- Haneke E. (2017). Important malignant and new nail tumors. J Dtsch Dermatol Ges. 15(4):367-386.
- Grover C, Singal A, Bhattacharya SN. (2021). Pterygium Complicating Nail Psoriasis and Trachyonychia: Is It Rare? Skin Appendage Disord. 7(4):298-305.
- Fawcett RS, Linford S, Stulberg DL. (2004). Nail abnormalities: clues to systemic disease. Am Fam Physician. 69(6):1417-1424.
- Saray Y, Seçkin D, Güleç AT. (2004). Nail disorders in hemodialysis patients and renal transplant recipients: A case-control study. J Am Acad Dermatol. 50(2):197-202.
- El Darouti MA, Hussein S, Al Tahlawy SR, Al Fangary M, Mashaly HM. (2011). Clinical study of nail changes in leprosy and comparison with nail changes in diabetic patients. J Eur Acad Dermatol Venereol. 25(3):290-295.