Previous Issues Volume 2, Issue 1 - 2017
A Case of Remitting Psoriasis in Association with Hyperthyroidism in a Morbidly Obese Iraqi Female
Ahmed Al-Imam*1,2
1Novel Psychoactive substances unit, University of Hertfordshire Doctoral College, Hertfordshire University, UK. 2Department of Anatomy and Cellular Biology, college of Medicine, University of Baghdad, Iraq.
Corresponding Author: Ahmed Al-Imam, Novel Psychoactive substances unit, University of Hertfordshire Doctoral College, Hertfordshire University, UK, Tel: +44 (0) 7482 571679; E-Mail: [email protected]
Received Date: 24 Mar 2017
Accepted Date: 19 May 2017
Published Date: 20 May 2017
Copyright © 2017 Al-Imam A
Citation: Al-Imam A. (2017). A Case of Remitting Psoriasis in Association with Hyperthyroidism in a Morbidly Obese Iraqi Female. Mathews J Dermatol. 2(1): 012.
ABSTRACT
Psoriasis is a very common Papulosquamous dermatosis; its manifestations are not limited to the skin; other bodily systems can also be involved. It mainly occurs with bimodal peaks of age distribution. This condition can be highly variable in severity, with an indirect effect on the quality of life and the psychiatric health.
Case Presentation: An Iraqi female patient and a medical student, nineteen years old, diagnosed with a mild chronic plaque psoriasis. The patient is morbidly obese with a 53.7 Body Mass Index. Her psoriatic condition was triggered by a stressful event four years ago, it became bilateral and localised to the feet, knees, and the scalp. She was also on Propranolol tablets as a treatment for her palpitation, for which she self-medicated against her physician many warnings. Later, she was diagnosed with hyperthyroidism and was selectively treated surgically; this surgical decision was justified by the severity of manifestations of illness, failure of medicinal (conservative) treatment, and the biochemical profile (thyroid function test). This surgery was a success, her endocrine system was back to normality, and she did not need to take Propranolol. Moreover, within one month, her psoriatic plaques resolved spontaneously and gradually towards full remission, and she was no longer in need of any psoriasis treatment.
Conclusion: The patient has an existing triggering mechanism of her psoriasis, including: psychologic, endocrine, cardiovascular, and a medicinal trigger. To the best of the authors knowledge, this is the first case report to be published, in which a spontaneous, full remission of chronic plaque psoriasis, has occurred following a subtotal thyroidectomy and withdrawal of a medicinal trigger of psoriasis. This particular report will also explore the related concept of Climatotherapy.
KEYWORDS
Psoriasis; Papulosquamous Disorders; Koebner phenomenon; Hyperthyroidism; Post-Traumatic Stress Disorders; Morbid Obesity; Propranolol; Inderal; Climatotherapy; Caspian Sea.
INTRODUCTION
Psoriasis is a chronic and a very common papulosquamous skin pathology; it affects more than three percent of the population in the United States. Although it occurs in all age groups, it primarily affects adults with a bimodal peak of age at the 3rd and 6th decades of life. It almost equally affects males and females. Psoriasis prevalence is variable across the globe. Therefore, the worldwide incidence and prevalence of psoriasis are poorly understood. Parisi et al. In their systematic review, concluded that the prevalence in children ranged from 0% in Taiwan to 2.1% in Italy, while varied in adults from 0.91% to 8.5% in the United States and Norway respectively. Data indicated that psoriasis varied according to age and geographic region, being more frequent in countries that are located far away from the equator. Prevalence estimates also varied in relation to demographics [1, 2].
Psoriasis can be very crippling, affecting other body systems, including the musculoskeletal system in the form of psoriatic arthritis (PsA) to be specific, and the cardiovascular system. The Quality of Life (QoL) can be affected, not only by the feeling of embarrassment and shame, and social isolation and withdrawal but also as a result of the involvement of other body systems as aforementioned. Prey et al. In their systematic review, revealed that PsA could affect up to 24% of psoriasis patients. PsA may even predate the cutaneous involvement. In relation to the cardiovascular system, Miller et al. In their meta-analysis, indicated that psoriasis patients are at a significantly higher risk, to develop hypertension, both systolic and diastolic, higher lipid profile especially Low-Density Lipoprotein Cholesterol and Triglycerides. Additionally, such patients have natural propensity to be obese and to have a higher blood glucose levels and higher HbA1c. Another systematic review and meta-analysis in 2013, reported that the relative risks of cardiovascular diseases (CVD) were highest in the younger patients, and patients with severe psoriasis, while absolute risks were greatest in older individuals with severe psoriasis [3-5]. In relation to morbid obesity, both overweight and obesity, are associated with the incidence of multiple other co-morbidities including type-2 diabetes, cancer and CVD. Furthermore, psoriasis also serves as an independent risk factor for CVD. Systemic therapies for moderate to severe psoriasis also potentiate the cardiovascular risk and CVD [6, 7]. Consequently, the QoL of patients with psoriasis will be jeopardised. De Korte and colleagues, clarified that more severe psoriasis was associated with lower levels of quality of life. There was a tendency that older patients had slightly lower levels of physical functioning. These studies were based on multiple QoL indices including DLQI Dermatology Life Quality Index (DLQI), Psoriasis Disability Index (PDI), SF-36MOS 36- Item Short-Form Health Survey SF-36, and Sickness Impact Profile (SIP) [8]. Furthermore, stress is not only inducible by psoriasis, but psoriasis is frequently triggered by a stressful and/or a traumatic psychologic event, as in post-traumatic stress disorder (PTSD). Neria et al. In their systematic review on PTSD, revealed that PTSD is associated with a range of predisposing factors and correlates, including demographic variables, socioeconomics, event exposure characteristics, social factors and personality traits [9].
Psoriasis is a very complex and an unpredictable dermatosis, many medicinal and chemical products, have been found to be associated with the triggering and/or exacerbation of psoriasis including lithium, beta-adrenergic receptor blockers, and antimalarial drugs. The withdrawal of corticosteroids has been associated with activation pustular psoriasis. On the other hand, Nonsteroidal anti-inflammatory drugs were found to worsen psoriasis. Similarly, therapeutics for psoriasis itself, both topical and systemic, may cause a flare of psoriasis [10].
The level-of-evidence of this paper is Level-5, in accordance with the classification system by the Oxford Centre for Evidence-based Medicine (CEBM) [11]. In relation to the literature review, medical databases, paramedical databases, and grey literature (unpublished data), all were scrutinised systematically using prespecified keywords. The keywords are Psoriasis; Papulosquamous; Koebner; Hyperthyroidism; Post-Traumatic Stress Disorders; Morbid Obesity; Propranolol; Inderal; Climatotherapy; Azerbaijan; and Caspian Sea. These keywords were also used in combination, by using Boolean operators to achieve accurate search results [12]. Searched medical and paramedical databases included: PubMed, The Cochrane Library, Scopus, EBSCO and CINAHL, OpenGrey, and Google Scholar.
Papers of the highest level of evidence in the literature were included for referencing of this manuscript, most of these were systematic reviews and meta-analyses of the top hierarchy of evidence, while other papers and resource materials, were considered when finding pertinent to the presented topic. To the best of our knowledge of the available literature, this is the 1st reported case of a localised flexural chronic plaque psoriasis, in which a complete remission was achieved following a medicinal withdrawal (Propranolol discontinuation), and in combination with a concomitant surgical treatment of hyperthyroidism, a coexisting endocrine abnormality.
CASE PRESENTATION
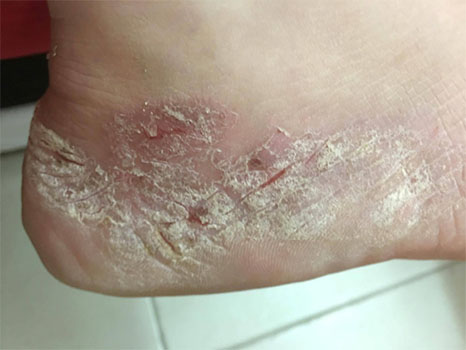
The patient is a nineteen years old female patient and a medical student, who has been diagnosed four years ago, with localised and a mild form of flexural psoriasis (Figure 1).
Figure 1: Psoriatic Plaque on the Lateral Aspect of the Right Heal.
The patient is also suffering from Morbid obesity, with a Body Mass Index (BMI) of 53.7. There is also a positive family history of obesity and morbid obesity. However, there is no family history of classical psoriasis, i.e. chronic plaque psoriasis, or any of psoriasis clinicopathological subtypes. Fortunately, the patient has no history of accompanying hyperlipidemia, hypertension, diabetes, or other manifestations in relation to the Metabolic syndrome. The patient chronologically correlated and attributed the development of her psoriasis, with a post-traumatic stress disorder, which occurred four years ago, that developed as a result of a nearby explosion and firearm shots in the city of Baghdad. Within two months, she developed the first manifested psoriatic plaque; a plaque localised unilaterally to the medial aspect of the right foot. The patient applied some mild cortisone ointments to the lesion, and the psoriatic plaque soon disappeared completely to relapse again after two years. Thereafter, the lesion appeared bilaterally on the lateral and dorsal surface of the feet, extensor aspects of both knees, and the back of the scalp. Accordingly, the patient consulted a Dermatologist, and she was diagnosed as a mild case of chronical plaque psoriasis, the extent of the disease was based on the clinical examination, Psoriasis Area Severity Index (PASI) score, and Quality of Life assessment. The patient had no involvement of the nails, nor the joint (psoriatic arthropathy), or any other systemic involvement with psoriasis, including the cardiovascular system. However, the patient was complaining of a palpitation for which she self-medicated with propranolol, a non-selective Beta blocker and a well-known contraindicated trigger of psoriasis, she has accessed this medicine over-thecounter from a local pharmacy and without a medicinal prescription. Further, her physician urged her persistently to stop this medication.
Accordingly, she was prescribed with Verapamil by a cardiologist. However, the patient switched back to Inderal (propranolol) tablets, as her palpitations were not controlled with Verapamil. Since then, she was on 40 mg tablets of Inderal once daily, and she refused to try any replacement medications after consulting several cardiologists. Later, she was instructed to perform a Thyroid Function Test (TFT) to exclude coexisting endocrine disturbances. Truly, she was diagnosed with hyperthyroidism; there was a significant elevation of both T3 and T4, and a proportional reduction in TSH level. Over the next 2 years, she kept taking anti-thyroid medications. However, her hyperactive goitre was unresponsive and was considered for an elective surgical subtotal thyroidectomy. Meanwhile, she kept treating her psoriatic plaque lesions using potent and superpotent topical steroids +/- topical antibiotics for accompanying infection. The patient was selective for the use of creams rather than the use of greasy ointments.
Her surgical procedure was a success, and her thyroid hormone levels were restored back to normality. Furthermore, her palpitations were not existent anymore, and her propranolol was stopped completely. Her psoriasis used to relapse and remit prior to her surgical thyroidectomy, in correspondence with stress, exposure to the sun, localised trauma and/or itching (Koebnerization), and sometimes in association with travelling to other countries. During one of her trips to Azerbaijan, the patient reported a considerable improvement of her psoriasis, followed by a complete remission for some months during her vacation near the Caspian Sea. She associates her skin condition improvement with the topical application of the sea water to her psoriatic plaque.
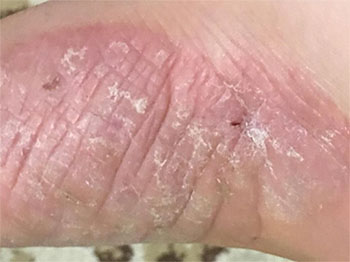
Furthermore, following her recovery from surgery and the withdrawal from Inderal tablets, her psoriasis started to regress gradually and spontaneously, merely within few months after her surgery (Figure 2), and followed by a complete and indefinite remission until this very moment, the patient was no longer in need to apply any topical medications to her previously morbid skin. To summarise, the patient had multiple triggering mechanisms for her psoriasis, including a stressful psychologic event and a subsequent PTSD, Koebnerization, a medicinal trigger, and morbid obesity.
Figure 2: Psoriatic Plaque on the Lateral side of the Left Foot
DISCUSSION
This is an interesting case of a young Iraqi female patient with a classic case of mild psoriasis. The patient is morbidly obese with a subsequently diagnosed endocrine abnormality, a hyperthyroid goitre. Her psoriasis was localised to both feet, knees, and scalp. Her psoriasis was treated with topical medications only, including superpotent topical steroids, and topical antibiotics-steroids combination when there were signs of an accompanying infection. The patient also had refractory tachycardia and palpitations, for which she self-medicated with propranolol tablets, and refused to replace with other medications. The patient correlated the development of her psoriasis in a historical association with her post-traumatic stress disorder and the use of propranolol.
Later, she was electively planned to undergo an ablative subtotal thyroidectomy for her hyperactive thyroid goitre. This surgery restored her normal endocrine status and also suc-ceeded in reversing her pathologic tachycardia. Furthermore, she was no longer in need of propranolol oral tablets. Following the withdrawal of this medication and within merely few months, the patient reported gradual and spontaneous recession of her psoriatic plaque lesion, which remitted completely, and the patient was no longer applying any topical or having any systemic medications for psoriasis. This is the first case report in literature in which a total remission of psoriasis, which was achieved in association with thyroidectomy, endocrine status normalisation, and propranolol withdrawal. This case definitely shows the importance of patient compliance and avoidance of certain already known triggers of psoriasis including medicinal and endocrine anomalies. Additionally, the Climatotherapy, at the Caspian Sea in Azerbaijan as reported by this patient and others in published literature, is worthy of further scientific analyses, particularly chemical analysis of seawater and the employment of pragmatic Randomised Clinical Trials. Another important factor that might contribute to her psoriasis is her morbid obesity. However, that was of the genetic basis and beyond the capacity of the patient to control. The patient is considering a stomach bypass surgery in the near future; the patient decision was based on the high BMI which is not only endangering her health, social status, but also her psychologic stability.
REFERENCES
- Parisi R, Symmons DP, Griffiths CE and Ashcroft DM. (2013). Global epidemiology of psoriasis: a systematic review of incidence and prevalence. Journal of Investigative Dermatology. 133(2):377-385.
- U.S. National Library of Medicine, PubMed Health. Psoriasis.
- Prey S, Paul C, Bronsard V, Puzenat E, et al. (2010). Assessment of risk of psoriatic arthritis in patients with plaque psoriasis: a systematic review of the literature. Journal of the European Academy of Dermatology and Venereology. 24(s2): 31-35.
- Miller IM, Skaaby T, Ellervik C and Jemec GB. (2013). Quantifying cardiovascular disease risk factors in patients with psoriasis: a meta-analysis. British Journal of Dermatology. 169(6): 1180-1187.
- Samarasekera EJ, Neilson JM, Warren RB, Parnham J, et al. (2013). Incidence of cardiovascular disease in individuals with psoriasis: a systematic review and meta-analysis. Journal of Investigative Dermatology. 133(10): 2340-2346.
- Guh DP, Zhang W, Bansback N, Amarsi Z, et al. (2009). The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC public health. 9(1): 1.
- De Korte J, Mombers FM, Bos JD and Sprangers MA. (2004). Quality of life in patients with psoriasis: a systematic literature review. In Journal of Investigative Dermatology Symposium Proceedings 9(2): 140-147.
- Neria Y, Nandi A and Galea S. (2008). Post-traumatic stress disorder following disasters: a systematic review. Psychological medicine. 38(4): 467-480.
- Abel EA, DiCicco LM, Orenberg EK, Fraki JE, et al. (1986). Drugs in exacerbation of psoriasis. Journal of the American Academy of Dermatology. 15(5):1007-1022.
- Coumbe AG, Pritzker MR and Duprez DA. (2014). Cardiovascular risk and psoriasis: beyond the traditional risk factors. The American journal of medicine. 127(1): 12-18.
- (2009). Oxford Centre for Evidence-based Medicine. Levels of Evidence.
- Fox EA and Sharan S. (1986). A comparison of two methods for soft boolean operator interpretation in information retrieval.