Information Links
Related Conferences
Previous Issues Volume 11, Issue 1 - 2026
Role of Autologous Bone Marrow Aspirate Therapy in Wound healing and Preventing Abnormal Scarring in Thermal Burn Patients
Nagarjun S Ghatti1, Ravi Kumar Chittoria2,*, Kanav Gupta3
1Observer, Department of Plastic Surgery, JIPMER, India
2Professor and Associate Dean (Academic), Head of IT Wing and Telemedicine, Department of Plastic Surgery and Telemedicine, JIPMER, India
3Senior Resident, Department of Plastic Surgery, JIPMER, India
*Corresponding Author: Dr. Ravi Kumar Chittoria, MCh, DNB, MNAMS, FRCS (Edin), DSc, PhD (Plastic Surgery), Professor and Associate Dean (Academic), Head of IT Wing and Telemedicine, Department of Plastic Surgery and Telemedicine, JIPMER, Puducherry, India – 605006, Mobile: 9442285670, E-mail: [email protected]
Received Date: October 06, 2025
Published Date: February 17, 2026
Citation: Ghatti NS, et al. (2026). Role of Autologous Bone Marrow Aspirate Therapy in Wound healing and Preventing Abnormal Scarring in Thermal Burn Patients. Mathews J Case Rep. 11(1):216.
Copyrights: Ghatti NS, et al. © (2026).
ABSTRACT
The aim of this case report is to evaluate the role of autologous bone marrow aspirate in promoting wound healing and preventing abnormal scarring in a burn patient. Clinical assessment was conducted to determine the extent of the burn injury, and standard burn care, including antibiotics, intravenous fluids, analgesics, dressings, regenerative therapies, and scar management, was administered. Autologous bone marrow aspirate was incorporated as an adjunctive therapy. Its application demonstrated accelerated wound healing and reduced risk of abnormal scarring. These findings highlight the potential of bone marrow aspirate as a valuable regenerative option in the management of complex burn wounds.
Keywords: Autologous Bone Marrow Aspirate Therapy, Wound healing, Abnormal Scar, Prevention, Regenerative Therapy, Burns.
INTRODUCTION
Wound healing in the case of burn scars is a coordinated process involving complex mechanisms that progress through various stages, including blood clotting, inflammation, cellular proliferation, angiogenesis, and reconstruction of the extracellular matrix. Disruption or failure in any of these stages—due to factors such as ischemia, reperfusion injury, bacterial infection, or aging—can lead to chronic inflammation and result in a non-healing wound. In this article, we discuss the role of autologous bone marrow aspirate therapy in enhancing wound healing and preventing abnormal scar formation in burn injuries [1].
MATERIALS AND METHODS
This study was conducted at a tertiary care hospital in South India after obtaining approval from Institutional Ethics Committee. Informed consent from the patient obtained. The patient was a 46-year-old gentleman with alleged history of accidental thermal burns to chest abdomen and right arm forearm. (Figure 1). The patient was admitted to the burns ward and managed according to standard WHO protocol, which included antibiotics, intravenous fluids, analgesics, and regenerative therapies. As part of the regenerative approach, autologous bone marrow aspirate therapy was utilized to promote wound healing and prevent the development of abnormal scarring. Wound Score was documented using the Bates Jansen Wound Assessment Tool. Wound measurements were recorded by the ImitoMeasure app (Figure1). Wound Score and measurements were recorded weekly. Wound tissue culture was sent and antibiotic was started according to the sensitivity. The Debridement of necrotic tissue was done before the application of autologous bone marrow aspirate. The bone marrow was aspirated from the iliac crest (Figure 2) and applied (Figure 3). A total of 5 ml of aspirate was collected and was performed once alongwith other regenerative techniques, VSS score was noted for healed areas.
.png)
Figure 1(a,b). Dimensions of the burn wound over anterior chest wall and arm region measured using imitomeasure app.
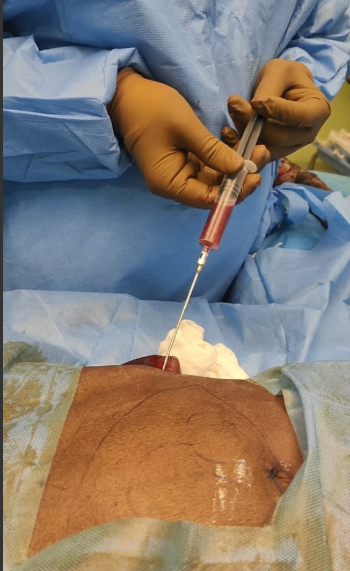
Figure 2. Autologous bone marrow aspiration from right iliac crest using Jamshidi needle.
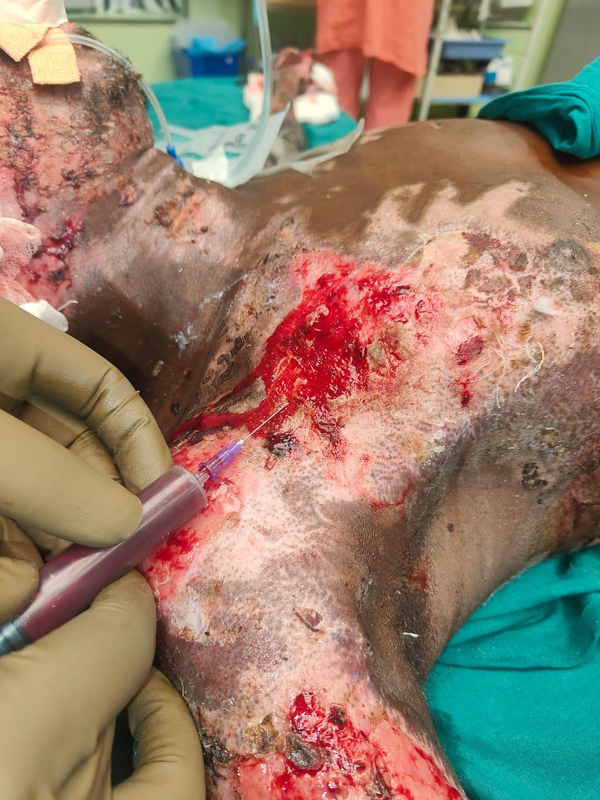
Figure 3. Application of ABMAT in burn wound.
RESULTS
Autologous bone marrow aspirate therapy demonstrated progressive improvement in wound healing, with measurable reduction in wound size and improvement in granulation tissue quality. No adverse events or complications were observed. The therapy contributed to minimization of hypertrophic scarring as reflected by improved VSS scores (Figure 4). The procedure was well tolerated, with no complications observed.
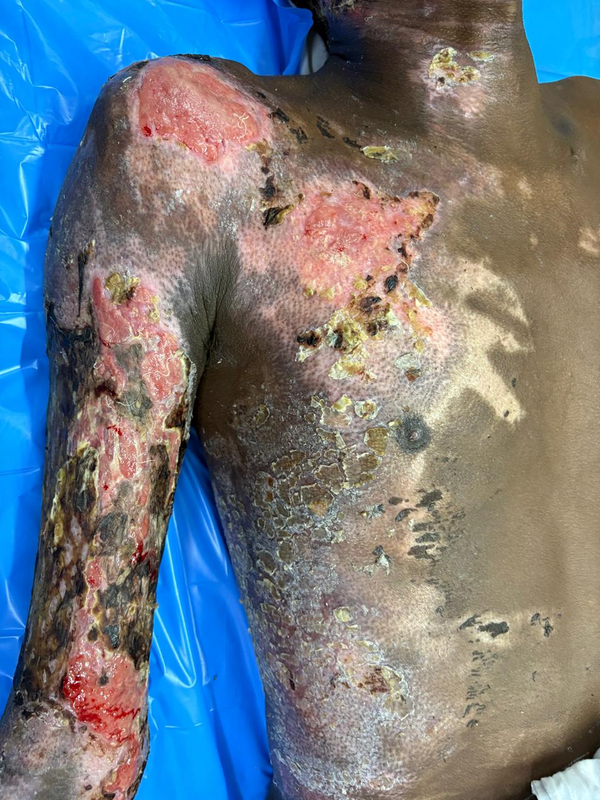
Figure 4. Raw area significantly reduced after 1 week.
DISCUSSION
With the rising prevalence of burn scars, various therapies have emerged to address the associated challenges. However, substantial evidence still highlights gaps in the effective treatment of burn scars [2]. Stem cell therapy has been extensively explored as a potential solution to bridge this gap. Due to the technical and regulatory complexities involved in using embryonic stem cells, adult autologous bone marrow-derived stem cells have emerged as a promising alternative. When mesenchymal stem cells (MSCs) derived from bone marrow were found to be linked to the origin of epidermal cells, their potential role in cutaneous wound healing gained attention. It is postulated that MSCs mobilize from the bone marrow niche and migrate to ischemic tissues through peripheral circulation in response to cytokine signalling [3,4]. Upon reaching the injury site, these cells differentiate into various epidermal and dermal cell types.
Neovascularization, or new blood vessel formation, is a critical aspect of wound healing, essential for oxygen and nutrient supply as well as waste removal. In vitro studies have shown that MSCs can differentiate into endothelial cells, suggesting their role in postnatal vasculogenesis during the healing process. Additionally, MSCs exert significant therapeutic effects through paracrine signaling pathways [5,6]. With increasing evidence supporting the effectiveness of stem cell therapy in wound healing, current research is now focused on optimizing cell delivery methods. The clinical success of MSC therapy is closely linked to the number of cells delivered, prompting the development of innovative delivery techniques aimed at enhancing cell engraftment and minimizing inhibitory factors [7,8].
For instance, Ichioka et al. demonstrated that a bone marrow-impregnated collagen matrix can enhance wound repair by promoting angiogenesis [9]. Hydrogels have also gained popularity as MSC delivery vehicles due to their extracellular matrix-like hygroscopic nature, offering a favorable environment for cell survival and integration [10,11].
Although autologous bone marrow aspirate therapy shows promise, several challenges remain. These include variability in stem cell yield, limited cell survival in hostile wound environments, and difficulty in ensuring uniform cell distribution across large or deep burn wounds. Innovative strategies aimed at improving MSC survival, such as using hydrogel scaffolds, collagen matrices, or platelet-rich fibrin as delivery vehicles- have shown potential to enhance cell engraftment and prolong viability. Optimization of delivery techniques and the microenvironment may significantly improve therapeutic outcomes.
CONCLUSION
Autologous bone marrow aspirate serves as an important regenerative tool in enhancing wound healing and preventing abnormal scar formation in burn patients. Its role as an adjunct to standard burn care warrants further evaluation in larger clinical studies.
CONFLICTS OF INTEREST
Nil.
REFERENCES
- Mustoe TA, O'Shaughnessy K, Kloeters O. (2006). Chronic wound pathogenesis and current treatment strategies: a unifying hypothesis. Plast Reconstr Surg. 117(7 Suppl):35S-41S.
- Masoud M, Wani AH, Darzi MA. (2014). Topical heparin versus conventional treatment in acute burns: a comparative study. Indian J Burns. 22:43‑50.
- Phillips TJ, Machado F, Trout R, Porter J, Olin J, Falanga V. (2000). Prognostic indicators in venous ulcers. J Am Acad Dermatol. 43(4):627-630.
- Hamou C, Callaghan MJ, Thangarajah H, Chang E, Chang EI, Grogan RH, et al. (2009). Mesenchymal stem cells can participate in ischemic neovascularization. Plast Reconstr Surg. 123(2 Suppl):45S-55S.
- Kim WS, Park BS, Sung JH, Yang JM, Park SB, Kwak SJ, et al. (2007). Wound healing effect of adipose-derived stem cells: a critical role of secretory factors on human dermal fibroblasts. J Dermatol Sci. 48(1):15-24.
- Ichioka S, Kouraba S, Sekiya N, Ohura N, Nakatsuka T. (2005). Bone marrow-impregnated collagen matrix for wound healing: experimental evaluation in a microcirculatory model of angiogenesis, and clinical experience. Br J Plast Surg. 58(8):1124-1130.
- Lutolf MP, Hubbell JA. (2005). Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nat Biotechnol. 23(1):47-55.
- Dash NR, Dash SN, Routray P, Mohapatra S, Mohapatra PC. (2009). Targeting nonhealing ulcers of lower extremity in human through autologous bone marrow-derived mesenchymal stem cells. Rejuvenation Res. 12(5):359-366.
- Liew A, O'Brien T. (2012). Therapeutic potential for mesenchymal stem cell transplantation in critical limb ischemia. Stem Cell Res Ther. 3(4):28.
- Chen L, Tredget EE, Wu PY, Wu Y. (2008). Paracrine factors of mesenchymal stem cells recruit macrophages and endothelial lineage cells and enhance wound healing. PLoS One. 3(4):e1886.
- Mundra V, Gerling IC, Mahato RI. (2013). Mesenchymal stem cell-based therapy. Mol Pharm. 10(1):77-89.