Previous Issues Volume 2, Issue 1 - 2017
Multiple Thromboembolic Stroke and Myocardial Infarction in a Young Male in the Setting of Amphetamine Use
Naji Rad S1 *, Kandakatla p1 , Sanivarapu RR1 , Sayedy N1 , Frieri M2 , Chua W3
1Department of Medicine, Nassau University Medical Center, East Meadow, New York. 2Division of Allergy Immunology, Department of Medicine, Nassau University Medical Center, East Meadow, New York. 3Division of pulmonary and critical care medicine, Department of Medicine, Nassau University Medical Center, East Meadow, New York.
Corresponding Author: Sara Naji Rad, Department of Medicine, Nassau University Medical Center, East Meadow, New York, Tel: 516-572-6501; E-Mail: [email protected]
Received Date: 09 Jun 2017 Accepted Date: 21 Jun 2017 Published Date: 23 Jun 2017
Copyright © 2017 Naji Rad S
Citation: Naji Rad S, Kandakatla P, Sanivarapu RR, Sayedy N, et al. (2017). Multiple Thromboembolic Stroke and Myocardial Infarction in a Young Male in the Setting of Amphetamine Use. Mathews J Cardiol. 2(1): 012.
ABSTRACT
Amphetamines are first line treatment for Attention-Deficit Hyperactivity Disorder (ADHD). Known to have serious cardiovascular adverse effects such as MI, Stroke, and sudden death specially if used in high doses or long term. ADHD patients are predisposed to have concomitant substance use disorder. Substances like cocaine and marijuana increase risk of cardiovascular events. By knowing these, clinicians must be cautious in prescribing CNS stimulant agents. Precise personal, medical, drugs and medication history needs to be obtained before and during treatment. Herein, we present a young male with ADHD treated with amphetamines and concomitant marijuana use who presented with multiple thromboembolic stroke and acute myocardial infarction.
KEYWORDS
Amphetamine; Attention-Deficit Hyperactivity Disorder; Cardiovascular Disease.
ADHD: Attention deficit hyperactivity disorder, MI: Myocardial infarction, CNS: Central nervous system, WHO: World Health Organization, NIH stroke scale: National institutes of health stroke scale, MCA: Middle cerebral artery, PCA: Posterior cerebral artery, CVA: Cerebrovascular accident, AKI: Acute kidney injury, CPR: Cardiopulmonary resuscitation, ACLS: Advanced cardiac life support, STEMI: ST elevation myocardial infarction
INTRODUCTION
Attention-Deficit Hyperactivity Disorder (ADHD) is a cognitive disorder as a result of imbalance between the catecholamine and dopamine systems in the prefrontal cortex. In the USA, the prevalence of ADHD among children and adults is estimated at 11% and 4.4% respectively [1, 2]. CNS stimulants such as amphetamines are considered first line treatment for ADHD in adults and children. Clinical use of amphetamines dates back to 1920s for treatment of asthma [3] and later used to increase alertness in military troops in World War II and also as a weight loss medication. Amphetamines are the second most commonly used illicit drugs worldwide, with an estimated 4.7 million Americans who have tried these medications at some point in their life [4]. Many studies have revealed high-doses and long-term use of amphetamines associated with numerous adverse effects, especially serious cardiovascular events and sudden death. Multiple cases have reported atrial filtration and acute myocardial infarction in recreational amphetamine abusers [5, 6]. Other psychiatric illnesses such as mood disorders (38%), anxiety (47%) and poor impulse control (20%) are also found among adults with ADHD resulting in a higher likelihood of leading an unhealthy lifestyle (i.e obesity, smoking, substance abuse, etc) and subsequently cardiovascular events. Studies have revealed that 15% of ADHD patients have concomitant substance use disorders [1]. Substances like cocaine and marijuana increase risk of cardiovascular events. World Health Organization (WHO) recently reported that chronic use of cocaine may be associated with myocardial infarction and stroke [7]. Gerhard et al study reported that 80% of adult patients with ADHD with evidence of = 1 preexisting cardiovascular diseases were treated with CNS stimulants. Despite knowledge of preexisting cardiovascular disease (10.5%) in ADHD patients, no significant reduction in stimulants prescription has been observed [8].
CASE PRESENTATION
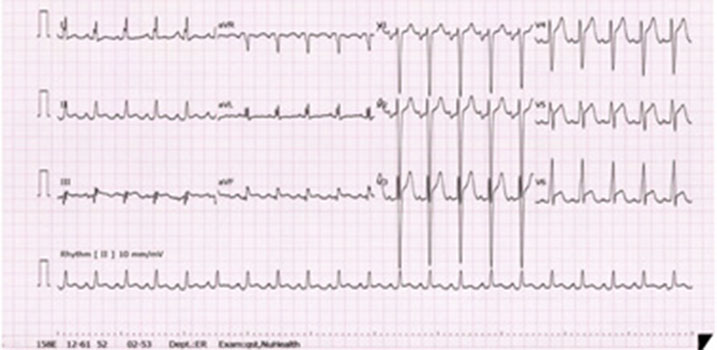
A 37-year-old man presented to the emergency department with left facial droop and left sided weakness which started 45 minutes prior to admission. All history was obtained from his wife because he was intubated upon arrival to emergency ward. He was diagnosed with ADHD at age 13 and was prescribed amphetamine-based medication up until he graduated from college. Amphetamine was re-started by his primary care physician one year ago due to the patient`s lack of concentration at his new job. He was taking Adderall XR 25 mg daily. According to his wife he was in his normal state of health until afternoon of admission day when he suddenly developed left facial droop and left sided weakness. He did not have reported chest pain, nausea or diaphoresis. His past medical history was unremarkable except for ADHD. His family history was unremarkable for cardiovascular diseases. His wife reported patient consumes marijuana daily, however, she was not aware of patient’s last marijuana use. He drinks alcohol occasionally and does not smoke tobacco. He was on Adderall XR 25 mg daily, azithromycin for recently diagnosed sinusitis. He had no known drug allergies. In the ED patient’s vital signs were as follows: blood pressure: 170/90 mmHg, pulse rate: 127 beats per minute, respiratory rate: 20 breaths per minute, O2 saturation: 100% and temperature: 36.5 C. Physical exam was remarkable for slurred speech, left facial palsy and ipsilateral hemiplegia. NIH stroke scale upon arrival was 5. Patient met the window period for TPA administration. Head CT to rule out hemorrhagic stroke was performed and TPA was initiated. Patient became agitated and combative 30 minutes after arrival, three rounds of Ativan was administered with no improvement. Eventually, he was intubated for airway protection. TPA therapy was completed and followed with a head CT scan, which was negative for intracranial pathology. A 12-lead Electrocardiogram revealed sinus tachycardia, ST elevation in V3-V6, II, III, AVF and reciprocal ST depression in I, AVL (figure1). First set of cardiac biomarkers: Troponin 3.76 ng/ml, CPK 367 u/l, CK-MB 5.4 ng/ ml, CK-mass 1.47 ng/ml. Urine toxicology was only positive for amphetamine. Chest XR (AP) revealed pulmonary vascular congestion, pulmonary interstitial edema, and an enlarged and somewhat globular cardiac silhouette.
Figure 1: Electrocardiogram on admission to hospital.
He was admitted to intensive care unit for hemodynamic monitoring, serial neurologic checks, EKGs, and blood testing. Urgent neurology and cardiology consults were placed for evaluation of stroke and anterior inferior STEMI. Repeated EKGs revealed sinus tachycardia, ST elevation but decreased in V3-V6, II, III, AVF and Q waves in III, and AVF. Troponin up trended on serial check with a peak of 55.1 ng/ml. On day one, a bedside echocardiography with difinity contrast revealed left ventricular ejection fraction of less than 15% with global systolic dysfunction, mild MR and no evidence of LV thrombus. As per in-house interventional cardiologist, patient was not a candidate for catheterization or balloon pump due to TPA administration and acute CVA. A third head CT scan within 6 hour interval was obtained and revealed a right MCA territory infarct with mass effect and no midline shift. Patient was started on aspirin 81 mg, Plavix 75 mg and Atorvastatin 40 mg. Initiation of heparin drip was postponed in light of the high risk of conversion of ischemic stroke to hemorrhagic stroke, Risks and benefits were discussed with the patient’s family members including his wife. Within 24 hours of admis-sion, patient developed cardiogenic shock and pulmonary edema in the setting of massive MI. Vasopressor support was initiated and his blood pressure eventually normalized in response to treatment with norepinephrine, phenylephrine and dobutamine drips. Patient was clinically in volume overload with pulmonary edema, which was managed with intravenous furosemide pushes. On day two of admission, patient was weaned off sedation and in a comatose state. The fourth CT scan of his head now revealed expansion of stroke and addition of left PCA territory infarct to previous right MCA infarct. Patient was continued on three vasopressors for blood pressure support. Day three of admission, echocardiography revealed a moderate, fixed thrombus on the apical wall of the left ventricle. Patient`s hospital course was complicated with acute renal failure and resistant hyperkalemia secondary to acute kidney injury (AKI). Hemodialysis was initiated. Day four of admission, he spiked a fever, with increasing endotracheal tube secretions and chest X-ray confirming new consolidation, Intravenous antibiotics was started for treatment of health care associated pneumonia. Day five of admission, patient had no improvement in clinical status and his prognosis remained poor due to extensive myocardial infarct, multiple cerebrovascular accidents and multi-organ failure. Neurology team cleared patient for anticoagulation therapy and heparin drip was initiated. Treatment was discussed again with family, risks and benefits were explained. Day seven of admission, patient had cardiopulmonary arrest. CPR was executed according to ACLS guidelines; patient was with pulseless electrical activity all throughout course of CPR. Patient was pronounced dead after 35 minutes of CPR.
DISCUSSION
Adderall is a CNS stimulant prescribed for persons of all age groups with ADHD. The active ingredient of Adderall is Damphetamine and L-amphetamine salts in the ratio of 3:1. Amphetamines have sympathomimetic activity by releasing norepinephrine from sympathetic nervous system [9, 10]. Adverse cardiovascular events of stimulant drugs have always been concerning which include sudden death, stroke, and myocardial infarction [11, 12]. Due to these concerns, in February 2005, the FDA conducted a review of their cardiovascular risks. Finally, in February 2007, the FDA issued an advisory for all stimulant medications used in treatment of ADHD and requested manufacturers to develop guides to inform patients of the cardiovascular risks associated with stimulant drugs [13, 14]. The exact mechanism of cardiovascular effects of CNS stimulant drugs is not completely clear. Suggested mechanisms are as follows: increase in heart rate and blood pressure, catecholamine-induced platelet aggregation which subsequently increases risk of thrombus formation [15, 16], increased circulating catecholamines resulting in vasospasm and myocardial ischemia [17], vasculitis caused by high production of pro-inflammatory immuno-active glycation end products in circulation [18], hyperplasia of coronary artery intima [19], prolonged QT interval which can progress to torsades de pointes [20]. CNS stimulants such as amphetamines increase heart rate and blood pressure which have been discriminated to accelerate cardiovascular diseases [21, 22]. Epidemiologic studies have revealed increased resting heart rate as a valuable predictor of mortality and decreased life expectancy [23, 24]. Cooney et al study, revealed increased heart rate by 15 bpm, is associated with increased cardiovascular mortality rate by 23-50%, in both genders [23]. Also, Perret-Guillaume et al, demonstrated increase in heart rate by 10 bpm of baseline is associated with increased rate of cardiac death by 20% [24]. Mick et al study, reported that CNS stimulants significantly increased resting heart rate and systolic blood pressure by 5.7 bpm and 1.2 mmHg, respectively. CNS stimulants dysregulate interaction of autonomic system and myocardial function, which might cause some cardiac arrhythmias such as, atrial fibrillation and atrial flutter, especially in patients with prior structural cardiac problems [25, 26]. Another condition in which sympathetic response has an essential role in cardiovascular events is pheochromocytoma, a catecholamine-producing tumor. Ten percent of patients with pheochromocytoma have left ventricular dysfunction [27]. Catecholamine induced cardiomyopathy in the setting of pheochromocytoma has similar presentation as stress induced cardiomyopathy [28]. Smith et al, reported a case with congestive heart failure of unknown etiology, who had taken dextroamphetamine over a long period of time. Autopsy of the heart revealed histological findings with similarities to myocarditis associated with pheochromocytoma. They proposed a possible relationship between amphetamines and cardiomyopathy [29]. Movahed et al, reported a case who presented with tachycardia and hypertension after inhalation of amphetamines. Patient had ST depression in precordial leads on EKG and elevated cardiac enzymes. Echocardiography showed an ejection fraction of 20% with basal akinesia and normal RV function. Angiography revealed normal coronary arteries. Diagnosis of Takotsubo cardiomyopathy was made. They proposed tachycardia and hypertension associated with amphetamine use had induced reverse apical ballooning or reverse Takotsubo [30]. Sympathetic response increases release of chemotactic and mitogenic factors, which may influence the progression of cardiovascular diseases through acceleration of atherosclerosis [31]. Current clinical recommendations for initiation of CNS stimulant agents are to obtain personal and family history of cardiovascular events such as, premature death, sudden death, long QT syndrome, abnormal heart rhythms and cardiomyopathy. It is recommended to monitor blood pressure and heart rate prior and during period of treatment [32]. Available studies do not support performing electrocardiogram as routine monitoring [33].
CONCLUSION
We report a case with multiple thromboembolic stroke and MI with severe LV dysfunction (EF <15%) in the setting of polysubstance abuse including amphetamines and marijuana (likely synthetic marijuana). This case emphasizes the importance of being aware that patients can present with multiple diagnoses. Amphetamines have hemodynamic effects and concomitant use of marijuana accelerates their cardiovascular effects by increasing catecholamine release. Our patient had severe global LV systolic dysfunction, unknown whether chronic or acutely stunned in the setting of STEMI. Studies are still limited to assess long term cardiovascular effects of CNS stimulants. Clinicians must be cautious in prescribing CNS stimulant agents. Precise personal, medical, drugs and medication history needs to be obtained before and during treatment.
REFERENCES
- Kessler RC, Adler L and Berkley R. (2006). The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. American Journal of Psychiatry. 163(4): 716-723.
- Visser SN, Danielson ML, Bitsko RH, Holbrook JR, et al. (2014). Trends in the parent-report of health care provider-diagnosed and medicated attention-deficit/hyperactivity disorder: United States, 2003-2011. J. Am. Acad. Child Adolesc. Psychiatry. 5334-5346.
- Anderson RJ, Reed WG and Hillis LD. (1982). History, epidemiology, and medical complications of nasal inhaler abuse. Clin. Toxicol. 19(1): 95-107.
- Anglin MD, Burke C, Perrochet B, Stamper E, et al. (2000). History of the methamphetamine problem. J Psychoactive Drugs. 32: 137-141.
- Sinha A, Lewis O and Kumar R. (2016). Amphetamine abuse related acute myocardial infarction. Case Reports in Cardiology. 1-6.
- Gandhi PJ, Ezeala GU and Luyen TT. (2005). Myocardial infarction in an adolescent taking Adderall. American Journal of Health-System Pharmacy. 62(14): 1494-1497.
- World Health Organization. (WHO). (2016). The health and social effects of nonmedical cannabis use. 62.
- Gerhard T, Winterstein AG and Olfson M. (2010). Preexisting cardiovascular conditions and pharmacological treatment of adult ADHD. Pharmacoepidemiology and Drug Safety. 19(5): 457-464.
- Sinha A, Lewis O and Kumar R. (2016). Adult ADHD Medications and Their Cardiovascular Implications. Case Rep Cardiol. 1-6.
- Jacobs LJ. (1989). Reversible dilated cardiomyopathy induced by methamphetamine. Clin Cardiol. 12(12): 725-727.
- Okie S. (2006). ADHD in adults. N Engl J Med. 354: 2637- 2641.
- Robison LM, Sclar DA and Skaer TL. (2005). Datapoints: trends in ADHD and stimulant use among adults: 1995– 2002. Psychiatr Serv. 56(12): 1497.
- (2007). US Food and Drug Administration. FDA News: FDA Directs ADHD Drug Manufacturers to Notify Patients About Cardiovascular Adverse Events and Psychiatric Adverse Events.
- (2007). Silver Spring, Md: US Food and Drug Administration. FDA Directs ADHD Drug Manufacturers to Notify Patients About Cardiovascular Adverse Events and Psychiatric Adverse Events.
- Ragland AS, Ismail Y and Arsura EL. (1993). Myocardial infarction after amphetamine use. Am Heart J. 125(1): 247-249.
- Lange RA, Cigarroa RG and Flores ED. (1990). Potentiation of Cocaine-Induced Coronary Vasoconstriction by BetaAdrenergic Blockade. Ann Intern Med. 112(12): 897-903.
- Kaye S, McKetin R, Duflou J and Darke S. (2007). Methamphetamine and cardiovascular pathology: a review of the evidence. Addiction. 102(8): 1204-1211.
- Treweek JB, Dickerson TJ and Janda KD. (2009). Drugs of abuse that mediate advanced glycation end product formation: a chemical link to disease pathology. Accounts of Chemical Research. 42(5): 659-669.
- Cohle SD. (2013). Fatal coronary artery intimal hyperplasia due to amphetamine use. Cardiovascular Pathology. 22(3): e1-e4.
- Haning W and Goebert D. (2007). Electrocardiographic abnormalities in methamphetamine abusers. Addiction. 102: 70-75.
- Qureshi AI, Suri MFK, Kirmani JF, Divani AA, et al. (2005). Is prehypertension a risk factor for cardiovascular diseases? Stroke. 36(9): 1859-1863.
- Mick E, McManus DD and Goldberg RJ. (2013). Metaanalysis of increased heart rate and blood pressure associated with CNS stimulant treatment of ADHD in adults. European Neuropsychopharmacology. 23(6): 534-541.
- Cooney MT, Vartiainen E, Laakitainen T, Juolevi A, et al. (2010). Elevated resting heart rate is an independent risk factor for cardiovascular disease in healthy men and women. American Heart Journal. 159(4): 612-619.
- Perret-Guillaume C, Joly L and Benetos A. (2009). Heart rate as a risk factor for cardiovascular disease. Progress in Cardiovascular Diseases. 52(1): 6-10.
- Ghuran A and Nolan J. (2000). The cardiac complications of recreational drug use. Western Journal of Medicine. 173(6): 412-415.
- Mugmon M. (2012). Atrial flutter with aberrant conduction in a patient taking amphetamine salts and caffeine. Journal of Community Hospital Internal Medicine Perspectives.
- Park JH, Kim KS, Sul JY, Shin SK, et al. (2011). Prevalence and patterns of left ventricular dysfunction in patients with pheochromocytoma. J Cardiovasc Ultrasound. 19: 76-82.
- Movahed A, Reeves WC, Mehta PM, Gilliland MG, et al. (1994). Norepinephrine-induced left ventricular dysfunction in anesthetized and conscious, sedated dogs. Int J Cardiol. 45: 23-33.
- Smith HJ, Roche AHG and Jagusch MF. (1976). Cardiomyopathy associated with amphetamine administration. 91(6): 792-797.
- Ramaraj R and Movahed MR. (2010). Reverse or inverted takotsubo cardiomyopathy (reverse left ventricular apical ballooning syndrome) presents at a younger age compared with the mid or apical variant and is always associated with triggering stress. Congest Heart Fail. 16(6): 284-286.
- Baumgartner HR and Hosang M. (1988). Platelets, platelet-derived growth factor and arteriosclerosis. Experientia. 44: 109-112.
- Gerhard T, Winterstein AG and Olfson M. (2010). Preexisting cardiovascular conditions and pharmacological treatment of adult ADHD. Pharmacoepidemiol Drug Saf. 19(5): 457-464.
- Vetter VL, Elia J and Erickson C. (2008). Cardiovascular monitoring of children and adolescents with heart disease receiving medication for ADHD: a scientific statement from the American Heart Association Council on Cardiovascular Disease in the Young Congenital Cardiac Defects Committee and the Council on Cardiovascular Nursing. Circulation. 117(8): 2407-2423.