Previous Issues Volume 2, Issue 1 - 2017
Left Pulmonary Artery Sling Misdiagnosed as Agenesia of Left Pulmonary Artery at the Postnatal Ultrasound Examination
Adjagba PM1 *, Sonou A2 , Codjo L3 , Hounkponou Amoussou-Guenou M1 , Eyissè Kpossou Y4 , Assani Moutaïrou S1 , Tchabi Y1 , Houénassi MD1
1Departementof cardiology, Teaching Hospital of Cotonou (CNHU), University of Abomey-Calavi (UAC),Bénin. 2Teaching Hospital of Ouémé and Plateau, Porto-Novo, University of Abomey-Calavi (UAC), Bénin 3Teaching Hospital of Borgou and Alibori, University of Parakou (UP), Parakou, Bénin 4Polyclinique Atinkanmè, Cotonou,Bénin
Corresponding Author: Philippe Mahouna Adjagba, Departementof cardiology, Teaching Hospital of Cotonou (CNHU), University of Abomey-Calavi (UAC), Bénin, Tel:+22997243282; E-Mail:[email protected]
Received Date: 23 Mar 2017 Accepted Date: 06 Apr 2017 Published Date: 10 Apr 2017
Copyright © 2017 Adjagba PM
Citation: Adjagba PM, Sonou A, Codjo L, Amoussou-guenou MH, et al. (2017). Left Pulmonary Artery Sling Misdiagnosed as Agenesia of Left Pulmonary Artery at the Postnatal Ultrasound Examination. Mathews J Cardiol. 2(1): 011.
ABSTRACT
Left pulmonary artery sling (LPAS) is a rare form of vascular ring, in which the left pulmonary artery (LPA) originates from the right pulmonary artery (RPA), runs posterior to the trachea and leads to an airway compression. We present the case of a 30 day old girl with delayed growth, respiratory distress and desaturation. Large Atrial Septal Defect (ASD), patent ductus arteriosus (PDA) and LPA agenesia/hypoplasia were reported as initial echocardiography findings. The diagnosis of LPAS with tracheal stenosis was finally made by CT-scan. The echocardiographic particularities of Left pulmonary artery sling (LPAS) may be known to avoid diagnostic errors. The cardiac scanner remains an excellent imaging tool for the confirmation and evaluation of the impairment on the tracheobronchial tree.
KEYWORDS
Left Pulmonary Artery Sling (LPAS); Tracheal Stenosis; Echocardiography; CT-Scan.
INTRODUCTION
Left pulmonary artery sling (LPAS) is a rare congenital condition in which the left pulmonary artery (LPA) originates from the right pulmonary artery (RPA) and encircles the distal trachea and right mainstem bronchus as it courses between the trachea and oesophagus to reach the helm of the left lung [1]. The presentation of LPAS varies from asymptomatic patients to infants with severe symptoms such as respiratory distress, stridor, wheezing, dyspnea, recurrent respiratory tract infections, and dysphagia caused by compression of the trachea, the esophagus or both. We present the case of a 30 day old girl with delayed growth, respiratory distress and desatura tion. Large Atrial Septal Defect (ASD), patent ductus arteriosus (PDA) and LPA agenesia were reported as initial echocardiog raphy findings. The diagnosis of LPAS with tracheal stenosis was finally made by CT-scan.
CASE REPORT
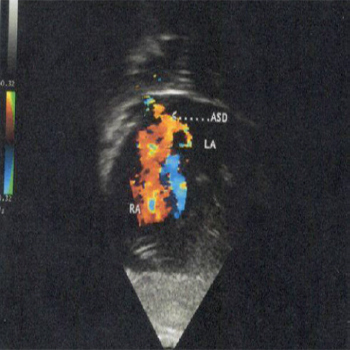
A 30 days- old-girl, birth weight 2550 g had stridor since birth. She was admitted to hospital for respiratory distress. Physical examination showed that her respiration was noisy and was associated with sternal retraction and desaturation up to 85%. She was treated like “bronchiolitis” and refered to cardiologist to rule out cyanotic congenital heart disease. Cardiac examination showed bunding pulses and large splitting of S2, and continuous heart mumur under left clavicular. Echocardiogram showed large ASD, large PDA and pulmonary hypertension (PHT) (Figures 1, 2).
Figure 1: Subcostal view, Doppler color showing ASD.
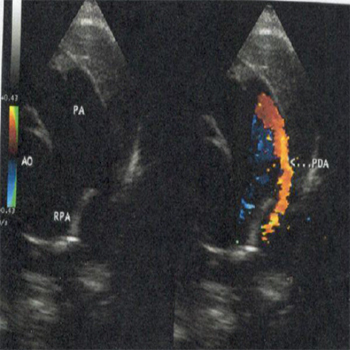
Figure 2: Parasternal short axis view, 2D and color Doppler comparison: showing PDA in the MPA (arrow).
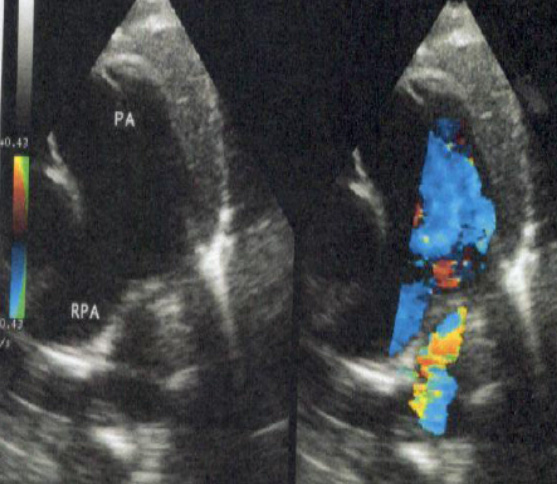
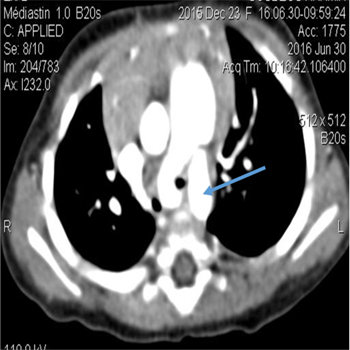
At 3 months and 5 months of age, she has been hospitalized for respiratory distress and deep desaturation. New echocardiogram was performed regarding the importance of respiratory symptoms and delayed growth. Given the impossibility of exposing the left pulmonary artery irrespective of the incidence (Figure 3), the diagnosis of agenesis / hypoplasia of the left pulmonary artery is evoked. A CT scan (Figure 4, 5), identified that the left PA was arising from the right PA running behind the trachea. The trachea is compressed at the level of its left arterial impression where it measures 2 mm of width versus 5 mm for the normal portion.
Figure 3: Parasternal short axis view, 2D and color Doppler : absence of pulmonary bifurcation.
Figure 4: CT scan showing, PA, PDA (arrow).
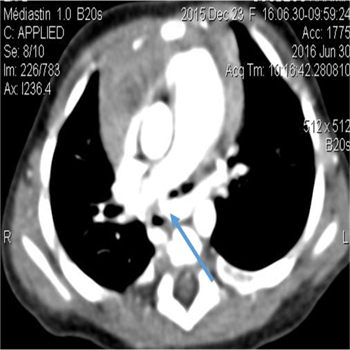
Figure 5: CT scan showing LPA (arrow) arising from RPA with a posterior course behind trachea and subsequent tracheal stenosis.
DISCUSSION
The exact incidence of LPAS is unknown. Coexisting diffuse tracheal stenosis is identified in up to 65% of case of LPAS [2]. In more recent serie, all patients with LPA sling presented with tracheal stenosis (100%), and there was a high incidence of combined right tracheal bronchus (22%), underdeveloped right lung (22%), persistent left superior vena cava (22%), and left patent ductus arteriosus (39%) [3]. Our patient showed important tracheal stenosis, which was responsible of respiratory distress. We did not find another tracheobronchial or pulmonary impairment. Pierron C et al. reported 2 cases of right pulmonary aplasia with the left pulmonary artery sling responsible for severe respiratory symptoms [4]. Tracheobronchial and pulmonary impairment associated with LPAS had widely reported [2-5]. Diagnosis of LPAS by echocardiography is almost always possible, but requires increased [6, 7] alertness if other intracardiac and/or vascular disorders (LPA hypoplasia) coexist [7]. The presence of PDA especially when it’s wide may be a diagnosis trap. In case, the LPA is missing, the two main diagnoses to eliminate are LPAS sling and isolated pulmonary artery when LPA arises from the aorta. For echo diagnosis, the basic rule is a thorough assessment of the division, region of the pulmonary trunk [7]. In LPAS, the echocardiographic presentation is usually characteristic. Firstly, there is no division of the pulmonary trunk. In addition, the pulmonary trunk runs more to the right and the RPA constitutes its extension. The lack of the division is striking and the vessel, which is directed to the dorsal side and originates from the posterior wall of the RPA, is not visible until the wall’s middle part [7]. High left parasternal view: the most useful for the diagnosis of the sling. Other diagnosis tools are chest radiograph, barium swallow, computed tomography (CT), magnetic resonance imaging (MRI) arteriography or bronchoscopy. In this case report, diagnosis was finally made by computed tomography (CT). Congenital heart defects are found in 50% of LPAS cases, the most common being atrial and ventricular septal defects, patent ductus arteriosus, left superior vena cava, and tetralogy of Fallot [8]. The associated congenital heart disease showed by in this case report are ASD, PDA. PHT may be the consequence of the tracheal stenosis.
CONCLUSION
LPAS is a rare congenital heart disease. The echocardiographic presentation is usually characteristic. A supra sternal echocardiography examination targeted for LPAS should be performed for all patients presenting symptoms compatible with LPAS. CT-scan, as second-line investigations in diagnosis of LPAS should be performed for every patient suspected of having a LPAS even when echocardiography in negative.
REFERENCES
- Potts WJ, Holinger PH and Rosenblum AH. (1954). Anomalous left pulmonary artery causing obstruction to right main bronchus: report of a case. J Am Med Assoc.155: 1409-1411.
- Berdon WE, Baker DH, Wung JT, Chrispin A, et al. (1984). Complete cartilage-ring tracheal stenosis associated with anomalous left pulmonary artery: the ring-sling complex. Radiology. 152: 57-64.
- Chen SJ, Lee WJ, Lin MT, Wang JK, et al. (2007). Left pulmonary artery sling complex: computed tomography and hypothesis of embryogenesis. Ann Thorac Surg. 84(5): 1645-50.
- Pierron C, Sigal-Cinqualbre A, Lambert V and Le Bret E. (2011). Left pulmonary artery sling with right lung aplasia. J Pediatr Surg. 46(11): 2190-4.
- Backer CL, Mongé MC, Popescu AR, Eltayeb OM, et al. (2016). Vascular rings. Semin Pediatr Surg. 25(3): 165-75.
- Lai WW, Mertens LL, Co- hen MS and Geva T (red). (2009). Echocardiography in Pediatric and Congeni-tal Heart Disease: From Fetus to Adult. Blackwell Publishing g 523–536.
- Madry W and Karolczak MA. (2013). Ultrasound diagnosis of pulmonary sling with proximal stenosis of left pulmonary artery and patent arterial duct. J Ultrason. 13(52):104-110.
- Backer CL, Mavroudis C, Dunham ME and Holinger LD. (1999). Pulmonary artery sling: results with median sternotomy, cardiopulmonary bypass, and reimplantation. Ann Thorac Surg. 67: 1738-1744.