Information Links
Related Conferences
Previous Issues Volume 8, Issue 3 - 2023
Histopathological Patterns of Cervical Cancer among Females Presenting to a Pathology Core Reference Laboratory in Kampala, Uganda: A 5-Year Review
Mwanja Moses1,*, Lopwonya Fred2
1School of Medicine, College of Health & Medicine, King Ceasor University, Bunga Hill, Kampala, Uganda
2School of Biomedical Sciences, College of Health Sciences, Makerere University, Kampala, Uganda
*Corresponding author: Mwanja Moses, School of Medicine, College of Health & Medicine, King Ceasor University, Bunga Hill, P. O. Box 88, Kampala, Uganda; Tel: +256 756575899; Email: [email protected]
Received Date: August 24, 2023
Publication Date: September 11, 2023
Citation: Moses M, et al. (2023). Histopathological Patterns of Cervical Cancer among Females Presenting to a Pathology Core Reference Laboratory in Kampala, Uganda: A 5-Year Review. Mathews J Cancer Sci. 8(3):42.
Copyright: Moses M, et al. © (2023)
ABSTRACT
Introduction: Cervical cancer ranks fourth in global female cancer cases, with about 604,000 new cases and 342,000 deaths in 2020. It's most prevalent in low- and middle- income countries, particularly in sub-Saharan Africa. In Uganda, cervical cancer is the leading cause of cancer-related sickness and death, with approximately 6,959 new cases and 4,607 deaths in 2020. Understanding the histopathological types of cervical cancer is crucial for treatment and prognosis, but there's limited data in Uganda. This study aimed to identify cervical cancer histopathology patterns in females at Makerere University's pathology reference laboratory. Methodology: A retrospective cross-sectional study at Makerere University's pathology reference laboratory collected quantitative data on cervical cancer diagnoses via histology from 2017 to 2021. Data analysis was descriptive, utilizing SPSS version 21. Results: The study included 120 patients spanning from 2017 to 2021, with an average age of 45.53 (SD 13.02) years, ranging from 21 to 80 years. Cervical cancer was most common among women aged 35 to 54 years (67 or 55.8%) and those with HIV infection (26 or 21.7%). Squamous cell carcinoma was the predominant cervical cancer type, observed in 102 cases (85%), followed by adenocarcinoma (7 cases or 5.8%) and adenosquamous (5 cases or 4.2%) histological patterns. Conclusions: Cervical cancer is most common in HIV-positive women and those aged 35-55. Squamous cell carcinoma is the prevailing type, affecting 9 out of 10 patients. Screening all HIV-positive and women aged 35+ is advised.
Keywords: Cervical cancer, Histopathological patterns, Uganda
INTRODUCTION
Cervical carcinoma is a malignant neoplasm that arises from the cervical epithelium, particularly the transformation zone. It begins with a prolonged pre-invasive phase, involving abnormal growth of cervical epithelial cells, known as cervical intraepithelial neoplasia (CIN). These changes can either resolve naturally or advance to invasive carcinoma when untreated [1].
Persistent infection with Human papillomavirus (HPV) infection is the primary etiological factor for cervical carcinoma. HPV is responsible for 99.7% of cervical cancer and infects 75 - 80% of sexually active adults at some point, however, it can be cleared by the body’s immune system most of the time and is preventable. Over 200 types of HPV are currently known, most are not associated with cervical cancer or genital warts [2]. The High-risk types (16, 18) are associated with cancer and the low-risk types (6, 11) are associated with genital warts [3].
Worldwide, cervical cancer is the fourth most frequent cancer in women with an estimated 604 000 new cases in 2020. Of the estimated 342,000 deaths from cervical cancer in 2020, about 90% of these occur in low- and middle-income countries [3]. Women living with HIV are 6 times more likely to develop cervical cancer compared to women without HIV, and an estimated 5% of all cervical cancer cases are attributable to HIV [4].
In Uganda, the crude incidence rate of cervical cancer is estimated at 30 per 100 000, while the mortality rate is estimated at 19.9 per 100 000. Cervical cancer is the number one cause among women of both age-standardized cancer-related incidence and cancer- related deaths from all cancers in Uganda [5]
Like in other parts of the world, the involvement of human papillomavirus (HPV) infection in this malignancy in Uganda is comparable to the rest of the world with HPV-16 and HPV- 18 as the major oncogenic strains [6]. A 2011 review reported several estimates of high- risk HPV prevalence from 20 studies, ranging from 10.2% to 40% among HIV-negative women and ranging from 37% to 100% among HIV-positive women. The HPV prevalence estimates among women with normal cytology included in the HPV Information Centre report range from as low as 15.2% in women aged 25-60 to as high as 73.2% in women aged 12-24 [7]. Most of the prevalence studies were conducted before the introduction of the HPV vaccination programs in Uganda; therefore, these estimates may not reflect the current situation.
The WHO recommends a screen-and-treat strategy to reduce the incidence of cervical cancer [3]. The target age group is women 25 to 49 years old. Screening occurs every 3 years for HIV-negative women and annually for HIV-positive women. Midwives and nurses are the primary providers of cervical cancer screening as well as treatment [8]. The screening methods include visual inspection with acetic acid (VIA), visual inspection with Lugol’s iodine (VILI), colposcopy, and HPV testing and pap smear. Patients who screen positive should undergo histological confirmation for diagnosis of cervical intraepithelial neoplasia (CIN) or cervical carcinoma [1].
Before enrollment of patients for cervical cancer treatment, a diagnostic or confirmatory test must be done to make a definitive diagnosis or confirmation of pre-cancer or cancer lesions [7]. Colposcopy, biopsy and endocervical curettage (ECC) are the most commonly used diagnostic tests for cervical cancer. Colposcopy and endocervical curettage are not routinely done in Uganda, and thus biopsy is the gold standard for the diagnosis of cervical cancer in Uganda. A biopsy is used to determine the degree of abnormality of the cell changes at the cervix and to rule out cancer. After examination, the result is classified as normal, as cervical intraepithelial neoplasia (CIN), or as invasive carcinoma. The precancerous lesions are classified as low-grade (CIN1) or high-grade (CIN2 and CIN3, collectively referred to as CIN2+) pre-cancer. The World Health Organization (WHO) categorizes cervical intraepithelial neoplasia (CIN) according to the depth of the abnormal epithelial proliferation relative to the basement membrane. The proportion of cervical epithelium exhibiting dysplastic cells determines the grade of the dysplasia. Specifically, CIN is classified as low-grade (CIN1), if the abnormal epithelial proliferation extends less than one-third of the thickness of the epithelium; as high-grade (CIN2), if the abnormal epithelial proliferation extends for more than one-third but less than two-thirds of the thickness of the epithelium; and CIN3, if the abnormal epithelial proliferation extends for more than two-thirds of the thickness of the epithelium. Dysplasia becomes cancer when it invades the basement membrane. For cancerous lesions, the histological pattern of the malignancy is also determined [1].
There are many histopathological patterns of cancer of the cervix. This must be determined as it influences the treatment and prognosis of the disease. The common histopathological patterns are Squamous cell carcinoma (SCC), adenocarcinoma, adenoid cystic carcinoma, adeno-squamous carcinoma, clear cell carcinoma and mucinous carcinoma. Some of the tumors can be well-differentiated, moderately differentiated or poorly differentiated tumors [9]. This study aims to assess the histopathological patterns of cervical cancer in Uganda.
The commonest histological type of cervical cancer is squamous cell carcinoma (85-90%) either well-differentiated or moderately or poorly differentiated. The sources of the squamous epithelium that turn into malignancy arise from a squamocolumnar junction or squamous metaplasia of the columnar epithelium. Squamous cell carcinoma is further subdivided histologically into three groups: (i) large cell keratinizing, (ii) large cell non- keratinizing and (iii) small cell type. Patients with small cell type have got poor prognosis compared to the large cell types. There’s also a rare type; basaloid squamous cell carcinoma (BSCC) which is an aggressive variant of oral squamous cell carcinoma. Some patients present with adenocarcinomas, and others less commonly with mixed carcinomas (features of both squamous cell carcinoma and adenocarcinoma) of the cervix [10].
Other histopathological patterns of cervical cancer are adenocarcinoma (10–15%) which develops from the endocervical canal, either from the lining epithelium or from the glands. Currently increased number of cervical adenocarcinomas is observed especially in the younger age group. The majority (80%) of them are purely endocervical type. The remainders are endometrioid, clear cell, adenosquamous or a mixed type. Adenoma- malignum is an extremely well-differentiated adenocarcinoma with a favourable prognosis. Neuroendocrine tumors, sarcomas and lymphomas are rare tumors of the cervix [10,11].
In a review conducted in Nigeria, poorly differentiated squamous cell carcinoma was the leading variants of cervical cancer. Squamous cell carcinoma (SCC) was seen in 90.8% of patients while 7.1% of patients had adenocarcinoma. One patient each had adenoid cystic carcinoma, adenosquamous carcinoma, clear cell carcinoma and mucinous carcinoma [9]. In the same study, the majority of the patients, (50.5%) had poorly differentiated tumors, 32.7% had well-differentiated tumors, and the rest 16.8% had moderately differentiated tumors [9].
In another review conducted in India, the most common malignancy was squamous cell carcinoma (88.1 %) among which moderately differentiated squamous cell carcinoma comprised (73.1 %) followed by well-differentiated squamous cell carcinoma (11.3 %) and poorly differentiated (3.7 %). Other variants of cervical cancer were papillary, adenosquamous and basaloid variants [12].
In a study done in Kenya in East Africa, the most prevalent histological type of cervical cancer was squamous cell carcinoma (SCC) (89.9%), followed by adenocarcinoma (AC) (5.6%). Two patients had anaplastic carcinoma, and another two had sarcoma of the cervix. Among those with SCC, most had moderately differentiated SCC (39.2%), with 32.0% and 21.3% having poorly differentiated and well-differentiated diseases respectively. At the time of diagnosis, the majority of patients (80.5%) presented with stage 2B disease or above [13].
Since histopathology is a cornerstone in the detection and diagnosis of cervical cancer, studies have studied how histopathological classification of cervical cancer influences the management, treatment and surveillance planning of newly diagnosed cervical cancer. A study conducted in the United States using the United States Surveillance, Epidemiology, and End Results (SEER) population data found that Small cell carcinoma and adenocarcinomas were generally associated with poorer survival [14]. In the same study, cause-specific mortality hazard ratios by histological type relative to non-micro-invasive squamous cell carcinoma were: micro-invasive squamous cell carcinoma 0.28, carcinoma not otherwise specified 0.91, non-mucinous adenocarcinoma 1.06, adenosquamous carcinoma 1.35, mucinous adenocarcinoma 1.52 and small cell carcinoma 1.94. This study therefore greatly highlights the importance of histopathological classification of cervical cancer in determining treatment choices, morbidity and mortality due to the disease [14].
Despite known histopathological patterns of cervical cancer in different countries, the case is different for Uganda. There is a knowledge gap regarding histopathological patterns of cervical cancer among cervical cancer patients in Uganda. The purpose of this study was to address the gap.
Problem Statements
The global burden of cervical cancer is heavily concentrated in low- and middle-income countries (LMICs), having the highest rates in sub-Saharan Africa (SSA) [15]. In Uganda, due to an increased burden of HIV, the prevalence, morbidity and mortality from cervical cancer have been increasing in recent years. Uganda ranks seventh in the world for cervical cancer incidence, with an estimated rate of 56.2 per 100,000 people in 2020 (compared to a global rate of 13.3) [16]. Cervical cancer is the leading cause of cancer morbidity and mortality in Ugandan women with an estimated 6959 new cases and 4607 deaths in 2020 [16].
The histopathological differentiation of cervical cancer is a major determinant in treatment options for cervical cancer and is a major determinant of the prognosis of the disease. For example, a study done in Romania demonstrated that cervical cancer patients with adenocarcinomas and adenosquamous carcinomas had a significantly poorer treatment response to chemo-radiotherapy than those with squamous cell carcinomas [17]. There is a paucity of data regarding the histopathological cervical cancer patterns in Uganda. This makes it difficult to plan for appropriate treatment modalities aimed at maximizing treatment benefits for cervical cancer patients.
Justification
Histopathology and cytopathology form the scientific and clinical basis for the current prevention and treatment of cervical cancer. Histopathology determines the treatment of cancer and precancer by classifying into a diagnosis the patterns of microscopic organization of cells in tissue sections from biopsy or surgical specimens. Understanding the histopathological patterns of cervical cancer in Uganda will provide a basis for designing interventions to reduce cervical cancer morbidity and mortality. This will help reduce cancer-related deaths and will lead to socioeconomic transformation.
OBJECTIVES
General Objective
To determine the common histologic patterns of cervical cancer among females presenting to Makerere University pathology core reference laboratory.
Specific Objective
To determine the factors associated with cervical cancer among females presenting to Makerere University pathology core reference laboratory.
MATERIALS AND METHODS
Study Design
This was a quantitative retrospective cross-sectional study. This study design helped the researcher collect enough information for a period of 5 years in a short period.
Study Area
The study was conducted within the Makerere University pathology core reference laboratory found at Makerere University College of Health Sciences in Mulago Hill, Kampala Uganda. The Makerere University pathology laboratory is a core reference laboratory in Uganda receiving different types of specimens from all over the country. Therefore, the information generated on cervical cancer patterns could be representative of the whole of Uganda.
Study Population
The study population were cases of cervical cancer that had histology done from Makerere University pathology core reference laboratory from 2017 to 2021 as documented in the laboratory Health Management Information System (HMIS) books.
Selection Criteria
This includes both inclusion and exclusion criteria
Inclusion criteria
1. Patients with a positive cervical cancer histology done from Makerere University pathology core reference laboratory.
2. Patient information must have been recorded in the HMIS books or the computer
3. The histological diagnosis must have been made from 2017 to 2021
Exclusion criteria
1. Patient information is incomplete such as unspecified type of cervical cancer. A total of 5 studies were excluded from the study due to missing information. This was mainly due to the poor handwriting of the technician as the written information could not be read by the researcher during data collection.
Sample size determination
Total population sampling was used and therefore all reports belonging to patients that met the inclusion /exclusion criteria were recruited in the study.
Sampling technique
The total population were captured and processed for data analysis.
Data collection methods
The data collection guide was developed and then exported to a mobile data collection platform. For this purpose was therefore transferred from laboratory HMIS books to Epicollect 5.
Data analysis
The Data collected was analyzed using SPSS version 21.
Quality control
Pre-testing of the data collection tool was done before starting data collection to ensure that the tool was able to capture all necessary information. Only complete information was entered into the mobile data collection tool.
Ethical considerations
Ethical approval was obtained from the School of Biomedical Sciences Institution Review Board. Administrative clearance was obtained from Makerere University pathology core reference laboratory. Privacy and confidentiality of patient information were mentioned all the time by concealing patient identifiers and using strong passwords in computers containing patient data.
Dissemination of results
A dissertation has been written and shared with Sir Albert Cook library at Makerere University College of Health Sciences, Uganda Cancer Institute and Uganda Ministry of Health. A peer-reviewed publication will be written. Presentation of findings at both national and international conferences will be made.
RESULTS
Table 1: Sociodemographic characteristics of respondents.
|
Variable |
Frequency |
Percentage |
|
Age |
||
|
Less than 35 |
21 |
17.5 |
|
35 -44 |
34 |
28.3 |
|
45-54 |
33 |
27.5 |
|
55-64 |
21 |
17.5 |
|
65-80 |
11 |
9.2 |
|
Tribe |
||
|
Muganda |
49 |
40.8 |
|
Munyankole |
15 |
12.5 |
|
Musoga |
9 |
7.5 |
|
Munyoro/Mutoro |
6 |
5.0 |
|
Others |
41 |
34.2 |
A total of 120 patients from 2017 to 2021 were recruited into the study. The mean age of the patients was 45.53 (Standard deviation 13.02), the youngest patient was 21 years and the oldest was 80 years of age. Cervical cancer was more prevalent in women aged between 35 to 54 years 67(55.8%).
Table 2: Associated conditions and Stage at diagnosis
|
Variable |
Frequency |
Percentage |
|
Associated condition |
||
|
HIV/AIDS |
26 |
21.7 |
|
Pregnancy |
4 |
3.3 |
|
Confirmed HPV infection |
11 |
9.2 |
|
Family history of cervical cancer |
3 |
2.5 |
|
None of the above |
76 |
63.3 |
|
Stage at diagnosis |
||
|
Localized |
24 |
20.0 |
|
Local spread |
32 |
26.7 |
|
Regional spread |
4 |
3.3 |
|
Distant metastases |
3 |
2.5 |
|
Stage not determined |
57 |
47.5 |
The majority of cervical cancer patients had associated HIV infection 26(21.7%). The stage of cervical cancer at the time of diagnosis for the majority of the patients 57 (47.5%) could not be determined. However, 24 (20.0%) patients had cervical cancer localized, 32 (26.7%) had a local spread and 3 (2.5%) patients had distant metastases.
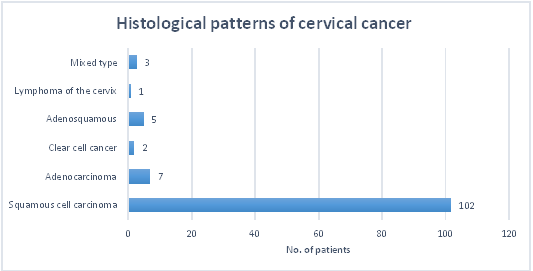
Figure 1: Histopathological patterns of cancer.
Squamous cell carcinoma present in 102 (85%) patients was the most prevalent pattern of cervical cancer. This was followed by adenocarcinoma 7 (5.8%) and adenosquamous 5 (4.2%) histological patterns of cervical cancer.
DISCUSSION
This study showed that cervical cancer was more prevalent in women aged between 35 to 54 years with an average age of diagnosis at 45.53 years. The findings are consistent with the 2022 American Cancer Society key statistics which reported that cervical cancer is most frequently diagnosed in women between the ages of 35 and 44 with the average age at diagnosis being 50 [18]. The prevalence of cervical cancer increases with age due to long-lasting infection with certain types of human papillomavirus (HPV) among women, which later causes cervical cancer due to diminished immune functioning associated with an increase in age.
The present study demonstrates that the majority of cervical cancer patients had associated HIV infection. The findings are consistent with a report from WHO which showed that women living with HIV are 6 times more likely to develop cervical cancer compared to women without HIV [3]. HIV is responsible for around 5% of all cervical cancer cases worldwide and is the leading cause of death among women living with HIV [19]. Although the mechanism by which HIV increases the risk of cervical cancer is not completely understood, studies suggest that HIV-induced immunosuppression leads to an inability to control the expression of HPV and the production of HPV oncoproteins E6 and E7 [20,21]. This risk appears to be associated with increased HPV persistence that may result from immunosuppression related to HIV [22].
In the present study, squamous cell carcinoma patients were the most prevalent cervical cancer pattern (85%). This was followed by adenocarcinoma 5.8% and adenosquamous 4.2% histological patterns of cervical cancer as seen in Figure 1. The findings of this study correspond to findings of a study done in 2000 which reported that was accounted for three-fourths of all cervical cancers [23]. In the same study, adenocarcinoma and adenosquamous cell carcinoma represent 10–15%, and other or unspecified histology represents the remaining 10–15% [23]. However, a study in 2007 reported an overall increasing number of adenocarcinomas and adenosquamous carcinomas [14]. A predominance of SCC in Uganda implies that treatment of cervical cancer with chemotherapy would increase the chances of response to treatment and decline in mortality. This is because SCC is associated with higher chances of survival than other histological such as small cell carcinoma, several subtypes of adenocarcinoma- mucinous, clear cell, and common types of adenocarcinoma- and adenosquamous carcinoma [14].
CONCLUSIONS, LIMITATIONS AND RECOMMENDATIONS
CONCLUSIONS
1. Cervical cancer is more prevalent among women suffering from HIV and older women aged between 35 to 54 years.
2. Squamous cell carcinoma is the most prevalent pattern of cervical cancer in Uganda present in every 9 out of 10 cervical cancer patients.
LIMITATIONS
The data's accuracy relied on the pathologist's expertise, raising questions about reliability. This study, conducted in a single laboratory, offers valuable but limited insights into Uganda's cervical cancer patterns. Handwriting issues from technicians and limited clinician-provided information were additional challenges.
RECOMMENDATION
1. Routine screening of all HIV-positive women and women aged 35 years and above is recommended.
2. Further follow-up studies are warranted.
DECLARATIONS
Ethics Approval and Consent to Participate
The study received all required ethical approval and privacy and confidentiality were observed.
Consent for Publication
Not applicable.
Availability of Data and Materials
All information fronted in this article can be retrieved from the Makerere University, Pathology laboratory. The authors can also avail the raw data.
Competing Interests
The authors declare no competing interests
Author’s Contributions
MM conceptualized the context and methodology of the study and was the major contributor and editor of the manuscript.
LF did the data collection from the laboratory, analysis and interpretation.
Both authors read and approved the final manuscript.
Funding
This study was not funded
Acknowledgements
Not applicable
REFERENCES
Uganda Cancer Institute. (2017). Cervical Cancer Information, education and communication booklet for health workers, First. Kampala: Uganda Cancer Institute.
HPV reference clones. (2022). hpvcenter. (https://www.hpvcenter.se/human_reference_clones/)
WHO. (2022). Cervical Cancer, (https://www.who.int/news- room/fact-sheets/detail/cervical-cancer)
Stelzle D, Tanaka LF, Lee KK, Ibrahim Khalil A, Baussano I, Shah ASV, et al. (2021). Estimates of the global burden of cervical cancer associated with HIV. Lancet Glob Heal. 9(2):e161–e169.
Nakisige C, Trawin J, Mitchell-Foster S, Payne BA, Rawat A, Mithani N, et al. (2020). Integrated cervical cancer screening in Mayuge District Uganda (ASPIRE Mayuge): a pragmatic sequential cluster randomized trial protocol. BMC Public Health. 20(1):142.
Yousif HM, Albasri AM, Alshanqite MM, Missawi HM. (2019). Histopathological Patterns and Characteristics of Abnormal Cervical Smear in Madinah Region of Saudi Arabia. Asian Pac J Cancer Prev. 20(5):1303–1307.
PRESCRIP-TEC project. (2021). About cervical cancer in Uganda. (https://prescriptec.org/countries/uganda/)
Nakisige C, Schwartz M, Ndira AO. (2017). Cervical cancer screening and treatment in Uganda. 20:37-40.
Abdus-salam AA, Eriba LO, Abdus-salam RA, Dawotola DA. (2013). Histolopathological Patterns of Cervical Carcinoma Seen at A Radiotherapy Centre in Ibadan, Nigeria. Nig Q J Hosp Med. 23(4):334-337.
Dutta DC. (2013). Dutta’s test book of gynecology. Jaypee Brothers Medical Publishers (P) Ltd.
Vinay K, Abul KA, Jon CA. (2013). Robbins Basic Pathology. Elsevier.
Priya T, Indumati B. (2020). Retrospective Histopathological Analysis of Cervical Cancer in a Tertiary Care Center. J Evol Med Dent Sci. 9(47):3523–3527.
Maranga IO, Hampson L, Oliver AW, Gamal A, Gichangi P, Opiyo A, et al. (2013). Analysis of Factors Contributing to the Low Survival of Cervical Cancer Patients Undergoing. PLoS One. 8(10):e78411.
Vinh-Hung V, Bourgain C, Vlastos G, Cserni G, De Ridder M, Storme G, et al. (2007). Prognostic value of histopathology and trends in cervical cancer: a SEER population study, BMC Cancer. 7(1):164.
Beyer K, Kasasa S, Anguzu R, Lukande R, Nambooze S, Amulen PM, et al. (2022). High-resolution disease maps for cancer control in low-resource settings: A spatial analysis of cervical cancer incidence in Kampala, Uganda. J Glob Health. 12:04032.
Globocan. (2020). Uganda. (https://gco.iarc.fr/today/data/factsheets/populations/800-uganda-fact-sheets.pdf.)
Voinea S, Herghelegiu CG, Sandru A, Ioan RG, Bohilțea RE, Bacalbașa N, et al. (2021). Impact of histological subtype on the response to chemoradiation in locally advanced cervical cancer and the possible role of surgery. Exp Ther Med. 21(1):93.
American Cancer Society. (2022). Key Statistics for Cervical Cancer.
Kahesa C, Mwaiselage J, Wabinga HR, Ngoma T, Kalyango JN, Karamagi CA. (2008). Association between invasive cancer of the cervix and HIV-1 infection in Tanzania: the need for dual screening. BMC Public Health. 8(1):262.
Newfield L, Bradlow HL, Sepkovic DW, Auborn K. (1998). Estrogen Metabolism and the Malignant Potential of Human Papillomavirus Immortalized Keratinocytes. Proc Soc Exp Biol Med. 217(3):322–326.
Ngwalle EW, Mgaya HN, Mpanju-Shumbusho W, Chirenje ZM, Kirumbi L, Lebelle T, et al. (2001). Situational analysis for diagnosis and treatment of cervical cancer in mainland Tanzania. East Afr Med J. 78(2):60-64.
Hawes SE, Critchlow CW, Sow PS, Touré P, N'Doye I, Diop A, et al. (2006). Incident high-grade squamous intraepithelial lesions in Senegalese women with and without human immunodeficiency virus type 1 (HIV- 1) and HIV-2. J Natl Cancer Inst. 98(2):100–109.
Vizcaino AP, Moreno V, Bosch FX, Muñoz N, Barros-Dios XM, Borras J, et al. (2000). International trends in incidence of cervical cancer: II. Squamous-cell carcinoma. Int J cancer. 86(3):429–435.