Information Links
Related Conferences
Previous Issues Volume 7, Issue 2 - 2022
Giant Pedunculated Liver Hemangioma Torsion a Rare Clinical Presentation, Case Report
Ali Akbariyan Mohsen, Ansari Majid*
Surgical Oncology Research Center, Emam Reza Hospital, Mashhad University of Medical Sciences, Iran
Received Date: May 07, 2022
Published Date: July 18, 2022
*Corresponding Author: Ansari Majid, Endoscopic and Minimally Invasive Surgery Research Center, Ghaem Hospital, Mashhad University of Medical Sciences, Iran. Tel: +989153230207 E-mail: [email protected]
Citation: Ansari M, et al. (2022). Giant Pedunculated Liver Hemangioma Torsion a Rare Clinical Presentation, Case Report. Mathews J Case Rep. 7(2):72.
Copyright: Ansari M, et al. © (2022).
ABSTRACT
Introduction: Hemangioma is the most common benign tumor of liver but pedunculated liver hemangioma is not a common clinical presentation. In addition complicated liver pedunculated hemangioma with torsion is an extremely rare clinical manifestation of liver hemangioma. Case presentation: A 58 years old woman with acute abdominal pain. After clinical investigation it was found that she had torsion of giant pedunculated liver hemangioma and she was undergone laparoscopic resection of hemangioma. Discussion: The most common benign tumor of liver is hemangioma, but pedunculated type is not common and complicated with torsion is extremely rare condition and only a few cases have been reported. It is more occur in left liver lob and more than half of cases are asymptomatic. Our patient had acute abdominal pain. She had left liver lob originated pedunculated hemangioma which was complicated with torsion. Conclusion: Pedunculated liver hemangioma is a rare type of liver hemangioma but it can be one of the possible causes of acute abdominal pain if it is complicated.
Keywords: Pedunculated Liver Hemangioma, Torsion, Case Report
INTRODUCTION
The most common benign tumor of liver is hemangioma (0.4%-20% in necropsies). It is more common in women and it is present as a solitary lesion which is usually found in the posterior segments of the right liver lob. Exophytic liver hemangiomas, especially pedunculated hemangiomas, are very rare and only a few cases have been reported in literature. There is some disagreement about size criteria, but generally hemangiomas over 10 cm are called giant hemangiomas [1].
Hemangiomas are liver vascular malformations which is not commonly symptomatic. Hemangiomas are often asymptomatic without growth in size and only less than 10% of cases undergo enlargement [2].
Physical examination is usually normal and only rarely cases are presented as a large abdominal masses with arterial murmur in right upper quadrant. Different ways of imaging such as ultrasound, computed tomography (CT) scan and magnetic resonance imaging (MRI) with sensitivity more than 90% and specificity between 55%-85% are used as diagnostic manners of liver hemangiomas. Only the symptomatic or complicated hemangiomas should be treated and the first option is surgery (96% improvement of symptoms) [3].
According to Chi D. Ha et al. report of published English literature about pedunculated liver hemangioma; they were more common in females, less than 50% of cases were symptomatic, around 85% of cases had typical CT scan findings and left liver lob was significantly more common than right for pedunculated liver hemangioma presentation [4].
CASE PRESENTATION
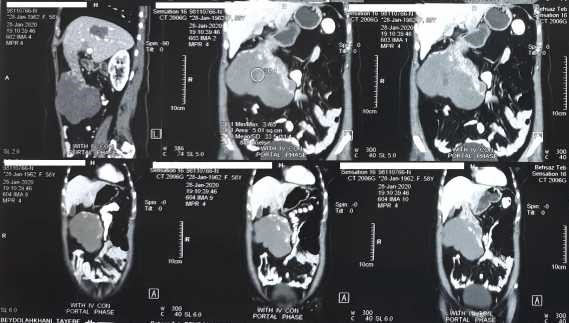
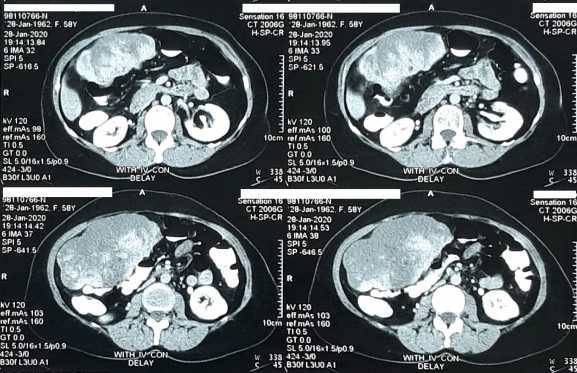
A 58 years old woman with acute progressive abdominal pain in upper abdomen was referred to our hospital (Sina Hospital in Mashhad, Iran). She had abdominal pain since 3 days ago which was more severe in right upper quadrant. She had no drug consumption history or alcohol abuse and also smoking. In physical examination she had tenderness in right upper abdomen without rebound and mass like lesion was palpable in right upper quadrant. In laboratory tests there were not any abnormal findings. It was shown a pedunculated 13.2 cm diameter liver hemangioma with torsion signs by abdominal CT scan with IV and oral contrast (Figure1, 2).
Figure1. Coronal and sagittal CT scan with IV and oral contrast
Figure 2. Axial abdominal CT scan with IV and oral contrast
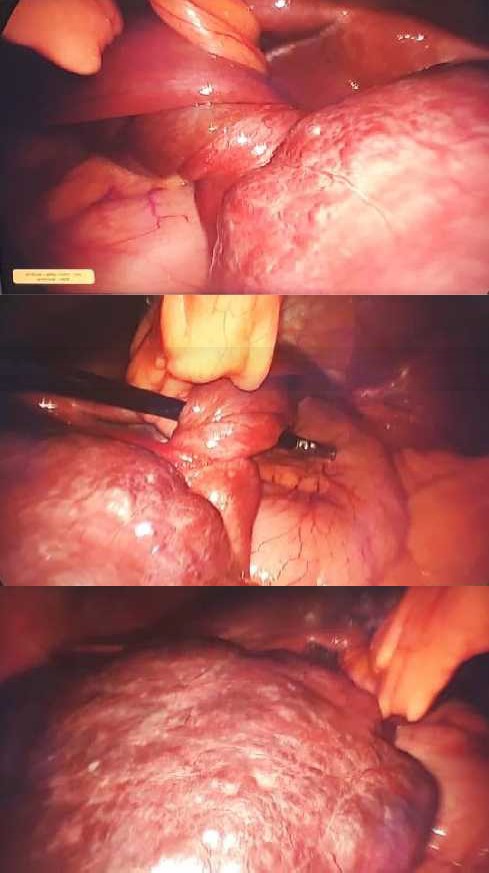
She was undergone laparoscopic resection of pedunculated liver hemangioma (Figure 3).
Figure3. Laparoscopic intraoperative images of pedunculated liver hemangioma with torsion around its stalk and originated from left liver lob.
Hemangioma was originated from left hepatic lob; specimen was extracted through a 7 cm midline incision. The patient was discharged after 2 days of surgery with good condition and in pathologic finding report the mass was cavernous hemangioma without malignancy.
DISCUSSION
The most common benign tumor of liver is hemangioma, on the other hand pedunculated liver hemangiomas are very rare and only a few cases have been reported [1]. Only 24 cases of pedunculated liver hemangiomas have been reported up to date worldwide according to Al Farai A et al. [5]. Pedunculated liver hemangioma according to Chi D. Ha et al., report of published English literature is more occur in left liver lob and more than 50% of cases are asymptomatic [4]. In our case, pedunculated liver hemangioma was originated from left liver lob, but it was symptomatic. The average size of tumor is 8.6 cm (3.5-15), average age of patients is 53 years old (35-71) and 85% of cases have typical CT scan findings [4]. In this case report the patient was 58 years old with typical CT scan finding of pedunculated liver hemangioma. Pedunculated liver hemangioma is a very rare lesion which is presented as an extrahepatic mass with attachment to the liver by a thin pedicle that is not visible all-time in imaging [6, 7]. Unlike this in our patient the pedicle is seen in CT scan images. Pedunculated liver hemangiomas can undergo torsion around their long mobile pedicles and may become symptomatic and the most frequent symptom is pain [8]. Like our case who had abdominal pain duo to torsion of hemangioma around its stalk. Male to female ratio for liver hemangioma in-hospital patients is 1:1.9 and cavernous hemangioma is the most common pathological type of liver hemangioma [9]. In this case also the patient was a woman with cavernous giant liver hemangioma without malignancy in pathological report.
CONCLUSION
Pedunculated liver hemangioma is a rare type of liver hemangioma in addition complicated pedunculated liver hemangioma with torsion is extremely rare but it is one of the possible causes of acute abdominal pain that must be considered in patient with abdominal pain.
ETHICAL APPROVAL
Duo to hospital ethical board approval investigation this case does not meet the criteria for human subject research.
CONSENT
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
REFERENCES
1. Venkatram K, Bajaj SK, Abhilash S, Gupta N. (2019). Atypical exophytic liver mass: Giant pedunculated hepatic haemangioma masquerading as a gastrointestinal stromal tumour of the gastric wall. S. Afr. J. radiol. 23(1): 1-7.
2. Chang MC, Lin SP, Lin CH, Hsu DW, Wei CK, et al. (2007). Early Treatment for Symptomatic Giant Hepatic Hemangioma: Report of Three Cases and Literature Review. Surgery Journal, 2(4): 45-49.
3. Montero LG, Canchari PG, Peña AL, Guerra EG. (2017) Review Article: A Giant Hepatic Hemangiomas. Gastroenterol Hepatol Open Access 7(5): 00251.
4. Ha C, Kubomoto S, Whetstone BM., Parascandola S. (2013). “Pedunculated Hepatic Hemangiomas often Misdiagnosed Despite Their Typical Findings.” The Open Surgery Journal. 7: 1-5.
5. Castañeda PL, Loli YT, Medina CS. (2020). Torsion of a giant pedunculated liver hemangioma: Case report. Int J Surg Case Rep.; 75:207-210.
6. Klotz T, Montoriol PF, Da Ines D, Petitcolin V, Joubert-Zakeyh J, et al. (2013). Hepatic haemangioma: common and uncommon imaging features. Diagn Interv Imaging. 94(9):849-859.
7. Vilgrain V, Boulos L, Vullierme MP, Denys A, Terris B, et al. (2000) Imaging of atypical hemangiomas of the liver with pathologic correlation. Radiographics. 20(2):379-97.
8. Ersoz F, Ozcan O, Toros AB, CulcuS, Hasan B, et al. (2010). Torsion of a giant pedunculated liver hemangioma mimicking acute appendicitis: a case report. World Journal of Emergency Surgery. 5:2-2.
9. Tang T, Wang X, Mao Y, Li J, Wen T, et al. (2021). Real-world data on the clinicopathological traits and outcomes of hospitalized liver hemangioma patients: a multicenter study. Ann Transl Med. 9(13):1067.