Information Links
Related Conferences
Previous Issues Volume 8, Issue 1 - 2023
Favorable Long Term Outcome of Locally Advanced Adenocarcinoma Epididymis - An Extended Follow-Up: Case Report
Renata Soumarová1,*, Viktor Maňásek2, Ivan Ferák3
1Department of Radiotherapy and Oncology, Faculty Hospital Královské Vinohrady, Prague, Third Faculty of Medicine, Charles University, Prague, Czech Republic
2Radiotherapy and oncology department, Cancer center Nový Jičín, Czech Republic
3Pathology department, Cancer center Nový Jičín, Czech Republic
*Corresponding author: Renata Soumarová, Department of Oncology, Faculty Hospital Královské Vinohrady, Prague Šrobárova 1150/50, Praha 10, Third Faculty of Medicine, Charles University, Prague, Czech Republic; Email: [email protected]
Received Date: November 28, 2022
Publication Date: January 02, 2023
Citation: Soumarová R, et al. (2023). Favorable Long Term Outcome of Locally Advanced Adenocarcinoma Epididymis - An Extended Follow-Up: Case Report. Mathews J Case Rep. 8(1):80.
Citation: Soumarová R, et al. (2023). Favorable Long Term Outcome of Locally Advanced Adenocarcinoma Epididymis - An Extended Follow-Up: Case Report. Mathews J Case Rep. 8(1):80.
ABSTRACT
Background: Primary epididymal adenocarcinoma (PEA) is very rare disease with only about twenty described cases in the literature. Therefore, there is no standard treatment up to date. Case presentation: We present the case of young man (34 years of age) with a locally advanced PEA treated by definitive radiotherapy to the scrotal and groin region. This patient had a complete recovery and the positive outcome continues today, ten years after radiotherapy, with relatively minor late effects including telangiectasia and fibrosis. Conclusion: The patient enjoys a very good quality of life including penile erection. The presented case describes an unusual, very positive, therapeutic response of a locally advanced carcinoma of the epididymis.
Keywords: Epididymis, Adenocarcinoma, Radiotherapy
BACKGROUND
Primary tumors of the epididymis (PEA) are extremely rare and in most cases they are benign. Malignant tumors of the epididymis only occur in about 25% of all cases and the most common are rhabdomyosarcomas [1]. Metastases from other tumors can also occur in epididymis, such as adenocarcinomas from the gastrointestinal tract, prostate or lungs [2-5].
Primary adenocarcinoma of the epididymis is a tumor disease growing from epididymal epithelial cells. The literature contains dozens of case reports that document the rather poor prognosis of this disease [6,7]. Tumor growth is locally invasive and can spread to peri-epididymal soft tissue, the spermatic cord and testes. It manifests as a painful mass. Lungs, bone and abdominal organs are common metastatic sites [8]. In 2008 Ganem JP, et al. [8] found only 22 cases in the literature, in 2017 Zi-jun Zou published an update that only identified 17 cases of PEA [9].
CASE PRESENTATION
A 34-year-old male came to the urology department with a two-month history of painful and “squeezed” left hemi-scrotum. An inguinal radical orchidectomy and orchiectomy was conducted with the finding of an enlarged epididymis with a total size 7×1.5×1 cm and with a gray-white, solid, cylindrical tumor measuring 3.0×1.5×1.5 cm which appeared as a homogeneous structure surrounded by a sharp boundary.
The histological finding described the adenocarcinoma of the epididymis as tubular, papillary, with low differentiation, with high and atypical mitotic activity (MAI 10 and more mitoses/10 HPF). Well-differentiated tumor structures were found, too. Apparent and relatively frequent endo-lymphatic, endo-venous and (peri) endo-neural tumor permeation was detected. No tumor infiltration of the funiculus spermaticus (spermatic cord) was found. There was polynodular style of tumour growth with predominantly massive desmoplasia, the creation of pseudo capsules and incomplete septal separation of tumour structures. Malignant tumour penetration and perforation of pseudo capsules were seen. A detailed description of the histopathology was presented in the original article [13].
A post-operative CT/PET in February 2007 was negative, nevertheless, elective retroperitoneal lymphadenectomy was indicated. Although the role of this procedure in the treatment of adenocarcinoma of the epididymis is not clear, according to published case reports, occurrence of retrioperitoneal metastases is common [14].
The adenocarcinoma metastases were confirmed in three retroperitoneal lymph nodes in our patient. Due to the extremely low number of patients with this diagnosis, there are no clear recommendations for adjuvant therapy. Paclitaxel and platinum-based adjuvant chemotherapy was refused by the patient.
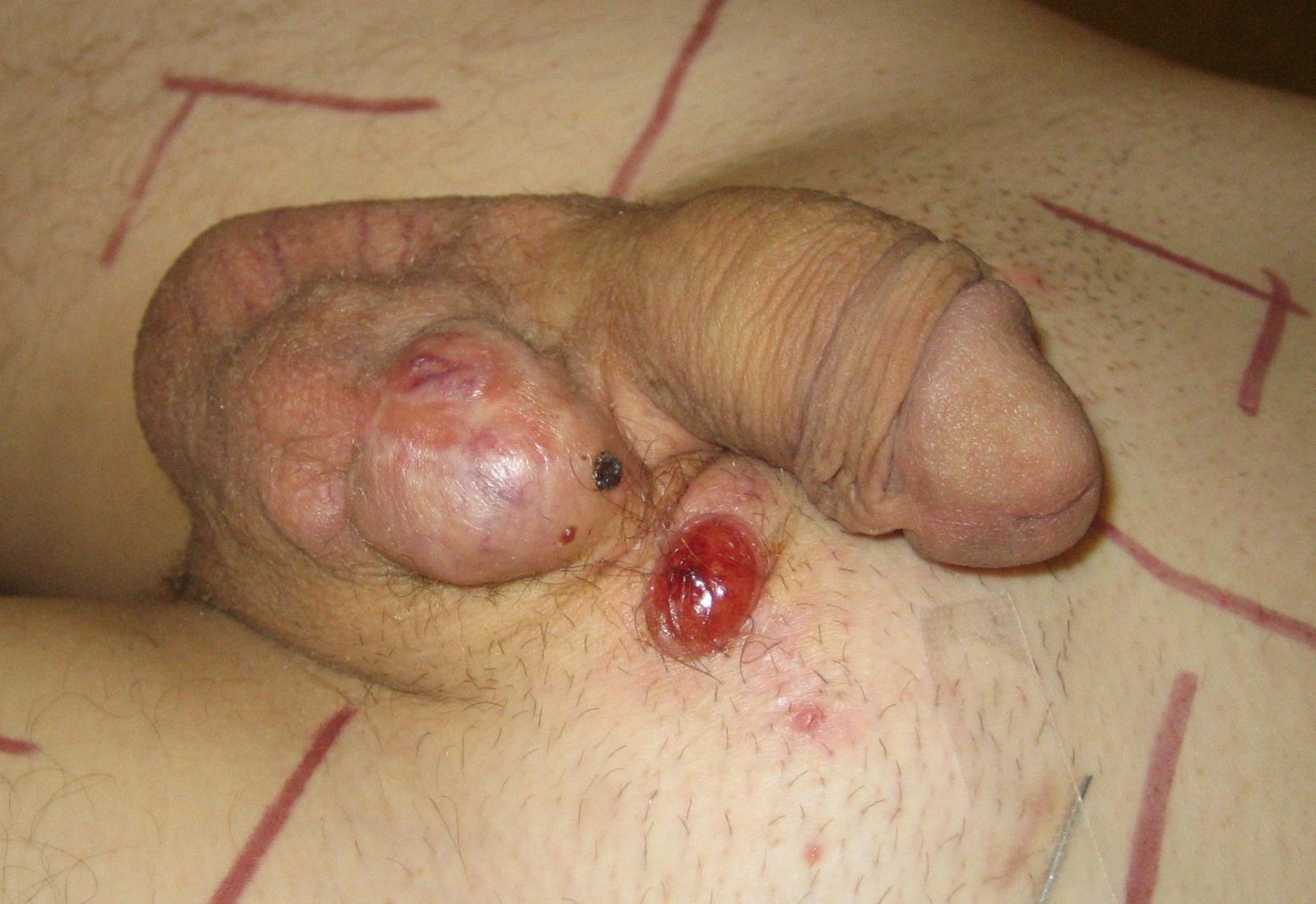
The patient did not come for the follow-up appointments either, however, after 6 months he was referred by a practitioner back to our clinic for a local recurrence of the tumor which measured 8×4×5 cm and penetrated into the skin of scrotum (Figure 1).
Figure 1: Locally advanced tumor of the epididymis prior to radiotherapy.
Local finding with infiltration of the skin was not considered operable, CT showed no distant dissemination, therefore radiotherapy was indicated for the area of tumor recurrence with a palliative intent. The patient was referred for cryopreservation of sperm before treatment. Spermiogram was normal. However, due to the patient’s young age a relatively high “radical” dose of radiation was chosen (2,5 Gy per fraction, 25 fractions, the biologically equivalent dose was 73.5 Gy). The technique of conformal (3D) radiotherapy was used. The patient tolerated the significant acute reaction, particularly the desquamative dermatitis, very well. After the radiotherapy a complete remission of the disease (Figure 2) was achieved based on a clinical examination as well as imaging methods. The remission has persisted for 10 years. Late changes after irradiation included telangiectasia on the skin and fibrosis under the skin. This was most apparent 3 years after the treatment.
Figure 2: Three months after radiotherapy a complete remission was achieved.
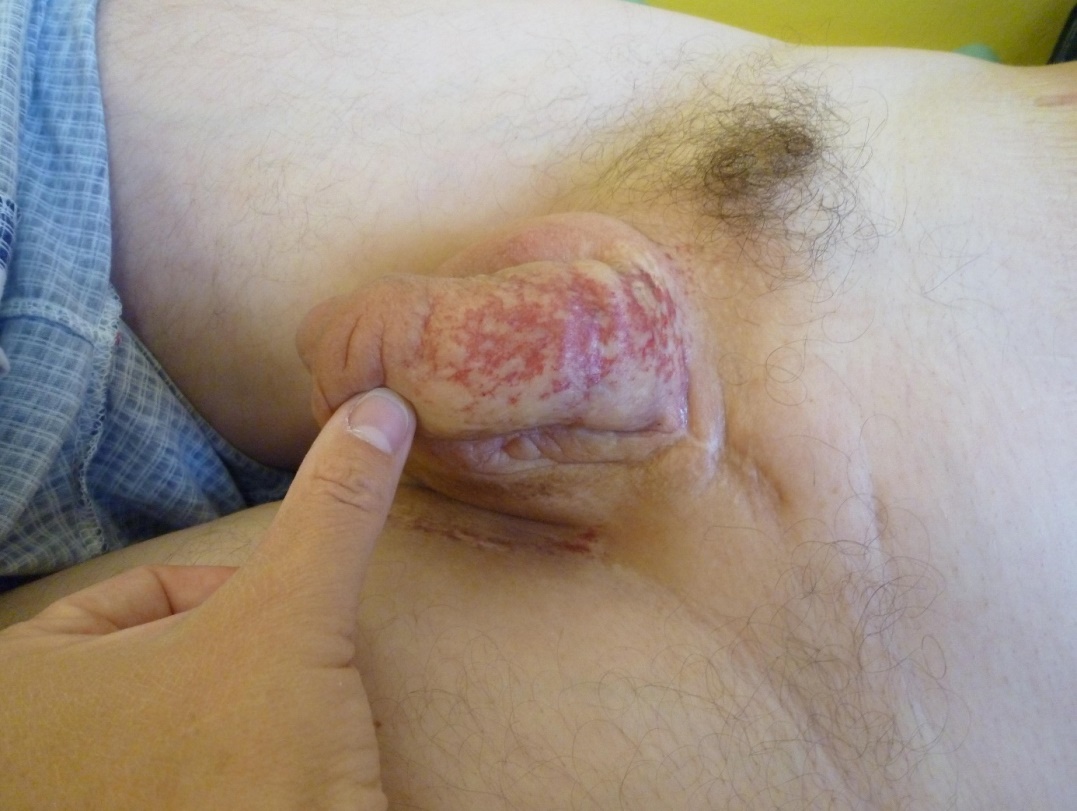
Atrophy of the subcutaneous tissue is apparent now, which was documented both clinically and photographically (Figure 3). The patient does not have lymphoedema of the scrotum or penis, has no functional problems and urinates without compliant. Erectile function was preserved but without ejaculation. Examinations of the lung, abdomen and pelvis do not show any metastases. Laboratory tests including testosterone levels have been performed on each visit every three to six months. All laboratory tests, including blood counts and biochemical parameters, were in the norm. Metastases were not detected on the imaging methods either. The first biochemical signs of primary hypogonadism (low testosterone level) were detected 5 year after radiotherapy. The endocrinologist recommended substitution of testosterone and it is ongoing till now.
Figure 3: Ten years after treatment, the regression of post-radiation late effects can be seen.
DISCUSSION
This relatively rare type of tumor in the epididymis has no clear or standard treatment which would normally include surgical removal of the tumor. According to other published cases, the importance of retroperitoneal lymphadenectomy in patients is in the control of locoregional disease. It may be curative even in case of proven lymphadenopathy and should be performed in all patients without distant metastases [14]. Each clinician must also consider the value of a retroperitoneal lymphadenectomy and, eventually, the appropriate adjuvant systemic therapy, i.e., most often chemotherapy or less often radiotherapy [10]. The use of radiotherapy has been rarely reported and its effect is considered palliative with a very short duration [11].
There was a case report published in 2015 involving a radiotherapy-treated adenocarcinoma patient, however, the follow-up lasted only 9 months [12]. In 2012 we published the treatment results of this case, at that time 5 years after the radiotherapy [13]. Since the oncologic, as well as the favorable functional outcome, has persisted for more than ten years now, we decided to republish this case with a longer follow-up period.
We present excellent results of radical radiotherapy for a recurrence of locally advanced adenocarcinoma of the epididymis with metastases into the retroperitoneum, in a 34-year-old male. Complete remission was achieved and continues. The patient has an excellent quality of life and retains functional sexual and urinary outcomes. He had no problems, no complaints. In this case, the late side effect of radiotherapy was only primary hypogonadism caused by the dose of radiation on the testicular area. Other symptoms which are usually associated with hypogonadism (hair loss, erectile dysfunction, etc.) did not appear. The patient then had testosterone replacement.
Although the late post-irradiation changes are considered irreversible, the patient did experience partial spontaneous regression of scrotal and penile fibrosis.
CONCLUSION
The treatment for this type of tumor includes usually surgical treatment in the event of metastases in lymph nodes or distant metastases using chemotherapy. Our report demonstrates possible inclusion of radical radiotherapy into the treatment algorithm.
FUNDING
This research was not supported.
AVAILABILITY OF DATA AND MATERIALS
Data sharing is not applicable to this article, since no datasets were generated or analyzed.
AUTHORS’ CONTRIBUTIONS
RS analyzed and interpreted the patient data, drafted the manuscript, and created the figures. Together with VM they performed the physical examinations and provided all medical care. IF described the histology of the tumor. All authors read and approved the final manuscript.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
No ethics committee approval is required at our institution for a case report involving a single patient.
CONSENT FOR PUBLICATION
Written informed consent was obtained from the patient for publication of this case report and all accompanying images. A copy of the written consent will be available for review by the Editor-in-Chief of this journal.
COMPETING INTERESTS
The authors declare that they have no competing interests.
REFERENCES
- Jones MA, Young RH, Scully RE. (1997). Adenocarcinoma of the epididymis: a report of four cases and review of the literature. Am J Surg Pathol. 21:1474.
- Moreno AF, Sastre Valera J, Loboff de León B, López-Tarruella S, Ortega Medina L, Díaz-Rubio E. (2005). Epididymal metastases as the first sign of a colon cancer recurrence. Clin Transl Oncol. 7:321-323.
- Tanaka H, Yasui T, Watase H. (1999). Metastatic tumor of the epididymis from pancreatic carcinoma: a case report. Hinyokika Kiyo. 45:649-652.
- Johansson JE, Lannes P. (1983). Metastases to the spermatic cord, epididymis and testicles from carcinoma of the prostate-five cases. Scand J Urol Nephrol. 17:249-251.
- Coussa-Koniski ML, Maalouf PA, Raad NE, Bejjani NA. (2015). Scrotal wall metastasis from a primary lung adenocarcinoma. Respir Med Case Rep. 15:77-79.
- Chauhan RD, Gingrich JR, Eltorky M, Steiner MS. (2001). The natural progression of adenocarcinoma of the epididymis. J Urol.166:608-610.
- Arisan S, Akbulut ON, Cakir OO, Ergenekon E. (2004). Primary adenocarcinoma of the epididymis: case report. Int Urol Nephrol. 36:77-80.
- Ganem JP, Jhaveri FM, Marroum MC. (1998). Primary adenocarcinoma of the epididymis: Case report and review of the literature. Urology. 52:904-908.
- Zou Z, Xiao Y, Liu Z, Zhang R, Liang J, Tang Y, Lu Y. (2017). Clinicopathological Characteristics, Treatment, and Prognosis of Rarely Primary Epididymal Adenocarcinoma: A Review and Update. Biomed Res Int. 2017:4126740.
- Briasoulis E, Kalofonos H, Bafaloukos D, Samantas E, Fountzilas G, Xiros N, et al. (2000). Carboplatin plus paclitaxel in unknown primary carcinoma: a phase II Hellenic Cooperative Oncology Group Study. J Clin Oncol.18:3101.
- Chauhan RD, Gingrich JR, Eltorky M, Steiner MS. (2001). The natural progression of adenocarcinoma of the epididymis. J Urol.166:608-610.
- Sahoo TK, Dhal I, Das Majumdar SK, Parida DK. (2015). Primary Adenocarcinoma of epididymis: A case report and review of literature. SEAJCRR. 4:1538-1543.
- Soumarova R, Manasek V, Perkova H, Ferak I. (2012). Radiotherapy in the treatment of epididymal adenocarcinoma - case report. Onkologie. 35:43-45.
- Stanik M, Dolezel J, Macik D, Krpensky A, Lakomy R. (2012). Primary adenocarcinoma of the epididymis: the therapeutic role of retroperitoneal lymphadenectomy. Int Urol Nephrol. 44:1049-1053.