Previous Issues Volume 2, Issue 1 - 2018
The Prevalence of Vitamin D Deficiency in Patients with Hashimoto's Hypothyroidism
Mahdis Solhjoo1*, Alireza Rastgoo Haghi2, Nasim Golchin3, Zahra Ahmadvand4, Hossein Moin Tavakoli4
1Department of Medicine, Nassau University Medical Center, USA, NY.
2Department of Pathology, Hamadan University of Medical Sciences, Hamadan, Iran.
3Department of Medicine, Icahn School of Medicine at Mount Sinai Queens Hospital Center, NY, USA.
4Department of Medicine, Hamadan University of Medical Sciences, Hamadan, Iran.
Corresponding Author: Mahdis Solhjoo, Department of Medicine, Nassau University Medical Center, USA, NY.
Tel: 15165720123; E-Mail: [email protected]
Received Date: 27 Jul 2018 Accepted Date: 07 Aug 2018 Published Date: 13 Aug 2018
Copyright © 2018 Solhjoo M
Citation: Solhjoo M, A Rastgoo Haghi, Ahmadvand Z, Golchin N, et al. (2018). The Prevalence of Vitamin D Deficiency in Patients with Hashimoto's Hypothyroidism. M J Immu. 2(1): 006.
ABSTRACT
Introduction:Vitamin D has some anti-inflammatory and immune-modulating attributes and in recent studies its low levels has been associated with some autoimmune diseases. Hashimoto's hypothyroidism is one of the most common endocrine disease worldwide and in this study the aim is to investigate the relation between the level of vitamin D and Hashimoto's hypothyroidism.
Material and Methodes:40 patients with hypothyroidism and 40 healthy subjects with normal TSH level were selected from Besat Hospital, Hamadan, Iran during the period of April to August 2016. Their serum levels of 25 (OH) D, Anti-TPO and TSH were checked and recorded in the checklist.
Results:There was a significant difference between the two groups in terms of vitamin D mean. Also the vitamin D mean in patients with subclinical and clinical Hashimoto's disease was 18.3 ng/ml and 5.52 ng/ml respectively and the difference was statistically significant. Based on logistic regression test there was no significant difference between serum levels of vitamin D and TSH in both groups.
Conclusion: Based on the results it can be concluded that there is an association between low level of vitamin D and Hashimoto's thyroiditis.
KEYWORDS
Vitamin D; Hypothyroidism; Hashimoto's; Autoimmune Disease.
INTRODUCTION
Vitamin D deficiency is a global problem and more than one billion people worldwide are vitamin D deficient [1]. Vitamin D has an important role in the homeostasis of calcium and phosphate and prevention of osteoporosis [2]. Also vitamin D can prevent excessive cell proliferation and cell differentiation, thus may prevent the development of diseases like cancers [3]. According to the recent studies, vitamin D deficiency is associated with the autoimmune diseases such as rheumatoid arthritis (RA), Systemic Lupus Erythematosus (SLE), Inflammatory Bowel Disease (IBD), Multiple Sclerosis (MS) and Type 1 Diabetes (DM1). Vitamin D can prevent the incidence or progression of these diseases [4]. Furthermore, in a number of articles low levels of vitamin D have been reported on Hashimoto's patients [5,6]. Vitamin D is a fat soluble vitamin which exposure to ultraviolet B light is its main source in the body [5]. Then it will hydroxylate in the liver and turn into the form of 25-hydroxycholecalciferol (25(OH)D) which is its inactive form. Its active metabolite, 1,25-dihydroxycholecalciferol (1,25(OH)2D) which is known as calcitriol is being produced in the kidneys [7]. The normal range of 25(OH)D is 30 to 32 ng/ ml and levels less than 12 ng/mL is concidered as severe vitamin D deficiency [8]. The calcitriol applys its work in the body by binding to vitamin D receptor (VDR). VDR is seen almost in all nucleated cells. Any genetic change in the VDR, predisposes the person to autoimmune thyroid disorders including Hashimoto's thyroiditis and Grave's disease [6]. More than 200 genes are regulated by vitamin D, either directly or indirectly. These genes are responsible for cell devision and differentiation control as well as cell death so vitamin D reduces the division of malignant cells. Vitamin D also inhibits the production of inflammatory factors that are important in the development of Hashimoto's thyroiditis. This hormone not only inhibits the activity of T-cells, but also inhibits the production of interferon gamma, Interleukins and T helper cells. In addition, vitamin D prevents B cells proliferation and induces their apoptosis [9].
Hypothyroidism is one of the most common endocrine disease in the western developed countries and also in the developing countries. Generally, the most common cause of hypothyroidism in the world is iodine deficiency and the most common cause of hypothyroidism in adults taking iodine in normal value is Hashimoto's which is a chronic hypothyroidism caused by the antibodies that are involved in the immune response [8].
In the present study our goal was to examine the relationship between Hashimoto's hypothyroidism and vitamin D deficiency and to find the relation between them.
MATERIALS AND METHODS
This Comparative Cross-Sectional study was conducted in the Besat Hospital, Hamadan, Iran during the period of April to August 2016. 40 patients with hypothyroidism and 40 healthy subjects with normal thyroid-stimulating hormone (TSH) level between 0.4 to 5 microU/ml were selected and their serum level of 25(OH)D, Anti-thyroid peroxidase (Anti-TPO) and TSH was obtained. Exclusion criteria were patients with diabetes, chronic renal failure, IBD and other intestinal diseases, liver diseases, lupus, MS and patients who had taken vitamin D supplements. Patients with subclinical (SCH) hypothyroidism with the criteria of Anti-TPO positive and TSH level between 6-10 microU/ml despite normal level of free thyroxin (0.8-2.8 ng/dl) and clinical Hashimoto's hypothyroidism with criteria of Anti-TPO positive and TSH>10 micro U/ml with decrease level of free thyroxin (< 0.8 ng/dl) were involved into the study. Also vitamin D levels less than 12 ng/ml was considered as Vitamin D deficiency [8]. Informed consent was taken from all the study subjects. For data analysis, independent t-test method was used and all comparisons were based on the presence of a significant correlation with p value of less than 0.05.
RESULTS
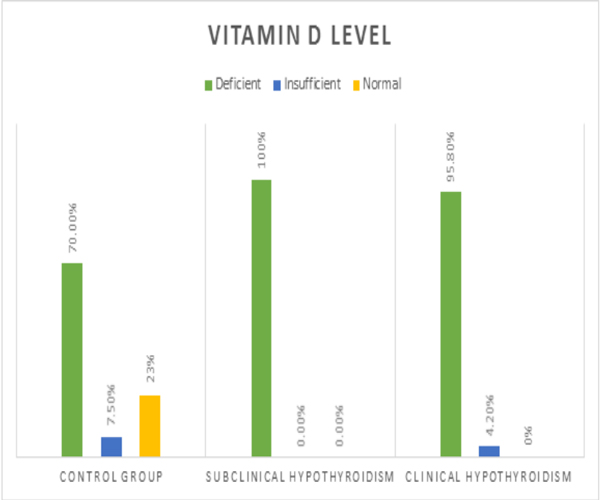
In this study 80 subjects were evaluated which included 30 men and 50 women. T- test result showed that the average age and gender in both groups were close and no statistically significant difference was observed. Table (1) shows the mean S.D values of age and gender distribution in our study. Also it includes the Serum 25(OH)D and TSH levels in both groups. 67 cases (83.7%) were diagnosed with hypovitaminose D which 39 (58.2%) of them were in patients group and 28 (41.8%) of them were among the control group. Figure (1) demonestrates the persentage of vitamin D insufficiency (serum 25(OH)D <20 ng/ml) and deficiency (serum 25(OH)D <12 ng/ml) in the in control group versus patients with subclinical versus clinical Hashimoto's. The average vitamin D in Hashimoto's patients was 14.8 ± 7.17 ng/ml and in the healthy subjects was 26.08 ± 17.3 ng/ml. According to these results there was a significant difference between the two groups in terms of the vitamin D avarage level. After adjusting the groups for gender and age this result persisted. The mean level of vitamin D was lower in female patients in comparison with male patients but this was not significant.
Table 1: Demographical and clinical characteristics of the studied subjects.
| Parameters : Mean ±SD | Case Group | Control Group | P Value |
|---|---|---|---|
| Gender | 13 M 27 F | 17 M 23 F | P > 0.05 |
| Age (years) | 39.4 ± 11.2 | 36.87 ± 11.75 | P > 0.05 |
| Serum 25(OH) D(ng/ml) | 14.8 ± 7.17 | 26.08 ± 17.3 | P < 0.001 |
| Serum TSH (mU/L) | 9.9 ± 5.36 | 2.5 ± 1.05 | P < 0.001 |
Figure 1: The persentage of vitamin D insufficiency and deficiency in the in control group versus patients with subclinical versus clinical Hashimoto's.
DISCUSSION
Vitamin D is a fat-soluble vitamin that has an important role in the homeostasis of calcium and phosphate and bone metabolism. Vitamin D controls calcium absorption in the intestine and it mediates skeletal mineralization in cooperation with parathyroid hormone. Also it has some anti-inflammatory and immune-modulating attributes probably caused by its affects on cytokine levels. Recent studies have shown relationship between low vitamin D levels and many diseases like cardiovascular diseases, cancer, and autoimmune diseases such as multiple sclerosis [10]. In Kragt study an inverse relationship was found between vitamin D levels and MS risk especially for vitamin D levels measured in young patients [11]. Also it seems that exposure to sun light in early childhood reduces the risk of developing multiple sclerosis [12]. There are few studies available about the association between the levels of vitamin D and Hashimoto's hypothyroidism and their results are conflicting. Hence in this study we aimed to evaluate the levels of vitamin D among patients with Hashimoto's hypothyroidism compared to healthy subjects. According to Lagunova study the level of vitamin D is related to the gender, age and body mass index (BMI) [13]. In our study the mean level of vitamin D was lower in females in comparison with males in both groups but it was not significant which we can refer it to the small sample size. Our results are similar to Hashemipour [14] and Mackawy [6] studies which show non-significant difference in level of vitamin D between males and females. In contrast, some studies are showing that regarding of the vitamin D level, there is a significant difference between males and females, in some studies it is more in females [15] and in others it is more in males [16]. In a study by Verdoia et al [17], it is found that gender significantly affects the vitamin D level and its lower levels observed in females, plays an important role in the severity of coronary artery disease. Age, race, exposure to sunlight, dietary vitamin D intake, chronic diseases and seasonal variations can be the explanation of the dissension between these studies.
In our study there was no correlation between Vitamin D and TSH levels but in Mackawy [6] study the results showed negative correlation between these two parameters. In addition according to our results, vitamin D level was significantly lower in hypothyroid patients compared to the control group and vitamin D deficiency prevalence was significantly higher in patients in comparison with the controls group.
There are several studies in concordance to our results [5,18]. In a study by Mansournia et al. [19] in 2014, the results demonstrated that in addition to lower levels of vitamin D in patients with Hashimoto's disease compared to healthy individuals, high levels of vitamin D is associated with reduced risk of Hashimoto's hypothyroidism. According to his study, each 5 ng/ml increase in vitamin D levels, reduced the risk of Hashimoto's upto 19%. The mean vitamin D level in this study was15.9 ng/ml in the patients and 24.38 ng/ml in the healthy individuals which is close to the results of our study. In 2009 Goswami et al. [20] cunducted a study on individuals aged 16 to 60 years to determine the relation between the level of vitamin D and thyroid autoimmun diseases. The average vitamin D in patients was 17.5 ng/ml and 87% of them were vitamin D deficient. Also a weak inverse association between the levels of 25 (OH) D and Anti-TPO was entitled. Some articles demonstrate that vitamin D deficiency may exacerbate the onset and development of Grave's disease and its correction can reverse the disease [21]. Vitamin D receptor has been identified in the thyroid follicular cells which can be suggestive of the role of 1,25(OH)2D in the thyroid. It has been shown that vitamin D has an important role in T helpers type 1 and 2 as a regulater. Vitamin D reduces the production of interleukin-2 (IL2), gamma interferon (INF?), and tumor necrosis factor (TNF) and also inhibits the expression of IL-6 and the production of autoantibodies by B lymphocytes [22]. Therefore, vitamin D deficiency may act as an trigger of autoimmune diseases like Hashimoto's and Grave's disease [23].
In summary, based on the results of this study and comparison with the other studies, it can be concluded that there is an association between low level of vitamin D and Hashimoto's thyroiditis. According to this result, it is recommended to do the screening test for Vitamin D deficiency in all hypothyroid patients. It seems that prescibing vitamin D to these patients can prevent the progresion of the disease or even can cause reversion. Latter statement needs more study with larger sample size to determine the effective dose of vitamin D which is needed to reduce disease progression in Hashimoto's thyroiditis.
ACKNOWLEDGMENT
We thank our colleagues who provided insight and expertise that greatly assisted the research,
REFERENCES
- Hollick MF and Chen TC. (2008). Vitamin D deficiency a worldwide problem with health consequences. Am J Clin Nutr PubMed. 87(4): 10805-10865.
- Cranney A, Horsley T, O'Donnell S. (2008). Effectiveness and Safety of Vitamin D in Relation to Bone Health. Evidence Reports/Technology Assessments. 158: 543-550.
- Samuel S and Sitrin MD. (2008). Vitamin D's role in cell proliferation and differentiation. Nutr Rev. 66(10 Suppl 2): 116-124
- Baeke F, Takiishi T, Korf H, Gysemans C, et al. (2010). Vitamin D: modulator of the immune system. Curr. Opin Pharmacol. 10: 482-496.
- Tamer G, Arik S, Tamer I and Coksert D. (2011). Relative vitamin D insufficiency in Hashimoto's thyroiditis. Thyroid. 21(8): 891-896.
- Mackawy AM, Al-Ayed BM and Al-Rashidi BM. (2013). Vitamin d deficiency and its association with thyroid disease. International Journal of Health Sciences. 7(3): 267- 275.
- Lips P. (2006). Vitamin D physiology. ProgBiophysMol Biol. 92(1): 4-8.
- Qamar J, Khan and Carol J Fabian. (2010). How I Treat Vitamin D Deficiency. J Oncol Pract. 6(2): 97-101.
- Martin Hewison. (2010). Vitamin D and the immune system: new perspectives on an old theme. Endocrinol Metab Clin North Am. 39(2): 365-379.
- Teresa Kulie, Amy Groff, Jackie Redmer, Sarina Schrager, et al. (2009). Vitamin D: An Evidence-Based Review. J Am Board Fam Med. 22(6): 698-706.
- Kragt J, van Amerongen B, Killestein J, Lips P, et al. (2009). Higher levels of 25-hydroxyvitamin D are associated with a lower incidence of multiple sclerosis only in women. Mult Scler. 15(1): 9-15.
- Kampman MT, Wilsgaard T and Mellgren SI. (2007). Outdoor activities and diet in childhood and adolescence relate to MS risk above the Arctic Circle. J Neurol. 254(4): 471-477.
- Lagunova Z1, Porojnicu AC, Lindberg F, Moan J, et al. (2009). The dependency of vitamin D status on body mass index, gender, age and season. Anticancer Res. 29(9): 3713-3720.
- Hashemipour S, Larijani B, Adibi H, Ebrahim J, et al. (2004). Vitamin D deficiency and causative factors in the population of Tehran. BMC Public Health. 4: 38.
- Sedrani SH, Elidrissy AW and El Arabi KM. (1983). Sunlight and vitamin D status in normal Saudi subjects. Am J Clin Nutr. 38(1): 129-132
- Yamashita H, Noguchi S, Yamashita H, Takatsu K, et al. (2001). High prevalence of vitamin D deficiency in Japanese female patients with Grave's disease. Endocr J. 48(1): 63-69.
- M. Verdoia, A. Schaffer, L. Barbieri, G. Di Giovine, et al. (2015). Impact of gender difference on vitamin D status and its relationship with the extent of coronary artery disease. Nutr Metab Cardiovasc Dis. 25(5): 464-470.
- Bozkurt NC1, Karbek B, Ucan B, Sahin M, et al. (2013). The association between severity of vitamin D deficiency and Hashimoto's thyroiditis. Endocr Pract. 19(3): 479-484.
- Mansournia N, Mansournia MA, Saeedi S and Dehghan J. (2014). The association between serum 25OHD levels and hypothyroid Hashimoto's thyroiditis. J Endocrinol Invest. 37(5): 473-476.
- Goswami R1, Marwaha RK, Gupta N, Tandon N, et al. (2009). Prevalence of vitamin D deficiency and its relationship with thyroid autoimmunity in Asian Indians: a community-based survey. 102(3): 382-386
- Omar N Alhuzaim and Naji Aljohani. (2014). Effect of Vitamin D3 on Untreated Grave's Disease with Vitamin D Deficiency. Clin Med Insights Case Rep. 7: 83-85.
- Hong Zhang, Lingyun Liang and Zhongjian Xie. (2015). Low Vitamin D Status Is Associated With Increased Thyrotropin-Receptor Antibody Titer in Graves Disease. Endocr Pract. 21(3): 258-263.
- Claudia Diniz Lopes MarquesI, Andrea Tavares DantasII, Thiago Sotero FragosoIII and angela Luzia Branco Pinto DuarteIV. (2010). The importance of vitamin D levels in autoimmune diseases. Rev Bras Reumatol. 50(1): 67-80.