Information Links
Related Conferences
Previous Issues Volume 7, Issue 3 - 2023
Feline Sporotrichosis: Case Report
Marcela Sargo Gatti1, Juliana Weckx Peña Muñoz1, Alexandre Fakih Cascardi5, Esther Lopes Ricci2, Maria Aparecida Nicoletti1,3, André Rinaldi Fukushima1,4,*
1CETAC—Veterinary Training Center, São Paulo 01532-000, Brazil
2Mackenzie Presbyterian University, Center for Biological and Health Sciences, Graduate Program in Developmental Disorders, São Paulo, SP, Brazil
3Faculty of Pharmaceutical Sciences, University of Sao Paulo, Sao Paulo 05508-000, Brazil University Center of the Americas, Sao Paulo, Brazil
4University of São Paulo, Faculty of Veterinary Medicine and Animal Science, Department of Pathology, Graduate Program in Experimental and Comparative Pathology, São Paulo, Brazil
5University of Marilia, Brazil
*Corresponding author: André Rinaldi Fukushima, CETAC—Veterinary Training Center, São Paulo 01532-000, Brazil, and University of São Paulo, Faculty of Veterinary Medicine and Animal Science, Department of Pathology, Graduate Program in Experimental and Comparative Pathology, São Paulo, Brazil, Tel: (11) 98133-7311, ORCID: 0000-0001-6026-3054; E-mail: [email protected].
Received Date: July 14, 2023
Published Date: July 27, 2023
Citation: Gatti MS, et al. (2023). Feline Sporotrichosis: Case Report. Mathews J Vet Sci. 7(3):23.
Copyrights: Gatti MS, et al. © (2023).
ABSTRACT
The main factor of feline sporotricosis is the action of the fungus Sporothrix schenckii, being a chronic or subacute disease transmissible among domestic animals, also affecting humans. With increasing rates of transmission from felines to humans, zoonosis is worrying, both for health policies and for animal protection policies, since many animals are abandoned when contracting sporotrichosis, generating greater risks of spreading the disease among humans and other animals. Therefore, the objective of the article is to demonstrate that the disease can be successfully treated through the report of clinical experience. The method used for diagnosis was by imprinting the lesion, where the presence of the fungus Sporothrix schenckii was found in the yeast form with degenerated neutrophils and macrophages. The treatment performed was with Itraconazole at a dose of 100mg/day in the manipulated, similar and original versions, showing through the report the greater effectiveness of the original version of the drug.
Keywords: Zoonosis, Domestic animals, Treatment of Sporotrichosis.
INTRODUCTION
Domestic felines are associated as the main transmission agents of the zoonotic disease Sporotrichosis, a chronic infection that affects the skin and subcutaneous tissues of animals and can be transmitted to humans [1-3]. The pathogenic fungus Sporothrix schenckii is present in plant debris in moist and tropical climates [4-6].
The disease is characterized by the presence of firm and nodular lesions, which become soft over time and can ulcerate, releasing purulent exudate and blood [7]. The lesions can vary from cutaneous to subclinical infections, disseminated or solitary lesions, extracutaneous signs, and involve mucous membranes [8,9]. Usually, ulcerated lesions that resist healing and rapidly spread are observed [10].
The infectious agent, the fungus Sporothrix schenckii, has a worldwide distribution, except for Antarctica, with the highest prevalence of Sporotrichosis reports in occupational dermatoses related to gardening or agricultural activities associated with fungal species S. schenckii and S. globosa [3,11].
The dissemination of the disease is uneven among regions, with South America being considered an endemic area. In the 1990s, the first reports of zoonotic outbreaks caused by Sporothrix schenckii were recorded in the states of São Paulo and Rio de Janeiro, spreading to other territories and regions [12]. The highest number of reports of infection in humans and animals comes from the Southeast region of the country, followed by the South, North, and Northeast regions [3,10].
Domestic felines are the main responsible for the transmission of the disease, with intact males that have free access to public areas being potential epidemiological agents. Transmission occurs through skin lesions in contact with an infected animal [4,13].
For accurate diagnosis, it is necessary to isolate the pathogenic fungus in culture medium for identification, a procedure that can take up to 20 days. Treatment involves the administration of antifungal drugs, such as Itraconazole at doses ranging from 100 to 200mg/day [14], the allylamine terbinafine, which also has fungicidal action, at dosages ranging from 250mg to 1g/day [15], as well as sodium and potassium iodides, ketoconazole, amphotericin B, the triazoles posaconazole and fluconazole, surgical removal of lesions, cryosurgery, and local thermotherapy [3]. The duration of treatment may vary depending on the severity and progression of the lesions.
An alternative for veterinary treatment that has become quite attractive is compounding in compounding pharmacies since these establishments fill a gap that the pharmaceutical industry does not meet.
Compounded medication offers significant benefits, such as the possibility of preparing formulations with active components not available in the pharmaceutical industry and personalizing formulations for patients with intolerance to commercially manufactured medications. Additionally, it allows for adapting the pharmaceutical form to facilitate use in specific populations, such as children and the elderly, by preparing liquid medications with flavorings and sweeteners, as well as offering alternative pharmaceutical forms. Compounding is especially necessary for unstable medications that need to be prepared and used rapidly, making large-scale production unfeasible. Other advantages include the possibility of combining medications for multiple therapies and the convenience of individualized doses, avoiding waste. Furthermore, compounding allows for rescuing discontinued medications by pharmaceutical companies due to economic reasons or lack of market interest [16,17].
On the other hand, compounded medication presents disadvantages that raise concerns, especially regarding the production process and safety of use. Some advanced technological processes, which ensure the homogeneity of mixtures in solid form, as well as various quality control tests performed by the pharmaceutical industry, are not viable in small-scale personalized production, such as in compounding pharmacies.
The compounding of medications in compounding pharmacies has been a matter of concern for Health Surveillance due to reported cases of severe adverse events. Ensuring the safety and quality of these medications is crucial, considering the significant growth of the compounding pharmacy market in Brazil, which has become an important economic source and employs many pharmacists.
Safety in the compounding of medications in compounding pharmacies has proven to be a challenge for Health Surveillance. These pharmacies, also known as compounding pharmacies, are gaining prominence in the Brazilian medication scene. This sector of the pharmaceutical profession has grown significantly in recent years and has become an important economic player in the Brazilian market, as well as one of the sectors employing the most pharmacists in the country. It is evident that there is a need to provide safe and quality products, especially considering the growth of the compounding pharmacy market, as pointed out by [18].
From 2000 to 2005, the National Institute of Quality Control in Health (INCQS), a reference laboratory in health surveillance linked to the Oswaldo Cruz Foundation, received 131 samples of compounded medications for analysis of their contents. During this period, severe cases related to the consumption of these medications were recorded, resulting in deaths, coma, hospitalizations, poisonings, burns, and adverse effects due to technical quality deviations in the production of these products. Notable cases include the poisoning of four children in 2003 resulting in death due to the use of compounded medications containing clonidine, as well as cases reported in São Paulo associated with compounded medications containing levothyroxine. In Bahia, three deaths occurred related to compounded medications containing clonidine and lidocaine, and twelve people experienced discomfort for the same reasons in Itagiba-Bahia [19,20].
On December 10, 2011, the Department of Health of Minas Gerais (SES/MG) investigated eight deaths registered in the region of Teófilo Otoni, possibly related to the ingestion of the compounded medication Secnidazole 500mg, produced by a compounding pharmacy. The investigation considered the possibility of cross-contamination with another compounded medication on the same date, an antihypertensive drug [20].
The analysis of cases occurring between 2000 and 2005, involving deaths, poisonings, and other adverse events related to the use of compounded medications, highlights the need for regulation and strict control in this sector. It is essential to establish measures that ensure the quality of the inputs used, proper compounding, appropriate labeling of products, and training of the professionals involved.
Given the risks and benefits associated with the compounding of medications, a balance between the flexibility provided by the personalization of formulations and a guarantee of product safety and efficacy is necessary. It is essential to promote greater integration between compounding pharmacies and health authorities to establish clear guidelines, good practice standards, and effective monitoring to ensure the quality and safety of compounded medications.
In this context, the present report aims to contribute to elucidating the efficacy of different formulations of Itraconazole, providing scientific evidence regarding the superiority of the reference version of the drug. The outcomes achieved through this study can support clinical decision-making and facilitate appropriate selection of the medication for the treatment of specific clinical conditions.
CASE REPORT
The present description refers to the clinical case of a domestic female cat, approximately 5 years old, which has free access to the street and lives with other animals. During the clinical consultation, ulcerated lesions of various diameters, exudative in nature, were observed, predominantly in the facial region, including the nose, eyes, and ears, as illustrated in Figure 1. Such ulcerated lesions are commonly observed clinical signs in a large number of cases referred for veterinary clinical evaluation [21,22].
Figure 1. Animal with ulcerated and exudative lesions
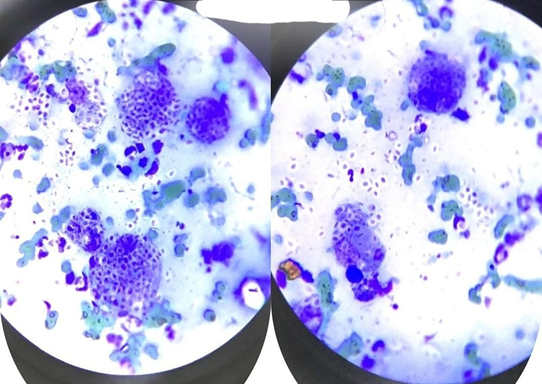
After observing the cutaneous lesions, a sample was collected for diagnosis using the imprint method of the lesion. In the cytopathological examination, the presence of the fungus Sporothrix schenckii in the yeast form was identified, along with degenerated neutrophils and macrophages, as illustrated in Figure 2.
The imprint collection technique, as described by [21], allowed the visualization of fungal structures in the cytopathological examination. The slides were stained using the Romanowsky technique with the basic dye methylene blue and the acidic dye eosin.
Figure 2. Slides stained by the Romanowsky method with yeast-like structures compatible with Sporothrix spp.
The results obtained in this case report are consistent with previous studies that reported the presence of mucosal lesions in the respiratory system caused by Sporothrix schenckii, such as the studies by [15,21], and [3]. Delay in the treatment of the disease can lead to pulmonary complications and even death of the animal, as evidenced in previous studies.
In a study conducted by [4], which evaluated 100 animals, with 66 testing positive for Sporothrix schenckii, it was observed that most infected animals were unneutered males (69.6%) and had access to the outdoors (89.3%). Furthermore, it was found that 65.2% of the animals presented focal lesions, while 34.8% presented disseminated lesions. Among the clinical cases analyzed by [4], 31.8% resulted in death or euthanasia, highlighting the severity of the disease when not properly treated.
In this case report, the animal was initially treated with compounded Itraconazole, without showing clinical improvement after 2 months of treatment. Subsequently, the similar version of the chemical compound was administered for an additional 2 months, with little clinical improvement. However, when the original version of the chemical compound was administered, a sudden clinical improvement was observed, with a reduction in lesions in less than a month. The treatment was continued for an additional 3 months, following widely recommended therapeutic protocols to prevent relapses [23], state that most cases that progress to chronicity or death occur due to therapeutic inefficiency, lack of appropriate therapies, or relapses. After 3 months of treatment, no lesions were found, even after discontinuation of the medication. A small wound in the nasal region was observed; however, a new cytological examination did not detect the presence of the fungus, suggesting that this new lesion may have been caused only by some minor trauma or scratch on the animal's face.
Itraconazole is widely used in the treatment of sporotrichosis due to its lower incidence of adverse reactions compared to other antifungals [4,24]. Studies such as those by [3] also highlight the good results in lesion healing and the acceptability of treatment with Itraconazole in felines and canines.
Results from Itraconazole treatments, such as the studies by [23] and [6], demonstrate the effectiveness of the medication in lesion regression. Administration of the drug for at least one month after lesion regression is recommended, according to studies by [3,4,25].
During the treatment period, no adverse reactions were observed in the animal. The patient exhibited a docile behavior, facilitating the daily administration of the medication. Although it is important to note that the efficacy of the medications used in this specific case cannot be generalized without conducting broader studies with a larger number of cases, it was clear the rapid progression of clinical healing with the use of the original version of the medication, as shown in Figure 3.
It is crucial to highlight that case reports, such as this one, contribute to the accumulation of scientific evidence regarding the efficacy and impact of Itraconazole treatment in sporotrichosis. However, further studies, such as controlled clinical trials, are needed to confirm these results and establish more precise therapeutic protocols for managing this disease in domestic felines.
In conclusion, this case report highlighted the importance of proper treatment for sporotrichosis in domestic felines. The use of Itraconazole, especially in the reference version, proved to be effective in the regression of cutaneous lesions caused by Sporothrix schenckii. The prolonged administration of the medication, following recommended therapeutic protocols, contributed to preventing relapses. However, further research is needed to provide a solid foundation and establish more definitive therapeutic guidelines for treating sporotrichosis in this animal species.
Figure 3. Photograph of ulcerated lesions found in the domestic feline.
CONCLUSION
Feline sporotrichosis, caused by the fungus Sporothrix schenckii, is an endemic zoonosis in Brazil, especially in the Southeast region. The main transmission agents are male, non-neutered cats with free access to the streets and other animals. The disease is transmissible to humans, which requires protective measures and care for the felines, such as neutering and restricting access to the streets, as well as proper hygiene of the animal's living areas.
The reported clinical case highlighted the effective effect of the medication Itraconazole in its reference version, in a female feline with sporotrichosis presenting exudative ulcerated lesions. However, further research must be conducted to understand the effects of the medication and its efficacy in different stages of sporotrichosis.
REFERENCES
- Driemeier RMS. (2021). Esporotricose humana, felina e zoonótica na Região Metropolitana de Porto Alegre. Dissertação. 46f. (Especialista em micotologia). Brazil, Porto Alegre: Federal University of Rio Grande do Sul.
- Monteiro HRB, Taneno JC, Neves MF. (2008). Esporotricose em felinos domésticos. Electronic Scientific Journal of Veterinary Medicine. 10.
- Santos AF, Rocha BD, de Valgas e Bastos C, de Oliveira CSF, de Magalhães Soares DF, Pais GCT, et al. (2018). Guia Prático para enfrentamento da Esporotricose Felina em Minas Gerais. V&Z Magazine in Minas. 137:16-27.
- Almeida AJ, Reis NF, Lourenço CS, Costa NQ, Bernardino MLA, Vieira-da-Motta O. Esporotricose em felinos domésticos (Felis catus domesticus) em Campos dos Goytacazes, RJ. Pesq Vet Bras. 38(7):1438-1443.
- Larsson CE. (2011). Esporotricose. Braz J Vet Res Anim Sci. 48(3):250-259.
- da Rocha RFDB. (2014). Tratamento da esporotricose felina refratária com a associação de iodeto de potássio e itraconazol oral. Dissertação. 73f. (Mestre em Ciências). Brazil, Rio de Janeiro: Oswaldo Cruz Foundation.
- da Silva GS, Ortiz EC, da Silva CCF, da Silva ATB, da Silva EL. (2020). A esporotricose em felinos. Revista Intellectus. 56(1):51-63.
- De Macêdo-Sales PA, da Silveira Souto SRL, Destefani CA, de Lucena RP, da Silva da Rocha EM, de Souza Baptista AR, et al. (2018). Diagnóstico laboratorial da esporotricose felina em amostras coletadas no estado do Rio de Janeiro, Brasil: limitações da citopatologia por imprint. Rev Pan-Amaz Saude. 9(2):13-19.
- Marques ABS, Smaniotto C, Dias DCS, Gusso ABF, de Carvalho RJMP, de Camargo MHB, et al. (2022). Esporotricose felina na região periocular-eficácia do tratamento com itraconazol. Acta Scientiae Veterinariae. 50(Suppl 1):744.
- Gonçalves JC, Gremião IDF, Kölling G, de Almeida Duva AE, Ribeiro PMT, et al. (2019). Esporotricose felina, o gato e a comunidade. Enciclopédia Biosfera. Centro Científico Conhecer–Goiânia. 16(29):769-787.
- Pires C. (2017). Revisão de literatura: esporotricose felina. Revista de Educação Continuada em Medicina Veterinária e Zootecnia do CRMV-SP, , Brazil, São Paulo: Conselho Regional de Medicina Veterinária. 15(1):16-23.
- Barros MBL, Schubach TP, Coll JO, Gremião ID, Wanke B, Schubach A. (2010). Esporotricose: a evolução e os desafios de uma epidemia. Rev Panam Salud Publica. 27(6):455-460.
- Pimentel MC, Bolzan Q, Sommer C, Martins DB, Fiss L, Rossato CK, et al. (2011). Esporotricose felina–relato de caso. XVI Seminário Interinstitucional de ensino, pesquisa e extensão, Unicruz.
- Neves BF, da Nóbrega LB, Fernandes MV, de Barros YO, Trindade LC. (2018). Esporocritose: relato de caso. Revista de Ciências & Saúde Nova Esperança. 16(1):26-32.
- Heidrich D, Stopiglia CDO, Senter L, Vectoratto G, Valente P, Scroferneker ML. (2011). Sucesso terapêutico da terbinafina em um caso de esporotricose. Anais Brasileiros de Dermatologia. 86(4):182-185.
- Ferreira AO. (2008). Guia Prático da Farmácia Magistral. Juiz de Fora, Brazil.
- Leal LB, da Silva MDCT, Bedor DCG, Pimentel MF, de Santana DP. (2008). Desenvolvimento de teste de dissolução para o meloxicam utilizando o Planejamento fatorial: estudo comparativo de produtos industrializados X produtos magistrais. Revista Brasileira de Farmácia. 89(2):160-163.
- Vieira Filho G. (2003). Gestão da qualidade total: uma abordagem prática. Brazil, Campinas: Alínea.
- Pontes FA. (2007). Medicamentos manipulados: avaliação dos processos e dos laudos de análise das amostras recebidas pelo Laboratório Central Noel Lutels (2003-2006). PPGVS/INCQS. FIOCRUZ.
- Secretaria de Saúde do Estado de Minas Gerais. SES/MG investiga suspeita de 08 óbitos por intoxicação medicamentosa.
- da Silva FDS, dos Santos Cunha SC, de Moraes VA, da Silva Leite J, Ferreira AMR. (2020). Esporotricose felina: um relato de caso de disseminação cutânea e sistêmica em gato negativo para FIV e FeLV. Revista Brasileira de Ciência Veterinária. 27(4):183-187.
- da Silva BTM, Bentudo HDL. (2021). Esporotricose localizada em felino jovem: relato de caso. Research, Society and Development. 10(17):1-9,
- da Luz MV, Bergoli R, Giacomolli C, Gnoatto F, Pesamosca N, Bassuino DM, et al. (2017). Tratamento terapêutico com Itraconazol® em um felino com esporotricose. XII Seminário Interinstitucional de ensino, pesquisa e extensão.
- Teixeira GNRF, Teixeira, Soares DFM, Keller KM, Silva JAMC, Parents GCT, Morais MHF, et al. (2016). Esporotricose e implicações à saúde pública com vistas à ocorrência da doença no município de Belo Horizonte. Cadernos Técnicos de Veterinária e Zootecnia. 82:46-58.
- da Rosa CS, Meinerz ARM, da Gama Osorio L, Cleff HM, Meireles MCA. (2017). Terapêutica da esporotricose: revisão. Science and Animal Health. 5(3):212-228.
.png)