Information Links
Related Conferences
Previous Issues Volume 4, Issue 1 - 2020
The Traditional Chinese Medicine Intervention of Pre-diabetes Based on Information Platform: Study Protocol for A Clinical Trial
Deng JL#, Dai Y#, Li PL, Zhao LG, Shan MY, Ren XD, Xu ZH*
Department of Intergrative Medicine, Xinqiao Hospital, Third Military Medical University, Chongqing, China *Corresponding author Xu ZH, Department of Intergrative Medicine, Xinqiao Hospital, Third Military Medical University, Chongqing, China, E-mail: [email protected]
Received Date: May 13, 2020 Published Date: July 07, 2020 Copyright: Xu ZH, et al. ©2020. Citation: Xu ZH. (2020). The Traditional Chinese Medicine Intervention of Pre-diabetes Based on Information Platform: Study Protocol for A Clinical Trial. Mathews J Diabetes Obes. (4)1: 01.
ABSTRACT Background: Diabetes has become the third largest non-infectious disease threatening public health. The awareness rate of type 2 diabetes in Chinese adults is only 30.1%. Clinical studies have shown that nearly 11% of pre-diabetes patients develop into diabetes without any intervention every year. Once developed into diabetes, it will seriously affect the physical and mental health of patients and bring a heavy burden to individuals, families, and society. Therefore, it is necessary to carry out early interventions in the pre-diabetes population to effectively curb the increasing prevalence of diabetes. Methods: This study is a single-center and randomized parallel design trial. In this trial, 500 participants will be recruited and randomly assigned to the intervention group and the control group at a ratio of 1:1. Taking advantage of the modern information technology platform and combining with the traditional Chinese medicine treatment strategy, a network-intervention method of “individual-family-society” is constructed, and its effect will be evaluated. Objective: The purpose of this study is to establish a new community intervention model suitable for the prevention and controlling of diabetes or some other chronic diseases, and to build a foundation for the development of new ideas for disease prevention and improvement of population health. Trial registration: 2016-Yan-No.033-01 from Human Research Ethics of Xinqiao Hospital of the Third Military Medical University. Keywords: Protocol; Pre-diabetes; Information platform; Clinical trial Abbreviations: TCM: Traditional Chinese Medicine; IFG: Impaired Fasting Glucose; FPG: Fasting Plasma Glucose; 2hpg: 2 Hour-Plasma Glucose; OGTT: Oral Glucose Tolerance Test; BMI: Body Mass Index. INTRODUCTION Type 2 diabetes is a disease caused by genetic and environmental factors that endanger public health [1]. At present, hereditary factors are still unknown, and it has been confirmed that type 2 diabetes is closely related to a high-calorie diet, lack of exercise, obesity, etc. [2,3]. It has been reported that the overall incidence of diabetes in Chinese adults is about 11.6%, and the pre-diabetes incidence in these people is 50.1%. However, the awareness rate of type 2 diabetes is merely 30.1%, and numerous pre-diabetes patients do not receive any interventions and eventually developed into diabetes every year [4,5]. Once developed into diabetes, the long-term hyperglycemia will affect multiple tissues and organs of the whole body, leading to various complications, such as cardiovascular and cerebrovascular diseases, chronic kidney disease, amputation, retinopathy, etc. [6-10]. Therefore, the early intervention must be carried out on the pre-diabetic population to reduce the growth rate of pre-diabetes to diabetes. As the main environmental risk factors mentioned above are known to all, many countries have carried out intervention research to prevent the further development of diabetes. The Chinese Daqing Diabetes Prevention Study [11], the Finnish Diabetes Prevention Study [12], and the US Diabetes Prevention Program [13] are regarded as milestones of diabetes prevention. Daqing Diabetes Prevention Study has spent 30 years to prove that lifestyle intervention can effectively prevent diabetes, reduce the incidence of complications including myocardial infarction, cerebral infarction, sudden death, and significantly reduce mortality [11]. In the US diabetes prevention program [14], 3234 patients with IGT were randomized into the intensive lifestyle intervention group, metformin + conventional lifestyle group, and the control group. After an average follow-up of 2.8 years, the incidence of diabetes in the lifestyle intervention group and the metformin group decreased by 58% and 31%, respectively. Researchers continued to follow up 2766 patients in this study for seven years, and the results showed that compared with the control group, the incidence of diabetes in the lifestyle intervention group reduced by 34%, while that in the metformin group decreased by 18%. Subsequently, lots of research groups conducted similar studies and achieved the same results [15-18]. All these studies have confirmed that comprehensive behavioral interventions, such as weight loss, exercise, and a healthy diet, can effectively prevent diabetes, and the development of scientific and effective health behavioral interventions will help improve the long-term health of their communities. In recent years, prospective clinical intervention studies [19-21] have shown that lifestyle changes or drug interventions could restore blood glucose to normal levels in pre-diabetes, and reduce the incidence of diabetes. However, there is still a lack of effective interventions for pre-diabetes patients, and the effects of intervention are limited. Among the interventions, TCM is highly praised for its amazing efficacy and small side effects in the prevention and treatment of diabetes [22-24]. The use of TCM in the early stage of diabetes is a critical approach to prevent the development of diabetes. Scientific and effective health behavior interventions with TCM will help improve the health of pre-diabetes people in the community. METHODS Study Design The study is a single-center and randomized parallel-group study. Based on the fundamental propositions laid out in the Declaration of Helsinki, we have received permissions from all the adult subjects. All trial procedures are carried out in the Xinqiao Hospital of the Third Military Medical University in China. The 500 recruited participants are randomly assigned to two groups: the control group and the intervention group.
Ethics Approval The trial is being conducted at the Xinqiao Hospital of the Third Military Medical University, Chongqing, China. This trial was designed ethically under the guidance of the Declaration of Helsinki. All trial procedures are in the interests of the participants. The present study protocol has already been ethically reviewed and further approved by the Ethics Review Committee on Traditional Chinese Medicine with the ethical approval identifier of 2016-Yan-No. 033-01.
Participants All participants have pre-diabetes. They will be briefed on the study and informed to fill out a general information form during their initial visit to the investigator. Based on the baseline information, eligible participants will be familiar with all the benefits and potential damages that they may suffer in this trial. Besides, they have the right to withdraw the study at any time without specific reasons. Further procedures, such as recruitment, physical examination, and randomization will only be carried out after the participants provide the written informed consent. Inclusion Criteria 1) Voluntarily participate in the test and sign the informed consent 2) Pre-diabetes patients are defined as: 1. IFG:FPG≥6.1mmol/L (110mg/dl) and<7.0mmol/L (126mg/dl), 2hPGafter the OGTT<7.8mmol/L (140mg/dl) 2. IGT: FPG<7.0mmol/L(126mg/dl),and 2hPG after OGTT ≥7.8mmol/L (140mg/dl) and<11.1mmol/L (200mg/dl) according to the WHO Diabetes Classification Standard, if both IGT and IFG are present, the diagnosis result is IGT 3) Both male and female participants 4) Over 25 and under 60 years old 5) Overweight or obese: 24kg/m2≤ BMI <35 kg/m2 6) Able to use WeChat or short message 7) Able to provide a family member, 1-2 friends or colleagues to participate in this intervention test Exclusion Criteria 1) Has been diagnosed as a diabetic patient 2) Unable to use mobile phone text messages or WeChat 3) Diagnosed by a clinician to be unsuitable for participation in the study, such as having severe cardiovascular and cerebrovascular diseases, mental and psychological diseases, cancer, etc. 4) Be pregnant or breastfeeding (excluding women who will end breastfeeding in the following six weeks) and women who have a pregnancy plan during the study period 5) Another member of the family is a staff member of the trial or a participant in the study 6) Current or previous participation in other intervention research projects that may affect the effectiveness of this intervention 7) Those who have taken hypoglycemic agents, lipid-lowering and weight-loss drugs in the past six months 8) Those who are thought to have any other conditions that are not suitable for entering this study. Randomization After enrollment following physical examination at the first visit, the investigator collects and inputs medical history and baseline information of all subjects and enters them into a case report form with his/her own account. According to the principle of random grouping, the community was randomly assigned to the intervention group and the control group at a ratio of 1:1 to ensure the comparability of the two groups at baseline. The randomization code is available only to the researchers who have no further role in the recruitment and treatment of subjects. The statistical data will be analyzed by the researchers who don’t participate in the whole sessions.
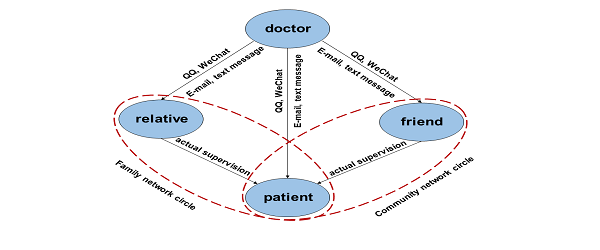
Information Platform Construction Build an intervention network: three core network circles and five network connection routes have been established (Figure 1).
Figure 1: Community pre-diabetes patient intervention network.
The network circle of health institutions is composed of clinicians, health education experts, psychologists, nutritionists, etc. They are mainly responsible for the design, implementation and evaluation of intervention projects, providing funds, platforms, technologies, information, and instructions for the project, real-time evaluation, and improving the content of measures; Family network circle refers to the family core members provided by patients, who concern about the health of the family and could interfere with the behavior of patients. They are mainly responsible for the basic unit of behavioral execution, receiving intervention information and disseminating information, supervising patients to execute intervention instructions, and responding to instruction requirements. The community network circle is composed of 1-2 friends or relatives provided by patients. They are mainly responsible for the auxiliary chain of behavior execution, monitoring the behavioral changes of patients, and increasing the intensity of intervention information. Intervention Package Design The intervention package refers to intervention instructions for the community, including standardized and personalized behavior, diet, and exercise menus. The design method is completed by the system analysis and qualitative research. Intervention 1. Health survey The pre-diabetes people were screened and examined to investigate their health status, including gender, age, ethnicity, occupation, education, smoking, drinking, eating, sleep, exercise habits, etc., and measure the fasting blood glucose, blood pressure, blood lipids, and BMI. 2. TCM constitution identification The subjects will be identified by the “Traditional Chinese Medicine Quality Table” and “Traditional Chinese Medicine Classification Standards”. The Chinese medicine clinician will diagnose the individuals. After that, all the results are combined to finally determine the test subject’s corporeity. Individualized treatment such as early lifestyle and Chinese medicine intervention will be made according to the physical characteristics of pre-diabetes. 3. Health guidance The unhealthy diet is an important factor leading to pre-diabetes and diabetes. Therefore, reasonable diet control is helpful in improving the metabolic imbalance of the body. For patients with IGT, good dietary compliance will enable them to obtain the optimal metabolic control. The corresponding TCM dietary guidance will also be given according to different constitution types. 4. Sports guidance Glucose uptake in non-insulin-dependent tissues and insulin sensitivity can be increased through exercise, which is helpful to control blood sugar and lose weight. The IGT people are encouraged to carry out appropriate physical activities. It is believed that the medium-intensity activity like Tai Chi is a great choice. Tai Chi can move the whole-body joints and muscles, regulate mental stress, enhance cardiopulmonary function, promote blood circulation, and improve the metabolism and various physiological functions of the human body. 5. Face-to-face health guidance During the baseline survey, all participants will receive 20-30 minutes of health guidance on the basic knowledge of pre-diabetes to improve the understanding of pre-diabetes and project compliance. The health guidanceis performed by professional clinicians or diabetes specialists. 6. Information technology intervention Behavioral interventions are implemented through WeChat or phone text message platform to send the intervention package information; 1) Overweight and obese, the basic body weight is reduced by 5%-7% 2) Daily physical training 3) Recommend a reasonable diet 4) Avoid smoking and alcohol The intervention information will be periodically sent to the family or friends of patients through the software platform. The intervention information reflects the personalized characteristics, which means that the content of the short message received by each participant is based on the baseline condition of the patient with the same total amount of information. The information content of the patient’s family members or friends should reflect the importance of social support to the patients’ behavior intervention. Outcome Measurement At the beginning of the survey, 3, 6, 12, 24, 36 and 60 months after the intervention, the incidence of diabetes is assessed by the questionnaire, physical measurement, and biochemical indicators. The effect indicator such as blood glucose (FPG, 2hPG), BMI, blood pressure, blood lipids (triglycerides, total cholesterol, high-density lipoprotein cholesterol, and low-density lipoprotein cholesterol) will be tested. The lifestyle quality score (SF-36) [25], physical activity and eating behavior scores, and the knowledge level of diabetes prevention and control will also be evaluated. The entire flowchart is as shown in figure 2.
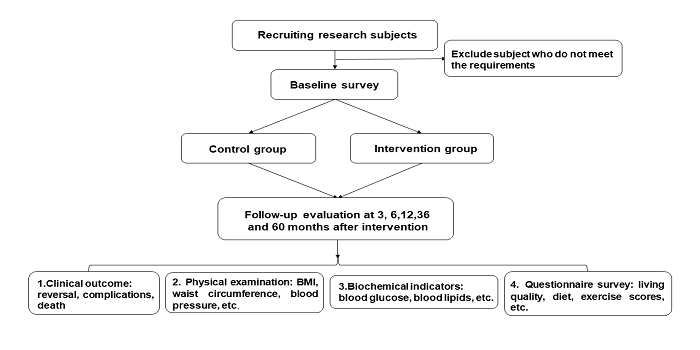 Figure 2: Flow chart of this protocol.
Figure 2: Flow chart of this protocol.
Sample Size According to the literature, after one year of pre-diabetes intervention, the 2hPG of the intervention group and the control group were 8.05 ± 3.00 and 7.11 ± 2.25, respectively, and the variance was 9.0. With the test level α = 0.05 (bilateral) and β = 0.20 (power = 80%), 320 samples are required to be calculated. The diabetes conversion rate in the pre-diabetes population was 10-15% per year in the previous study. With RR = 0.5 in the control group and the intervention group, α = 0.05 (bilateral), and β = 0.20 (power = 80%), 394 samples are required to be calculated. In order to avoid the final effect evaluation of the control group and the loss of the study subjects during the implementation of the project, the final sample size is determined to be 500 cases. Data Analysis The relevant data are analyzed through the statistical method, and the SPSS 21.0 software package is used for t test, F test, χ2 test, and logistic regression model analysis. The relative risk ratio (odds ratio) was used to estimate the relevant risk factors. DISCUSSION Diabetes includes several metabolic disorders characterized by increased blood glucose, which is a chronic disease seriously affecting human health [26]. It is estimated that there were nearly 415 million people with diabetes in 2015 around the world, of which 5.0 million died of diabetes [27]. The incidence rate of pre-diabetes among Chinese adults is 50.1%. Unfortunately, alarge part of them is developed into diabetes without any intervention every year [4,5]. Type-2 diabetes can be prevented by changing the lifestyles of high-risk subjects. Therefore, how to effectively prevent the conversion of pre-diabetes into diabetes is extremely urgent. The intervention subjects included in this study are pre-diabetes patients. It is shocking that so many people do not realize that they are in pre-diabetes as well as the importance of controlling in time. The unawareness tends to be the main cause of the formation of diabetes. As investigated, plenty of studies have found that type 2 diabetes can be controlled by diets, exercise, or both for individuals in pre-diabetes [28-31]. Nevertheless, interventions may be useful in some countries or societies, but may not work in other countries, because the social situation, economic, and cultural forces will have significant influences on the diets and exercise [32]. Besides, how to make patients have proper compliance is also vital. Therefore, it is critical for the pre-diabetes population to find some applicable and suitable interventions in China. Thus, it is of great social significance to observe and analyze the behavioral characteristics of the pre-diabetes population, find some corresponding coping methods or techniques, and accumulate experiences for overcoming the difficulties of behavioral interventions. In this study, the Internet will be adopted to build an intervention network composed of society, families, and individuals, aiming to construct a comprehensive and the effectiveness pre-diabetes intervention model in combination with virtual and reality. Furthermore, mobile phone text messages and WeChat will also be used in the intervention of this study, which can reduce the cost of interventions and avoid the shortage of medical staffs. Multiple intervention opportunities, roles, and information are combined in this network to enhance the interventionist’s execution, inspire the patient’s initiative, and improve the intervention effectiveness. Moreover, the network can also be used as a test to develop a healthy behavioral model and establish a platform for the intervention research and the promotion of health behavior of similar chronic diseases. At present, as an essential part of health care, TCM is getting more and more attention and popularization in the whole world due to its remarkable efficacy and small side effects. As a complementary and alternative medicine, TCM has been widely used to prevent and cure diabetes and its complications in Asian countries [33-35]. TCM can regulate the overall function of human body, and it has special superiorities in the treatment of diabetic related diseases. The mechanisms of TCM function is considered to be achieved through multiple links, channels, and factors. Wen P [36] used Liu wei Di huang pill (The prescription contains Shudihuang, Shanzhuyu, Mudanpi, Shanyao, Fuling, and Zexie) and Huangqi to treat diabetic nephropathy, Tian J [37] treated diabetic kidney disease with Shen zhuo formula (The prescription includes Gancao, Ganjiang, Fuling and Baizhu), Wang TZ [38] adopted YiqiHuajuQingli formula (The formula composed of Huangqi, Huanglian, Puhuang, Zexie, Ludouyi, Liuyuexueand Fuzi) for the treatment of metabolic syndrome, and they all achieved great curative effect. The application of TCM treatment in the early stage of diabetes is critical for preventing the occurrence and development of diabetes. Based on the guidance of TCM theory, the establishment of an integrated system combining TCM and western medicine for early prevention and intervention of diabetes will definitely be more effective. In the complete network information platform constructed in this study, pre-diabetes patients will receive the timely and accurate intervention to prevent further development of diabetes. The intervention instructions issued by the platform can precisely combine the actual situations of each patient. In addition to the regular diet or exercise intervention, the content will also be based on the doctors’ analysis on the patient’s specific condition, combined with TCM and western medicine integrated intervention. The intervention mode can make full utilization of the social network circle of society, friends, and family to improve the patients’ compliance, which largely determines the conversion of pre-diabetes into diabetes. The method can greatly decrease the risk of diabetes for pre-diabetes patients. Furthermore, it can reduce the workload of medical stuffs and the cost of the social medical care. Once the intervention mode is mature, it can be widely applied to the early intervention of various chronic diseases, leading to a decrease of the prevalence of chronic diseases and the social medical costs. Disclaimer Statements All authors were involved in the design, gathering of information, write up and final edits.
Funding This work was supported by the grants from the National Natural Science Foundation of China (Nos. 8162800042, 8157041835) and a Clinical Research Award from the Third Military Medical University. Declaration of Interest None. Patient Consent Obtained. The Author Contribution JLD–manuscript writing. YD, JLD and ZHX–participated in the design of this trial. PLL, LGZ, MYS, XDR and ZHX–critical revision of manuscript. All authors wrote, read and approved the final manuscript, and agree to be accountable for all aspects of the work. The authors would like to thank all the participants involved in this study.
Ethics and Dissemination This study passed ethical approval by Medical Ethics Committee of the Second Affiliated Hospital of the Third Military Medical University of the Chinese People's Liberation Army, and the ethical approval identifier is 2016-Yan-No.033-01.
REFERENCES
- Shaw JE, Sicree RA, Zimmet PZ. (2010). Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res Clin Pract. 87(1):4-14.
- Franks, Paul W. (2012). The Complex Interplay of Genetic and Lifestyle Risk Factors in Type 2 Diabetes: An Overview. Scientifica. 2012(11):1-11.
- Pan XR, Li GW, Hu YH, Wang JX, Yang WY, et al. 1997. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance. The Da Qing IGT and Diabetes Study. Diabetes Care. 20(4):537.
- Martinovic AB, Zdravkovic A. (1981). A mass survey of diabetes mellitus in a population of 300,000 in 14 provinces and municipalities in China. Chin J Intern Med. 20(11):678-683.
- Xu Y, Wang L, He J, Bi Y, Li M, et al. (2013). Prevalence and control of diabetes in Chinese adults. JAMA. 310(9):948-959.
- Gerstein HC, Yusuf S, Bosch J, Pogue J, Sheridan P, et al. (2006). Effect of rosiglitazone on the frequency of diabetes in patients with impaired glucose tolerance or impaired fasting glucose: a randomised controlled trial. Lancet. 368(9541):1096-1105.
- Lee JY, Jeon I, Lee JM, Yoon JM, Sang MP. (2013). Diabetes mellitus as an independent risk factor for lung cancer: a meta-analysis of observational studies. Eur J Cancer. 49(10):2411-2423.
- Erbach M, Mehnert H, Schnell O. (2012). Diabetes and the risk for colorectal cancer. J Diabetes Complicat. 26(1):50-55.
- Boyle P, Boniol M, Koechlin A, Robertson C, Valentini F, et al. (2012). Diabetes and breast cancer risk: a meta-analysis. Br J Cancer. 107(9):1608-1617.
- Shimoyama S. (2013). Diabetes mellitus carries a risk of gastric cancer: a meta-analysis. World J Gastroenterol. 19(40):6902-6910.
- Zimmet PZ, Magliano DJ, Herman WH, Shaw JE. (2014). Diabetes: a 21st century challenge. Lancet Diabetes Endo. 2(1):56-64.
- Uusitupa M, Louheranta A, Lindström J, Valle T, Sundvall J, et al. (2000). The Finnish diabetes prevention study. Br J Nutr. 83(S1):S137-S42.
- Group DPPR. The Diabetes Prevention Program (DPP): description of lifestyle intervention. Diabetes Care 2002;25(12):2165-2171.
- Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, et al. (2002). Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med. 346(6):393-403.
- Harati H, Hadaegh F, Momenan AA, Ghanei L, Bozorgmanesh BR, et al. (2010). Reduction in incidence of type 2 diabetes by lifestyle intervention in a middle eastern community. Am J Prev Med. 38(6):628-636.
- Lindström J, Ilanne-Parikka P, Peltonen M, Aunola S, Eriksson JG, et al. (2006). Sustained reduction in the incidence of type 2 diabetes by lifestyle intervention: follow-up of the Finnish Diabetes Prevention Study. Lancet. 368(9548):1673-1679.
- Nicolucci A, Balducci S, Cardelli P, Cavallo S, Fallucca S, et al. (2012). Relationship of exercise volume to improvements of quality of life with supervised exercise training in patients with type 2 diabetes in a randomised controlled trial: the Italian Diabetes and Exercise Study (IDES). Diabetologia. 55(3):579-588.
- Tuomilehto J, Lindström J, Eriksson JG, Valle TT, Hamalainen H, et al. (2001). Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med. 344(18):1343-1350.
- Rejeski WJ, Ip EH, Bertoni AG, Bray GA, Evans G, et al. (2012). Lifestyle change and mobility in obese adults with type 2 diabetes. N Engl J Med. 366(13):1209-1217.
- Valencia WM, Stoutenberg M, Florez H. (2014). Weight loss and physical activity for disease prevention in obese older adults: an important role for lifestyle management. Curr Diab Rep. 14(10):539.
- Shah K, Villareal DT. (2013). Weight loss and improved fitness slow down the decline in mobility in obese adults with type 2 diabetes. Evidence-Based Medicine. 18(2):e18.
- Chen Z, Liu X, Chen D, FUQ, Liu Y. (2001). Observation of clinical efficacy on prescriptions of traditional Chinese medicine in 60 cases of type 2 diabetes. J Chin Physician. (08):1035-1037.