Information Links
Related Conferences
Previous Issues Volume 5, Issue 2 - 2020
Improving Glycemic control and Optimizing Care of the Surgical Patients - A Retrospective Longitudinal Study
Leopoldo Muniz da Silva*, Arthur de Campos Vieira Abib, Saullo Queiroz Silveira, Rafael Souza Fava Nersessian, Renata Mazzoni de Queiroz, Anna Beatriz Aranha, Wilson Porfírio de Medeiro Nunes
Anesthesiology Departmentof São Luiz Hospital - Anália Franco/ Rede D òr – CMA Anestesia team, São Paulo, SP, Brazil
*Corresponding author: Leopoldo Muniz da Silva, Rua Dr. Alceu de Campos Rodrigues, 229, Conj. 403, CEP 04544-000 – São Paulo, SP, Brazil, E-mail: [email protected].
Received Date: June 29, 2020 Published Date: December 09, 2020 Copyright: da Silva LM. © 2020. Citation: da Silva LM, et al. (2020). Improving Glycemiccontrol and Optimizing Care of the Surgical Patients - A Retrospective Longitudinal Study. Mathews J Emergency Med. (5)2:36.
SUMMARY
Introduction: The target-guided glycemic control was proposed to reduce the occurrence of perioperative morbidity by improvement of healthcare. Meantime, to promote adherence to the protocol and ensure effectiveness in clinical outcome, it is necessary to study and develop promoting and divulging strategies, associated to continuing education of medical assistance staff. Thus, based on the concept of quality improvement in health process, the present study intend to evaluate strategies and interventions to increase adherence to the perioperative glycemic control protocol and the effectiveness of the implemented actions in clinical outcome of the evaluated patients.
Methods: Retrospective longitudinal study conducted from January 2017 to December 2018 in a tertiaty hospital. Monthly, adherence rates to the glycemic control protocol and educational strategies adopted to improve adherence each month were analyzed. Data were compared after each change made to assess the trend and consolidation of safety culture in relation to the protocol application. The medical continuing education program (MCEP) constitutes in a strategy of focused and individualized training. The anesthesiologist who presented nonconformity in any action of the protocol, received an individualized training, dialogue-based interactive exposure and in review articles about the discussed theme. Results: The initial adherence rate to the protocol was 20%. Comparing the adherence rate in the first 6 months (median = 46 [40-5.5]), in which three initial dissemination strategies were implemented, with the following 6 months (median = 55 [54-57.75]), there was no lasting and positive improvement (p = 0.09). The median adherence rate to the protocol in 2017 was 54% (52-57%). Comparing seven months before the implementation of the medical continuing education program (MCEP) (median=54 [53-57,5]), with the following seven months (median=75 [69,5-75,5]), with a 39% increase in the indicator’s baseline when comparing periods pre and post-implementation of MCEP (p<0,001). The effectiveness rate of the protocol in adjusting glycemic level within the stipulated range was 93,5%.
Conclusion: The management strategy of the glycemic control protocol and continuing medical education as an intentional action was effective in adjusting glycemic level within the stipulated range in improving the quality of care for perioperative glycemic management.
KEYWORDS: Education; Continuing; Blood glucose; Intraoperative
INTRODUCTION
Quality problems in health care incur loss of opportunity of better results regarding avoidable damage and unnecessary costs. Actions designed to develop changes to address such matters in healthcare institutes are still poorly fomented and divulged as validated tools to improve health processes [1]. Initiatives to improve quality of healthcare and patient’s safety frequently endup generating changes that are limited, not sustainable and difficult to replicate especially considering diverse organizational contexts [2,3]. Healthcare quality improvement is defined by changes that produce, directly or indirectly, better healthcare outcomes in a lasting manner, encompassing standardized technical concepts, but, mainly, favoring interaction of processes and actions in a multidisciplinary context4. In the analysis of surgical patient care, perioperative hyperglycemia is a prejudicial and quite common condition, especially in diabetic patients who represent a growing portion of this population. Hyperglycemia presents several causes, standing out among them the endocrine-metabolic-immunological response to stress, leading to various deleterious organic alterations, as increased inflammatory response, susceptibility to infection, injury and disfunction of multiple organs and systems. Thus, the implement of a managed perioperative glycemic control protocol, with patronization of healthcare procedures, target setting theory and evaluation of adherence by the anesthesiologist assistants to these recommendations, with analysis of the effectiveness of the protocol in patient outcome, is crucial [5].
The target-guided glycemic control was proposed to reduce the occurrence of perioperative morbidity by improvement of healthcare. Meantime, to promote adherence to the protocol and ensure effectiveness in clinical outcome, it is necessary to study and develop strategies, associated to continuing education of medical assistance staff. We hypothesized that Continuing Medical Education can be used successfully to change physician attitudes and practice. Thus, based on the concept of quality improvement in health process, the present study intend to evaluate strategies and interventions to increase adherence to the perioperative glycemic control protocol and the effectiveness in adjusting glycemic level within the stipulated range.
METHODS
Retrospective longitudinal study conducted from January 2017 to December 2018 in atertiary hospitalat São Paulo, Brazil. We reincluded all 322 surgical diabetic patients with Type I and II diabetes mellitus (2.5% of 12.800 surgeries in two years).
The perioperative glycemic control protocol was established in 2017, with it’s publication in the information channels of the Hospital. Since January 2017, medical records were audited monthly to evaluate conformity of the glycemic control protocol. Diabetes mellitus reported by the patient during preanesthetic consultation were inclusion criteria in the monthly audit. All medical records were audited through electronic charts: preanesthetic consultation chart (measured preoperative capillary blood glucose), anesthetic records (propermonitoring, management and serial results of blood glucose adequately registered), post-anesthetic recovery chart (follow up of the monitoring and transfer of care to the medical ward or intensive care unit). In order to characterize conformity, all steps of the process related to the protocol should be conform properly registered in medical records. Data obtained were included in a specific database for the formulation of monthly indicators, analysis and elaboration of improvement strategies accordingly to results obtained by the hospital’s quality sector. It contained the monthly adherence rate to the protocol and the educational strategies adopted to improve adherence month-to-month. Monthly data were compared after each change made to assess trend and consolidation of safety culture in relation to the protocol application. The indicator of adherence rate was calculated by the number of patients with conformity in all steps of protocol divided by the number of patients analyzed per month x 100.
Strategies adopted to increase adherence to the protocol were, in sequence: 1 – Elaboration of a written document (protocol) and it’s publication in information channels of the institution (January 2017) 2 – Divulging lectures and discussion of the proposed actions (March 2017) 3 - Monthly meeting with medical staff for discussion of monthly indicators results and suggestions of necessary adjustments (May 2017) 4 – Creation of illustrated and informative flowcharts about de protocol actions and distribution of it in all operating rooms for consultation by the medical staff (August 2017) 5 – Continuing education program (January 2018). The medical continuing education program (MCEP) constitutes in a strategy of focused and individualized training. The anesthesiologist who presented nonconformity in any action of the protocol, received an individualized training, dialogue-based interactive exposure and in review articles about the discussed theme. To select the articles, the inclusion criteria were: articles published in a free full-text manner in periodic in selected databases, suitable to the proposed objective and descriptors and/or keywords listed in the protocol previously validated. The physician, after training, received study material and was subjected to a post-test composed of objective questions about preoperative glycemic control. The stablished target of correct answers was above 85%. Approval in conformity test after training was linked to the annual evaluation of performance of each member of the anesthesiologists staff.
The same staff of anesthesiologists remained working at the hospital during the assessed period and the new anesthesiologists who entered the team were subjected to institutional integration process, standardizing the consciousness of the protocol by the staff. The total number of physicians participating was 37.
INSTITUTIONAL GLYCEMIC CONTROL PROTOCOL
According to the institutional protocol, all diabetic patients should have preoperative capillary blood glucose tested and should be subjected to the specific management by the anesthesiologist. Preoperative testing of capillary blood glucose could take place in the preoperative period, at the medical wardor in the beginning of the surgery, in anurgency/emergency context. Test results must be clearly indicated on medical records.
The glycemic target for diabetic patients is upto 180 mg/dL. Diabetic patients with glycemia >180 mg/dL should be tested once an hour and the management of blood glucose should be established by continuing infusion of glucose and insulin or intravenous bolus of insulin, according to evaluation of the anesthesiologist and considering the magnitude of the surgery and the patient’s previous clinical status [6]. It is recommended that patients with adequate glycemic control must have capillary glucose tested once every two hours, with proper information registration on anesthetic chart. If blood glucose was lower than 70 mg/dL (hypoglycemiacriteria), it is recommended fast infusion of 25 mL of glucose 50% until normalization and then monitors glycemia once an hour. Every measurement of intraoporetive glycemia should indicate the time, so that the following monitoring of blood glucose continues during the whole studied period. Basal capillary blood glucose collected in preoperative period was the time reference adopted to further testing during intra operative monitoring, as well as therapeutic management referring glycemic control. If capillary blood glycemia remains above 180 mg/dL when patient is discharged from the post-anesthesia care unit (PACU) or transferred to the intensive care unit, the anesthesiologist must communicate the physician responsible for the medical ward or the intensivist, seeking the continuity of care and aiming better postoperative glycemic control, with proper registration on medical record.
STATISTICAL ANALYSIS
Improvement Science in Healthcare Quality considers as essential compounds: technical relevance of the intervention, the implementing strategy and the context in which the intervention is implemented [7]. This theoretical model states that, in order to a strategic change result in improvement, it must be lasting, relevant, positive and intentional.
Measurements of central and dispersion tendencies of the monthly analyzed indicators in historical series were the median and inter quartiles 25-75%, after analysis of distribution on the normal bell curve. In order to evaluate de effectiveness in promoting lasting, relevant and positive improvements, actions were compared by the median monthly indicators of quality pre and post-implementation. To address the comparison between these two periods of time, the Mann-Whitney test was applied. Confidence interval of 95% and p < 0,05 was the criteria of statistical significance. Statistical analysis was assessed by Statistical Package for Social Sciences 20.0 Mac (SPSS 20.0 Mac, SPSS Inc., Chicago, Illinois, EUA).
RESULTS
In 2017, the initial adherence rate to the protocol was 20%. Comparing the adherence rate in the first six months of 2017 (median = 46 [40-53,5], in which three initial strategies of divulgation were implemented, with the following 6 months (median=55 [54-57,75]), there was not lasting and positive improvement, without significant statistical difference between these two periods (p=0,09). The median of adherence rate to the protocol in 2017 was 54% (52-57%) (Table 1).
|
Interventions |
Outcomes |
|
|
Educational strategy |
Adherence rate1 |
Effectiveness in adjusting glycemiclevel |
|
Divulging lectures and discussion of the proposed actions; Monthly meeting with medical staff for discussion about glycemic control (A). |
46 [40-53.5] |
48 [42-56.5] |
|
Creation of illustrated and informative flowcharts about de protocol actions and distribution of it in all operatingrooms for consultation by the medical staff (B). |
55 [54-57.75] |
53 [49.5-56] |
|
The medical continuing education program (focused and individualized training about glycemic control) (C). |
75 [69.5-75.5]) |
93.5 [88-96-5] |
Table 1: Adherence/effectiveness to the glycemic control protocol. 1Values expressed in median (percentile 25-75%). Adherence rate: A = B>C (p < 0.05); Effectiveness in adjusting glycemic level: A = B>C (p < 0.05).
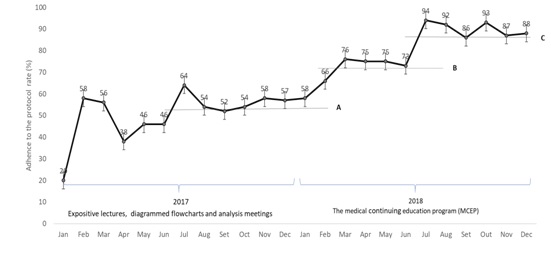
In January 2018, MCEP strategy was started. Comparing seven months before the implementation of MCEP (median = 54 [53-57,5]), with the following seven months (median = 75 [69,5-75,5]), statistically significant difference was observed between the adherence rate median (p = 0,003), with a 39% increase in the indicator’s baseline when comparing periods pre and post-implementation of MCEP. Comparing the year of 2017 (median = 54 [46-57,2]) and 2018 (median = 74,5-89]), there was statistical significant difference (p < 0,001), characterizing a relevant, positive and lasting improvement (Figure 1). The median of the score rate in the after-test took by the anesthesiologists was 92% (90-96,25%).
Figure 1. Adherence to the glycemic control protocol rate in 2017-2018. Values expressed in %. Changes were implemented in 2017, but the improvement process was accomplished in 2018, after implementation of intentional action MCEP (medical continuing education program). Line A (2017) – Median = 54%; Line B (2018) - Median = 75%; Line C (2018) – Median = 90% (p<0,05).
The effectiveness rate of the protocol in adjusting glycemic level with in the stipulated range after MCEP was 93,5%. In 6,5% of cases, glycemia remained over 180mgdL by the end of the surgery. Related factors were: severe active infection (70%) and uncontrolled diabetes before surgery (30%). After MCEP, developing processes and structures to prevent hypoglycemia through glycemic control protocol were implemented. Change and maintain a new culture of improvement that will allow the institution to maintain gains made and to continue improving over time. Preoperative hypoglycemia (capillary blood glucose below 70 mg/dL during pre anesthetic evaluation was diagnosed in 9% of patients (CI 95% [6-14%]). Hypoglycemia lower than 60 mg/dL was observed in 2% of cases (CI 95% [0,79-5%]).
DISCUSSION
Improvement Science in Healthcare Quality achieved recognition in the past few years, being described as the study of development and evaluation of interventions concerning healthcare quality improvement, aiming to explain how these actions are developed, which factors are associated to implementation success and publication of consolidated expected results [8,9]. This study has show that the implementation of an individualized medical education program, with interactive dialogued exposure followed by a knowledge test, was effective in improving the quality of care for perioperative glycemic management and with positive repercussions on the outcome of diabetic patients.
Quality improvement projects that value the conception and implementation of incremental changes and the acquired knowledge are fundamental for the consolidation of assistance processes, which goes beyond merely production of technical-scientific knowledge. These projects are characterized by a broader scope, being a dynamic process of tests and adjustments until the objectives is accomplished. In this analysis, changes made in the strategy of promoting good assistance practice of glycemic control protocol have not become improvement over the year of 2017. During critical analysis of indicators related to glycemic control, some factors were considered barriers to the improvement process, among the mis the gap in medical knowledge regarding the importance of peroperative glycemic control, the underestimated glycemic control in face to other intra operative anesthetic variables to be adjusted, the abscense of connection between the anesthesiologist’s actions during intraoperative period and the patient’s clinical outcome in immediate or late postoperative status and the difficulty of maintaining a patronization of medical management in a work team, generating conflict in transference and continuity of health care.
Over the years, there has been a gradual change in medical education from a passive learning approach to a more active and interactive approach. In order to strengthen the environment of knowledge acquisition, educators should be aware of the different styles of apprenticeship and, therefore, adapt strategies and pedagogical methodologies that optimize learning process [10]. This study observed that passive educational strategies, such as expositive lectures, publishing documents and dissemination of flowcharts and designed boards all over strategic points of the surgical environment, in an isolated manner, did not show to be effective in improving adherence of physicians to the glycemic control protocol. By considering individual non conformities and applying the process of training and evaluation, MCEP guaranteed greater participation of the professionals in the process, improving adherence over the time. The use of interactive dialogued exposures as a learning approach is quoted as promising strategy to develop competences within a continuing educational process [11]. In this approach, the focus is in the dialogue between the facilitator and the physician being trained. In addition, active participation of the physician is valued during the approach [11]. Continuing educational strategies directed to anesthesiologists and critical intraoperative situations, from the pedagogical point of view, are still little studied and must be analyzed and implemented for promotion of improvements in health care in a multidisciplinary context, and also allows strategies to be replicated in other institutions and contexts.
Study capacitation approaches to bring physicians closer to knowledge are mandatory. In addition to distance education, the constant use of resources that support clinical decision, such as protocols for particular contexts of healthcare, is an excellent alternative not only for clinical decision-making, but also to expand healthcare professional’s knowledge. This kind of tool should be incorporated into the workflow, providing more assertive decisions, which corroborates life saving and also cost balancing with avoidable complications. It is important to highlight that passive educational process with expositive lectures, designed boards and indicator’s discussion meetings prior to MCEP also contributed to improvement in adherence to glycemic control protocol, considering that the isolated effect of MCEP could not be quantified in this study, once the previous strategies were not eliminated when MCEP took place, but can be considered as summatory contribution to the objective accomplishment.
Hypoglycemia affects 5 to 20% of hospitalized patients, especially those treated with anti-diabetic drugs or insulin, but it also can occur among non diabetic patients with digestive surgery history, cancer or severe pathologies [12]. Hypoglycemia increases morbid mortality in diabetics and non-diabetic patients regardless of it’s severity. The incidence of hypoglycemia lower than 70 mg/dL is 16%, whereas of every hypoglycemia (lower than 60 mg/dL) is 0,5% within travenous therapy [13]. The hypoglycemia rate in this study was considered compatible with the literature. Factors that may have contributed are long fasting period, major surgical hospital with high turnover, in which patients are admitted short time before surgery and do not have enough time to receive fasting abbreviation solution. In addition, in diabetic patients, the incorrect use of hypoglycemiant drugs during the preoperative period may contribute to the occurrence of peroperative hypoglycemia. However, the analysis of causes of hypoglycemia was not the objective of this study. Yet, in intraoperative period, the absence of diagnosis and proper management of hypoglycemia can result in severe damage to the patient, once it is not possible to evaluate clinical symptoms on patients undergoing anesthesia. The result related to hypoglycemia will be the base for further improvements to be implemented in the protocol, with the purpose of lining up the processes regarding preoperative preparation of diabetic patients and multidisciplinary care after hospital admission for surgery.
When protocol was properly applied during the studied period, there was appropriate effectiveness regarding glycemic targets, with consequent favorable glycemic control outcome in the preoperative period, emphasizing that formal and standardized routines, with settlement of action and monitoring intervals to the assistance staff is effective in improving healthcare management and reduced amage caused by peroperative hyperglycemia.
Rigorous control over blood glucose levels during the preoperative period has been receiving substantial attention over the past 10 years, especially after publications of Van Der Berghe et al. [14], suggesting significant reduction in morbid mortality of critically ill patients. Glycemic control is an important aspect to be observed in prevention of surgical wound infection, occupying an equally relevant position among other traditional preventive measures, such as appropriate antibiotic prophylaxis, normothermia and trichotomy [15].
There still is a considerable distance between the progress of scientific knowledge regarding better management care practices and the care effectively given to the patients. Acknowledge that technical and organizational approaches are complementary in the improvement process of healthcare, as well as the prerogative that scientific evidences favoring determined process are not enough to promote changes in health care, pose new challenges to the area of quality in healthcare and continuing and permanent medical education in health organizations.
Our study does have some limitations. Causation cannot be concluded from this study as we used retrospective design. Because most of the educational strategies not require participants to register, we do not know if factors such as specialty, age, gender, or frequency of computer use to access educational information influenced our findings. We were unable to quantify any potential impact of confounders. The main limitation is that only a few factors were evaluated for adherence to the glycemic control protocol rate. Gender, age, and time since graduation could be used to divide patients into groups for further analysis.
CONCLUSION
Concluding, the management strategy of the glycemic control protocol and continuing medical education as an intentional action was effective in improving the quality of care for perioperative glycemic management.
REFERENCES
- Dyson J, Lawton R, Jackson C, Cheater F. (2013). Development of a theory-based instrument to identify barriers and levers to besthand hygienepractice among healthcare practitioners. Implement Sci. 8:111. doi: 10.1186/1748-5908-8-111.
- Davidoff F, Dixon-Woods M, Leviton L, Michie S. (2015). Demystifying theory and its use in improvement. BMJ Qual Saf. 24(3):228-38. doi: 10.1136/bmjqs-2014-003627.
- Grol R, Wensing M, Eccles M, Davis D. (2013). Improving patient care: the implementation of change in healthcare. Editor(s): Richard Grol Michel Wensing Martin Eccles David Davis. Hoboken: John Wiley& Sons.
- Batalden PB, Davidoff F. (2007). What is “quality improvement” and how can it transform healthcare? Qual Saf Health Care. 16:2-3.doi: 10.1136/qshc.2006.022046.
- Knaak C, Wollersheim T, Mörgeli R, Spies C, Vorderwülbecke G, et al. (2019). Risk Factors of Intraoperative Dysglycemia in Elderly Surgical Patients. Int J MedSci. 16(5):665–674. doi: 10.7150/ijms.32971.
- Duggan EW, Carlson K, Umpierrez GE. (2017). Perioperative Hyperglycemia Management: An Update. Anesthesiol. 126(3):547–560. doi: 10.1097/ALN.0000000000001515.
- Dixon-Woods M, Leslie M, Tarrant C, Bion J. (2013). Explaining Matching Michigan: anethnographic study of a patient safety program. Implement Sci. 8:70. doi: 10.1186/1748-5908-8-70.
- Berwick DM. (2008). The science of improvement. J Am Med Assoc. 299:1182-4.
- Portela MC, Pronovost PJ, Carter P. (2015). How to study improvement interventions: a brief overview of possible study types. BMJ Qual Saf. 24(5): 325–336. DOI:10.1136/bmjqs-2014-003620.
- Silva DM, Leal EA, Pereira JM. (2015). Learning styles and academic performance in Distance Education: a research in specialization courses. Rev Bras Gest Neg. 17(57):1300-1316.
- P Sprawls. (2008). Evolving models for medical physics education and training: a global perspective. Biomed Imaging Interv J. 4(1):16. doi: 10.2349/biij.4.1.e16.
- Umpierrez GE, Hellman R, Korytkowski MT, Kosiborod M, Maynard GA, et al. (2012). Management of hyperglycemia in hospitalized patients in non-critical care setting: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 97(1)16-38. DOI: 10.1210/jc.2011-2098.
- The NICE-SUGAR Study Investigators. (2009). Intensive versus Conventional Glucose Control in Critically Ill Patients. N Engl J Med. 360:1283-1297.
- Van denBerghe G, Wilmer A, Hermans G, Meersseman W, Wouters PJ, et al. (2006). Intensive insulin therapy in the medical ICU. N Engl J Med. 345(5)449-461.
- Tanner J, Padley W, Assadian O, Leaper D, Kiernan M, et al. (2015). Do surgical care bundles reduce the risk of surgical site infections in patients undergoing colorectal surgery? A systematic review and cohort meta-analysis of 8,515 patients. Surgery. 158(1):66-77.