Previous Issues Volume 3, Issue 1 - 2018
Predictors of Clinical Outcome after Intravenous Thrombolysis in Ischemic Stroke without Large Vessel Occlusion: The Role of Admission Glycemia
Bruno Chiara, Colavita Guillaume, Romero Gwendoline, Mahagne Marie-Helene, Suissa Laurent
Stroke Unit - University Hospital of Nice - Pasteur2 Hospital - Voie Romaine - 06000 Nice - France
Corresponding Author: Suissa Laurent, Stroke Unit - University Hospital of Nice - Pasteur2 Hospital - Voie Romaine - 06000 Nice - France, Tel: 0033492032790; E-Mail: [email protected]
Received Date: 05 Oct 2018 Accepted Date: 12 Nov 2018 Published Date: 16 Nov 2018
Copyright © 2018 Laurent S
Citation: BRUNO Chiara, COLAVITA Guillaume, ROMERO Gwendoline, MAHAGNE Marie-Helene, et al. (2018). Predictors of Clinical Outcome after Intravenous Thrombolysis in Ischemic Stroke without Large Vessel Occlusion: The Role of Admission Glycemia. Mathews J Emergency Med. 3(1): 030.
ABSTRACT
Introduction: In the era of mechanical thrombectomy, intravenous thrombolysis (IVT) by tissue plasminogen activator (tPA) remains the first choice treatment for ischemic stroke without large vessel occlusion. In literature few studies are available regarding the acute phase treatment of ischemic stroke without large vessel occlusion. The existence of potential predictive factors of clinical improvement after IVT treatment in this subgroup of stroke patients is not well established.
Aim of the study: To identify predictive factors of clinical outcome in patients treated with tPA alone for acute stroke without large vessel occlusion.
Methods: A retrospective analysis of a prospectively collected database of consecutive patients aged over 18 years, hospitalized in Stroke Unit of Nice from January 2012 to August 2016 for acute ischemic stroke without large artery occlusion, treated with IV tPA within 4.5 hours, were realized. Clinical outcome was apprehended by the modified Rankin Scale (mRS) at 3 months. To determine independent predictive pre-treatment variables of good clinical outcome (mRS=2), univariate and multivariate binary logistic regression models were used.
Results: 162 stroke patients were analyzed in the study. At 3 months, 119/162 (76.46%) patients had mRS=2. The multivariate analysis showed that age (/10 years; OR: 1.62 95%CI[1.10-2.40]), baseline NIHSS (/5 pts; OR: 1.57 95%CI[1.06-2.32]) and admission glycemia (/0.5 g/l; OR 1.63 [1.14-6.25]) were independent predictive factors of poor clinical outcome after IVT.
Conclusion: Age, baseline NIHSS and admission glycemia are independent predictive factors of clinical outcome after IVT. Admission glycemia was the only modifiable independent predictive factor found. Studies are required to demonstrate the potential benefit of an aggressive glucose-lowering treatment for the management of acute hyperglycemia in acute ischemic stroke including stroke treated by tPA alone.
KEYWORDS
Acute Ischemic Stroke; Thrombolysis; Outcome Predictor; Hyperglycaemia.
INTRODUCTION
Stroke is the leading cause of morbidity and mortality in industrialized countries [1]. It is a devastating condition requiring an immediate medical treatment by physicians well experienced in stroke management. Intravenous thrombolysis (IVT) with tissue plasminogen activator (tPA) has been shown to be capable of improving clinical outcome in a selected group of ischemic stroke patients within 4.5 hours after stroke onset [2, 3]. In 2015, randomized controlled trials (RCTs) demonstrated the effectiveness of mechanical thrombectomy (MT) in addition to IVT for acute stroke due to large artery occlusion. Since then, the way of approaching the treatment for any acute ischemic stroke was split, dividing the ones caused by large artery occlusion by the others. Although most of the attention is now focused on the MT, IVT alone remains the first choice treatment for ischemic strokes without large vessel occlusion, which statistically are the most frequent. Nevertheless, in literature few studies are available regarding the acute phase treatment of ischemic stroke without large vessel occlusion. The IVT efficacy is well established but the response to this treatment is variable. In order to select patients who will benefit the most from the IVT treatment, an accurate analysis aimed to detect potential predictive factors of clinical improvement could be very important. In the literature, a number of studies are available on this issue, analyzing demographic and biological characteristic, medication use before stroke and radiological characteristics [4,14]. The aim of this study is to identify predictive factors of clinical outcome for patients affected by stroke without large artery occlusion receiving IVT alone.
MATERIALS AND METHODS
Aim of the study To identify predictive factors of clinical outcome in patients treated with tPA alone for acute stroke without large vessel occlusion.
Patient selection and procedure We performed a retrospective analysis of a prospectively collected database of consecutive patients aged over 18 years, hospitalized in Stroke Unit in Nice from January 2012 to August 2016 for acute ischemic stroke without large artery occlusion, who received a recanalization treatment with IV tPA within 4.5 hours from symptoms onset. We excluded all patients who did not received a vascular neuroimaging at admission and those with missing clinical follow-up or presenting missing data after 3 months period. At the admission, every patient has been evaluated by a neurologist. Stroke severity has been graded using the National Institutes of Health Stroke Scale (NIHSS). Baseline clinical and biological characteristics are recorded. For each patient has been carried out an imaging evaluation by cerebral MRI or CT angiography scan, documenting the absence of large artery occlusion. We recorded radiological data as stroke volume (by circumventing manually hyperintensity area on diffusion weighted MRI (DWI) sequences), MRI Alberta Stroke Program Early Computed Tomography score (ASPECTS) applied to DWI, stroke localization (anterior or posterior), presence of an old ischemic stroke in MRI FLAIR, leucoaraiosis (Fazekas classification), Distal Hyperintense Vessel Sign (DHV) on FLAIR and presence of cerebral MicroBleeds in T2* sequence [15, 16]. IVT by tPA was administered according to the National Institute of Neurological Disorders and Stroke rt-PA Stroke Study protocol [2]. In case of admission elevated blood pressure (SBP>180 mmHg), a treatment by IV Nicardipine has been administered. The workflow's duration from stroke onset to emergency admission, radiological imaging and thrombolytic treatment was calculated. After 24 hours, the hemorrhagic complications were recorded in accordance with ECASS I classification. After 3 months, modified Rankin Scale (mRS) was computed based on clinical follow up by neurologist or by means of telephonic interview. After etiological evaluation every stroke event was classified in accordance with "Trial of Org 10172 in Acute Stroke Treatment" TOAST criteria. The main clinical outcome considered within this study is the mRS at 3 months. The modified Rankin Scale (mRs) is the most popular outcome measure and is an ordinal scale with 6 categories ranging from zero (no symptoms) to five (complete physical dependence). A sixth category can be added to signify death. The population was dichotomized into two groups: independent patients with a mRS between 0 and 2 and dependent or death patients with a mRS equal to 3 or higher. The research was conducted according to the principles of the Declaration of Helsinki.
Statistical analysis In order to define a statistically significant difference according to clinical outcome a univariate analysis of pretreatment data was computed. Chi 2 test was assessed for categorical variables and Student's t test for continuous variables. Non parametric continuous variables were represented by medians and interquartile ranges and medians and standard deviation for parametric variables. Categorical variables are presented by absolute numbers (%). p<0.05 was considered to be significant. Independent predictive variables of good outcome (mRS=2 at 3 months) were assessed by multivariate analysis by backward stepwise logistic regression. The regression model included all non-redundant variables associated to mRS=2 at 3 months with p<0.1 in the univariate analysis. Statistical analyses were conducted using STATA SE Version 10.0 software.
RESULTS
As from January 2012 to August 2016, 172 patients met the inclusion criteria. 10 patients were excluded from the study according to exclusion criteria. Baseline characteristics of studied population are presented in Table 1.
Table 1:Baseline characteristic of study population
| All patients (n=162) | |
| Demographic characteristics | |
| Age (Years) | 69.85±14.45 |
| Men | 92 (56.79%) |
| Comorbidities and risk factors | |
| Hypertension | 81 (50.00%) |
| Diabetes mellitus | 27 (16.67%) |
| Smoking (recent or current) | 32 (19.75%) |
| Atrial fibrillation | 20 (12.35%) |
| Coronary disease | 12 (7.41%) |
| History of ischemic stroke | 14 (8.64%) |
| Peripheral arterial disease | 8 (4.94%) |
| Hypercholesterolaemia | 33 (20.37%) |
| Anterior treatments | |
| Antiaggregation therapy | 56 (34.57%) |
| Statin therapy | 26 (16.05%) |
| Clinical characteristics | |
| Baseline NIHSS score | 9.56±5.09 |
| Systolic blood pressure (mmHg) | 159.39±26.05 |
| Diastolic blood pressure (mmHg) | 87.66±16.37 |
| Blood glucose (g/L) | 1.30±0.42 |
| Body temperature (ºC) | 36.91±0.58 |
| Sinus rhythm on baseline ECG | 122 (75.31%) |
| Imaging characteristics | |
| Baseline imaging by MRI | 152 (93.83%) |
| Anterior stroke | 119 (73.45%) |
| ASPECTS Score (DWI) | 9[8-9] |
| Stroke volume on DWI (cm3 | 10.70±16.87 |
| Old ischemic stroke in MRI FLAIR | 12 (7.41%) |
| Leucoaraiosis (Fazekas classification) | ) 1[1-2] |
| Distal Hyperintense Vessel Sign on FLAIR (y vs n) | 69 (42.59%) |
| Cerebral microbleeds (T2*) | 18 (11.10%) |
| Biological characteristics | |
| Haemoglobin (g/dl) | 14.47±7.07 |
| Leukocytes (G/l) | 8.50±3.49 |
| Clearance of creatinine MDRD (ml/ mn/1.73m2) | 77.78±23.40 |
| HbA1c (%) | 6.00±1.25 |
| Brain Natriuretic Peptide BNP (pg/ml) | 201.74±219.42 |
| C-Reactive Protein CRP (mg/l) | 10.91±26.24 |
| Platelets count (G/l) | 227.74±65.27 |
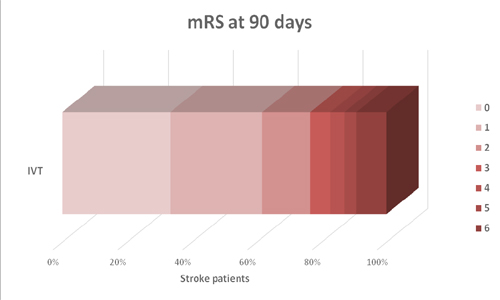
The mean age was 69.85±14.45 years and 92/162 (56.79%) patients were men. At admission, the mean NIHSS was 9.56±5.09. 50.00% of patients had hypertension history, 16.67% had diabetes mellitus, 19.75% were smoker and 12.35% had atrial fibrillation. Baseline ECG showed sinus rhythm in 122/162 (75.31%) patients. 56/162 (34.57%) patients were already treated with antiplatelet therapy. In the cohort, 152/162 (93.83%) patients underwent brain MRI at admission. The mean stroke volume in DWI was 10.70±16.87 cm3. 119/162 (73.45%) subjects had an anterior circulation stroke. The mean workflow duration from stroke onset to IVT was 165.25±54 minutes. At 24 hours, the mean NIHSS was 5.33±6.31 and 23/162 (14.20%) patients presented hemorrhagic transformation. TOAST etiological stroke subgroups were distributed as follow: Large-artery atherosclerosis 9/162 (5.56%), cardioembolism 61/162 (37.65%), small-vessel occlusion 8/162 (4.94%), stroke of other determined etiology 4/162 (2.47%), negative evaluation 67/162 (41.36%) and incomplete evaluation 13/162 (8.02%). At 3 months, 124/162 (76.54%) patients had a favorable clinical outcome (mRS=2) and 38/162 (23.46%) patients had a mRS>2 (Figure 1). At 3 months, 15/162 (9.26%) patients was died.
Figure 1: modified Rankin Scale (mRS) at 90 days.
The univariate analysis is presented in Table 2. Looking at demographic and cardiovascular risk factors, characteristics associated to functional outcome at 90 days were age (p<0.001), hypertension history (p=0.006), tobacco use (p=0.039), coronary disease (p=0.021) and peripheral artery disease (p<0.001). Within the two groups no difference was reported with regard to history of atrial fibrillation. The stroke severity measured by NIHSS was a predictive factor of poor clinical outcome (11.68±5.10 versus 8.94±4.92; p=0.005). Admission blood glucose level before IVT was higher in patient with worse clinical outcome (1.24±0.39 g/dL versus 1.48±0.48 g/ dL; p=0.009). Patients with poor clinical outcome had higher stroke volume on DWI apprehended by measure of volume (16.45±22.09 cm3versus 9.08±14.81 cm3 ; p=0.088) or ASPECTS(p=0.066). As for biological characteristics, clearance of creatinine and BNP levels were significantly higher in the dependent-death group.
Table 2: Univariate analysis of pretreatment data. (* p<0.05; +p<0.1).
| mRS = 2 at 90 days n=124 (76.54%) | mRS > 2 at 90 days n=38 (23.46%) | p | ||
| Demographic characteristics | ||||
| Age (Years) | * | 68.01±15.08 | 75.86±10.22 | <0.001 |
| Men | 69 (55.65%) | 23 (60.53%) | 0.512 | |
| Comorbidities ans risk factors | ||||
| Hypertension | * | 55 (44.35%) | 26 (68.42%) | 0.006 |
| Diabetes mellitus | + | 17 (13.71%) | 10 (26.32%) | 0.061 |
| Smoking (recent or current) | * | 29 (23.39%) | 3 (7.89%) | 0.039 |
| Atrial fibrillation | 13 (10.48%) | 7 (18.42%) | 0.178 | |
| Coronary disease | * | 6 (4.84%) | 6 (15.79%) | 0.0219 |
| History of ischemic stroke | 10 (8.06%) | 4 (10.53%) | 0.612 | |
| Peripheral arterial disease | * | 2 (1.61%) | 6 (15.79%) | <0.001 |
| Hypercholesterolaemia | 27 (21.77%) | 6 (15.79%) | 0.449 | |
| Anterior treatments | ||||
| Antiaggregation therapy | * | 34 (27.42%) | 22 (57.89%) | <0.001 |
| Statin therapy | 20 (16.13%) | 6 (15.79%) | 0.994 | |
| Clinical characteristics | ||||
| Baseline NIHSS score | * | 8.94±4.92 | 11.68±5.10 | 0.005 |
| Systolic blood pressure (mmHg) | 158.01±26.06 | 164.00±25.84 | 0.222 | |
| Diastolic blood pressure (mmHg) | 87.41±16.09 | 88.49±17.47 | 0.738 | |
| Blood glucose (g/L) | * | 1.24±0.39 | 1.48±0.48 | 0.009 |
| Body temperature (ºC) | 36.92±0.55 | 36.88±0.67 | 0.691 | |
| Sinus rhythm on baseline ECG | 95 (76.61%) | 27 (71.05%) | 0.718 | |
| Imaging characteristics | ||||
| Baseline imaging by MRI | 117 (94.35%) | 35 (92.11%) | 0.635 | |
| Anterior stroke | 93 (75.00%) | 26 (68.42%) | 0.421 | |
| ASPECTS Score (DWI) | + | 9[8-9] | 9[7-9] | 0.066 |
| Stroke volume on DWI (cm3) | + | 9.08±14.81 | 16.45±22.09 | 0.088 |
| Old ischemic stroke in MRI FLAIR | 10 (8.06%) | 2 (5.26%) | 0.581 | |
| Distal Hyperintense Vessel Sign | + | 1[1-2] | 1[1-2] | 0.072 |
| Leucoaraiosis (Fazekas classification) | 56 (45.16%) | 13 (34.21%) | 0.263 | |
| Cerebral microbleeds (T2*) | 16 (12.90%) | 2 (5.26%) | 0.199 | |
| Biological characteristics | ||||
| Haemoglobin (g/dl) | + | 14.82±7.94 | 13.34±2.40 | 0.073 |
| Leukocytes (G/l) | 8.23±2.56 | 9.36±5.45 | 0.222 | |
| Clearance of creatinine (ml/mn) | * | 81.16±23.11 | 66.94±21.80 | <0.001 |
| HbA1c (%) | 5.92±1.25 | 6.27±1.21 | 0.132 | |
| Brain Natriuretic Peptide (pg/ml) | * | 176.97±186.52 | 0.042 | |
| C-Reactive Protein CRP (mg/l) | 8.33±15.96 | 19.11±44.99 | 0.155 | |
| Platelets count (G/l) | 231.02±67.39 | 217.26±57.58 | 0.222 | |
The multivariate analysis showed that age (/10 years; OR: 1.62 95%CI[1.10-2.40]), baseline NIHSS (/5 pts; OR: 1.57 95%CI[1.06-2.32]) and admission glycemia (/0.5 g/l; OR 1.63 [1.14-6.25]) were independent predictive factors of poor clinical outcome after IVT (Table 3).
Table 3: Independent pretreatment data associated to poor clinical outcome at 3 months.
| OR [95% CI] | |
| Age (/10 years) | 1.62 [1.10-2.40] |
| NIHSS score baseline (/5pts) | 1.57 [1.06-2.32] |
| Glycemia baseline (/0.5 g/l) | 1.63 [1.14-6.25] |
DISCUSSION
IVT constitutes the mainstay of therapy in acute ischemic stroke. In recent years, most of the attentions are focused on stroke due to large vessel occlusion, and in literature few studies are available regarding the acute phase treatment of ischemic stroke without large vessel occlusion. In this study, we have analyzed the predictive factors of clinical outcome after IVT in patients having an acute ischemic stroke with distal artery occlusion. In this context, we highlight that admission glycemia, a modifiable variable, is an independent predictor of clinical outcome like non-modifiable factors such as age and baseline NIHSS.
In this cohort, mortality rate and functional outcome at 3 months after IVT were in line to previous reports. Rai et al. found a good outcome rate of 69.4% and a mortality rate of 11.7% in stroke patients without large vessel occlusion 3 months after IVT (Respectively in this study 76.54% and 9.26%) [17]. Cochrane meta-analysis of randomized clinical trials (NINDS, ATLANTIS, and ECASS) supports significantly higher dependence and mortality rates [18]. This difference probably reflects the facts that in randomized controlled trials all stroke patients with or without large artery occlusion are analyzed together. In fact, in stroke patients without large artery occlusion, IVT alone is more effective on clinical outcome [17, 19].
This study supports that age, baseline NIHSS and admission glycemia are independent predictive factors of clinical outcome after IVT (Table 3). These results are in line to previous reports studying independent predictors of functional outcome in stroke patients with or without large vessel occlusion treated by tPA [20]. Clinical severity of stroke apprehended by baseline NIHSS is a classical independent predictive factor for poor functional outcome, and our analysis confirm it (/5 pts; OR 1.57 [1.06-2.32]) [21]. IVT in elderly is largely diffused. According to our results, increasing age is associated with poorer outcome (/10 years; OR 1.62 [1.10-2.40]). Nevertheless, clinical benefits were demonstrated also in elderly stroke patients treated by tPA [22, 23]. In this study, we highlight that the admission glycemia is modifiable independent predictive factor of clinical outcome. For a stroke patient treated by tPA alone, the increase in admission glycemia of 0.5 g/L leads to increase the risk of dependence (mRS>2) by 1.63[1.14-6.25]-fold. We consider that the increased risk of dependence at 3 months after IVT was equivalent for the increase in 0.5 g/L of admission glycemia, 10 years of aging or 5 points on baseline NIHSS.
In literature, up to 50% of patients in the acute phase of ischemic stroke have hyperglycemia [5]. According to existing studies, admission hyperglycemia is considered as a common risk factor for poor outcome after ischemic stroke accelerating the molecular processes leading to cell death on ischemic penumbra [4]. Hyperglycemia facilitates development of tissue acidosis in the ischemic penumbra and is associated with worsening of mitochondrial function. In MR studies, hyperglycemia in acute ischemic stroke is shown to promote the evolution of hypoperfused tissue to infarction by means of increased brain lactate production. Concerning IVT, hyperglycemia is a strong stimulus to inhibit plasma fibrinolysis, increase levels of plasminogen activator inhibitor type 1 (PAI-1) and decrease tissuetype plasminogen activator (tPA) activity [24±27]. According to our results, admission glycemia is considered as the only modifiable deleterious factor in stroke patients without large artery occlusion, independently of a preexisting diagnosis of diabetes mellitus.
The potential benefit of a glucose-lowering treatment with aggressive insulin titration in acute stroke is not yet demonstrated, and this hypothesis is currently being testing in a large randomized clinical trial [28]. Our results confirm the interest to demonstrate acute neuroprotection by insulin therapy in stroke including stroke without large vessel occlusion.
Limitations of the studyThere are some limitations to this single-center study. We included stroke patients without large vessel occlusion but we could not differentiate stroke patients with distal vascular occlusion from those in whom no vascular occlusion could be identified.
CONCLUSIONS
In this study, we highlight predictive factors of clinical outcome in stroke patients without large artery occlusion treated by tPA. We realized that age, baseline NIHSS and admission glycemia level are independent predictive factors of clinical outcome at 3 months after acute treatment. Admission hyperglycemia was found to be a predictive factor for poor outcome independently of a diagnosis of diabetes and it was the only modifiable factor found in our cohort. Further studies are required to demonstrate the potential benefit of an aggressive glucose-lowering treatment for the management of acute hyperglycemia in acute ischemic stroke including stroke treated by tPA alone.
REFERENCES
- Favate AS and Younger DS. (2016). Epidemiology of Ischemic Stroke. Neurol Clin. 34(4): 967-980.
- National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group. (1995). Tissue plasminogen activator for acute ischemic stroke. N Engl J Med. 333(24): 1581-1587.
- Hacke W, Kaste M, Bluhmki E, Brozman M, et al. (2008). Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med. 359(13): 1317-1329.
- Luitse MJ, Biessels GJ, Rutten GE and Kappelle LJ. (2012). Diabetes, hyperglycaemia, and acute ischaemic stroke. Lancet Neurol. 11(3): 261-271.
- Alvarez-Sabin J, Molina CA, Montaner J, Arenillas JF, et al. (2003). Effects of admission hyperglycemia on stroke outcome in reperfused tissue plasminogen activator--treated patients. Stroke. 34(5): 1235-1241.
- Ribo M, Molina C, Montaner J, Rubiera M, et al. (2005). Acute hyperglycemia state is associated with lower tPAinduced recanalization rates in stroke patients. Stroke. 36(8): 1705-1709.
- Luitse MJA, van Seeters T, Horsch AD, Kool HA, et al. (2013). Admission hyperglycaemia and cerebral perfusion deficits in acute ischaemic stroke. Cerebrovasc Dis. 35(2): 163-167.
- Hou D, Liu J, Feng R, Gao Y, et al. (2017). The role of highsensitivity C-reactive protein levels in functional outcomes in patients with large-artery atherosclerosis and small-artery occlusion. Neurol Res. 39(11): 981-987.
- Quan W, Chen Z, Yang X, Li J, et al. (2017). Mean platelet volume/platelet count ratio as a predictor of 90-day outcome in large artery atherosclerosis stroke patients. Int J Neurosci. 127(11): 1019-1027.
- Liberale L, Montecucco F, Bonaventura A, Casetta I, et al. (2017). Monocyte count at onset predicts poststroke outcomes during a 90-day follow-up. Eur J Clin Invest. 47(10): 702-710.
- Ni Chroinin D, Asplund K, Asberg S, Callaly E, et al. (2013). Statin therapy and outcome after ischemic stroke: systematic review and meta-analysis of observational studies and randomized trials. Stroke. 44(2): 448-456.
- Uyttenboogaart M, Koch MW, Koopman K, Vroomen PC, et al. (2008). Lipid profile, statin use, and outcome after intravenous thrombolysis for acute ischaemic stroke. J Neurol. 255(6): 875-880.
- Charidimou A, Turc G, Oppenheim C, Yan S, et al. (2017). Microbleeds, Cerebral Hemorrhage, and Functional Outcome After Stroke Thrombolysis: Individual Patient Data Meta-Analysis. Stroke
- Fierini F, Poggesi A and Pantoni L. (2017). Leukoaraiosis as an outcome predictor in the acute and subacute phases of stroke. Expert Rev Neurother. 17(10): 963-975.
- Pexman JH, Barber PA, Hill MD, Sevick RJ, et al. (2001). Use of the Alberta Stroke Program Early CT Score (ASPECTS) for assessing CT scans in patients with acute stroke. AJNR Am J Neuroradiol. 22(8): 1534-1542.
- Fazekas F, Chawluk JB, Alavi A, Hurtig HI, et al. (1987). MR signal abnormalities at 1.5 T in Alzheimer's dementia and normal aging. AJR Am J Roentgenol. 149(2): 351-356.
- Rai A, Cline B, Williams E, Carpenter J, et al. (2015). Intravenous thrombolysis outcomes in patients presenting with large vessel acute ischemic strokes--CT angiographybased prognosis. J Neuroimaging. 25(2): 238-242.
- Wardlaw JM, Murray V, Berge E and del Zoppo GJ. (2009). Thrombolysis for acute ischaemic stroke. Cochrane Database Syst Rev. (7): CD000213.
- Padma S and Majaz M. (2010). Intra-arterial versus intravenous thrombolysis within and after the first 3 hours of stroke onset. Arch Med Sci. 6(3): 303-315.
- Wahlgren N, Ahmed N, Eriksson N, Aichner F, et al. (2008). Multivariable analysis of outcome predictors and adjustment of main outcome results to baseline data profile in randomized controlled trials: Safe Implementation of Thrombolysis in Stroke-MOnitoring STudy (SITS-MOST). Stroke. 39(12): 3316-3322.
- Saposnik G, Young B, Silver B, Di Legge S, et al. (2004). Lack of improvement in patients with acute stroke after treatment with thrombolytic therapy: predictors and association with outcome. JAMA. 292(15): 1839-1844.
- Emberson J, Lees KR, Lyden P, Blackwell L, et al. (2014). Effect of treatment delay, age, and stroke severity on the effects of intravenous thrombolysis with alteplase for acute ischaemic stroke: a meta-analysis of individual patient data from randomised trials. Lancet. 384(9958): 1929-1935.
- Mishra NK, Ahmed N, Andersen G, Egido JA, et al. (2010). Thrombolysis in very elderly people: controlled comparison of SITS International Stroke Thrombolysis Registry and Virtual International Stroke Trials Archive. BMJ. 341: c6046.
- Nordt TK, Klassen KJ, Schneider DJ and Sobel BE. (1993). Augmentation of synthesis of plasminogen activator inhibitor type-1 in arterial endothelial cells by glucose and its implications for local fibrinolysis. Arterioscler Thromb. 13(12):1822-1828.
- Auwerx J, Bouillon R, Collen D and Geboers J. (1988). Tissue-type plasminogen activator antigen and plasminogen activator inhibitor in diabetes mellitus. Arteriosclerosis. 8(1): 68-72
- Juhan-Vague I, Roul C, Alessi MC, Ardissone JP, et al. (1989). Increased plasminogen activator inhibitor activity in non insulin dependent diabetic patients--relationship with plasma insulin. Thromb Haemost. 61(3): 370-373.
- Pandolfi A, Giaccari A, Cilli C, Alberta MM, et al. (2001). Acute hyperglycemia and acute hyperinsulinemia decrease plasma fibrinolytic activity and increase plasminogen activator inhibitor type 1 in the rat. Acta Diabetol. 38(2): 71-76
- Bruno A, Durkalski VL, Hall CE, Juneja R, et al. (2014). The Stroke Hyperglycemia Insulin Network Effort (SHINE) trial protocol: a randomized, blinded, efficacy trial of standard vs. intensive hyperglycemia management in acute stroke. Int J Stroke. 9(2): 246-251.