Information Links
Related Conferences
Previous Issues Volume 7, Issue 2 - 2023
Medical Responsibility Through a Dental Case Study
Marouane El Ouni, Nabiha Douki*,Amira Kikly, Neila Zokkar ,Sonia Zouiten
Faculty of Dental Medicine, University of Monastir, Tunisia
*Corresponding Author: Nabiha Douki, Faculty of Dental Medicine, University of Monastir, Tunisia; Email: [email protected]
Received Date: August 3, 2023
Publication Date: August 29, 2023
Citation: El Ouni M, et al. (2023). Medical Responsibility Through a Dental Case Study. Mathews J Dentistry. 7(2):37.
Copyright: El Ouni M, et al. © (2023)
ABSTRACT
Faced with a judicial system that suffers from a lack of laws and jurisprudence governing the liability of doctors in general and dentists in particular, and in the absence of a medical liability law to protect them, dentists are faced with a patient who is aware of his rights, believes in the omnipotence of science, is becoming increasingly demanding of the medical profession, and has difficulty accepting medical accidents.
The aim of this paper is to discuss, through the study of an accidental injection of sodium hypochlorite case report, the dentist's obligations towards his patient and his responsibility in the event of medical malpractice.
This is no more than an attempt to understand the judicial spiral, so that we can be informed and aware of the judicial system, whose language may seem too complex for a dentist.
Keywords: Medical Liability Law, Dental Responsability, Judicial System
INTRODUCTION
The proliferation of dental specialties, scientific progress and the advent of new exploration and treatment techniques have all contributed to the growing effectiveness of dental practice. On the other hand, changes in society (changing attitudes, desacralization of medicine, etc.), media coverage of dental successes and public information on medical liability cases are becoming increasingly important [1]. All over the world, the number of complaints against doctors has risen steadily in recent years [2]. Faced with a judicial system that suffers from a lack of laws and jurisprudence governing the liability of doctors in general and dentists in particular, and in the absence of a medical liability law to protect them, dentists are faced with a patient who is aware of his rights, believes in the omnipotence of science, is becoming increasingly demanding of the medical profession, and has difficulty accepting medical accidents [3].
The aim of this paper is to discuss, through the study of a clinical case, the dentist's obligations towards his patient and his responsibility in the event of medical malpractice.
CLINICAL OBSERVATIONS
Patient 'S.C', 29 years old, unbalanced diabetic, referred by her orthodontist to our department, for care of necrotic 34. The patient was managed by an intern (X1) working in the department.
During endodontic treatment, the patient experienced immediate, intense pain, reminiscent of a burning sensation. A few seconds later, a profuse intra-root canal haemorrhage appeared. This led to the diagnosis of accidental injection of sodium hypochlorite beyond the apex of the 34.
The management team (resident and university hospital assistant) intervened. Emergency procedures were performed in the session, with vacuum aspiration of blood from the canal, followed by irrigation with saline, and the tooth left open. The patient was kept under observation on the ward. 30 minutes later, a swelling of the left lower genital region appeared.
Team Communication with the Patient
The team tried to calm and reassure the patient. The information was delivered in simple terms, and covered:
- The nature of the accident: ''This is a rare accident caused by the passage beyond the apex of the tooth, of the endodontic irrigation solution (which is bleach-based and used to disinfect the canal); this solution, as long as it remains confined within the canal, is not nocive. But if it is expelled beyond the apex, this reaction will occur, since it is toxic to living tissue.
- The most likely cause of the accident: ''This accident may occur if the irrigation needle becomes blocked in the canal.''
- Probable complications of the accident: ''the swelling may persist for several days, with a possible change in the condition and color of the tumefaction. As for the pain, although violent, it is of short duration and will dissipate in a few minutes. Don't hesitate to contact us by phone or consult.
Development of the patient-practitioner conflict
An analysis of the patient's personality reveals a behavioral pattern similar to the "analyzing" social style. She would like a detailed explanation of the circumstances surrounding the accident, as well as the likely complications for her state of health. She addressed the care team with the following questions: emergency service if things get worse (breathing difficulties ).
Question 1 (according to him): ''If I understand correctly, you used a non-medical commercial bleach-based solution for disinfection? ''.
-Answer (from the supervisory team): ''Yes, but you should know that its effectiveness has been scientifically proven, and that the problem lies not in the irrigation solution itself, but rather in the act of forced injection, which can generate this type of accident''.
Question 2: ''So Doctor X1 was at fault, since he forced the injection? The patient decided to lodge a complaint against doctor X1.
Course of Action
- Questioning and thorough clinical examination revealed the following: The patient had received orthodontic treatment at the age of 15, and was currently undergoing a second orthodontic treatment, since the results of the first were unsatisfactory. The tooth in question is linguoversion, with a palpable arch in the vestibule opposite the root.
- A CBCT radiological examination was requested following these findings.
Recommendations
-Application of an ice pack for 24 hours to control swelling.
-Application of warm, moist compresses every 15 minutes for 24 hours the following day, to promote revascularization.
-Mouthwash with saline solution for 1 week.
Prescription
Antibiotic therapy for 7 days to prevent extension of the primary infection or occurrence of a secondary superinfection, No corticosteroid prescription (given his unbalanced diabetes).
Paracetamol-based analgesic combined with codeine for pain control.
- Daily telephone contact with the patient and weekly consultation until resolution of symptoms.
Follow-up Appointments
- Day 1 Favourable evolution with well-limited swelling. The patient is calmer and reassured.
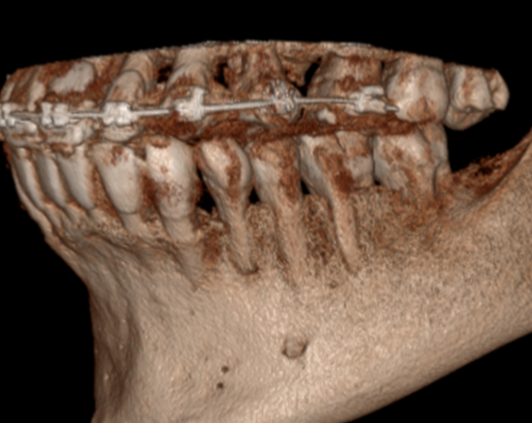
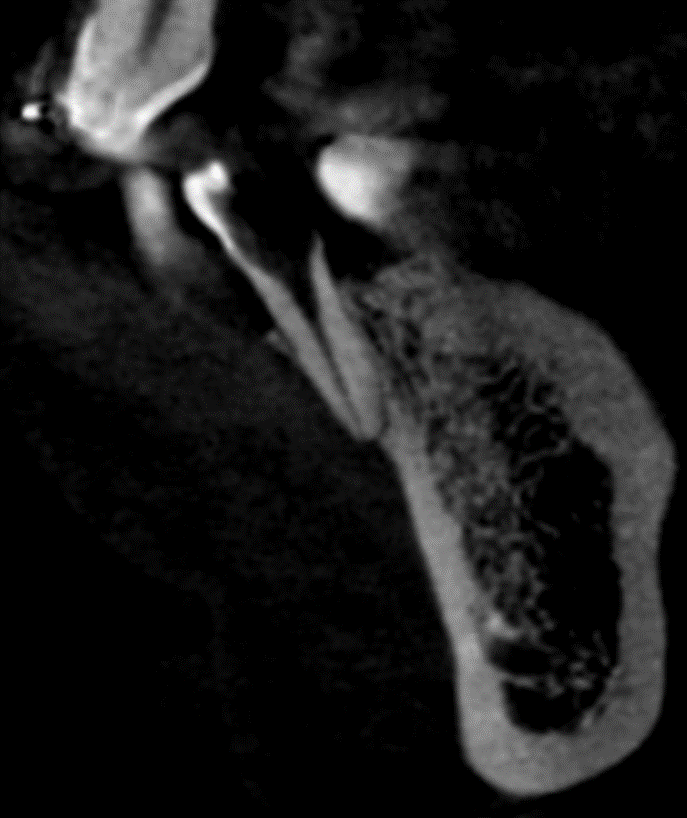
CBCT examination shows bone dehiscence opposite 34, 35 and the vestibular root of 36 (figure 1). A cross-section of 34 shows that the apical foramen is in direct contact with the overlying gingival mucosa (figure 2).
Figure 1: CBCT 3D viewFigure 2: Sagittal section of the 34.
Day 15: Favourable outcome with complete regression of swelling
CASE DISCUSSION
A reading of the facts reported in this clinical case highlights a number of medical errors committed by practitioner X1 and the supervisory team, which may engage their medical responsibility. But first of all, what is medical malpractice and what is medical liability?
Medical malpractice is defined as any act performed by a dentist in a patient's oral cavity which results in abnormal damage in relation to the foreseeable evolution of the patient's state of health [3], not to be confused with a therapeutic hazard, which is an event that could not be foreseen, and against which nothing could be done. It is not a fault, nor an error, nor a failure of care, but an uncontrollable risk independent of any failure on the part of the practitioner [4].
As for the notion of medical responsibility, it is defined as the moral or legal obligation incumbent on all physicians to answer for their actions before themselves and before society, and to assume the consequences [5].
According to the literature, the anatomical position of teeth in relation to the alveolar bone is an important factor in the occurrence of this type of accident, particularly when the root apex is surrounded by thin bone or only soft tissue. In such cases, extrusion of a small volume of irrigant can lead to symptoms with a risk of propagation [7-9], as in our patient's case.
The question that arises here is whether this favourable factor in the sodium hypochlorite injection accident can spare the practitioner medical liability.
In our case, even with the anatomical defect present (bone dehiscence), the accident could be avoided in the absence of a forced injection of sodium hypochlorite. In other words, it was a technical error that caused the accident: blocking the endodontic irrigation needle and/or over-instrumenting the apical foramen, which in turn can be explained by working on a short-rooted tooth without a preoperative X-ray; actions that would not have been taken by a prudent, conscientious practitioner. The anatomical defect is thus merely an additional risk factor.
Generally speaking, to hold a dental practitioner liable in the event of fault, three elements are essential: proof of fault on his or her part, of damage suffered by the patient, and of a causal link between the two [3]. This is indeed the case with the accidental injection of sodium hypochlorite. In this case, the healthcare professional has failed in his or her obligation to provide care in accordance with the rules of the art. This brings us back to a discussion of the practitioner's obligations, the breach of which may give rise to liability.
In France, this was formalized in 1932 by the Mercier ruling, according to which "The obligation of care arising from the medical contract and incumbent on the doctor is an obligation of means; the doctor cannot undertake to cure, but only to give care that is not arbitrary but conscientious, attentive and in accordance with the acquired data of science".[3] Thus, the dental practitioner is not under an obligation to cure his patient, but must use all the means at his disposal to achieve this, and thus has an obligation of means. He must provide attentive care in line with the latest scientific findings, both at the stage of diagnosis and therapeutic decision, and in the performance of his acts of care. This is not the case for doctor 'X1'. On the one hand, he started the endodontic treatment without having recourse to the preoperative retroalveolar radiograph, i.e. without having any idea of the working length, and moreover, on the CBCT, we realize that the tooth is quite short (16 mm).
On the other hand, he worked without a dam, and without resorting to pre-endodontic coronal reconstitution (major decay of the distal wall of the tooth concerned). In France, since 2008, the Haute Autorité de Santé has defined a dam as an obligation of means during endodontic treatment.
Another form of obligation of means is the obligation of safety of care, which concerns the equipment and method used to perform the act of endodontic irrigation. This obligation was not respected in our case, since practitioner 'X1' used a 21 gauge (0.73 mm) bevelled hypodermic needle, which is not dedicated to the act of endodontic irrigation. As for the management of the accident and the announcement of the damage, a number of errors were also noted.
Fear and panic on the part of both the patient and her doctor led to the supervisory team stepping in to manage the situation, while at the same time removing the doctor (X1) from the scene of the accident. This can break down the practitioner-patient duality and be detrimental to the relationship of trust between these two partners. This attitude can only aggravate the patient's doubt and confusion. In fact, it is the professional who is responsible for the care delivered to the patient (in our case, Doctor 'X1') who is in the best position to lead (possibly accompanied by a member of his or her team) the announcement of damage associated with care. It should be noted that, when a patient takes legal action against his or her doctor, it is often the doctor's behavior that prompts him or her to lodge a complaint. Patients do not accept a lack of consideration on the part of their doctor, but they understand that a mistake may have been made, and that the fault is human. So, in the event of a medical accident, total transparency and compassion are essential. We must provide the patient with exhaustive information, and try to explain why he or she has been the victim of an injury
DISCUSSION & CONCLUSION
Today, medical liability cases are making a lot of noise, and would tend to alarm many dentists who fear being implicated in the context of their activity. As a result, patients who are victims of medical accidents are more likely than in the past to seek to identify the person responsible, in order to obtain compensation for the damage caused to them [10]. In Tunisia, and in the absence of legal texts defining the doctor's obligations and responsibilities, some might claim that the vacuum in this area can only be in the caregiver's favor, protecting him or her from medico-legal proceedings, whereas in reality this only constitutes a great danger for both doctor and patient [3]. Tunisian law therefore needs to evolve towards the introduction of a medical liability law in order to curb the judicialization of the doctor-patient relationship and limit the number of lawsuits and unfounded claims[2].
The aim of this work was to inform dentists about the particularities of their obligations. This is no more than an attempt to understand the judicial spiral, so that we can be informed and aware of the judicial system, whose language may seem too complex for a dentist.
REFERENCES
- Helmlinger L, Martin D. (2004). La judiciarisation de la médecine, mythe et réalité. Les Tribunes de la santé. 5(4):39-46.
- Zribi M, Bardaa S, Feki N, Ben Amar W, Hammami Z, Maatoug S. (2017). Etude de la responsabilité médicale dans la région de Sfax et du sud Tunisien. 25:36-39.
- Mlika M, Ben Khelil M, Hamdoun M, Mezni F. (2017). Legal responsibility of the pathologist in Tunisia.Tunis Med. 95(6):388-392.
- Thouvenin D. (2006). Responsabilité médicale: de quoi s'agit-il exactement? Commentaire. Sciences sociales et santé. 24(2):35-42.
- Thibierge M, Fournier L, Cabanis EA. (1999). Principles of medical liability and practice in medical imaging. J Radiol. 80(7):701-707.
- Howell S, Perry MM, Patel N. (2016). Protocols for treating patients with end-stage renal disease: a survey of AEGD/GPR dental residencies. Spec Care Dentist. 36(6):325-327.
- Kleier DJ, Averbach RE, Mehdipour O. (2008). The sodium hypochlorite accident: experience of diplomates of the American Board of Endodontics. J Endod. 34(11):1346-1350.
- de Sermeño RF, da Silva LA, Herrera H, Herrera H, Silva RA, Leonardo MR. (2009). Tissue damage after sodium hypochlorite extrusion during root canal treatment. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 108(1):e46-e49.
- Farook SA, Shah V, Lenouvel D, Sheikh O, Sadiq Z, Cascarini L, et al. (2014). Guidelines for management of sodium hypochlorite extrusion injuries. Br Dent J. 217(12):679-684.
- Sriha Belguith A, Elmhamdi S, Bouanene I, Ben Saad M, Ben Salah A, Harizi C, et al. (2015). Quality of the medical record notification in primary health care. Tunis Med. 93(3): 148-152.