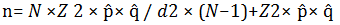Information Links
Related Conferences
Previous Issues Volume 7, Issue 3 - 2023
High Reproductive Risk and Contraception
Alexander Porter Magaña1, Suria Denisse Soriano León1, Víctor Manuel Vargas Hernández2,*
1Regional General Hospital “Licenciado Ignacio García Téllez Mexican Institute of Social Security, Mexico
2Mexican Academy of Surgery, National Academy of Medicine of Mexico, Mexico
*Corresponding author: Dr. Víctor Manuel Vargas Hernández, Obstetrics and Gynaecology, Department of Director of Women’s Health Clinic, Insurgentes Sur 605-1403, Nápoles 03810, Mexico, Tel: (52)5552 179782, E-mail: [email protected].
Received Date: November 09, 2023
Published Date: November 28, 2023
Citation: Magaña AP, et al. (2023). High Reproductive Risk and Contraception. Mathews J Gynecol Obstet. 7(3):30.
Copyrights: Magaña AP, et al. © (2023).
ABSTRACT
Background: Patients with high reproductive risk have important risk factors for the development of complications, including maternal death. Rejection of a method is influenced by various factors, including: biological, cultural and social factors. Objective: Identify the main sociocultural and demographic factors associated with not choosing a contraceptive method in women at high reproductive risk. Material and methods: it is an observational, cross-sectional, analytical and prospective study with non-probabilistic sampling carried out in pregnant women with high reproductive risk who were offered contraception through a questionnaire. Results: 75 patients with high reproductive risk (20%) were included, with an average age of 27 years, occupation as a housewife (48%), living in an urban area (66.7%), complete primary schooling (22.67%), Catholic religion (72%), married (57.3%), middle class (72%); alcoholism in 2 patients (2.67%) and 2 other drugs (2.67%); 68% rejected contraception; for personal reasons (76.4%). A significant relationship was found with the Jehovah's Witness religion (p = 0.018). Conclusions: rejection of contraception is influenced by personal history and religion, with implications for reproductive health
Keywords: Contraception, Rejection, Religion, Schooling.
BACKGROUND
The History of human contraception (CA) has the purpose of achieving sexual pleasure, avoiding fertilization [1]. In the Papyrus of Petri, from 1850 BC, contraceptive recipes already appeared; crocodile excrement, pessary [2], coitus interruptus, condom, spermicides with vinegar. The intrauterine device emerged in 1863, in 1934 progesterone was isolated and in 1956 the pill was discovered [2]. Surgical techniques began at the end of the 19th century, with female sterilization and later vasectomy, under informed consent [3].
AC constitutes the fundamental basis of reproductive health (RH); the benefits include the reduction of poverty, maternal and perinatal mortality, with a better quality of life, greater opportunities for education, work, and an equal society. In Mexico with more than 35 years in the promotion and improvement of CA, with changes in the legal and public health framework; In 1973, it was the second in the world and first in Latin America to establish in its Constitution the right to decide in a free, responsible and informed manner about the number and spacing of their children (Article 4 of the political constitution of the United Mexican States). In 1974, population growth was regulated within the General Population Law, with a National Family Planning Plan 1977-1979; resulted in the reduction of the global fertility rate from 7.26 children per woman in 1962 to 3.43 in 1990, and to 2.01 in 2012 [4]; however, in the last 12 years there is a slowdown. Contraceptive coverage for women increased from 15.0% in 1973 to 74.5% in 2003 to decrease to 70.9% in 2006; reporting 72.5% in 2009 [4]; According to the National Demographic Dynamics Survey (ENADID) 2018, the median age at the beginning of sexual life is 17.5 years, of which 59.4% did not use any contraceptive method. Among women between 15 and 49 years old, they did not use a contraceptive method in their first sexual relationship, due to not having planned the sexual relationship (28.4%), followed by the desire for pregnancy (24.3%), lack of knowledge of the methods (24.1%), or hoping not to get pregnant (11%) and for reasons (10.9%) [5].
Globally, it is estimated that 214 million women of reproductive age have unmet needs for contraception in emerging countries and 67 million unplanned pregnancies, 36 million induced abortions and 76 thousand maternal deaths could be avoided each year [6).
The reasons why women and their partners do not use contraceptive methods are multiple. In sub-Saharan Africa, for example, low use of the contraceptive method, fear of adverse effects, lack of partner approval due to social and cultural beliefs that include traditional abstinence practices and waiting for the return of menstruation to initiate contraceptive use [7], they are misconceptions and monitoring, improves the continuity of contraceptives.
The World Health Organization established the medical eligibility criteria for the use of contraceptives according to the health conditions of each patient and considering special situations. The use of modern contraceptives is associated with sociodemographic, sociocultural and economic factors [8]. The evaluation of reproductive risk, a method that allows measuring care needs, helps determine health priorities, it is about having sufficient coverage and information for each woman with high reproductive risk, to reduce perinatal maternal morbidity and mortality and complications due to risks. Reproductive, which is defined as the probability that a woman has of suffering damage during the reproduction process, which affects the mother, the fetus or the newborn, with an increased risk of maternal morbidity and death [9]; the identification of pathologies or high reproductive risk, such as chronic non-communicable diseases, which are rare in reproductive age? There are many factors that are related to definitive sterilization; Married women are the ones who most opt for this method, the couple, for emotional and economic support; Unlike single women, the sexual behavior of the couple influences; Women who reject this definitive method, those who have been mentioned have fears of side effects, breastfeeding, the transition to menopause [4], other reasons include: illness of the partner (which limits the frequency of sexual relations), infrequent or non-existent sexual relations, a couple who travels for long periods of time, interrupted intercourse or because their partner does not agree, formal education, place of residence and socioeconomic level, influence the choice of a contraceptive method [4]. Society and culture influence family size, family pressures to have children, customs and religious beliefs [10] where machismo society predominates [11]; Maternal mortality rates (MMR) between countries, and even between different regions of the same country, show their intrinsic link with poverty and marginalization [12].
Maternal death worldwide is unacceptably high, every day around 830 women die worldwide from complications related to pregnancy, childbirth or the postpartum period; All of these deaths occur in emerging countries and the majority are avoidable [13]. In Mexico it was reported in 2017; 20.8 deaths per 100 thousand estimated births; mainly those between 45 and 49 years old [14], and from 2013 to 2015 in Yucatán it was 43.5; various preventive actions to reduce maternal mortality; a) promote prenatal care and b) prevent pregnancies in patients who have risk factors. Contraception has the potential to save millions of women's and infants' lives, determining the health and economic well-being of millions of families.
MATERIAL AND METHODS
An observational, analytical, cross-sectional, prospective study was carried out; at the Dr. Ignacio García Tellez Regional General Hospital (T-1) Mexican Social Security Institute (IMSS) of Mérida Yucatán; in the gynecology and obstetrics outpatient clinic during the period from June 2022 to June 2023; in pregnant women at high reproductive risk. In 5938 of pregnant patients (N); a confidence level of 95% (Z=1.96), a proportion of 50% (p̂= 0.5), therefore, a proportion complement of 0.5 (q̂ =1- p̂) and an error of 5% (d=0.05) for finite population.
n= sample size
N= total population for one year.
Z= critical Z value, calculated from the area under the curve tables. Confidence level.
p̂= approximate proportion of the phenomenon under study in the reference population
q̂= proportion of the reference population that does not present the phenomenon under study
(1 p).
d= absolute precision level.
Resulting in a sample of 360 patients, the sampling was non-probabilistic. To determine patients with “reproductive risk” the Manual of family planning procedures in the units of the Mexican Social Security Institute, code 2230-003-001, Table 1 was used.
Table 1. Manual of family planning procedures in the units of the Mexican Social Security Institute key 2230-003-001, format MF-6/2000. Fill out this form using the data obtained by direct questioning of the patient
NAME:
PROCEEDINGS:
Age _______Years
Occupation ☐ Housewife ☐ Student
☐ Farm employee ☐ Merchant
☐ Secretarial activities ☐ Technical
☐ Others
Place of Residence ☐ Urban ☐ Suburban ☐ Rural
Education ☐ Illiterate ☐ Incomplete primary school
☐ Complete primary ☐ Incomplete secondary
☐ Complete secondary school ☐ Incomplete Baccalaureate
☐ Completed high school ☐ Bachelor's degree
Religion ☐ Catholic ☐ Christian
☐ Jehovah's Witness ☐ Mormon
☐ Adventist ☐ Other religion
☐ None
Marital status ☐ Single ☐ Married
☐ Divorced ☐ Free union
☐ Widowed ☐ Separated
Socioeconomic level ☐ Marginal ☐ Low
☐ Medium ☐ High
Alcoholism ☐Yes ☐No
Drug use ☐Yes ☐No
Family planning method
Definitive
☐Yes ☐No
Reason for rejection of method
Definitive family planning
☐ Personal cause ☐ Religious cause
☐ Economic cause ☐ Cause of the couple
☐ Social cause ☐ Family cause
The protocol was submitted to review by the hospital's research and ethics committees. The reproductive risk survey was applied to 360 patients from the obstetrics outpatient clinic who met the selection criteria, studying those who had a reproductive risk greater than or equal to 4 points, which was a total of 75 patients. A second questionnaire was administered to the 75 patients with high reproductive risk, in which sociodemographic and family planning data were obtained.
RESULTS
A total of 360 patients who met the previously described selection criteria were interviewed. There were 75 patients included in the study as they presented a reproductive risk greater than 4 and who agreed to participate in the study, which formed the present investigation. The average age of the sample was 27 years ± 5.3. The most frequent occupation was housewife with 38 patients (48%). Regarding origin, the patients were mostly of urban origin, 50 patients (66.7%). The most frequent education was completed primary school with a frequency of 17 patients (22.67%) followed by bachelor's degree and high school. The most frequently found religion was Catholic in 54 patients (72%) followed by Christian in 11 occasions (15%). The most frequent marital status was married in 43 cases (57.3%) followed by common law in 17 cases (22.67%) as shown in Table 2.
Table 2. Frequency of reasons for not accepting contraception
|
Reasons |
N |
(%) |
|
Staff |
39 |
(76.47%) |
|
Religious |
3 |
(5.88%) |
|
Economic |
0 |
(0%) |
|
Couple |
7 |
(13.73%) |
|
Social |
0 |
|
|
Family |
2 |
(3.92%) |
A descriptive analysis was carried out on the patients who did not accept contraception. The average age was 27.15 years ± 5.29 years. The most frequent occupation was housewife in 25 patients (49%). The most frequent origin was an urban area in 30 patients (58.82%) represented in Table 3. The most frequent education was complete primary school in 14 patients (27.45%), the same as the education of the rest of the patients.
Table 3. Patients who did not accept contraception
|
Origin |
N |
(%) |
|
Urban |
30 |
(58.82%) |
|
Suburban |
15 |
(24.41%) |
|
Rural |
6 |
(11.76%) |
Regarding the most frequent religion of the patients who did not accept contraception, it was the Catholic religion. The most frequently found marital status was married in 62%, while the socioeconomic level that we found most was medium level in 70%, as reported in Table 4. Analytical statistics were performed with logistic regression, finding a significant statistical association only in the religion variables as shown in Table 5.
Table 4. Socioeconomic level of patients who did not accept contraception
|
Marital status |
N |
(%) |
|
Marginalization |
1 |
(1.96%) |
|
Under |
14 |
(27.45%) |
|
Medium |
36 |
(70.59%) |
|
High |
0 |
Table 5. Frequency of reasons for not accepting contraception
|
Variables |
Error |
Error Standard |
Error Significant |
|
Age |
0.193 |
0.122 |
0.114 |
|
Occupation |
0.825 |
||
|
Origin |
0.104 |
||
|
Education |
0.561 |
||
|
Religion |
0.107 |
||
|
Jehovah's Witness |
11.56 |
4.87 |
0.017 |
|
Marital status |
0.709 |
||
|
Socioeconomic level |
0.998 |
||
|
Alcoholism |
1 |
||
|
Drug consumption |
0.603 |
DISCUSSION
Of the total of 360 patients interviewed, a high obstetric risk rate was obtained for 75 patients, who were included in the study. Only 24 patients accepted the planning method (32%), and in the reasons of the patients who did not accept the family planning method, personal reasons prevailed, stating that they wanted to have even more children. This represents a 68% rate of refusal of definitive contraception in high obstetric risk patients. The average age of the sample was 27 years ± 5.3, without finding a statistically significant relationship with the refusal of contraception; similar data in different countries [16,17] did not find an association with age. The most frequent occupation was housewife with 38 patients (48%) also without a significant relationship, similar to others [18]. The origin of the patients was mostly urban areas with 66.7% similar to others [19] who reported 69.5 and 30.5% in rural areas, without finding a significant association with non-acceptance of contraception at the first level of care.
The most frequently found schooling was complete primary school, different from others [20] where they had completed high school, and completed secondary school [21], this can contrast due to regional differences and the average age of their samples was greater than the Our average age is 30 to 39 years old. These studies reported a significant association with education and refusal to use contraception.
The most frequently found religion was Catholic in 54 patients (72%), similar to others [22]. In our study, a significant association with religion was found, a fact that was not found in previous studies in Mexico [16,19,21,22], although the significant association was presented with the Jehovah's Witness religion (p= 0.017), a religion that was not studied in Mexico, unlike others [23] who found a significant association (0.03) with religion on the refusal of contraception [24] where religion was a significant factor in association with non-use of the implant (p=0.005), in both studies the frequency of patients who were Jehovah's Witnesses was similar to ours (3 patients and 7 patients respectively).
In most Latin American countries, religion has an important effect on the availability of contraception, health policies, and health service providers may not offer this type of service for fear of confronting religious institutions.
In general, the most frequently practiced religions in Mexico consider contraception as part of home life and as an important factor in the stability of marriage. The majority agrees in affirming that contraception constitutes an obligation of responsible parenthood, as long as the designs of the church are respected, such is the case of the Catholic Church and Jehovah's Witnesses, who consider the rhythm method as the only acceptable way. In rural areas, religion plays a significant role in relation to the low prevalence of contraceptive practice, especially when there is low education, in which it is considered that one should not talk about issues related to sexuality or contraception [25].
The most frequent marital status was married in 43 cases (57.3%), others did not find a similar association in 41 patients being married, the most frequent marital status being. Marital status is a condition that influences the use or non-use of methods, and it is reported that married women tend to be the most accepting, unlike single women who, due to their condition, would be socially singled out; however, this had no impact in the sample studied.
Regarding the socioeconomic level of the patients, the most frequently found was middle class in 54 patients (72%), in both cases without a statistically significant relationship, similar to others [26] who found the low middle socioeconomic level as the most frequent in its population of first-level care female patients who did not accept contraceptives, without finding a relationship with statistical significance (OR 0.33, p 0.18, CI 0.06-1.81). with similar results to others in that the majority of their respondents in Zacatecas did not consume alcohol and/or drugs (OR 0.58, p 1.16, CI 0.22-1.55) comparable to the 2 patients (2.67%), and 2 patients ( 2.67%) reported drug use in our study without finding a significant association in any of these variables.
CONCLUSIONS
The frequency of high reproductive risk in pregnant women, the sociodemographic characteristics of patients with refusal of contraception in patients with high reproductive risk, a significant relationship was only found with Jehovah's Witness religion.
JOB LIMITATIONS
One of the main limitations of the present work is that it is a non-randomized study, which could obtain more precise information with randomized controlled clinical studies, in addition to being a study limited to a single medical center, in this case a second-class hospital. Level, more representative results can be obtained from multicenter studies at the regional or even national level.
STRENGTHS
The present study has the strength of being prospective, with broad sampling, obtaining data from direct interviews; strength is having considered various variables probably related to the refusal to use the family planning method, in addition to carrying out a multivariate analysis with regression, logistics, avoiding confounding variables.
RECOMMENDATIONS
It is recommended to carry out new studies, this time considering intervention type studies, seeking to reduce the rate of refusal to use definitive contraception, in addition to raising the possibility of carrying out long-term follow-up cohort studies, investigating the degree of obstetric complications, as in Kaplan Mayer curve studies.
Derived from the results, both the obstetric risk rate and the rate of refusal to use contraception are worrying, so efforts must be increased to raise awareness among patients at reproductive risk of the high risks of complications if they try, new pregnancies. Likewise, it would be important to work with the population of religions such as Jehovah's Witnesses, which proved to be a variable associated with the refusal of contraception.
CONFLICT OF INTEREST
The authors have no conflict of interest.
REFERENCES
- Núñez JA. (2018). Historia evolutiva de la anticoncepción. Real Academia Nacional de Medicina de España. 135(1):56-59.
- Díaz Alonso G. (1995). Historia de la anticoncepción. Revista Cubana de Medicina General Integral. 11(2):192-194.
- Salud MDE, Social B. Manual de Planificación. 2016.
- Allen-Leigh B, Villalobos-Hernández A, Hernández-Serrato MI, Suárez L, De la Vara E, De Castro F, et al. (2013). Inicio de vida sexual, uso de anticonceptivos y planificación familiar en mujeres adolescentes y adultas en México. Salud Publica Mex. 55(Supl 2):S235-S240.
- INEGI. Encuesta Nacional de la Dinámica Demográfica (ENADID) 2018. México.
- Cavallaro FL, Benova L, Owolabi OO, Ali M. (2020). A systematic review of the effectiveness of counselling strategies for modern contraceptive methods: what works and what doesn’t? BMJ Sex Reprod Health. 46(4):254-269.
- Barrera Coello L, Olvera Rodríguez V, Castelo-Branco Flores C, Cancelo Hidalgo M de J. (2019). Causas de desapego a los métodos anticonceptivos. Ginecología y obstetricia de México. 87(Suppl 1):S128-S135.
- Capella D, Schilling A, Villaroel C. (2017). Criterios Médicos de elegibilidad para el uso de anticonceptivos de la OMS. Rev Chil Obstet Ginecol. 82(2):212-218.
- Rodriguez ML. (2010). Enfoque de Riesgo en el Proceso de Reproduccion La. Salud Reproductiva y Planificación Familiar Universidad Los Angeles de Chimbote. p. 1-5.
- Suárez Gutiérrez JJ, Rangel Villasenor O. (2014). Índice de aceptación de Método de Planificación Familiar definitivo en el Hospital Regional ISSEMYM Tlalnepantla, del 1 de enero 2013 al 31 de junio de 2013.
- Ráez LE. (2019). La esterilización voluntaria como medio para planificar la familia. Aciprensa. Available from: https://www.aciprensa.com/recursos/la-esterilizacion-voluntaria-como-mediopara-planificar-la-familia-249.
- del Carmen Elu M, Pruneda ES. (2004). Mortalidad materna: una tragedia evitable. Perinatol Reprod Hum. 18(1):44-52.
- ONU SF. Objetivos de desarrollo sostenible. 17 objetivos para transformar nuestro mundo. Available from: https://www.un.org/es/climatechange/17-goals-to-transform-our-world.
- Epidemiologia DG de. Informe defunciones maternas. 2020.
- Morales-Andrade E, Ayala-Hernádez MI, Morales-Valerdi HF, AstorgaCastañeda M, Castro-Herrera GA. (2018). Epidemiología de la muerte materna en México y el cumplimiento del Objetivo 5 del Desarrollo del Milenio, hacia los objetivos de desarrollo sostenible. Revista de especialidades médicoquirúrgicas. 23(2):61-86.
- Mejia Carlos ML, Pineda Diaz RM. (2018). Factores asociados al no uso de métodos anticonceptivos durante el puerperio, hospital Víctor Ramos Guardia-Huaraz, 2017. Available from: https://repositorio.unasam.edu.pe/bitstream/handle/UNASAM/2717/T033_46629403_T%20.pdf?sequence=1&isAllowed=y.
- Morante Veliz GV, Vásquez Álvarez AC. (2020). Factores que influyen en la elección de un método anticonceptivo en mujeres en edad fértil de 14 a 30 años de edad que acuden a la consulta externa del centro de salud Antonio Sotomayor del cantón Vinces, los ríos, enero-junio 2019. Babahoyo: UTB-FCS.
- Carrillo Rivas KC, Jarquín Trujillo HM. (2019). Factores sociales y culturales del uso de métodos anticonceptivos en adolescentes, atendidas en el programa de planificación familiar Centro de salud El Calvario, Chinandega, II semestre 2019.
- de la Vega Apanco E. (2017). Causas de no aceptación de métodos de planifiación familiar en mujeres en edad reproductiva en una clínica en primer nivel de atención. Universidad Nacional Autónoma de México.
- Velazquez Mejia B, Reyes Jimenez O, Marquez Gonzalez J. (2021). Causas de aceptación y no aceptación de un método de planifiación familiar en el puerperio de pacientes de la UMF 92. Universidad Nacional Autónoma de México.
- Reyes Aguilar A, Ceja Aladro A. (2019). Causas de no aceptación de método de planifiación familiar en púerperas de HGZ MF No1 de Pachuca Hidalgo. Universidad Nacional Autónoma de México.
- Arreola Ávalos MG. (2015). Causas de no aceptación de métodos de planifiación familiar en mujeres en edad fértril de 12 a 49 años en el centro de salud de conca, arroyo seco en el periodo de enero - febrero del 2013. Tesis. Universidad Nacionala Autónoma de México.
- Pinta MJL. (2022). Elección del Método Anticonceptivo en una Población Rural. Polo del Conocimiento: Revista científico-profesional. 7(1):250-269.
- Xiomara NHS, Lily TMT. (2020). Factores socio culturales asociados al no uso del implante sub dermico “implanon” en mujeres usuarias de planificacion familiar, centro de salud Monterrey, Huaraz 2019.
- Mundigo AI. (2005). Religión y salud reproductiva: encrucijadas y conflictos. Center for Health and Social Policy II Reunión de investigación sobre embarazo no deseado y aborto inseguro. Desafíos de salud pública en América Latina y el Caribe Ciudad de México, 17 a 19 de agosto de 2005.
- Ramirez Vázquez MG. (2020). Factores socioculturales asociados a la no utilización de métodos de planificación familiar en adolescentes en una unidad de primer nivel de atención. Vol. 2, Tesis. Universidad Nacional Autónoma de México.