Information Links
Related Conferences
Previous Issues Volume 4, Issue 1 - 2020
Fluoride Application and Prescribing: Evidence Based Toolkit and How Well Salford Community Dental Service is Giving Fluoride Intervention
Maria Jackson BDS, MFDS RCPS (Glasg)
University of Liverpool Dental Hospital, United Kingdom
Corresponding author: Maria Jackson BDS, MFDS RCPS (Glasg), University of Liverpool Dental Hospital, United Kingdom, E-mail: [email protected]
Received Date: October 02, 2020 Publication Date: October 28, 2020 Copyrights: Jackson M. ©2020. Citation: Jackson M. (2020). Fluoride application and prescribing: Evidence based toolkit and how well Salford Community Dental service is giving fluoride intervention. Mathews J Dentistry. 4(1):26.
ABSTRACT
Introduction: The dental patients that are seen at SRFT services often have a high caries risk due to many different reasons such as an inability to brush properly through either a disability or living circumstances. In 2007 Public Health England published a toolkit for dentists with guidance of preventative aids to help reduce tooth decay which includes appropriate fluoride intervention for patients.
Aims and Objectives: The aims of this retrospective study and audit was to find out if SRFT dental services are following fluoride intervention guidelines for every patient or whether more can be done to ensure we are helping our patients to prevent tooth decay.
Methodology: 120 child and adult examination notes were assessed at random from six different dentists (20 from each). The criteria used to assess the notes was whether patient’s oral hygiene status was documented, whether the patient had been caries risk assessed, and if high caries risk, was fluoride varnish or a fluoride prescription provided.
Results: 83% of notes at the patient’s oral hygiene status documented, 82% of notes had been caries risk assessed and 49% of high caries risk patients had the appropriate fluoride intervention.
Conclusion: Improvements across all categories are required including what is documented in patient notes and following fluoride prevention guidelines to provide excellent care to our patients and help to reduce caries risk.
KEYWORDS: Tooth decay; Fluoride Application; Toolkit; Oral hygine, Dental services
BACKGROUND
Tooth decay has an impact not only on a patient’s oral health but also on their quality of life. It can cause many problems including pain, lack of sleep, bullying, absence from school or work and anxiety. In 2007, Public Health England published a toolkit for dentists with guidance of preventative aids to help reduce tooth decay, including fluoride application and prescribing guidance.
The world health organisation states there are two significant global burdens of oral disease, one being dental caries and the other being periodontal disease. Both of these are mainly preventable diseases which is why it is so important to aid patients with the right preventative tools.
Children’s oral health in the UK has improved over the last 20 years but there is still a large room for improvement. It is still a big problem in the UK as tooth decay was the most common reason for hospital admissions in children for five to nine year olds in 2012-2013 [1] and in 2014/15 hospital trusts spent £35million on extractions of teeth for children under 18 [2].
In 2009 the Adult health survey in the UK found that 94% of adults had at least one natural tooth [3] compared to the 1978 survey which found 72% of adults had at least one natural tooth [4]. This shows that people are keeping their teeth for a lot longer so it is important to continue delivering preventative advice throughout a patient’s life to help prevent decay and dental pain.
Salford Royal Community dental service provides specialised dental services to people living in Salford and surrounding areas with complex needs who are unable to use general dental services. These patients are more likely to have a higher caries risk due to these complex needs such as an inability to brush their teeth. Salford is in the North West of England which is a more deprived area than other places in the country. In the Northwest of England 34.8% of five year old children had tooth decay compared to 21.2% in south east England [1]. The North West of England was the region with the most tooth decay for five year old children in England. This is why it is so important we do as much as we can to prevent tooth decay.
In the North West of England only 7% of adults had excellent oral health, which means 93% of adults can improve their oral hygiene to help prevent oral diseases. In this area there is 30% of adults with carious teeth and 11% of adults were found to be in some degree of dental pain on examination.
To target high levels of decay the focus must be on prevention – including tailored brushing advice, diet advice to reduce sugar intake and exposure to fluoride through varnish, toothpaste and rinses. By giving the correct and useful information to patients, it will help stop dental problems before they develop [5].
AIMS & OBJECTIVES
The aims of this retrospective study and audit was to find out if Salford Royal community Dental Service are following fluoride intervention guidelines for every patient or whether more can be done to ensure we are helping our patients to prevent tooth decay.
To assess if fluoride should be prescribed through toothpaste or fluoride rinse or whether fluoride varnish should be applied a caries risk assessment needs to be completed. If a high caries risk is found then one or more fluoride adjuncts should be given to the patient. This is to be done to assess current records to see if they meet best practice, identify examples of poor record keeping highlighting problems and aid training for staff members to improve records and fluoride intervention.
Caries risk assessment should be carried out by collecting information about:
- the patient’s oral hygiene regime
- the patient’s oral health status
- any visible plaque
- any active caries
- if the patient suffers from a dry mouth
- if the patient has any orthodontic appliances
- if the patient has any special needs
- any other predisposing factors to caries
STANDARDS
The guidelines set out in ‘Delivering better oral health: an evidence-based toolkit for prevention’, Third edition, Public Health England’ (March 2017) have been used to set the standards for this audit and for recommendations to improve the Dental services prevention plan [6].
Below are the guidelines set out in the toolkit
Fluoride varnish application
- All children aged 3 and over should have fluoride varnish applied to teeth two times a year (2.2% NaF)
- Any patients (child or adult) from 0 years old who are giving concern should have fluoride varnish applied to teeth two or more times a year (2.2% NaF)
Fluoride toothpaste prescription
- Children aged 10 or above with active caries should be prescribed 2800ppm fluoride toothpaste (0.619% NaF)
- Any patient aged 16 or above with active caries should be prescribed 5000ppm fluoride toothpaste (1.1% NaF)
Daily fluoride rinse
- Children aged 8 or above with active caries should be prescribed a daily fluoride rinse (0.05% NaF) to be used at a different time to brushing
- Adults with active coronal or rot caries should be prescribed a daily fluoride rinse (0.05% NaF) to be used at a different time to brushing
Oral hygiene routine
- In order to know whether to provide fluoride and what instructions to give, the patient’s own oral hygiene regime must be documented
Caries risk assessment
- In order to know whether to provide fluoride intervention a caries risk assessment must be carried out, and every patient should be given a low, medium or high caries risk
Standard 1: All notes have the patient’s oral hygiene regime documented; this is to include how often they brush their teeth and using what.
Standard 2: All patients should be risk assessed and given caries risk of low, medium or high
Standard 3: All high risk caries patients should have the correct fluoride intervention provided either through a fluoride prescription (if of appropriate age) or fluoride varnish application or both.
METHODOLOGY
- 20 notes from each dentist were analysed, totalling 120 notes (appendix 1)
- Notes included children and adults of all ages
- These notes were chosen at random from clinic lists on R4 from 01/10/2018 to 30/11/2018
- This data was collected retrospectively as notes had to be written prior to collecting data
- All notes were clinical examinations of routine patients of SRFT community dental services, not patients referred for treatment only
- Data was analysed using the dental collection pro forma (appendix 2), tally charting for each dentist what had been included in the online dental note
- The criteria used to assess the notes are as follows:
- Was the patient’s oral hygiene routine documented
- Was the patient’s oral health status documented
- Was there any active caries
- Has the patient any predisposing factors to caries e.g. special needs, dry mouth
- Has the patient’s caries risk been documented
- Has the patient got a high caries risk 8. If the patient was given a high caries risk, the notes were assessed on the following points:
- Has the patient been prescribed high fluoride toothpaste
- Has the patient been prescribed a daily fluoride rinse
- Has the patient had fluoride varnish applied to their teeth
Problems encountered
There were several problems that were encountered when collecting data which made the process more time consuming and made analysing the data slightly more challenging.
The first problem encountered was that although there was a dental examination pro forma which included most questions and information required, some dentists were not using the pro forma correctly which meant the information was incorrect and was not filled in a lot of the time. This made it difficult to establish what the caries risk for the patient was and what fluoride intervention was suitable for these patients. This also caused challenges when making recommendations, as there was already a dental proforma in place that was not working.
Another problem encountered was that sometimes fluoride prescriptions had been given to patients but not documented correctly within the notes which meant there was no record of the prescription being given. This made data collecting more time consuming as not only patient records had to be analysed but also the prescription pad logbook to see whether or not a prescription had been written but not documented. This was a problem not only for the audit but also could cause patients to be overprescribed if nothing is shown from the previous appointments.
Another problem encountered when collecting data was that dentists did not state if fluoride application was attempted and failed, they just did not include this in their notes. Often fluoride varnish can’t be placed due to the patient’s limited cooperation. Salford community dental services see a lot of special needs patients who are unable to allow fluoride varnish application. If a reason for not placing fluoride varnish was not documented, then was presumed to have been inappropriate fluoride intervention.
RESULTS
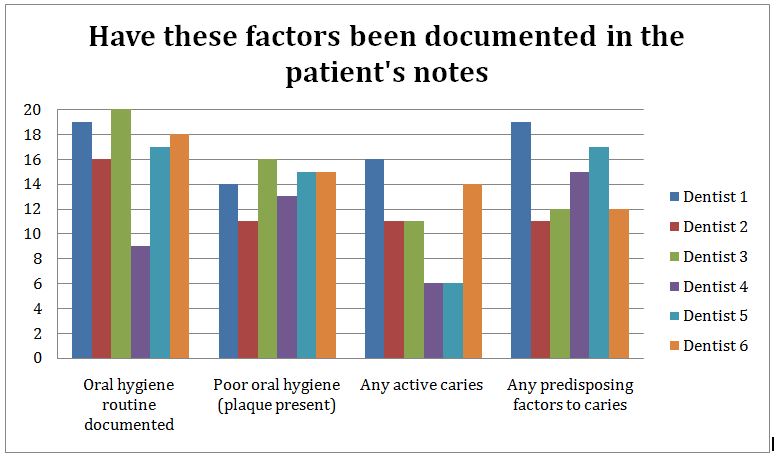
Figure 1: Factors documented in patient’s notes.
This chart shows (figure 1) what factors have been documented in a patient’s notes. There is a large deviation in results between dentists.
Poor oral hygiene, active caries and any predisposing factors to caries findings are dependent on the patient being seen and are criteria which dentists should document but this should not be 20/20 as not all of our patients will have poor oral hygiene, active caries or predisposing factors.
A patient’s oral hygiene regime should be documented in 100% of the notes set out in standard 1. One dentist had documented oral hygiene regime in 100% of notes, however another dentist had only included oral hygiene regime in their notes in 45% of notes.
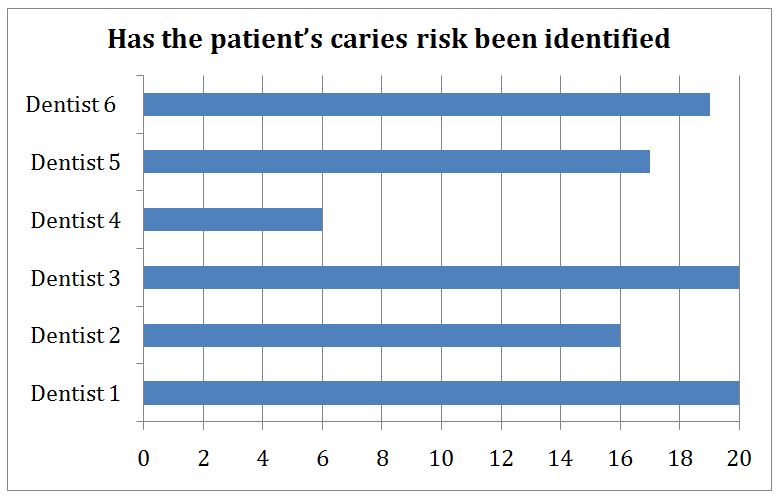
Figure 2: Caries risk to a patient at routine examination.
This chart shows (Figure 2) whether a caries risk was given to a patient at that routine examination appointment. Again, this chart shows that there is a large deviation in results between dentists. There should always be a caries risk assessment carried out as outlined in standard 2 and a low, medium or high caries risk given to every patient seen.
Two dentists gave 100% of their patient’s a caries risk compared to one dentist gave only 30% of patient’s a caries risk.
Whether or not a patient was given a high caries risk depends on the patient and their oral health. However, if not all patients were caries risk assessed then we were unable to see the accurate number of high caries risk patients and whether the correct intervention was provided.
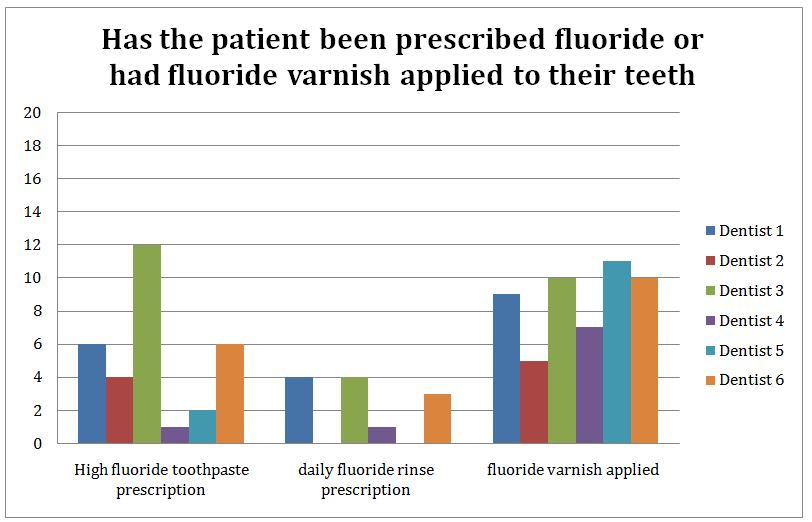
Figure 3: Number of patients that had either fluoride prescribed or applied to their teeth.
This chart shows (figure 3) the number of patients that had either fluoride prescribed or applied to their teeth. These categories should not be at 100% as not all patients analysed were of a high caries risk and what can be prescribed is subject to age.
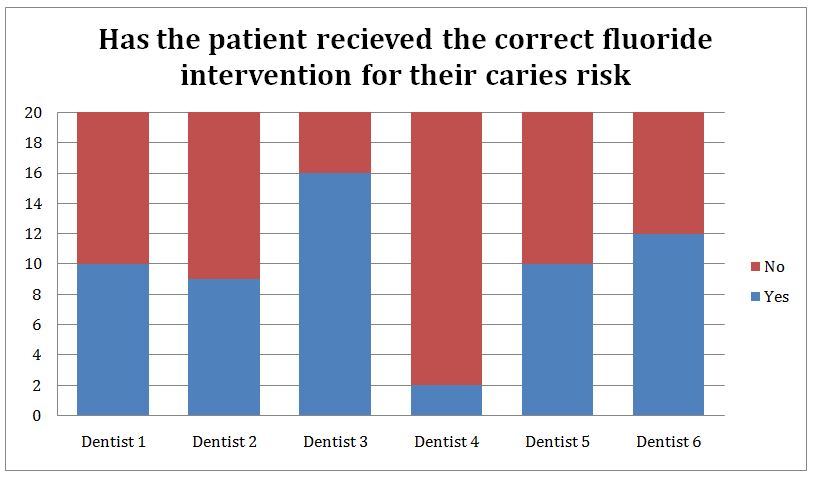
Figure 4: Whether the patients received the correct fluoride intervention for their caries risk.
This chart shows (Figure 4) whether the patients received the correct fluoride intervention for their caries risk given. It again shows a wide range of results between different dentists. All patients seen should be receiving the correct fluoride intervention as outlined in standard 3. If a patient’s notes had not included a caries risk then it was analysed as not having received the correct fluoride intervention as it is unclear what fluoride should have been provided to these patients.
Not one dentist met the set standard of standard 3.
The highest scoring dentist gave 80% of patients seen the correct fluoride intervention compared to the lowest scoring dentist that gave only 10% of patients seen the correct fluoride intervention.
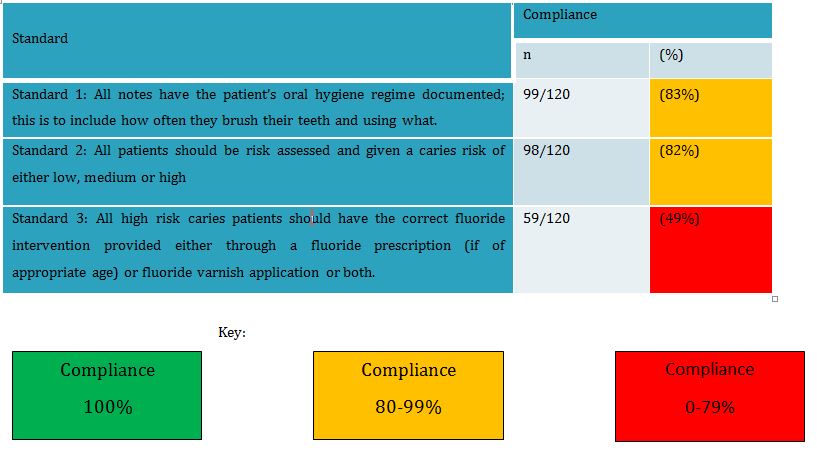
Table 1: Compliance of standards.
SUMMARY OF OBSERVATIONS
Areas requiring improvement
- All notes have the patient’s oral hygiene regime documented; this is to include how often they brush their teeth and using what. Only 83% of notes were compliant with this standard.
- All patients should be risk assessed and given caries risk of low, medium or high. Only 82% of notes were compliant with this standard.
- All high caries risk patients should have the correct fluoride intervention provided through a fluoride prescription (if of appropriate age) or fluoride varnish application or both. Only 49% of notes were compliant with this standard (Table 1).
The findings showed there were improvements that needed to be made not only in fluoride intervention but also in note taking and documenting discussions that occur at the dental examination appointments. This is not only important for prevention but also for documenting discussions and the consent process undertaken regarding treatment plans. The spread of data across dentists indicates that some staff requires educating more than others.
Over all of the standards assessed, dentist 4 consistently scored the lowest and dentist three consistently scored the highest, however as the data was anonymized, all dentists were required to undergo the same training to improve these standards.
All of the patients should be getting the correct fluoride intervention for their caries risk with 100% compliance. If a patient has been identified as high caries risk then they should be having fluoride varnish placed and a fluoride prescription given if of the appropriate age.
Oral hygiene should be documented in 100% of the notes as this is information gathering. Caries risk should be identified in 100% of the notes as this is required to give patients an examination recall and what fluoride intervention should be being placed. It is also useful information to refer back to, to see if a patient has improved their brushing and eating habits.
RECOMMENDATIONS
In order to meet Standard 1, the current dental pro forma was altered to make it shorter and easier to use. The dental pro forma already in place was very long with a lot of text to read and only areas for free text. It did include a section to detail a patient’s oral hygiene maintenance but this was not being filled in appropriately by the dentists, perhaps due to the fact it required free text and was unclear. Brushing frequency, type of toothbrush, inter dental aids and what toothpaste the patient uses was added to the pro forma to ensure clinicians were asking and documenting this information. These are in a drop down format to make it easier for dentists to select an answer. There is also an area underneath to add any free text if required, for example to document who was brushing the patient’s teeth for them.
In order to meet Standard 2, a caries risk assessment has to be documented. The same dental pro forma as above, already included a section for a patient's caries risk, but like with oral hygiene maintenance it was not being filled out properly. The clinicians need to ensure they are inputting low, medium or high into this section. This was created again as a drop down list to make it easier to select an answer. A departmental meeting was held to underline the importance of filling out the pro forma correctly and documenting the relevant information gained at these appointments. The clinical and legal reasons for this were highlighted to ensure the whole team understood the requirements for accurate documentation.
In order to meet Standard 3, several recommendations were made. Fluoride varnish application was added to the same dental pro forma, again as a drop down list of yes, no or attempted. If it had been attempted but not achieved then a reason why could be documented within the additional free text area for example if there was limited cooperation.
At the staff departmental meeting audit findings were presented to the whole team including dentists, dental nurses and reception staff in order to highlight the areas for improvement and make staff aware of the lack of intervention for some patients. They were educated on the importance of information gathering from a patient and the uses of fluoride intervention and aids. For most this was a refresher and reminder session.
The importance of working as a team was also highlighted. If the dentist forgets to apply fluoride or write a prescription, the rest of the team should be reminding them to do so. Having these areas included in the pro forma will remind not only the dentist but also the assisting dental nurse as often it is the nurse that fills the pro forma in initially.
DISCUSSION
There are many take home messages from the findings of this audit. Firstly that it is important to establish good brushing from a young age to build brushing into day to day routine the same as washing [7]. If a patient says they are brushing their teeth two times a day; morning and night, there is still further information that can be gained, such as what toothpaste they are using or are they rinsing with water afterwards. There is evidence to suggest that tooth brushing is most beneficial preventatively if certain advice is given to patients and it is followed. These include; brushing starting as soon as the first deciduous tooth erupts, using appropriate fluoride toothpaste and brushing twice daily [6].
This audit did not look into whether dentists were assessing a patients diet but there is a wealth of evidence showing the impact of diet on tooth decay. On examination of any patient information about their diet habits should be investigated. Not only if they’re eating chocolate and sweets but the frequency they are eating anything containing sugar and what drinks are being consumed throughout the day. There is evidence showing the amount of sugar eaten and the frequency it is being consumed increases the risk of dental decay [8]. As healthcare professionals it is important to be educating patients in healthy diets, not only to help oral health but overall health. Non-milk extrinsic sugars are foods or drinks that have had sugar added to it by either consumer or manufacturer or they are fruit juices/smoothies. These sugars are the largest cause of tooth decay and guidelines say reducing the intakes of these sugars should be the main message given to the public [9]. Advice given should state these sugars should only be consumed four times daily including meal times as this will help reduce risk of tooth decay [10].
As stated throughout, a caries risk of a patient needs to be established. Caries risk is based upon any active caries present, oral hygiene regimes and diet. If a patient is high caries risk they will have either active caries present, poor oral hygiene or a poor diet or a combination of several risk factors. Those patients with a high caries risk should be provided with a fluoride adjunct to help reduce tooth decay. A Cochrane systematic review analysed 22 trials which looked at fluoride varnish application and the prevention of caries in children. It found that fluoride varnish applied to permanent teeth experienced 43% less carious teeth than the children in the no treatment groups. It also found that fluoride varnish applied to primary teeth experienced 37% less carious teeth than children in the no treatment groups. The trials used in this Cochrane review mainly used 22,600 ppm fluoride varnish [11]. There is very few contraindications to the applying fluoride varnish, one being a small risk of allergy to the colophony within the varnish. In patients with ulcerative gingivitis and stomatitis, and children who have had hospital admission due allergic reactions, including asthma, application of fluoride varnish is contraindicated [6]. For patients that varnish is not applied then extra attention should be paid to ensure they have excellent oral hygiene and a healthy balanced diet.
There are limits to how reliable this audit is as there is only a small sample size and it is a retrospective design which increases the risk of bias when collecting results. The bias has been minimised as much as possible by randomly choosing notes to assess but cannot be eliminated completely. This audit does however highlight the issues surrounding not providing patients with the best preventative aids.
In putting in place the recommended delivering better oral health guidelines, patients should become better educated in how to care for their oral health but also a reduction in caries should be seen from patients that have been given preventative advice and fluoride varnish application or prescriptions. However, even if excellent preventative advice is given to patients, verbally and through leaflets, it is up to the patient to follow this advice at home. If advice is not followed then their caries risk will not be reduced as home care and diet is the most important aspect of caries risk which cannot be controlled by dentists.
In conclusion, by providing patients with information that is recommended by the delivering oral health guidelines, applying fluoride varnish and providing fluoride prescriptions to those with high caries risk, a reduction in caries should be seen. It must be stressed to patients that oral hygiene routines at home and diet are the most important ways in which a patient’s caries risk can be reduced.
REFERENCES
- Local authorities improving oral health: commissioning better oral health for children and young people, an evidence-informed toolkit for local authorities, Public Health England. June 2014. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/321503/CBOHMaindocumentJUNE2014.pdf
- Tackling poor oral health in children, Local government’s public health role, Local government association. April 2016. https://www.local.gov.uk/sites/default/files/documents/tackling-poor-oral-health-d84.pdf
- Adult dental health survey 2009, published march 2011. https://files.digital.nhs.uk/publicationimport/pub01xxx/pub01086/adul-dent-heal-surv-summ-them-exec-2009-rep2.pdf
- Adult oral health: applying all our health, published 11 December 2017, public health England. https://www.gov.uk/government/publications/adult-oral-health-applying-all-our-health/adult-oral-health-applying-all-our-health
- Victoria Chenery, Ian O’ Sullivan, Deborah Lader, Adult dental health survey, England - key findings, 24th March 2011.
- Delivering better oral health: an evidence-based toolkit for prevention, Third edition, Public Health England. March 2017. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/605266/Delivering_better_oral_health.pdf
- Duijster D, Jong-Lenters M, Verrips E, Loveren CV. (2015). Establishing oral health promoting behaviours in children – parents’ views on barriers, facilitators and professional support: a qualitative study. BMC Oral Health. 15:157.
- Moynihan PJ. (2002). Dietary advice in practice. British Dental Journal. 193:563–568.
- Oral Health and Nutrition Guidance for Professionals, NHS Health Scotland. June 2012. http://www.healthscotland.scot/media/2337/oral-health-and-nutrition-guidance-for-prof-2012.pdf
- World Health Organization. Diet, nutrition and the prevention of chronic diseases: report of a joint WHO/FAO expert consultation. (WHO Technical Report Series 916.) Geneva: World Health Organization; 2003.
- Marinho VCC, Worthington HV, Walsh T, Clarkson JE. (2013). Fluoride varnishes for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 7:CD002279.
APPENDIX 1 – Standards Table.
|
Standard |
Target |
Exception |
Source |
|
|
Section 1 - Admission Documentation |
||||
|
1 |
All notes have the patient’s oral hygiene regime documented; this is to include how often they brush their teeth and using what. |
100% |
|
Delivering better oral health: an evidence-based toolkit for prevention’, Third edition, Public Health England’ (March 2017)
|
|
2 |
All patients should be risk assessed and given a caries risk of either low, medium or high |
100% |
|
Delivering better oral health: an evidence-based toolkit for prevention’, Third edition, Public Health England’ (March 2017) |
|
3 |
All high risk caries patients should have the correct fluoride intervention provided either through a fluoride prescription (if of appropriate age) or fluoride varnish application or both. |
100% |
|
Delivering better oral health: an evidence-based toolkit for prevention’, Third edition, Public Health England’ (March 2017) |
APPENDIX 2 – Copy of Data Collection Proforma Dentist initials: Patient Identification number: Patient age:
|
|
Yes |
No |
|
Has the patient’s oral hygiene routine been documented in the notes? |
|
|
|
Has the patient got poor oral health? (plaque visible) |
|
|
|
Has the patient got any active caries? |
|
|
|
Does the patient have dry mouth/orthodontic appliance/special needs (predisposing factor to caries)? |
|
|
|
Has the patient’s caries risk been identified in the notes? |
|
|
|
Has the patient got a high caries risk? |
|
|
|
Has the patient been prescribed high fluoride toothpaste? |
|
|
|
Has the patient been prescribed a daily fluoride rinse? |
|
|
|
Has the patient had fluoride varnish applied to their teeth? |
|
|
|
|
Yes |
No |
|
Has the patient had all the correct fluoride intervention provided for them for their caries risk? |
|
|