Information Links
Related Conferences
Previous Issues Volume 7, Issue 1 - 2023
A Review on Analytical Method of Dapagliflozin and Empagliflozin by QBD Approach
Deepak Dalal*, Ravi Kant, Reena Badhwar
Department of Pharmaceutical Quality Assurance, SGT University, Gurugram, Haryana,122505, India
*Corresponding Author: Deepak Dalal, Department of Pharmaceutical Quality Assurance, SGT University, Gurugram, Haryana, 122505, India; Email: [email protected]
Received Date: 17 February, 2023
Published Date: 20 March, 2023
Citation: Dalal D, et al. (2023). A Review on Analytical Method of Dapagliflozin and Empagliflozin by QBD Approach. Mathews J Pharma Sci. 7(1):17.
Copyrights: Dalal D, et al. © (2023).
ABSTRACT
Type 2 diabetes mellitus affects 90% of people with diabetes and causes high blood sugar levels and other medical conditions that are associated with it, including an increased risk of cardiovascular disease, kidney disease, ophthalmic diseases, and neurological problems. Several analytical methods have been illustrated in the literature, including UV spectroscopy, High-Performance Liquid Chromatography, High-Performance Thin Layer Chromatography, and Liquid Chromatography, Mass Spectrometry (LCMS). In order to gather information for this work, we reviewed the literature on a variety of stability tests, impurity profiling, and bio-analytical approaches that were used to establish the concentration of Empagliflozin and Dapagliflozin in formulations and singly. The Limit of Detection (LOD), Limit of Quantitation (LOQ), Standard Curve, Accuracy, and Precision are some of the analytical validating factors for the analysis of Empagliflozin alone or in combination with Linagliptin or Metformin that are covered in this review. This evaluation assists subsequent analytical studies on the aforementioned drugs.
Keywords: Dapagliflozin, Empagliflozin, UV-Spectroscopy, HPLC, QBD Approach
INTRODUCTION
Over 285 million people worldwide currently have diabetes, and that number is projected to rise. Type 2 diabetes mellitus is the cause of over 90% of all diabetes cases (T2DM). Diabetes is a long-term metabolic disease that results in hyperglycemia and raises the risk of both little and large vascular issues. Several medications, such as Metformin (MET), thiazolidinediones (Glitazones), which are insulin-sensitizing agents, sulfonylureas, which promote insulin secretion, glucagon-like peptide-1 analogues, and dipeptidyl peptidase-4 inhibitors act on the incretin pathway to stimulate insulin secretion while exerting additional metabolic effects in addition to insulin, are oral anti-diabetic [1]. Recent studies have explored the prospect of treating type 2 diabetes by investigating a novel method that inhibits the re-absorption of glucose from glomerular filtrate in order to enhance renal glucose excretion. The proximal tubules' S1 region is critical in controlling the re-absorption of glucose from glomerular filtrate when blood sugar levels are normal [2].
T2DM needs novel therapeutic drugs to improve treatment because it is a widespread and progressing condition. Worldwide, 347 million individuals have been diagnosed with diabetes, with 90–95 percent being type 2. Chronic hyperglycemia poses a risk of death for these patients. The majority of patients struggle to keep their blood sugar levels within normal ranges. Thus, even the milder individuals were able to manage the effect in other areas, such as blood pressure (BP) or lipid profiles. Hyperglycemia makes it challenging to control blood sugar levels due to medication side effects, drug-drug interactions, related disorders, and hospitalization. Despite the fact that diabetes care has shifted too much towards the patient, new recommendations urge starting a straightforward therapy like MET and making adjustments to one's daily routine. For patients with diabetes, achieving blood sugar levels that are as close to normal as possible is of utmost importance. Over half of the patient population in India is affected by hyperglycemia and vascular problems. Therefore, the use of innovative therapeutic medicines that can delay the development and severity of problems without compromising patient safety is urgently needed [3].
A significant therapy option for type 2 diabetes, dapagliflozin (DPG) is a novel medication that belongs to the group of sodium glucose co-transporter 2 (SGL-2) inhibitors [4]. Saxagliptin and metformin (MET) are two medications that can be taken along with DPG. Because Dapagliflozin can be used in a variety of combinations, researchers are interested in learning more about the pharmacological, analytical, and bio-analytical profile of the medication [5]. Due to how terrible the condition is, medicine is crucial for both therapy and related research. DPG is incredibly important to the pharmaceutical business both on its own and in conjunction with other anti-diabetic drugs [6].
Empagliflozin has the potential to be a highly selective sodium-glucose co-transporter-2 (SGLT-2) inhibitor for the management of type 2 diabetes mellitus when administered alone or in conjunction with metformin or dipeptidyl peptidase-4 (DPP-4) inhibitors [7].
DAPAGLIFOZIN
DPG, an antihyperglycemic drug, is now a well-known SGLT2 inhibitor. It demonstrates superior glucose level management over a period of more than two weeks. Because SGLT2 regulates the majority of renal glucose re uptake, inhibiting it increases renal glucose excretion and lowers blood sugar levels. DPG is demonstrating its efficacy as a type 2 diabetic treatment [8]. Inhibiting the transporter protein in the kidneys reduces the amount of glucose that is renally reabsorbs from the blood; as a result, less glucose is expelled in the urine, lowering blood glucose levels. The ability of the medicine to work is independent of insulin secretion and action. DPG's new method of action makes it possible to treat T2DM more effectively when combined with other anti-diabetic medications [9].
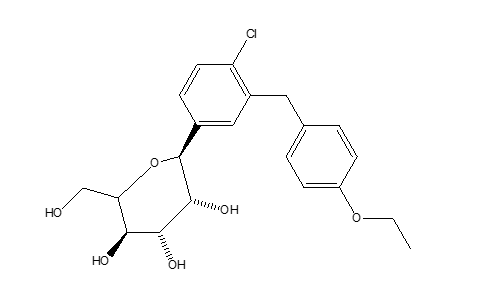
Structure of Dapagliflozin
PHARMACEUTICAL ANALYTICAL PROFILE OF DPG
LC and associated procedures were used in the vast majority of studies published for DPG alone or in combination, according to extensive literature searches for analytical methods of pharmaceutical substances published in relation to DPG [10]. HPLC was used to reach the highest level of analytical procedures, which were combined with SXG for second place and MET for third place, respectively. The rarest of all are single drug DPG LC findings.
There is very few HPLC-based literature that show forced degradation or stability tests. The articles explaining the stability-indicating method refer to stability investigations that are particular to the bulk medication. The years 2017–2019 witnessed the most articles in the literature on the subject of DPG estimation between 2010 and the present. There was no article about DPG research released in 2016. The findings of a study comparing literary works from various eras and analyzing them using various methodologies are provided [11].
ANALYTICAL METHODS FOR ESTIMATION OF DPG
HPLC Studies
HPTLC, a more advanced method of TLC, has developed into a crucial tool in bio-analytical and stability studies of pharmaceuticals. The literature review turned up three studies. Using pre-coated silica gel 60 F254 aluminum plates as the stationary phase and ACN ammonium acetate 10% - acetic acid as the mobile phase (9:0.9:0.1 v/v/v) at 225nm, the earlier study used HPTLC to estimate DPG [12].
In 2018, Nasser Sally et al. published the first report on the concurrent HPLC detection of DPG and MET HCl. In order to compare the effectiveness of each strategy, we used the pill form of XIGDUO.
The next year, two additional studies were found; the first was published by Ahmed et al., who calculated DPG and SXG along with their degradation product. The mobile phase contained a mixture of hexane, methanol, and ethyl acetate (4:2:4, v/v/v), and both medications were detected at 225nm. Farxiga was the preferred formulation in this experiment.
In 2019, Suma et al. released a new work on chromatographic separation utilizing a Merck pre-coated silica gel aluminum plate 60 F254 and a chloroform: methanol (9:1v/v) mobile phase. The detection was carried out using UV light with a wavelength of 223nm. OXRA pills with strength of 10.0 mg were employed in the accuracy research.
In a recent article, El-Shoubashy et al. reported on the simultaneous estimation of MET, SXG, and DPG. Chloroform, methanol, water, and acetic acid were used as the mobile phase during separation on Merck HPTLC plates at a scanning wavelength of 224nm [13].
UPLC
For the simultaneous measurement of SXG and DPG in tablets (10 mg DPG and 5 mg SXG), Madhavi, S. & Rani, A. P. present a UPLC method using an Acquity UPLC ethylene bridge (BEH) C18 1.7 m RP column with a mobile phase with 0.1% OPA and ACN as the composition (40:60). With PDA detection at 254nm, the injection volume was 10 l, the run time was 3.0 min, and the flow rate was 0.3 ml/min.
Kim et al. created a different technique for simultaneously identifying 26 anti-diabetic chemicals in dietary supplements. All of the compounds were separated with resolutions greater than 1.5. In the investigation, 96 samples were used, and a novel analytical method was used to analyse them. Seven of these samples had both pioglitazone and glibenclamide in them. This procedure seems to be a useful tool for stopping the widespread contamination of nutritional supplements with diabetes medications, which poses a severe risk to the general public's health [14].
EMPAGLIFOZIN
Empagliflozin (EMP), a sodium-glucose co-transporter 2 inhibitor, is a different gliflozin used to treat Type 2 diabetes mellitus (SGLT-2). The drug's activity is directed at sodium-glucose co-transporter-2 (SGLT-2) receptors in the proximal tubule. By inhibiting SGLT2, Empagliflozin increases glucose excretion in the urine and reduces renal re-absorption of glucose. The medication works independently of insulin to lower blood sugar levels. Empagliflozin 10 or 25 milligram caused a 64 or 78 gram increase in 24-hour urine glucose excretion in type 2 diabetic patients, respectively. Intravascular contraction is brought on by the diuretic and natriuretic actions of Empagliflozin, which reduce salt and volume load. Empagliflozin is also connected to a drop in blood pressure and a decrease in appetite without increasing heart rate [15].
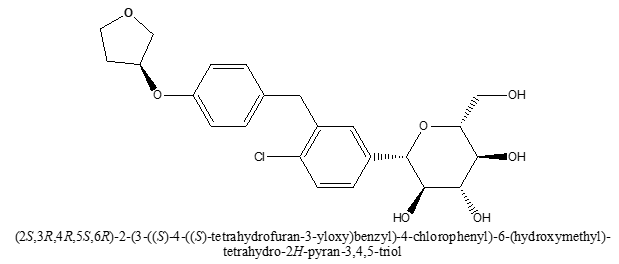
STRUCTURE OF EMPAGLIFOZIN
ANALYTICAL METHODS FOR ESTIMATION OF EMP
HPLC
Sushmita et al. created a stability-indicating RP- HPLC method for the aim of simultaneously assessing MET and EMP in tablet form. A standard BDS column with a 250 x 4.6 mm dimension, a 5m particle size column, and a flow rate of 1 ml/min was used to achieve the separation. The mobile phase used was a 0.1% orthophosphoric acid and 50:50 acetonitrile mixture. A number of stability tests were run on EMP, and data was gathered. Retention times for MET were 2.58 minutes and for EMP were 3.6 minutes [16].
A different RP-HPLC method was created by Syed Irfan Ali and Bharath Rathna Kumar P. for the estimation of EMP and MET in tablet dosage form. This method used a C18 column, 0.1% orthophosphoric acid, and acetonitrile as the mobile phase, a flow rate of 1.1 ml/min, and detection at the isobestic point of the two drugs at 226nm. The linearity ranges for MET and EMP were respectively 125-750 ppm and 3.12-18.75 ppm. According to ICH Q2 R1 criteria, it has been demonstrated to be effective [17].
S. K. Godasu and S. K. Sreenivas developed a reversed-phase high-performance liquid chromatography (RP-HPLC) method using a C18 column, methanol, and phosphate buffer at pH 3 as the mobile phase in order to quantify the amount of MET and EMP in a particular dosage or quantity of bulk medication. 1 ml/min was chosen as the delivery rate. The purity of MET and EMP were found to be 99.87% and 100.27%, respectively, with retention times of 2.403 and 3.907 minutes.
Using a BDS column as the stationary phase, 0.1% orthophosphoric acid and acetonitrile (70:30 v/v) as the mobile phase, and a flow rate of 1 ml/min with a wavelength of 233 nm, Shyamala et al. developed a validated RP- HPLC method to identify EMP in its active medicinal component form. The medicine was tested under acidic, alkaline, peroxide, photolytic, neutral, and oxidative degradation settings. The results revealed that the drug is most sensitive under oxidative and acidic conditions.
Anjali et al. created an RP-HPLC technique for the analysis of EMP and LIN in tablet dosage form that makes use of a C18 column (250mm 4.6mm, 5m). KDP buffer (pH 3.4) and methanol are combined in the mobile phase at a ratio of 70:30 (vol/vol). There was a linear trend between 50 and 150g/ml. Jaishwal et al. employed the HPLC method of analysis with 0.1% orthophosphoric acid and acetonitrile as the mobile phase and a detection wavelength of 230nm to calculate process-related pollutants in EMP pharmaceutical compounds. The use of a C8 column allowed for chromatographic separation (250mm 4.6mm, 5mm). [18] The column was maintained at 55 degrees Celsius, and all chromatographic parameters were assessed in accordance with ICH standards, ensuring the best resolution possible.
UV SPECTROSCOPIC METHOD
This section examines the few published techniques for EMP analysis. Bossom M. Ayoub has created two simple spectrometric procedures for determining EMP and MET in their dose form, i.e., SYNJARDY®. They employed an approach that was both economical and involved continual multiplication and a spectrum-subtraction methodology. For EMP and MET, the limits of detection are established to be 0.12 and 0.14 g/ml, respectively [19].
Another alternate method for studying EMP and MET together was developed by Bossom M. Ayoub [20]. The spiking method was used with zero-order spectral scan estimation to enhance focus. Methanol was employed as the blank for both medications, and the procedure was validated in compliance with ICH guidelines [21]. It was discovered that for EMP and MET, the limits of quantification and detection were 0.51 g/ml and 1.52 g/ml, and 0.31 g/ml and 0.94 g/ml, respectively.
B. M. Ayoub developed a spectrophotometric and chemo-metric method that involves altering the zero-order spectra to simultaneously quantify EMP and MET in tablet form. The sample enrichment procedure helped to increase the concentration. The linearity for both drugs was between 2 and 12 micrograms per millilitre. As LOD values, 0.20 g/ml and 0.19 g/ml were determined. EMP had a LOQ of 0.59 g/ml, whereas MET had a LOQ of 0.58 g/ml. The UV spectrophotometric approach, developed by N. Padmaja and G. Veerabhadram, is employed for the simultaneous determination of EMP and LIN in pharmacological dose form. For EMP and LIN, method validation was established with %RSD less than 2% and linearity between 5 and 15 g/ml and 2 to 6 g/ml, respectively.
DISCUSSION
T2DM is a chronic metabolic disease that is life-threatening due to a number of potentially serious consequences. Since type 2 diabetes affects 95 percent or more of diabetic patients, they require specialized care. SGLT2 inhibitors have gained a lot of attention recently due to their unique method of action. Because gliflozins are connected to substances found in nature, their therapeutic advantages are increased. Dapagliflozin (DPG), a new SGLT-2 inhibitor among the gliflozins, has been discovered to decrease renal glucose reuptake and lower plasma glucose levels, whereas empagliflozin specifically and potently inhibits SGLT2 in the kidneys, lowering glucose re-absorption in the proximal tubule. Therefore, these medications are of utmost importance to pharmaceutical experts. This review also discusses the new anti-diabetic origins of gliflozins.
This review also discusses the new anti-diabetic origins of gliflozins. The pharmacological, analytical, and physicochemical properties of DPG and EMP are covered in great length throughout the article. The analysis included all references to DPG & EMP analytical research since their 2010 discovery. Pharmaceutical analysis of any specific drug molecule is intrinsically erroneous if a method for assaying the drug in formulation cannot be created. As a result, the goal of this article is to examine the analytical techniques for DPG and EMP in formulations. In addition, we reviewed the current formulations' brand names, dosages, and formulations. Since these drugs are now only available as tablets, more research into alternative DPG & EMP-based drug delivery methods is urgently needed. EMP can be utilized with either LIN or MET, although at this moment, the market only offers the SXG and DPG combined medication formulation. Further DPG and other anti-diabetic drug combinations may be discovered through further research. The article specifies the precise pharmacological characteristics of the medicine, which will help with the bio-analytical evaluation of the drug and its future metabolomics. The isolation, categorization, and characterization of all the degradation by products are still pending.
CONCLUSION
The drug's effectiveness either alone or in conjunction with other specifically formulated anti-diabetic molecules is determined commutatively in the article. Both DPG and EMP are significant and brand-new contributions to the class of drugs known as SGLT2 inhibitors. The goal of this study's authors was to present the first in-depth, side-by-side, and effective analytical profile of DPG & EMP. In this paper, we assess the present approach for analyzing DPG and identify the more recent methodology for analyzing these medications individually or in combination.
Despite the widespread use of HPLC techniques, the authors concluded that further extensive research on forced degradation studies of the chemical in bulk/formulation and in the presence of other drugs is still required. However, the scope may be expanded to cover different experimental designs for a variety of reasons. Experimental designs like factorial, central composite, etc., are utilized for optimization of the analytical procedures which can be used to improve upon a current approach. There are presently no methods that include the full characterization of FDPs as IMPs or the reports necessary for determination in the presence of metabolites. As the reports for bio analytical determination mainly focus on blood plasma, more study into other biological fluids is required. These drugs' sensitivity to acidic, alkaline, and oxidative stress calls for additional investigation on photo stability and simultaneous exposure to numerous accelerated stress conditions. Our findings demonstrate the presence of distinguishable impurities in DPG and EMP, enabling a more complete assessment of their relative toxicities. It is possible to analyse bio-activity concurrently with other assays, which could produce beneficial outcomes for modern drug discovery and analysis. As a result, there is still a shortage of critical research on DPG and EMP analyses.
REFERENCES
- International Diabetes Federation. (2017). In: IDF Diabetes Atlast-8th Edition. Karuranga S, Fernandes JDR, Huang Y, Malanda B, (Ed) International Diabetes Federation; Brussels, Belgium.
- Beckman JA, Paneni F, Cosentino F, Creager MA. (2013). Diabetes and vascular disease: Pathophysiology, clinical consequences, and medical therapy: Part II. Eur Heart J. 34:2444–2452.
- Glechner A, Harreiter J, Gartlehner G, Rohleder S, Kautzky A, Tuomilehto J, et al. (2014). Sex-specific differences in diabetes prevention: A systematic review and meta-analysis. Diabetologia. 58:242–254.
- Hsia DS, Grove O, Cefalu WT. (2017). An update on sodium-glucose co-transporter-2 inhibitors for the treatment of diabetes mellitus. Curr Opin Endocrinol Diabetes Obes. 24(1):73–79.
- Plosker GL. (2014). Dapagliflozin: a review of its use in patients with type 2 diabetes. Drugs. 74(18):2191–2209.
- Meng W, Ellsworth BA, Nirschl AA, McCann PJ, Patel M, Girotra RN, et al. (2008). Discovery of dapagliflozin: a potent, selective renal sodium-dependent glucose cotransporter 2 (SGLT2) inhibitor for the treatment of type 2 diabetes. J Med Chem. 51(5):1145–1149.
- Padmaja N, Veerabhadram G. (2015). Development and validation of analytical method for simultaneous estimation of Empagliflozin and linagliptin in bulk drugs and combined dosage form using UV-visible spectroscopy. Scholar Res Lib. 7(12):306-312.
- Manoel JW, Primieri GB, Bueno LM, Wingert NR, Volpato NM, Garcia CV, et al. (2020). The application of quality by design in the development of the liquid chromatography method to determine empagliflozin in the presence of its organic impurities. RSC Adv. 10(12):7313-7320.
- Urooj A, Sundar PS, Vasanthi R, Raja MA, Dutt KR, Rao KNV, et al. (2017). Development and Validation of RP-HPLC method for simultaneous estimation of dapagliflozin and metformin in bulk and in synthetic mixture. World J Pharmacy Phar Sci. 6(7): 2139-2150.
- Ali SI, Kumar BRP. (2017). Stabilit Indicating Simultaneous Estimation of Metformin and Empagliflozin in Pharmaceutical Tablet Dosage form by RP HPLC. Asian J Res Chem. 10: 10(6):783-788.
- Yunoos M, Sankar GD. (2015). A validated stability indicating high-performance liquid chromatographic method for simultaneous determination of metformin hcl and dapagliflozin in bulk drug and tablet dasage form. Asian J Pharm Clin Res. 8(3): 320-326.
- Prameela KL, Veni RK, Satyanarayana PVVS, Babu HB. (2017). Development and validation of stability indicating reverse phase high performance liquid chromatography method with photodiode array detection for the simultaneous estimation of hypoglycemic agents, dapagliflozin and Metformin. Int J Pharma Bio Sci. 8(3):328-336.
- Hadi SA, Kumar BRP. (2017). Simultaneous estimation of metformin and dapagliflozin tablets by RP-HPLC. World Journal of Pharmacy and Pharmaceutical Sciences, 6 (11):1188-1199.
- Jayprakash R. (2017). Stability Indicating RP HPLC Method Development and Validation for the Simultaneous Determination of Vildagliptin and Metamorphin in Pharmaceutical Dosage Form. Int J Pharm Pharm Sci. 9(3):150
- Hermann LS, Kulhmann I, Plus W. (1995). Clinical pharmacology of biguanides. In: Hand Book of Experimental Pharmacology. Heidelberg, Germany: Springer: 374-407.
- Rajesh T, Lakshmi KS, Sharma S. (2009). Simultaneous determination of metformin and pioglitazone by reversed phase HPLC in pharmaceutical dosage forms. Int J Pharm Pharm Sci. 1(2):162-166.
- Shyamala M, Nirmala K, Mounika J, Nandini B. (2016). Validated stability indicating RP-HPLC method for determination of empagliflozin. Der Pharm Lett. 8(2):457-464.
- Ni L, Yuan C, Chen G, Zhang C, Wu X. (2020). SGLT2i: Beyond the Glucose Lowering Effect. Cardiovasc Diabetol. 19(1):98.
- Nasser S, Nasser I, Mostafa S, Elgawish M. (2018). Comparative high-performance liquid chromatographic and high-performance thin-layer chromatographic study for the simultaneous determination of dapagliflozin and metformin hydrochloride in bulk and pharmaceutical formulation. J Planar Chromat Modern TLC. 31(6):469-476
- Ganorkar SB, Sharma SS, Patil MR, Bobade PS, Dhote AM, Shirkhedkar AA. (2021). Pharmaceutical Analytical Profile for Novel SGL 2 Inhibitor, Dapagliflozin. 51(8):835-847.
- National library of medicine.